With the end of a congressional provision that had extended Medicaid coverage during the COVID-19 public health emergency, states are set to begin on April 1 what some Catholic health care leaders and Medicaid experts expect to be a chaotic and cumbersome process to redetermine the eligibility of the more than 90 million people currently enrolled in Medicaid or the Children's Health Insurance Program.
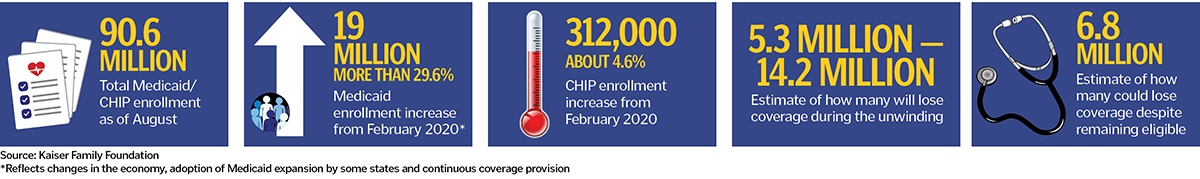
A sweeping budget measure passed by Congress and signed by President Joe Biden in the final days of 2022 ended the continuous Medicaid coverage requirement for states that had been in effect since March 2020. It allows the recertification of eligibility — a process dubbed the Medicaid unwinding — to start April 1. The end result of the unwinding will be that 5.3 million to 14.2 million people will lose their coverage, according to Kaiser Family Foundation estimates.
The Office of the Assistant Secretary for Planning and Evaluation within the Department of Health and Human Services predicts about half of those disenrollments will be of people who are eligible for coverage but stymied in providing proof by procedural hurdles, such as not being able to get through to the appropriate state agency because of overwhelmed phone lines.

Mike Slubowski, president and chief executive of Trinity Health, says the unwinding is certain to be a "real disruptor" for providers of care to the low-income Americans who rely on Medicaid.
The process will be complicated in part because each state will have its own methods and timelines of up to 12 months for the redeterminations of eligibility, Slubowski says. He points out that many states aren't planning for "an easy, warm handoff" of those who no longer quality for Medicaid to other coverage options such as the federally subsidized insurance marketplace. "We are worried about that."
Trinity Health, based in Livonia, Michigan, operates in 26 states and cares for 1.5 million patients who rely on Medicaid or states' CHIP coverage. CHIP provides low-cost insurance for children whose family income is too high for Medicaid but too low to purchase private insurance.
If just 5% of Trinity's Medicaid and CHIP insured patients lose coverage and have no other means to pay for treatment, Slubowski says the system stands to take an annual $80 million hit on revenue.
Compounding that financial blow, he says, could be that many of those patients, once uninsured, would no longer have access to a regular source of primary care to prevent or manage chronic conditions. Instead, acutely ill patients likely would turn to emergency rooms, where the cost of providing care is high, and urgent care facilities, where patients get only episodic treatment.

Temporary lifeline for children
Tricia Brooks, a research professor at the Georgetown University McCourt School of Public Policy's Center for Children and Families, urges all health care providers to be proactive in
informing patients about the unwinding. Brooks took part in a CHA webinar in November on the unwinding and discussed it during a later interview with Catholic Health World.
She notes that Medicaid and CHIP cover about half of the nation's children. "Medicaid is also the predominant source of coverage for pregnancy, people of color and rural communities," she adds.
Brooks says the redetermination requirement will affect all of the children enrolled in Medicaid and most of the children enrolled in CHIP because of how some of those state programs are connected to Medicaid.
She notes that researchers say 6 million children stand to lose Medicaid or CHIP coverage in the unwinding. For some of them, the coverage loss will be because they no longer qualify due to changes in their family income or situation. For others, the coverage will end because their families fail to successfully complete the reenrollment process.
However, the deal struck on Medicaid redeterminations in the end-of-the-year spending bill requires that states continue coverage for children for at least a year, even if a family's income makes them ineligible for government health insurance. The measure also makes permanent what had been a temporary rule letting states provide Medicaid coverage for a year postpartum.
Short staffs, unprecedented workloads
Congress put the continuous coverage requirement in place as one of several requirements for states to qualify for enhanced funding during the pandemic. Since then, the Medicaid and CHIP rolls have grown by more than 19 million, according to the Kaiser Family Foundation.
Brooks says some states might be under political pressure to finish the redeterminations on eligibility quickly and cull their rolls, especially given that the enhanced federal funding begins to phase out in the quarter after the provision ends.
The unwinding, Brooks says, "is a really big deal because of the unprecedented volume of work required for states to return to their routine eligibility and enrollment operations." She adds that it is coming at a time when states, like private employers, face challenges in recruiting and retaining workers.
Tools, partnerships
Brooks and her colleagues at Georgetown have created an extensive set of "unwinding resources" to assist various stakeholders throughout the process.
CHA also has created tools for systems to use and to customize to help in guiding Medicaid patients through the unwinding.

Paulo Pontemayor, senior director of governmental relations at CHA, notes that the organization's members provide care at more than 2,200 sites, putting them in direct contact with many patients who rely on Medicaid.
"CHA is committed to Medicaid and strengthening Medicaid but also to protecting beneficiaries as part of our commitment to ensuring access and affordability for all," Pontemayor says. "This is linked to our strategic advocacy goals and also really to the essence of what CHA's work is since the passing of the Affordable Care Act."

Another organization offering advice and assistance to health care providers on the Medicaid redeterminations is Catholic Charities USA. Ben Wortham, the group's vice president of behavioral health integration, and Susan Loughery, associate executive director of Catholic Charities Trenton in New Jersey, also took part in the CHA webinar in November.
Wortham notes that a majority of the billing that Catholic Charities does nationwide for behavioral and mental health care are Medicaid claims. The organization's revenue for that care falls far short of its expenses, he says.
"For someone to lose their insurance and Catholic Charities not be able to bill that insurance, it would really add to that deficit," Wortham says.
He says the organization is proactively working with clients who are reliant on Medicaid to ensure that they maintain their eligibility for the coverage.
Wortham says Catholic Charities partners with many Catholic hospitals and systems on programs. He welcomes any providers that overlap the organization's vast footprint to reach out for collaborations related to the Medicaid unwinding.
Prep work
Providence St. Joseph Health set up a steering team in fall 2021 to plan for the unwinding. Tue Nguyen, the system's director of patient outreach and financial sponsorship, says team members are from many
disciplines, including financial counseling, population health, communications and marketing, government relations, community health investment and physician enterprise. They have set up policies and best practices in advance of the unwinding
in hopes of minimizing its financial impact on patients and the system.

One of the team's strategies has been to build partnerships between the system's financial counselors, who are well-versed in Medicaid enrollment and qualifications, and its community health workers, who are on the frontlines in the rural and communities of color that are often most reliant on the public health insurance program.
At Providence ministries, the two groups are meeting virtually every other week to educate each other — the counselors discussing their resources and the community health workers sharing their outreach efforts.
The team is working on a variety of communications that will be deployed to reach patients before the unwinding begins. Some communications will be customized for enrollees by language and to point them to websites with information specific to the state in which they reside.
Nguyen says that because of the team's prep work, Providence is "very ready" for the start of the redeterminations.
Spinning plates
Slubowski says Trinity Health's preparations for the unwinding include identifying programs that can assist patients who might fall through the cracks. It is also readying an "education center" with
resources for staff, especially those at its safety net health centers, to understand and explain to patients the specifics of the redetermination process in their state.
Slubowski says the system's advocacy, well-being, community health, marketing and communication and revenue excellence teams are all playing a role in preparing care providers and patients for the unwinding.
"Our folks are nimble and they're doing their very best to keep the spinning plates going," he says. "But it's a challenge."
CHA offers toolkit to 'Protect What's Precious'
CHA is expanding the resources in its Medicaid Makes It Possible campaign to add free downloadable tools that member organizations can rebrand or co-brand and use to guide patients through the Medicaid eligibility redetermination process. That process has been on pause nationwide since the start of the pandemic but is set to restart April 1.
Josh Matejka, director of creative services at CHA, says the Protect What's Precious resources are designed to be patient-facing, with clear, concise messages.
One of the tools is a set of posters that have the address for the Medicaid-focused page on CHA's website and a QR code that, when scanned by a smartphone camera, links to Medicaid.gov, where users can access the websites of state agencies that are handing the reenrollment process. Postcard-size versions of the posters that can be used as handouts are also available. The posters are available in English and Spanish.
Ministry members can broadcast on their closed-circuit TV systems a CHA video with information about how patients can reenroll in Medicaid.
The toolkit also includes talking points on how to discuss the reenrollment process with patients. CHA will introduce the toolkit in a call from 1-1:45 p.m. ET, Jan. 25.
