DEBI PASLEY MS, RN
CHRISTUS Health Senior Vice President and Chief Nurse Executive
I became a nurse because I wanted to serve patients, and I became a nurse leader because I wanted to serve nurses. But never has a situation presented me more opportunities to do both than the COVID-19 pandemic.
In spring of 2020, as the pandemic escalated changes in our world, early directives from emergency management agencies and local and state governments moved to limit visitors in hospitals. Within days of shutdowns and other public health measures, local hospital leaders within CHRISTUS Health received these requests to prevent all but employees from being in our hospitals. Little did these agencies know the complications that would create.
CHRISTUS Health quickly recognized the inconsistency of isolating patients, who trusted us for their care, from their essential support persons and how that choice would keep us from the ability to fulfill our mission. Patients tell care providers who their essential support persons are. Generally, it's those who are closest to the patient who can provide physical and emotional support during and after illness.
But policies to keep patients' families and loved ones out of hospitals, intended to reduce infection spread, led to difficulties. Not only did these policies often cause fear and anxiety for our patients and their loved ones, they took a toll on our caregiving employees as well. In addition to the heightened workload while caring for patients who were alone, nurse ethicist Georgina Morley and her co-authors outlined in an article in the Hastings Center Report the impact of moral distress that grows from the absence of essential support persons in health care environments.1 The presence of loved ones has proven to improve mental status, decrease length of stay and improve safety in the acute care environment.
Not only that, but we received feedback from critical care physicians and employees that it was more difficult to relay the medical reality to families who could not be at the bedside and witness their loved ones' struggles. We realized we had clinical, ethical and mission-driven reasons to allow loved ones who provided patients with essential support into the facility, so we had to find a better way to provide care and support while maintaining a safe environment.
TEAM APPROACH TO COMMUNICATE WITH FAMILIES
There were times when we needed help. At the height of the surge, physicians, nurses and other clinicians couldn't always be there to ensure regular communication with anxious family members. Our highly trained teams were busy managing care and preventing death. That's why we developed a plan for patient care associates, our spiritual care team and others to manage the important task of open communication during the busiest of times. Each care team designed what would work for them based on their available resources. Even then, however, reevaluating protocols and expanding our visitor policy became an urgent need for our entire system.
NUANCED VISITOR POLICIES TO PREVENT ISOLATION
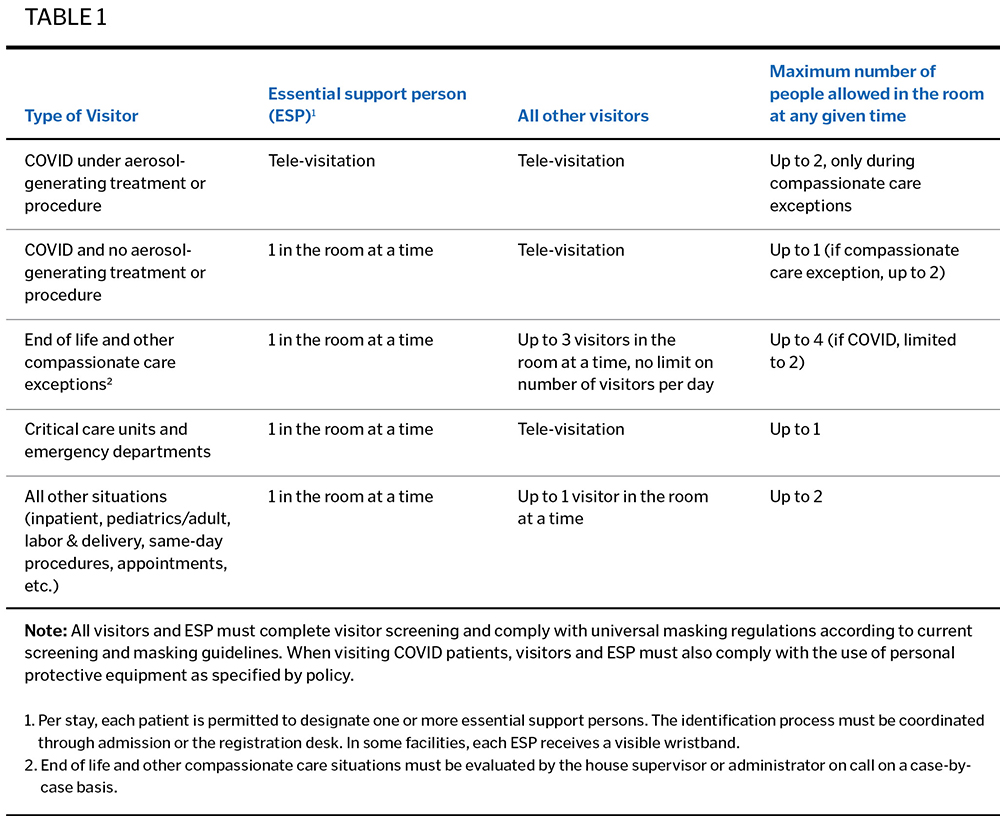
We engaged CHRISTUS Health's Advocacy team, which works on legislative matters, to evaluate state orders on the topic. We soon recognized that none of the executive orders in our states were absolute in those limitations. The wording around "essential support persons" gave us the flexibility to ensure safe support from key loved ones during hospital stays. This led us to categorize patients based on the nature of the care they were receiving. Life-changing events, such as birth and end of life, demanded more latitude. More high-risk situations, such as a COVID patient receiving aerosolizing procedures, required greater caution. CHRISTUS revised the guidance in its policies regarding the presence of essential support persons (Table 1).
Implementation of the guidelines was met with caution in some ministries. However, patient and caregiver feedback has reinforced the importance of advocating for our patients and families.
STAFF SHOW EXTRAORDINARY HEART
Family members rely on our comfort, something that our CHRISTUS nurses, like Betty Rutherford from Corpus Christi, Texas, fully realized during the pandemic when she cared for entire families devastated by last year's surge of the virus. She didn't just work at the top of her profession to prevent death. She worked to prevent suffering by being there for her patients when their families were not allowed inside the hospital hallways. She was with patients and then held family members when they lost loved ones. As her experience was replicated time and again, we began searching for a better way to ensure that no one we serve had to suffer in isolation. Critical care nurses like Nanette Foster from Shreveport, Louisiana, fought to save so many lives and to make sure no one would be forced to be alone. Spiritually and emotionally, it took a toll on all of us. That's why, as clinical leaders, we owe it to ourselves and others to make sure that we make family visits and communication the standard of exceptional care.
Many CHRISTUS employees experienced the myriad communication and visitation challenges wrought by COVID-19. Rosie Tijerina, who manages a CHRISTUS print shop, lost her 27-year-old grandson who was hospitalized an hour away from the nearest CHRISTUS facility. She spent weeks with the added stress of having to wait by the phone for terrible updates about her grandson until he succumbed to COVID and passed away.
Coordinating communication between family members and critical patients resulted in additional stress for our staff as well. Charge nurses would dress in protective gear and use laptops and cell phones to help loved ones say goodbye, many times over FaceTime. The family members had to watch via a screen as a mom or dad slept in a hospital bed. To witness them taking in the last moments of having a parent before they passed away changed everyone's perspective on the right and wrong way to treat those we serve. Isolation in health care should never be tolerated.
BALANCING NEEDS
While some were initially concerned about letting relatives or the support person into health care settings during the pandemic, we knew that we could keep our caregivers safe through the use of personal protective equipment (PPE). Our supply chain colleagues also secured an adequate supply of PPE to allow us to use it protect the essential support persons of our patients with COVID-19. We explained that enabling safe family presence is rooted in compassion, one of our core values. After all, healing is not always about physical restoration; it is also about spiritual and social repair. Allowing essential visitors to be with our patients allows mutual compassion between patients and family. We invited clinical leaders and front-line staff to evaluate what they would want for their own family members and the efficacy of our guidelines in stemming the spread of infection and COVID-19 within our facilities. In the end, it became clear that our mission, our patients and their families — as well as our associates and physicians — needed the support of visitors and essential support persons. We've implemented this expanded policy at all our U.S. CHRISTUS facilities and already are hearing that it has made a difference.
As a system with a calling to extend the healing ministry of Jesus Christ, it's easy to imagine Jesus working right alongside our care providers, sitting next to the beds of our patients and comforting their families. We've known Jesus has been here all along, and now we're glad to share that experience and that compassion with our visitors and support persons as well.
DEBI PASLEY is a system senior vice president and chief nurse executive for Irving, Texas-based CHRISTUS Health.
NOTE
- Georgina Morely et al., "Covid 19: Ethical Challenges for Nurses," Hastings Center Report 50, no. 3 (May 2020): 35-39, https://doi.org/10.1002/hast.1110.
