BY: MICHAEL S. KUSHNER and JOHN A. GALLAGHER, PhD
Catholic Organizations Should Evaluate Existing Methodologies
Mr. Kushner is vice president, compensation and benefits, and Dr. Gallagher is corporate director, ethics, Catholic Healthcare Partners, Cincinnati.
When it comes to defining and accurately quantifying community benefit, Catholic health care has led by example. The guidelines developed by the Catholic Health Association have been praised as a fair and accurate standard by members of Congress who examine this issue.1 Unfortunately, in our experience, there is no similarly clear direction on how a Catholic health care organization could calculate for its lowest-paid associates* a socially just wage that is consistent with Catholic social teaching.
CHP refers to its employees as "associates."
The fact that there is no guide for a socially just wage constitutes a tremendous opportunity for Catholic health care to differentiate itself from other-than-Catholic providers, and, at the same time, to give witness to some of the core theological tenets of the ministry. The authors' organization, Catholic Healthcare Partners (CHP), Cincinnati, has invested a good deal of time in consideration of this issue. In this article, we will:
- Make a quick review of Catholic social teaching
- Describe the efforts of CHP to calculate a socially just wage
- Suggest that Catholic health care create an inventory of currently used methodologies that are consistent with Catholic social teaching
Catholic Social Teaching
Catholic social teaching establishes a vision that Catholic health care organizations are to use in building model communities composed of individuals who flourish in both physical and spiritual health. Catholic social teaching also recognizes the individual's fundamental right to have basic needs met, including food, shelter, clothing, and health care. In Laborem Exercens, Pope John Paul II describes just remuneration for work as "remuneration which will suffice for establishing and properly maintaining a family and for providing security for the future."2 The pope goes on to say that a worker's total compensation should include health insurance as well as a pension and insurance for old age. Unfortunately, however, these general directives, important though they are, leave employers without clear guidelines for their wage and benefit packages.
Of course, when it comes to compensation and benefit programs, interpretation of the social teachings varies. For example, some organizations focus on the pay issue; others focus on benefits such as health care coverage or pensions; and still others look to create developmental opportunities for their lowest-paid employees.
Wages
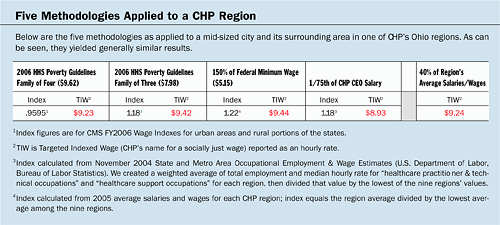
At CHP, we examined the following methodologies to calculate a socially just wage. Each, we found, has its advantages and disadvantages.
- HHS Poverty Guidelines and CMS Wage Indexes (Method 1) This methodology multiplies the U.S. Department of Health and Human Services (HHS) poverty guidelines for a family of four by the Centers for Medicare and Medicaid Service (CMS) wage indexes for urban areas and rural portions of states. This method allows the wage to reflect local market conditions.
- HHS Guidelines and CMS Wage Indexes (Method 2) This methodology multiplies the HHS guidelines for a family of three by the CMS wage indexes. The only difference from the first method involves the family size. After reviewing CHP's medical enrollment data for more than 7,000 associates with family coverage, we determined that average family size (including the associate him- or herself) was 3.08 members.
- Federal Minimum Wage We considered setting CHP's entry-level wage at 150 percent of the federal minimum wage, but decided that this methodology could be unstable since a legislative increase could dramatically alter this number very quickly.
- Fraction of the CEO's Salary We also considered calculating the targeted indexed wage as a fraction of the CEO's base pay. The fraction we had in mind was 1/75.
- Percentage of Regions' Average Base Pay And, finally, we considered using 40 percent of each of our nine regions' average base salaries as the targeted index wage for that region.
In the end, we decided to use the first guideline (HHS Guidelines and CMS Wage Indexes [Method 1]) because it is premised on a family wage, rather than on the individual worker, which is the traditional American model. The CMS wage index allowed us to account for regional differences and thus the cost of living within different communities served by CHP. Most of the methodologies we considered were modified by an index that allowed for regional differences in market conditions. The indexes used were either the CMS wage index, an index based on the U.S. Bureau of Labor Statistics' State and Metro Area Occupational Employment and Wage Estimates, or one based on the average salaries for each of our regions.
See the Box for a sample of the many combinations of methodologies we considered.
If, when CHP implemented the methodology in 2003, we had moved all eligible associates to the "targeted index wage" (TIW), the cost would have been $800,000. Approximately 1,600 (4 percent of CHP's 39,571 associates) would have moved to the target wage. To date, six of CHP's nine regions have fully implemented the TIW; the remaining three are balancing financial considerations. The cost of maintaining this wage, even as the index increases, is minimal and would probably have been less than 15 percent of the original annual cost of $800,000 year, if everyone eligible had been moved in 2003.
Benefits
CHP has made progress in the area of benefits coverage. In the past, because of our decentralized operating model, we merely collected and reported information during the annual open enrollment for medical benefits. We noted each year that about 21 percent of our 23,000 eligible associates declined coverage. Of those who declined it, 51 percent said they had other coverage; 2 percent said they could not afford it, or didn't want it, or had simply missed open enrollment; and 47 percent declined the coverage but gave no explanation for doing so. We believe that many who declined coverage without giving an explanation did so because they either 1) were too proud to admit that they couldn't afford it; or 2) saw such questions as an invasion of their privacy.
This year, CHP is piloting a program intended to provide associates greater access to coverage. The program's foundation involves communicating to associates the fact that, by disclosing personal information about why they have declined health coverage, they may get the coverage they need. Associates who do disclose that they are interested in coverage but cannot afford it will be directed to financial counselors in our business office. The counselors will help them obtain insurance based on the family need, through either the CHP associate plan or external sources such as Medicaid.
CHP has also looked at the pension area. Although we have spent time studying appropriate income-replacement ratios from all sources — CHP pension, Social Security, and personal savings — due to the regulatory complexities and the number of plans that we have within our system this will be the last area we focus on. Our current thinking is that, after a 30-year career, an associate will need a combination of CHP pension, Social Security benefits, and personal savings replacing approximately 70 percent of his or her pre-retirement income in order to maintain quality of life during retirement.
Associate Development
Finally, CHP has developed a program in our northern region to encourage associates who are at the lowest salary level to pursue advancement. In fact, the TIW is used to determine eligibility for the program, which we call "Visions." For associates who want to advance, Visions offers vocational evaluation, career guidance, job shadowing, counseling, career assessment tools, educational consultation, and referral to community resources. The program also pays tuition and book costs for those who enroll in classes. Visions has been so successful that it is currently being extended throughout the system.
Why Compare Methodologies?
The authors believe that Catholic health care should collect and evaluate the methodologies being used today in the ministry to calculate a socially just wage. By doing so, the ministry would be performing a public service analogous to its publication of A Guide for Planning and Reporting Community Benefit. Congress has looked to the ministry's leadership in this area, as well as in others. A careful inventory and evaluation of socially-just-wage methods could give the ministry a competitive advantage in recruitment and retention of staff, and also enhance our reputation in our communities and among unions. Best of all, it would create a range of options that are consistent with Catholic social teachings.
Much of the groundwork for such an evaluation has already been done by an ad hoc group, the Senior Human Resource Executives of Large Catholic Health Systems. The members of this group developed a statement of principles (see Box), which they published in Health Progress five years ago.3 These principles can form the foundation for determining if a methodology is consistent with Catholic social teaching.
One might ask: Why collect and evaluate methodologies rather than simply developing a standard method for all Catholic health care to use? The answer involves antitrust issues. According to John Cusack, an experienced antitrust attorney who specializes in health care with Drinker Biddle Gardner Carton, Chicago, "It is proper for ministries to consider appropriate living wages based on methodologies that consider poverty levels, cost of living statistics, and competitive wages in light of the significance of their mission; as well as the papal encyclicals. Yet there should not be a set formula; each salary should be arrived at independently by each ministry; and each ministry should, according to its mission, err on the side of generosity. This can be broadly referred to as 'a proper methodology.' In no circumstance should wages of two or more ministries be arrived at through any agreement, express or implied."4
Another concern has to do with effectively implementing and maintaining a living wage program in a union environment. To best manage any potential issue, Catholic health care would need to incorporate language into collective bargaining agreements that allowed the hospital in question to unilaterally increase wages for the lowest wage earners. According to Bruce Stickler, a health care labor and employment attorney with the same Chicago law firm, "Socially just wages in keeping with a ministry's mission can be provided in unionized as well as nonunion settings. It is incumbent upon providers to be strategic and flexible in setting living wages and increasing wages mid-term when faced with the limitations of collective bargaining agreements. This requires careful planning to avoid the pitfalls of unilateral actions that run afoul of labor laws."5
The Catholic health ministry must take action to fulfill its heritage while, at the same time, considering the stewardship of resources to create the right balance. The authors hope that this brief article will be the beginning of a concerted discussion of this issue in the ministry.
NOTES
- Catholic Health Association, A Guide for Planning and Reporting Community Benefit, Washington, DC, 2006.
- Pope John Paul II, Laborem Exercens, 1981, section 19.
- Jeffrey W. Hamlin, "A 'Just Wage': More than Dollars," Health Progress, March-April 2002, pp. 43-45, 59.
- John Cusack, e-mail of May 2007.
- Bruce Stickler, e-mail of May 2007.
Principles Concerning the Just Wage
Principle I Catholic health care organizations should establish plans to move them toward a just wage. Such plans should include different levels of remediation and skills development and should consider increasing pay to or above the prevailing market. They should take account of government societal programs already in place and provide for periodic assessment of their impact on all facets of the employee-employer relationship.
Principle II Providing a just wage is a societal issue as well as an individual employer issue. In cases where society has already established programs, Catholic organizations should inform workers about their eligibility concerning benefits (the Family Medical Leave Act or the earned income credit, for example) and help workers gain access to them.
Principle III A wage set at the federal poverty level is not a living wage because it does not consider household income or family composition (number, ages, sex), which are predominant factors in creation of a just wage.
Principle IV Competitive pay rates and market position can significantly challenge a Catholic organization's ability to provide just wages. At least in the case of lower-paid workers, however, such organizations should pay wages at or above prevailing market rates and provide benefits that support family needs and development of the worker.
Principle V Employers have an obligation to help unskilled and semiskilled employees raise their skill level and thereby enhance their productivity and marketability. Employees, on the other hand, have a responsibility to seek out and take part in skills training and job enhancement initiatives.
Principle VI Most eligible workers and their families receive health insurance coverage through employers. Catholic organizations should subsidize health coverage for their low-income workers.
Principle VII Catholic organizations' benefit packages must include affordable health care (subsidized for low-income workers), regular rest, adequate retirement income, workers compensation, disability protection, and safety in the workplace.
— Senior Human Resources Executives of Large Catholic Health Systems
(Health Progress, March-April, 2002, p. 44)
