BY: GORDON HILSMAN, DMin, and JUAN IREGUI, MD
Mr. Hilsman is manager, clinical pastoral education, St. Joseph Medical Center, and Dr. Iregui is an ethicist and palliative care physician, Franciscan Health System, both in Tacoma, Wash.
Quis custodes ipsos custodiet?
(Who takes care of those who take care?)
The basic definition of the word "catholic" as "universal" suggests, in the context of Catholic health care, a sincere effort to care for all people, certainly those within one's sphere of influence. Clearly, it follows that the mission of Catholic health care includes finding ways to care not only for patients within our institutions, but also for the souls of those who function as the basis of all health care: the medical practitioners themselves.
For the most part, however, institutional relationships with physicians have revolved around negotiations related to their need for medical equipment, practice space and other professional amenities, with support for physicians focused mostly on meeting those material needs. The jostling for power between medical practitioners and administrators that inevitably ensues has traditionally contributed to distance between the two groups. Meanwhile, even in Catholic health care systems, physicians' emotional and spiritual needs often go unmet in the workplace.
As Catholic institutions seek to develop formation programs aimed at bringing physicians' values into alignment with the existing health care culture, they may find that physician self-care and personal integration first need to be addressed. When formation is initiated by others, from without, it can easily feel subtly coercive. True personal integration, on the other hand, happens from within, through engaging with others in a process of mutually exploring and experiencing personal vulnerability as well as personal power.
If Catholic health care systems are to live up to their mission of caring for whole persons, it will be important to find ways to nurture physicians' souls — or perhaps better, to help physicians nurture one another, for the benefit of their emotional and spiritual needs.
Personal Integration: Mind, Body, Spirit
Who teaches physicians how to care for their own spirits and souls? Medical schools generally do not. Regrettably, neither do more experienced colleagues.1 For example, studies of oncologists suggest that nearly one-third experience significant career burnout, emotional exhaustion, depersonalization and a sense of low personal accomplishment. A large number also believe their family and personal lives suffer because of their chosen career.2 Br. Daniel Sulmasy, OFM, MD, Ph.D., summarizes the problem this way: "Unless health care professionals become aware of their own fallibility and vulnerability, they will make serious mistakes or begin to take out their angers and frustrations on the patients, or both."3 Indeed, wise and intentional shaping of a health care professional's personal development is a necessary component of both patient welfare and professional satisfaction in any health care profession.
The process of personal integration can be illustrated by the three intertwining circles in Figure 1. The human functions of thinking, doing, speaking and valuing emerge at different times during childhood and develop separately from one another. As result, they need to be pulled together as one matures. In the clinical practice of medicine, as in other fields that rely primarily on intellect, the spirit/soul circle often remains stunted, smaller than thinking and doing, functions that occupy most of a doctor's day. The life project of integration requires a specific context and engagement in certain types of endeavors from which many of us protect ourselves in favor of external success.
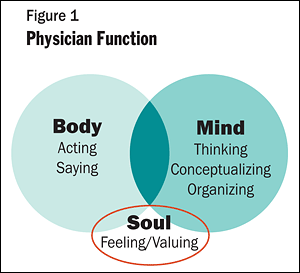 As integration evolves, humans become better at recognizing and accepting their vulnerability and incorporating soul or spirit — that is, emotions and values — into their decisions and actions. By contrast, in a person lacking integration, feelings and values may be compartmentalized. But as a professional becomes more comfortable with vulnerability, and allows emotions and values to influence decisions and actions, the circles shown in Figure 1 gradually move together, so that in a highly integrated person, they converge — though rarely perfectly — into a single circle. Body, mind and spirit/soul gradually coalesce into a more integrative whole.
As integration evolves, humans become better at recognizing and accepting their vulnerability and incorporating soul or spirit — that is, emotions and values — into their decisions and actions. By contrast, in a person lacking integration, feelings and values may be compartmentalized. But as a professional becomes more comfortable with vulnerability, and allows emotions and values to influence decisions and actions, the circles shown in Figure 1 gradually move together, so that in a highly integrated person, they converge — though rarely perfectly — into a single circle. Body, mind and spirit/soul gradually coalesce into a more integrative whole.
The potential for shared mutual vulnerability to support healing and personal integration became known during the 20th century, first through the success of Alcoholics Anonymous, then through a plethora of self-help groups that followed. Further, the healing benefits of openly disclosing emotional responses to serious illness have been clearly documented.4 When people connect on a significant level, on the level of spirit, or soul, hope is generated in some natural way that as yet cannot be explained. The term "soul flow," referring to this deep connectedness, suggests a spiritual perspective that need not be expressed in specifically religious terms.
Similarly, in the field of pastoral care, the formative educational model known as clinical pastoral education features interpersonal openness in small, facilitated group settings. Students in this type of educational program soon experience the enormous benefits, both personally and educationally, of shared vulnerability as they look closely and communally at their ministry practice.5
Romantic intimacy offers an analogy. It flourishes only when mutual vulnerability is fostered and maintained. Pulled into relationship by the highly emotional and ever-mysterious experience of falling in love, human beings are invariably challenged to develop skills and virtues required to sustain relational satisfaction and mutual fulfillment by a unique combination of emotional connectedness, thoughtful acquiescence and self-valuing assertiveness.6
In a physician's professional world, that healing power of shared mutual vulnerability is too often unavailable. The personal and professional vulnerability inherent in their roles, which may require them to make life-significant decisions several times a day, is perhaps assumed among them. But it is rarely shared in any healthy, open way. Many physicians hesitate to talk with one another about the ways their practice affects them personally. Institutions generally lack a forum for it, and medical training rarely provides for this important dimension of a physician's work.
Developing a Model for Physicians
In developing a program for physicians at Franciscan Health System, we postulated that if medical practitioners could be persuaded to come together in a small group, in a setting encouraging emotional disclosure about events of the day, they would quickly engage one another to their mutual benefit. We determined that essential elements would include a confidentiality agreement and an intellectual component in the form of background information on theories of personal integration. We also believed an experienced group facilitator would be an asset.
For this pilot project, the four physicians participating in the Franciscan Health System Hospice and Palliative Care provided a logical starting group. They were already meeting regularly to discuss cases, and some of them easily acknowledged that their emotional reactions to those cases were assumed to be out of bounds for discussion. Juan Iregui, MD, joined co-author Gordon Hilsman, manager of clinical pastoral education, in inviting Iregui's three colleagues and other physicians they thought might enjoy the adventure. The group, consisting of three men and two women, began meeting in October 2007.
The agreement was to meet every other week for an hour at 4 p.m. in a comfortable room of the clinical pastoral education program. The setting afforded members a neutral, quiet and confidential space. The group was given no name. We explained the purpose of the group was to provide a forum in which medical practitioners could talk together about how their practice had affected them recently, preferably that day. Philosophizing would be allowed to a degree, but the group's specific purpose would be to discuss case data in the context of the emotional effects of the situation on the physician. The clinical pastoral education supervisor, the only non-medical professional in the group, served as facilitator, striving to elicit the affective component of the interactions amid the more readily offered medical data.
Putting the Model into Practice
One initial member discovered that an unfortunate political situation existed with another member and attended only three meetings. Another postponed her regular participation after four sessions due to a family situation. In the 12th meeting, the group began to include two interested advanced registered nurse practitioners.
Initial meetings focused on the reasons physicians avoid sharing the aspects of their practice that make them vulnerable, i.e., how they are affected by the tragic, infuriating, sad and frustrating events that often make up their days. Stories abounded. Each member was also encouraged to tell at least one story illustrating how he or she learned that sharing the emotional aspect of medical care is, from the standpoint of personal development and patient welfare, a healthier approach than "stoically stuffing and stonewalling."
After six meetings, some group members expressed interest in exploring a theoretical basis for the group's work. They were seeking some conceptual framework in which to ground and bolster their growing mutual vulnerability. Had such a framework been presented before the group experienced significant intimate interaction among themselves, it is likely the presentation would have fallen flat.
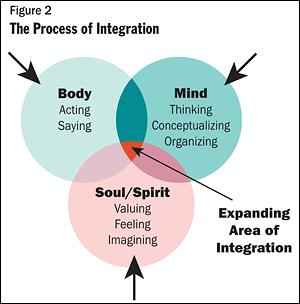 The facilitator obliged. He used Figure 2 in presenting material on the topic of personal integration as it relates to shared vulnerability in such programs as those that support healing in addiction recovery and bereavement, and in such professional settings as psychotherapy and clinical supervision. The general assertion was that endeavors that compel us to connect authentically with our deepest values (soul or spirit) and to use all facets of being human —cognition, affect and behavior (mind, body and spirit) — are those most likely to help humans consolidate their personalities and heal their spiritual wounds. Examples and experiences from members of the group were easily elicited to solidify the learning.
The facilitator obliged. He used Figure 2 in presenting material on the topic of personal integration as it relates to shared vulnerability in such programs as those that support healing in addiction recovery and bereavement, and in such professional settings as psychotherapy and clinical supervision. The general assertion was that endeavors that compel us to connect authentically with our deepest values (soul or spirit) and to use all facets of being human —cognition, affect and behavior (mind, body and spirit) — are those most likely to help humans consolidate their personalities and heal their spiritual wounds. Examples and experiences from members of the group were easily elicited to solidify the learning.
Subsequently, the group agreed to divide the sessions into two, one to continue the "today's events" section, and another to brainstorm about various related topics. The list of topics included grieving, recovery, religious heritage, dimensions of physician vulnerability, and the notion of "spiritual skill."
In May 2008, a decision was made to expand the group. Concerns over losing what had been gained gave way to a willingness to expand in order to extend the potential benefit to others. Efforts would be made to maintain the original membership as a separate small group.
An e-mail was sent to about 1,000 physicians, physician assistants and advanced registered nurse practitioners working in or admitting patients to facilities within the Franciscan Health System. Ten potential new members showed interest, and a few began to meet with the group.
Noting Areas Needing Work
As this project has unfolded, three types of results can be described: simple observation, anecdotal evidence from group members, and initial results of a research survey.
1) Observation
Group cohesion is in itself a measure of success. Attendance of those initially committed to the group has run about 80 percent. Given that busy professionals are disinclined to participate in endeavors that hold little interest for them, such high attendance is exceptional for professionals who often cannot finish their days on time.
2) Anecdotal Indications
Although bold emotional disclosure from physicians about their practice rarely happens in a context of intentional processing, in the first 10 months of group meetings, the disclosures have been profound. In the first meeting, members described experiences that demonstrated the need for such a group. One woman related a recent event in which she was kicked to the floor by a minimally cognitive patient while family members stood by and said nothing. She wondered: Are physicians not human too? Another, with tears in her eyes, described her reaction to working furiously one day to save the facility from a disastrous lawsuit, then receiving no mention of her efforts from administration.
In subsequent stories, a member described a situation in which a group of three watched in helpless silence for five minutes as a 58-year-old man bled to death, despite aggressive efforts to save him, following placement of a nasopharyngeal airway by a highly experienced respiratory therapist. The member who told the story eventually applied the word "impotent" to his feelings during that seemingly unending time.
After the topic of grieving was opened up, two physicians shared, in ways they reported they never had before, stories of losing their fathers to death before they were 10 years old. In another session, one member spoke of finding herself ill and in the hospital awaiting X-rays beside a young son of a patient she had cared for in hospice. In a wheelchair himself, he cared for her so tenderly that she was brought to tears. Having experienced a similar response from one of her own sons, this group member found herself more open to receiving care from members of the group, in contrast to her previous tendency to wear herself out in caring for others, including family members and friends.
At one time or another, all but one group member has cried.
3) Research
In order to provide a more objective appraisal of members' progress in the group — some measure of how professionals had grown to care more for themselves and to allow others to care for them — the facilitator developed a survey of "spiritual skills" to be given to new members, with the intention of repeating it a year later. The instrument includes 101 human behaviors associated with nurturing one's human spirit as well as that of others. It was given to enough nurses, chaplains, clinical pastoral educators and hospital managers to allow for comparisons to physician results over time.7
In the interest of providing resources related to in skill areas of interest to group members, strong and weak areas were identified in the survey and sorted by profession. Initial observations from the results showed that physicians see themselves as exceptionally good at eye contact and at behaviors that involve protecting people, and most in need of improvement in regard to their ability to rest when advisable, to ask for what they want, to tune in to others' emotions, to affirm themselves, and to maintain a hobby. The areas showing need for improvement will be developed into future topics for the group.
Evaluating Preliminary Results
What this facilitator and a small group of professionals are learning is slowly unfolding. The consensus of group members overall is that medical practitioners benefit highly when they allow themselves to enter an arena of mutual vulnerability around events related to their recent medical practice.
Experience to this point indicates that a combination of group time without an agenda, combined with group time for discussion of specific, relevant topics, offers the most success. Participants have found elements of sharply focused theory help them become more facile at relating with one another in depth and in integrating the emotional side of their experience more fully into their practice. Physicians will not go far down the lane of mutual vulnerability without some theory on which to base their openness.
These preliminary learnings suggest the following three benefits of offering such programs to medical professionals in Catholic health facilities:
1) Practitioner Integration
Integration of mind, body and spirit will grow when facilitated by open sharing that encourages mutual vulnerability. In-depth personal exchanges in small groups, such as the one operating in the Franciscan Health System, can play a significant role to that end, thereby improving the health and well-being of medical professionals and helping to maintain and foster values beyond the political and the financial. This can benefit individuals already practicing in medical fields as well as those newly entering them.
2) Physician Retention
Retention is likely to improve as practitioners find greater meaning in their work and learn to support one another on an emotional level. As medical professionals become better at sharing their own stories among themselves, they are more likely to elicit personal sharing from the people for whom they care. This will benefit both groups and is likely to increase the satisfaction professionals find in their work.
3) Mission
The mission of Catholic health care will be strengthened, in the sense that the mission includes contributing to the human care of medical practitioners and to their emotional support of one another. This is particularly important in an environment of rapid changes in the field — an environment in which professionals' frustrations are often on the rise. Although the word "catholic" has not yet been specifically applied to the group's work at St. Francis, the basic meaning of the term, "universal," suggests that projects such as the one described in this article, are not only implicitly spiritual but are also eminently well-suited to Catholic institutions dedicated to healing in the fullest, most universal, sense of the word.
Quis custodes? Ipsos custodient!
(Who cares? They care for one another!)
NOTES
- F. Stiefel, "Support of the Supporters," Support Care Cancer 16 (2008): 123-126.
- Tait Shanafelt, et al., "Shaping Your Career to Maximize Personal Satisfaction in the Practice of Oncology," Journal of Clinical Oncology 24, no. 24 (2006): 4020-4026.
- Daniel P. Sulmasy, The Healer's Calling (Mahwah, N.J.: Paulist Press, 1997), 164.
- M. Soledad Cepeda, et al, "Emotional Disclosure Through Patient Narrative May Improve Pain and Wellbeing: Results of a Randomized Controlled Trial in Patients with Cancer Pain," Journal of Pain and Symptom Management 35, no. 6 (June 2008): 623-630.
- Read the stated values of the Association for Clinical Pastoral Education at www.acpe.edu.
- Gordon J. Hilsman, Intimate Spirituality: The Catholic Way of Love and Sex (Lanham, Md.: Sheed & Ward, 2007), 15-46.
- Iregui and Hilsman presented initial data of the study at the national conference of the Association of Professional Chaplains in Pittsburgh in 2008. Final benchmark data is scheduled to be presented in Orlando, Fla., in February 2009, at the first Spiritual Care Collaborative meeting of the six primary pastoral care organizations in North America.
