BY: JOAN ELLIS BEGLINGER, RN, MSN, MBA
Ms. Beglinger is vice president, patient services, St. Marys Hospital Medical Center, Madison, WI.
A Wisconsin Hospital and Its Nurses Have Discovered the Power of Partnership
There is an increasing crisis in health care related to current and projected shortages in many of the disciplines essential to the provision of services. None has received greater public notice, nor generated more concern, than the nursing shortage. Those who manage health care facilities and systems increasingly implement desperate strategies—many of which exacerbate the crisis rather than ease it—largely because they understand neither the crisis' etiology nor the fundamental changes that will have to occur in most organizations if we are to see the situation turned around.
Amidst the crisis, however, there are nursing departments that are thriving, producing the results that all health care organizations seek. They enjoy excellent clinical outcomes and high patient and provider satisfaction. Turnover among nurses is low; operating margins are healthy. These departments must serve as prototypes for the future. Their approach must be studied and replicated. At such organizations, nurses are engaged in every facet of operations and have emerged as their organization's unexpected business partners. St. Marys Hospital Medical Center in Madison, WI, is one such organization.
A Portrait of Success
"Ownership" of an organization's services, by those who provide them, has been
demonstrated to be the most significant driver of the organization's success.
What is "ownership" and how is it achieved? Ownership, in this context, can
best be understood by contemplating the behaviors and attitudes of a partner
in any business. The partner is intellectually and emotionally committed to
acting in a way that will best advance the purposes of the enterprise at all
times. The partner not only feels free to act in a way that will be right for
the organization; he or she feels obligated to do so. Belief and investment
in the organization's mission is characteristic of ownership. A sense of ownership,
on the part of those who do the organization's work, is an essential characteristic
of success.
St. Marys' nursing department—called the Nursing Organization—has been identified as a model of success in turbulent times. Success can be substantiated by a review of the department's history, a summary of its results, and a discussion of lessons learned.
The Transformation
In 1991 the Nursing Organization began a deliberate process of transforming
itself from a traditional hierarchy into a shared-governance model. The latter
model is characterized by relationships between managers and staff that are
partnerships rather than the parent-child relationships found in traditional
hierarchies. In the shared-governance model, accountability for decision making
is located in multiple places throughout the organization, rather than concentrated
"at the top."
The shared-governance model is highly compatible with the Catholic principle of subsidiarity. Decision making is shared, which means that those with the most expertise in a given area are vested with the decisions in that area. Members of the clinical staff assume accountability for issues related to defining clinical practice, managing and improving the quality of that practice, and ensuring the competence of the practitioners. The clinical staff manages issues related to clinical practice. Managers manage resources and an environment intended to support excellence in clinical practice. This model is clearly differentiated from the traditional hierarchy in which management holds the final decision-making authority on all issues (whether or not it is competent to do so).
By 1994 shared decision making had been completely implemented at St. Marys, and by 2001 the transformation of the Nursing Organization had matured. The department was producing uncommon results consistently—and doing so in an environment that was proving disastrous for many other health care facilities. St. Marys' results were a byproduct of its nurses' strong sense of engagement in, and ownership of, the hospital's mission and strategy. The nursing department has responded to ever-growing demands for care without hiring agency nurses, mandating overtime, or paying "sign-on" bonuses or extra shift premiums. St. Marys' nurses view the provision of nursing care to patients as their responsibility and they collaborate with management to ensure that end. In return, they are involved in all aspects of the medical center's decision making, from development of the strategic plan to product selection to budget planning.
In 2002 the St. Marys nursing department became the 50th to receive the American Nurses Credentialing Center's Magnet Recognition* and, as a member of SSM Health Care, shared with that system's other members the Malcolm Baldrige National Quality Award. (SSM Health Care was the first health care organization to be thus honored.) The success of St. Marys' Nursing Organization had been identified by SSM Health Care as a "best practice," and a strategic imperative for organization-wide replication and was cited in the Baldrige application as such.
The Results
Clinical outcomes at St. Marys have been consistently excellent, with a focus
on continuous improvement. Interdisciplinary teams consistently evaluate and
improve practice against the best available evidence and benchmark against "best
practices" to ensure continued excellence.
Patient satisfaction is consistently high and is managed by those who provide the services. Satisfaction data are disseminated to the clinical staff monthly to provide them the information they need for improvement initiatives.
Experience has shown that it is only through satisfied employees that a health care facility can hope to have satisfied patients. Because this is so, St. Marys' Nursing Organization focuses on creating a satisfying practice environment in which nurses can feel good about their work. In a 2002 employee satisfaction survey, St. Marys' nurses scored higher than the survey's "best practice" (the top 10 percent of 455,000 health care employees in the selected vendor's data base) in three critical dimensions: overall job satisfaction, belief in the organization's concern for patient care, and belief in its strategy and mission (Table 1).

A close look at one question on the satisfaction survey reveals all one needs to know about why there is a nursing shortage. To the statement, "If I was in need of medical care, I would want to be treated at this organization," 91 percent of St. Marys' nurses responded "Agree" or "Strongly agree." Of the remainder, 8 percent were neutral and 1 percent disagreed (Table 2). Contrast this response with an American Nurses Association survey whose results were reported in 2001.1 In it, nearly 7,200 nurses were asked: "Would you feel confident having someone close to you receive care in the facility where you work?" Only 51 percent of nurses responded "yes," while 41.5 percent said "no." In far too many settings, our nation has created unworkable practice environments in which nurses do not believe they can deliver appropriate care.

The quality of nursing care in a hospital is often cited as a major driver in a physician's choice of facilities in which to practice. The 2002 physician satisfaction survey at St. Marys resulted in high marks on questions about nursing quality (Table 3). In that survey, the only question receiving a score of less than 90 percent was one that dealt with the nursing staff's training and skills. Written comments accompanying the survey remarked on the observation that an especially large number of novice nurses had entered the environment at the same time expert nurses were retiring. St. Marys has responded to this "thinning" of expertise with an entirely revamped orientation designed to provide additional structure and support for the novice nurse.

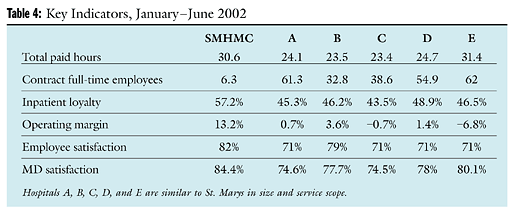
A reputation for excellence, a practice environment that is managed by the clinical practitioners, and a collegial relationship between management and staff have resulted in a turnover rate for nurses that is less than half of the national average, which in 2000 was more than 20 percent.2 Whereas the national vacancy rate for nurses is more than 10 percent, St. Marys' rate is about 3 percent. Meanwhile, St. Marys' operating margin is consistently far above national averages (Table 4).
Essential Elements of Success
St. Marys' leaders have identified five elements as essential to the success
of the Nursing Organization's professional practice environment.
Changing the Organizational Structure The structure of an organization is a map with which one can track accountability for actions taken. Ambiguity about who owns which decisions is the enemy of effective shared decision making. However, through an organizational design that supports shared decision making, roles are differentiated, skill-building needs are clarified, and behavioral changes are driven. Today, St. Marys' Nursing Organization has a very flat management structure, consisting only of the vice president of patient services and a unit director for each of the hospital's 18 nursing units. Since managers do not make all of the department's decisions, fewer managers are needed. This structure allows the department to focus the majority of its resources on patient care.
Broadly Sharing Information Sharing information to create a "big picture" context for all employees has proven to be an incredibly powerful tool. Accountants cannot be transformed into clinicians, but clinicians can certainly develop enough business savvy to help manage the hospital through the daily services they provide. At St. Marys, everything is shared with staff and is translated, when necessary, into terminology that is understood. Staff members see the monthly income statements and activity levels. They are educated about legislative measures (such as the Balanced Budget Act of 1997), industry trends, the competitive market, and St. Marys' strategic priorities. It is clear that having access to all available information is the key to gaining employee support for hospital initiatives.
Keeping Patients the No. 1 Priority Nothing is more important than ensuring that patients are always the organization's top priority. All health care facilities say they seek excellence in patient care; too often, however, money seems to drive decisions at the expense of patient care. Nurses in such facilities are asked, for example, to take on unreasonable assignments. This is the major reason so many nurses say they would be uncomfortable having loved ones cared for in their own hospitals. The perceived inconsistency between administrative words and actions has created tremendous cynicism in many organizations. Cynicism, perhaps more than any other factor, is death to organizations.
At St. Marys, the vice president of patient services spends one day each month in scrubs on a unit with staff. This enables her to make first-hand assessments of what staff members are being asked to do, and to stay in touch with how the demands for patient care are changing. In this way, a visible, engaged administration participates in ongoing discussion of the realities of patient care and planning for what can reasonably be done to ensure excellence in it. St. Marys' administration believes in observing at first hand the impact of administrative decisions on patient care. This has proven to be a very positive force in forging a positive relationship between management and staff, ensuring that concern for patients is a shared commitment.
Investing in the Skill Development of Management and Staff Few people working in hospitals today, whether they are staff members or managers, have the skills necessary to function effectively in a shared decision-making model. The traditional hierarchy comprises bosses and workers, and the relationship is often like that between parents and children. If a shared decision-making model is to succeed, very significant behavior changes are required of both managers and staff. Staff members must learn the meaning of "ownership," become systems thinkers, and learn how to make changes effectively. Managers (including administrators) must learn how to abandon "command and control" behavior and also learn how to facilitate a system of care, how to support staff development, and how to engage in self-development at the same time. To underestimate or underinvest in the amount of behavioral change required of all involved is to fail.
Budgeting the Necessary Resources Effective implementation of a shared decision-making model requires time and money. It is essential that time in decision-making groups (whether developing care pathways, working on quality improvement initiatives, or participating in peer review) be understood as real work and that it no longer be labeled "nonproductive" time. The premise of St. Marys' Nursing Organization is that investment in nurses produces real business results. Time spent on shared governance activities, plus conference time (budgeted at 16 hours per nursing organization employee) constitutes just 2.6 percent of the nursing budget.
Investing in the ongoing development of an organization's members is a critical component of the organization's continued success. Why do some organizations, when trying to save money, decimate their education budgets before making cuts in other places? Would any health care organization really want to have on staff, for example, cardiologists who do not attend national meetings or keep up with the medical literature? Why, then, should an organization want to have other clinical practitioners functioning at less than state-of-the-art levels? In health care, where the scientific evidence changes constantly, continuous education is not a luxury—it is a necessity. At St. Marys, the nursing education budget, which has grown consistently over the years, is managed by the clinical staff itself and has paid immeasurable dividends.
The Nursing Shortage
Our nation's agenda—which includes balancing the federal budget, eliminating
deficit spending, and reducing spending on health care—is on a collision course
with the realties of health care, which include increased demand from an aging,
chronically ill populace; increased costs (including labor, pharmaceuticals,
and technology); and decreasing reimbursement. Perhaps one of the greatest myths
perpetuated on the U.S. public is the notion we will someday spend less
on health care. There are three key reasons why this is so:
- The nation's population is aging ("baby boomers" will start becoming senior citizens in 2011).
- Older people require more health care, including acute services, than younger people.
- The cost of technology, already very high, keeps increasing.
Perhaps the greatest driver of the cost of care, however, is one seldom discussed: our reluctance to ration care, particularly on the basis of age. Walk through any intensive care unit and you will learn that heart surgery is routinely done on octogenarians and that premature infants on the brink of viability receive aggressive intervention. These decisions—about what to do, to whom, and for how long—are matters left strictly to patients and their physicians. As long as this is the case (and there is no evidence that it will change soon) the cost of care will continue to climb.
So the idea that we will someday spend less on health care is fantasy. Even so, the pressure to do so is very real. This pressure has been the catalyst for many of the problems in health care today—most prominently, the nursing shortage. Consider the contention that the single most significant factor in the creation of that shortage has been administrative responses to decreased reimbursement to hospitals. Many hospital administrators find this a stinging allegation. Still, it is time to come to grips with the fact that many hospitals have created unworkable practice environments.
Surveys of nurses tell us they are overworked, undervalued, and underpaid. Nurses believe that quality in their hospitals has declined. They have inadequate time to spend with their patients. They know that temporary help is diminishing the quality of care.
Too often, a lack of funds is cited as the rationale for decisions that have slowly dismantled an organization's ability to take good care of patients. The question begs to be asked: What is the cost of hiring agency staff, employing consultants who sell quick fixes, high turnover, union organizing efforts, poor outcomes associated with inadequate staffing, and low patient satisfaction/loyalty? How is the money that hospitals "don't have" being spent?
Understanding the Work
A significant contributing factor in the nursing shortage is the fact that
those who make decisions—especially decisions affecting a staff's ability to
do the work— poorly understand the work of nursing. The perception, held by
administrators who have no clinical experience themselves, of what nurses do
is often grossly inaccurate and results in decisions that are extremely detrimental
to care. In essence, nonclinical people often do not understand that nursing
is a profession of human connection. A nurse is constantly assessing his or
her patient in objective and subjective terms, applying a vast knowledge base,
and making judgments about the significance of findings. Changes in a patient's
condition are often insidious; in order to detect them and intervene appropriately,
a nurse must have contact with the patient. If a nurse is spread too thin, trying
to care for too many patients, he or she may miss important (though subtle)
changes. The results may be disastrous. This is the concept of "failure to rescue"
that is emerging in the literature as a result of research on staffing.3
A nurse can safely take care of only a finite number of patients, regardless
of the technological or ancillary support available. Research is now affirming
this fact, but to nurses it has been obvious all along.
Evidence-Based Management?
For all the enthusiasm that U.S. health care has mustered for ensuring that
clinical practice is based on the best available evidence, it has a paucity
of evidence-based management practice. An examination of the management
strategies being implemented around the country can lead to no other conclusion.
One sees, for example, "across-the-board" budget cuts, "doing more with less,"
and cutting nursing budgets simply because "they're the biggest." The irony
is that such strategies have never produced desired results, and they certainly
aren't doing so now.
In Search of the Quick Fix
One of the greatest leadership failures in the history of U.S. Health care
has been the excessive engagement of consultants in pursuit of the quick fix
of problems for which there is, in fact, no quick fix. Millions of dollars have
been spent on consultants selling "turn key" solutions, millions more spent
undoing the ill effects of bad advice, and still more millions spent fighting
union-organizing drives fueled by employee disenchantment. Where is the accountability
for the return on these huge investments? Leaders have been reckless in their
use of the term "best practice" when, in fact, what they were replicating was
a fad. Perhaps nothing illustrates this better than the "patient-focused care"
and "reengineering" notions that swept the nation in the 1990s. Such fads seem
to indicate a belief that the collective talent already residing in our organizations
cannot successfully meet the challenges we face.
An Unrealized Prediction
In the 1980s and '90s, experts predicted that health care would soon be provided
by networks, whose services would cover a person from birth to death and which
would be paid for through a capitated premium. In response, health care systems
scrambled to form these networks. They made major acquisitions to ensure that
they would be well positioned to bid for their share of "covered lives." Although
millions of dollars were shifted from service to hierarchy in the creation of
these networks, "capitated care" never materialized.
Selling Services for Less than Cost
Services cannot be sold for less than the costs of providing them. Hospitals
are a labor-intensive business. No matter what process improvements are made,
no matter what technological supports are in place, no matter how many ancillary
supports are provided, there will always be a finite number of patients a nurse
can safely care for. The research correlating registered nurse staffing with
patient outcomes demonstrates this.4 Yet hospital administrators
continue to sell services for less than they cost in competitive markets because
they believe they have no choice but to do so. The only way a hospital can sell
its services for 30 cents on the dollar is if its prices are three times higher
than they need to be.
Outdated, Meaningless Measures
The use of outdated and meaningless measures provides another example of the
paucity of evidence-based management practice in health care today. The "midnight
census," for example, is useful for one thing only: identifying how many patients
are in hospital beds at midnight. It has absolutely nothing to do with demands
for patient care during the day. Yet it is a measure many hospitals continue
to use to bring pressure on nursing organizations regarding staffing requirements.
"Patient days," in the absence of length-of-stay comparisons, are equally useless.
Many other examples could be identified.
Misuse of Indicators
Is the lowest possible number of hours spent on patient care a "best practice"?
Can hours of care be driven so low as to make patient, employee, and physician
satisfaction impossible? Can they be driven so low as to make safe care impossible?
Administrators' credibility depends upon demonstrating an understanding of the
relationships between and among different variables. An efficient and effective
organization is, for example, characterized by the lowest possible costs necessary
to generate the best clinical outcomes; the highest patient, employee, and physician
satisfaction; and the best operating margin. It is finding the balance that
poses the challenge to skilled administrators.
Yet, sadly, a single variable—low costs—is too often used as an example of a "best practice," despite poor outcomes in other areas. The truth is that, over the long run, success will be realized only through positive outcomes in multiple dimensions. Table 4, illustrates this concept. In it, Hospital C has posted the lowest-paid hours per adjusted patient day. Yet the facility's use of contract labor, its negative satisfaction scores, and its negative operating margin suggest a hospital in trouble. Do Hospital C's hours of care represent a "best practice"—or cutbacks so severe that high-quality results are impossible? Sadly, too many administrators would hold up the hours of care as a goal for others to aspire to.
Cost Reduction Is Not Always Improvement
Keeping all relevant variables in balance with one another is vital in hospital
administration. Equally vital, and closely related to the need for balance,
is the need to address the agenda with integrity when it comes to making improvements
versus cutting costs. Too often a cost-cutting agenda is thinly veiled with
references to "improvement." But improvements may not reduce costs—and cost
cutting may not improve anything over the long term. An improvement can
be defined as a change that produces a sustained, desired result. If cost reduction
is the goal, it is important to be candid about both it and the rationale for
carrying it out. Anything less than candor feeds organizational cynicism and
implies a lack of respect for the entity's employees.
The Bureaucracy of Compliance
As regulatory pressures have increased, many health care organizations have
created huge bureaucracies to ensure compliance. It is ironic to hear legislators
express concern about massive administrative costs in health care, seemingly
oblivious to the impact of all of the regulation they have helped heap on the
health care system. Consider responses to the "Y2K crisis," risk management
concerns, patient safety reports, the Leapfrog quality-control program, and
now the Health Insurance Portability and Accountability Act. Too often, whole
departments are created to ensure compliance and meet reporting requirements,
draining ever more resources away from patient care. Too often, the compliance
strategies are developed by nonclinical people who have no understanding of
the strategies' impact on the ability to provide care. The hands of the caregivers
are increasingly tied behind their backs. Would it be possible to approach compliance
by educating caregivers themselves concerning regulatory requirements and engaging
them in designing solutions that would least compromise their ability to take
care of patients?
Making It All about Money
The administrative response to declining reimbursement has disenfranchised
nurses. As a result, many have left hospitals for more satisfying environments,
meanwhile advising their children against considering nursing as a career. Nurses'
top priority has always been excellent patient care and the intrinsic rewards
associated with the practice. Certainly they want to be well-compensated for
their professional services, but few have ever gone into nursing primarily to
make money. Nurses are knowledge workers who are drawn to nursing because it
is one of the few professions that allows one the opportunity to make an incredible
difference in people's lives.
The lesson from thriving nursing services, such as St. Marys', is that what nurses care about is the practice environment. Yet, despite this lesson, health care organizations still tend to respond to staffing problems with money—one more example of the pervasive search for the quick fix as a contemporary management strategy. St. Marys' Nursing Organization focuses on the creation of a satisfying professional practice environment, partnership, engagement, and ownership. There are no monetary incentives of any kind, in contrast to the sign-on bonuses, extra-shift bonuses, and finder's fees seen at so many other hospitals. The nurse vacancy rate at St. Marys is 3 percent, while another hospital, with $10,000 sign-on bonuses, is importing nurses from the Philippines. How much more evidence is required?
Mandated Staffing Ratios
Recent legislation mandating staffing ratios in California is evidence of the
lack of partnership that has characterized too many health care organizations.
Nurses understand that ratios are a poor solution, because the nature of the
patient, the expertise of the nurse, the layout of the patient care unit, and
other variables must all be considered in determining an appropriate patient
care assignment. The strategy of turning to a legislature for staffing relief
is clearly one undertaken by desperate and powerless nurses. It is unfortunate
things have come to this, but mandated ratios are surely a sign of things to
come if administrators do not make significant changes in the way they try to
cope with reimbursement pressure.
A Different Path
Reviewing the mistakes U.S. Health care has made in grappling with the intense
reimbursement pressures on it can be discouraging. But it doesn't have to be.
The fact that some organizations have found success by taking a different path
must serve as a catalyst for rethinking and redirecting administrative efforts.
The recommendations that follow provide a roadmap to improved outcomes and,
ultimately, to creating practice environments that nurses want to be
part of.
Health care organizations must, first, implement real shared decision-making models. Among other things, this must include changing organizational structures to locate decision-making accountability where the expertise lies. Catholic organizations especially must do so, because putting decisions in the hands of those who perform the work is mandated by the Catholic principle of subsidiarity.
Management (including hospital and system CEOs) must give up command-and-control behavior and learn to be facilitators of the system of care. Substantial investments of time and money must be made in skill building in all segments of the organization. But a word of caution here: Growing evidence indicates that administrators may view pursuit of Magnet Recognition, for example, as the next quick fix—a new recruitment and retention strategy. But if shared decision-making is approached as a recruitment and retention strategy, failure is guaranteed. Success will come only if it is pursued because leaders see it as the best way to optimize the organization's performance.
In assessing where and how costs can be reduced, a health care facility's leaders should begin at the core of the organization, where patient care is delivered, taking care to protect that core—service providers and frontline managers—at all costs. They are the reason the organization exists.
Leaders should reevaluate and dismantle corporate structures as needed to ensure financial viability. Over the past decade, these structures have mushroomed out of control and endless reasons have been developed to defend them. Health care organizations today tend to be top-heavy—with managers reporting to directors, who report to assistant vice presidents, who report to vice presidents, who report to senior vice presidents, and on and on. Can this really be defended in a fiscally strapped environment? These structures are sapping the lifeblood out of patient care organizations. A benchmark worth striving for is to be the health care system with the fewest managers in relation to total employees.
But leaders seeking to "flatten" their organizations must remember to protect the core. In a nursing unit, the frontline manager is the primary person through whom strategy is deployed and staff development accomplished. It would be unwise to have this person manage more than one unit. At St. Marys, the vice president for patient services has 37 "direct reports"; they are producing exceptional results and their satisfaction is high.
Finally, we must come to grips with the fact that some hospitals cannot survive today's climate. How long is it reasonable to allow a hospital to bleed millions of dollars of red ink? If bureaucracies have been streamlined and all reasonable strategies have been exhausted, it is time to close the doors on hospitals that are not viable. If the underlying cause is overcapacity, the health care of the community will not be jeopardized. If the issue is unrealistically low reimbursement, it is time to dramatize the crisis and make it visible so that we can put to rest the myth of "spending less on health care." In any event, a strategy that hopes to deliver high-quality patient care with fewer resources than are required to do so will never succeed.
NOTES
- Analysis of American Nurses Association Survey, Cornerstone Communications Group, Warwick, RI, 2001.
- Acute Care Hospital Survey of RN Vacancy and Turnover Rates, American Organization of Nurse Executives, Chicago, 2002.
- Linda H. Aiken, et al., "Hospital Nurse Staffing and Patient Mortality, Nurse Burnout and Job Dissatisfaction," JAMA, October 23, 2002, pp. 1,987-1,993.
- Aiken; and Jack Needleman, et al., "Nurse-Staffing Levels and the Quality of Care in Hospitals," New England Journal of Medicine, May 30, 2002, pp. 1,715-1,721.
