BY: T.S. DHARMARAJAN, MD; ROSEMARIE LIFRIERI, RN; and LORRAINE S. GERSTNER, EdD
The United States is an aging society. Whereas only 4 percent of the nation's population was 65 years old or older in 1900, 12.6 percent was in that age group in 1990. And demographers estimate that nearly 22 percent will be 65 or older in 2050.1
The leaders of Our Lady of Mercy Medical Center, Bronx, NY, began to note this trend in the late 1980s. (In the North Bronx, where our facility is located, 14.9 percent of the population is 65 or older, a higher proportion than in New York City as a whole.) It became increasingly clear to us that not only were many of Our Lady of Mercy's patients older people; they also had multisystem illnesses requiring care qualitatively different from that usually provided in an acute care facility.
A New Geriatrics Division
In 1992 we opened Our Lady of Mercy's Division of Geriatrics as an 18-bed pilot project (since then, it has grown to comprise two units; a third unit will be opened soon).
Our geriatrics program was planned by a multidisciplinary task force led by a recently appointed medical chief of geriatrics and including other physicians and the administrators of the medical center's strategic planning, operations, patient care, and nursing departments. We were determined to create a seamless continuum of care into which elderly patients could be admitted through any portal of entry: home, physician's office, emergency room, acute care hospital, or long-term care facility. Once admitted, patients would receive holistic care reflecting all dimensions — physiological, psychological, sociocultural, and spiritual — of their lives. Believing that healthcare must treat people rather than diseases, we vowed that the new unit would be compassionate and sensitive to the needs of the whole patient.
To coordinate patient care, we created a multidisciplinary team consisting of a geriatrician, nurse, case manager, social worker, pastoral care worker, and pharmacist. Other specialists would join the team as the need arose.
In addition, we hired an interior decorator to design the unit so that it would meet the needs of older patients. And we used radio, television, and newspaper advertising to market the unit's services to area physicians, families, and insurers.
Division Operations
Since 1992 our program has expanded to include two Bronx units, one with 38 inpatient beds and another with 37. A third unit of 17 beds will open in White Plains, NY, before the end of the year.
Care in each unit is coordinated by a multidisciplinary team, which meets weekly. The overall program is supervised by a long-term care committee, which includes the program's medical chief and clinical nursing director as well as representatives of Our Lady of Mercy's administration and board of trustees. The long-term care committee (which replaced the original multidisciplinary task force) meets at least four times a year.
Assessment
All patients receive, along with care for the problems that brought them to the program, a comprehensive health assessment. This assessment, based on established guidelines, includes screening for infectious illnesses (and immunizations for them), malnutrition, cancer, cognitive impairment, a tendency to fall, and other illnesses. The patient's functional ability to perform the various activities of daily living is assessed as well.
Physician Services
Our geriatricians supervise the care given to inpatients. Discharged patients may, in the interest of continuity, choose to be seen as outpatients by the same geriatrician who provided the inpatient care or by another physician of their choice. (Each inpatient unit has an associated outpatient clinic that is open three days a week; the new White Plains unit will have a similar clinic. The division is also planning to build in the Bronx a much larger outpatient clinic, which would be open five or six days a week.) Our Lady of Mercy also has a home care program that enables patients to be evaluated in their homes.
Nursing Services
We provide five levels of nursing services along a continuum:
- Level 1 for patients in an optimal state of health and adapting well to the environment
- Level 2 for currently healthy patients at risk for sudden changes in health status
- Level 3 for patients with chronic illnesses who can with some support perform activities of daily living
- Level 4 for patients admitted to an inpatient unit for treatment of acute health problems
- Level 5 for patients who no longer perform activities of daily living and are dependent on caregivers for their survival
At each level, we formulate patient goals and nursing interventions according to geriatric nursing care standards.
Education Is a Vital Component
When we created the geriatric division, we realized that its ultimate success would depend on a strong educational component. In one sense, education is routinely imparted throughout the division. Family members, for example, are shown how to give patients home care. Division nurses receive formal training in geriatrics. And the division itself serves as a geriatric training site for interns, residents, medical students, nursing students, nurse practitioners, physician assistant students, and trainees from preventive medicine, psychiatry, and physical medicine.
But the division also has a more formal educational program: fully accredited fellowships for physicians planning to specialize in geriatrics. Launched in 1993 with a single fellow, the program today has eight, making it one of the largest and fastest growing in the nation.
Six Years of Success
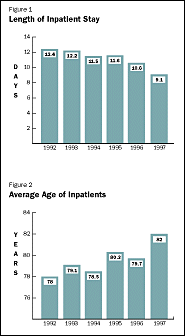
Since our program began, the average age of its patients has increased from 78 to 82. As in the nation as a whole, our patients are today older and more ill, and need more complex care than geriatric patients used to require. Fortunately, the program has demonstrated its ability to provide precisely such care. Between 1992 and 1997, for example, we cut the average length of patient stays from 12.4 days to 9.1 days. By the end of this year, the average length will have been reduced to fewer than 8 days.
In addition, we have learned that because so many of our inpatients are admitted from area long-term care centers, it is vital that we collaborate closely with key personnel from those facilities. (Our clinical director of nursing sends a weekly report on such patients to the care centers involved; our long-term care committee maintains an ongoing relationship with those centers' leaders.) This not only enhances our relationships with patients, their families, and the care centers; it also helps us to be better patient advocates.
Finally, our geriatric division is working with Our Lady of Mercy's research division to develop new products — for example, agents that will inhibit the growth of microorganisms in elderly patients. In recent years, several papers based on such research have been presented to various national and international conferences; they will be published soon.
Because of the aging of the nation's population, the future of geriatric care seems nearly limitless. At Our Lady of Mercy, we have developed a housing program and are considering building an assisted living facility and a long-term care center. Although we have achieved a great deal, much more needs to be done.
For more information call Rosemarie Lifrieri, 710-430-6392.
NOTES
- Vernon L. Greene, Deborah Monahan, and Patricia Coleman, "Primary Care Geriatrics," in D. B. Reuben, T. T. Yoshikawa, and R. W. Besdine, eds., Geriatric Review Syllabus, 3d ed., Kendall/Hunt Publishing, Dubuque, IA, 1996, pp. 5-7.
Dr. Dharmarajan is chief; Ms. Lifrieri is clinical director of nursing; and Dr. Gerstner (not pictured) was formerly director of education, Division of Geriatrics, Our Lady of Mercy Healthcare System, Bronx, NY.
LESSONS FOR NEW GERIATRIC PROGRAMS
The founders of Our Lady of Mercy Healthcare System's Geriatric Division share the following lessons:
- Geriatric units are not inexpensive. Be prepared to spend substantial capital.
- Plan on space for at least 25 to 40 beds. It is easier to reduce the number of beds than to increase them.
- Include in the unit's educational program students in medicine and nursing, nurse practitioners, physician assistants, podiatry residents, and medical residents, interns, and, if possible, fellowship recipients. The program should be well under way before the facility opens its doors.
- If possible, employ only nurses who are trained in geriatrics.
- Establish contacts with local nursing homes before the geriatric unit opens.
- Equip the facility with pressure-relief beds and/or mattresses to prevent bedsores and with devices (e.g., handrails) that help prevent patient falls.
MEDICAL SYSTEM FACES AGING U.S. POPULATION
Our Lady of Mercy's decision to create a new geriatric division was influenced by facts such as the following:
The most rapidly growing U.S. population segment is made up of people 85 and older. Between 1980 and 1991 this segment grew by 41 percent, to a total of 3.2 million people. The number of people aged 75 to 84 grew by 33 percent (Ronald I. Shorr, "Demography of Aging," in D. B. Reuben, T. T. Yoshikawa, and R. W. Besdine, eds., Geriatric Review Syllabus, 3d ed., Kendall/Hunt Publishing, Dubuque, IA, 1996, pp. 1-2).
Because they are often burdened with chronic illness, people 65 and over consume a disproportionate share of healthcare services. Although they make up just 12.6 percent of the population, they use nearly 28 percent of physician services, 40 percent of hospital days, and more than 90 percent of nursing home days (L. G. Pawlson, Donna L. Infeld, and Deborah Lastinger, "The Health Care System," in R. J. Ham and P. D. Sloane, eds., Primary Care Geriatrics: A Case-Based Approach, 2d ed., Mosby, St. Louis, 1992, pp. 122-123).
- People 65 and older are admitted to the hospital three times as often as the nonelderly (almost 40 percent of patients are 65 and over). In addition, the elderly stay 50 percent longer and use twice as many drugs. Most admissions of the elderly are triggered by chronic illness.
