Teaming Up for Patient-focused Care
In a process that began in 1992, Holy Spirit Hospital, Camp Hill, PA, has undergone a dramatic paradigm shift, breaking with traditional operating practices to focus on improving patient care while containing operating costs.
Mission-driven Program
The transformation was prompted by the distribution of the hospital's revised mission and values statements, which stressed patient dignity, holistic care, service, and stewardship. Financially, the hospital was barely breaking even. Holy Spirit administrators and managers realized they needed to translate these principles into concrete programs and policies to improve both the bottom line and patient care quality.
Their first step was to perform an organizational self-assessment using the Malcolm Baldridge National Quality Award criteria. The computerized assessment assigned rankings for 28 items within 7 categories: leadership, information and analysis, strategic quality planning, human resource utilization, quality assurance, quality assurance results, and customer satisfaction.
Each category includes specific factors to examine. For example, in assessing customer satisfaction—the most heavily weighted category—evaluators are asked to look at how the organization manages customer relationships, determines customer satisfaction, and gauges customers' future needs and expectations. They also look at the organization's overall commitment to customers, as well as how the level of their customers' satisfaction compares with that of competitors.
"Once we did the Baldridge assessments, we realized that some of our processes were not very patient oriented," said Mike Ciccocioppo, vice president, marketing and planning.
Participants at the hospital's strategic planning retreat used a summary of this assessment to identify strategic priorities for the organization. They decided Holy Spirit should pursue total quality improvement initiatives in all services areas, create an effective client-focused integrated delivery system, and redesign care practices to make them more patient focused.
Design Teams
Meanwhile, a system was put into place that engaged the entire organization in strategic initiatives. Logistics Management Corporation, which led the hospital through the process, introduced the concept of a "design team," a group of representatives from various departments with a common goal who meet regularly to solve problems that prevent that goal from being reached (see Figure).
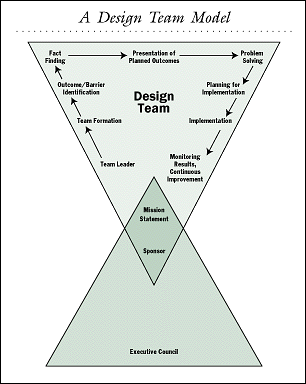
The teams systematically dissect every aspect of an operation, identifying barriers that prevent individual systems from working efficiently. The design teams have a sponsor from the executive ranks and members from all levels of the organization.
One of the first teams organized at Holy Spirit focused on patient treatment scheduling. Before the team was in place, the hospital delivered 45 percent of inpatient treatments on time. The team fashioned a mission statement, identified barriers and outcomes, did research, agreed on a new system for implementation, and implemented the system. It then monitored results for continuous improvement.
Communication problems were among the most significant barriers the team uncovered. For example, patients were usually not told when an examination was scheduled and so were often unprepared when a transporter arrived. Often, nurses were not informed when a scheduled test had been canceled, even when the test required that a patient not ingest anything for hours beforehand. "Each department focused on its own needs, like keeping x-ray technicians and radiologists productive, rather than patient needs," Ciccocioppo explains.
To address such problems, the patient treatment scheduling team devised easy-to-use, color-coded "paper clocks"—master schedules to record the time for each patient's nursing and ancillary care for the day. Care givers mark schedules with "in" and "out" arrows when the patient begins and ends treatments. The system also expedites scheduling of patients between departments and uses color-coded schedules with stars to indicate "delayed" or "canceled" treatments for future problem solving.
With easier scheduling and increased productivity, on-time treatments are at 93 percent and climbing, says Ruth Gillis, RN, the design team's leader and director of nursing. In addition, departments and physicians can plan better knowing when patients will be available.
Team Authority
Accountability is an important aspect of the design team process. When team members are given assignments, they are expected to use their authority or find authority to accomplish the task. In the past, an employee who identified a barrier usually had difficulty finding departmental support for overcoming it. Now, as long as the hospital's executives believe in the design team's mission and goals and have sanctioned their work, team members are empowered to accomplish their goals. And because hospital administrators have emphasized the effectiveness and permanency of the design team concept, the rest of the staff understands the importance of complying with that team's plan to solve the problem. Oversight and monitoring of each team's progress is the responsibility of its sponsor.
Making the necessary changes to solve a patient care problem often involves altering methods or procedures and crossing lines of authority—a difficult process, but one that is supported by the hospital's leaders. "We knew tremendous changes were ahead," says Sr. Romaine Niemeyer, SCC, Holy Spirit's president. "We had to position ourselves by using new skills to carry out our mission in today's world.
"Only the people who actually know what's going on can manage these changes in our system effectively," she continues. "That's why these design teams comprise a cross section of employees from various departments and at all levels of responsibility."
Other Teams
The patient treatment scheduling team, whose work is now completed, was only 1 of about 20 design teams established at Holy Spirit Hospital to look at operational efficiency and revenue enhancement. Once the team's recommendations were implemented throughout the hospital, its role shifted and the members began implementing a central transport system to improve and standardize patient transportation.
Other teams work to improve such operations as discharge procedures, standardized reporting, and billing and collection. One of the most significant accomplishments was a reduction in process time for emergency room admission from 4.4 hours to 2 hours and for patient discharge from 2.2 hours to 1 hour.
The new systems allow the emergency department to process more patients and provide higher-quality care with the same facilities. The emergency room team also implemented several new systems that help eliminate bottlenecks, one of the most effective of which has been a new triage system. Patients who enter the HealthCare24 system (for emergency care and family healthcare) are directed to the triage nurse, who assesses patients' conditions and immediately directs them to either area of care as needed. This system reduces the nonemergent visits to the emergency room and begins the patient's nursing care at an earlier point in the visit.
Another improvement, the addition of an office manager to oversee the emergency room's clerical staff, led to a 60 percent reduction in duplicate registrations. Improved signage, additional equipment, a redesigned phone system, a patient flow board, and new operating reports further improved the emergency room's efficiency. All improvements were essential, since 58 percent of the hospital's patients enter through the emergency room.
Performance Measurement
An important component of the cultural transformation to total quality management at Holy Spirit was a departmental productivity reporting system, introduced with the addition of performance measurement teams. These teams, which generally include all managers and many of the staff for a single area of the hospital, assess whether the department is "right sized" to handle the volume of patients and has the internal controls to ensure on-time performance and high-quality patient care.
The laboratory was the first hospital department to establish this system of improved work flow and productivity, implementing the following recommendations:
- Consolidate the office and phlebotomy sections and cross-train staff to do both functions
- Decrease the number of supervisors
- Buy personal computers for all supervisors to accomplish work more efficiently
- Buy four high-speed, high-performance printers to reduce time needed to monitor printer performance
- Rearrange system for compiling reports for physicians
- Create a flex pool to respond to fluctuating work load
- Begin direct order entry with all five satellite family health centers to eliminate unnecessary duplication of steps
Daily operating reports documented the laboratory's efficiency and heightened accountability for the hospital's executive group. Nearly all hospital departments now provide these reports, and total savings realized through performance measurement amount to more than $1.7 million annually. Many of the operational improvements in efficiency initiated through the design team process also contributed to these savings.
Ongoing Process
The implementation of patient-focused teams has contributed to a dramatic turnaround at Holy Spirit. In 1993, income from operations grew from $0.5 million the previous year to $3 million, and earnings as a percent of revenue increased from 0.7 percent to 3.8 percent. Patient satisfaction has also improved significantly.
"The exciting part is that the process we're engaged in will never end," says Sr. Romaine Niemeyer. "What this is all about is stewardship, and those of us who serve in the healthcare field are called to be responsible stewards—especially in this time of dramatically declining reimbursements and the uncertainty of healthcare reform."
Tamara Reisinger
Public Relations Director
Holy Spirit Hospital
Camp Hill, PA
