Ms. White is executive editor, Health Affairs.
Debate over healthcare reform has taken center stage with the release of President Bill Clinton's sweeping reform proposal before the September 22 joint session of Congress. Calling the American system "badly broken," Clinton appealed to Congress for swift, bipartisan action: "For the first time in this century leaders of both political parties have joined together around the principle of providing universal, comprehensive health care. It is a magic moment, and we must seize it."
Healthcare Politics
The president's September speech recalled the passion and high public approval ratings that surrounded his state of the Union address. A September 22 Washington Post—ABC News poll reported that, after the speech, approval of the administration's plan jumped 13 percentage points, to 56 percent of those surveyed; 24 percent said they disapproved.1
To achieve action on his plan, Clinton clearly needs to win and maintain a high measure of public support. Without strong public backing, the varied political and special interest groups will have a stronger influence on Congress in shaping the final legislation.
Clinton must also keep the momentum going, stay focused on the issue, and not waste political capital on tangential issues, as was the case early in his presidency. Healthcare reform is a complex undertaking. Political analysts are citing the president's plan as the most significant domestic policy legislation in decades. At stake is the restructuring of the nation's $900 billion healthcare enterprise–one-seventh of the U.S. economy.
At the moment Clinton and Congress appear committed to placing healthcare reform at the top of the political agenda. Indeed, the Washington Post editorialized on September 19, 1993: "The need to reconstruct the health care system is becoming increasingly urgent. For the next year, it is likely to be, properly and necessarily, the central preoccupation of American politics."
Bipartisan support and political compromise will be central to achieving any action on healthcare reform. The issue divides both political parties and makes for some interesting alliances. One political party cannot pass healthcare reform. Clinton will need to earn the support of the more liberal Democrats who favor a single-payer system, or Canadian-type plan, while also getting the backing of moderate Republicans who favor less government regulation and more private-sector competition to hold down healthcare costs.
The Republicans do seem open to working with Clinton on this issue. "There is a real interest in trying to work together . . . an interest in getting this problem solved," said Gail Wilensky in a conversation. "However, the fact is that there are some very serious differences that need to be reconciled, some of which are not negotiable," she added. Some of the philosophical differences she cited include "employer mandates, spending limits, premium caps, and highly regulated bureaucratic mechanisms." The other big issue is the budget. "Republicans are not at all inclined to increase taxes," and the numbers regarding financing Clinton's plan are "not real," Wilensky said. A health economist and former Bush administration domestic policy adviser, Wilensky is now advising Republicans in Congress on healthcare reform.
Sen. John Chafee, R-RI, will be a key Republican leader to watch in the coming debates as a potential Clinton ally. Sen. Dave Durenberger, R-MN, could be a major reform proponent. He has long been involved in healthcare issues, and since he is not running for reelection, "he has no reason not to go for it" on advancing the reform debate throughout the Senate, said Robyn Stone, a member of the White House working group on healthcare reform. Even Senate Minority Leader Robert Dole, R-KS–the president's foe in the budget battle–is supportive of healthcare reform. Dole's Chief of Staff Sheila Burke is a former nurse and health policy adviser. The direction his leadership takes must also be watched.
On the Democratic side, there are a number of important players. House Ways and Means Committee Chairperson Dan Rostenkowski, D-IL, will be a principal leader in negotiating a congressional compromise, particularly on financing, if he can maintain his political clout while under the cloud of an ethics investigation. Senate Finance Committee Chairperson Daniel Patrick Moynihan, D-NY, has already sharply questioned the financing numbers put forth by the president, but then in a later speech endorsed the president's plan. The Senate Finance Committee's political support will be necessary for passage of any healthcare legislation.
Other influential Democratic congressional leaders include Rep. Fortney H. (Pete) Stark, D-CA, who chairs the House Ways and Means Subcommittee on Health. Stark is a leading advocate of a Canadian-style health plan, along with Rep. Jim McDermott, D-WA, and Sen. Paul Wellstone, D-MN. Rep. Henry A. Waxman, D-CA, who chairs the House Energy and Commerce Subcommittee on Health and the Environment, is another long-time healthcare leader whose support in Congress will be necessary. Waxman has expressed concern about the level of savings the president hopes to achieve by cutting the rate of spending increase in Medicare and Medicaid to finance the new reform plan.
In the Senate, Democratic leaders on healthcare include Sen. Jay Rockefeller, D-WV, who chaired the Bipartisan Commission on Health Care Reform and now chairs the Senate Finance Medicare and Long-Term Care Subcommittee; and Sen. Edward Kennedy, D-MA, who chairs the Senate Labor and Human Resources Committee and has pushed for universal healthcare coverage throughout his career.
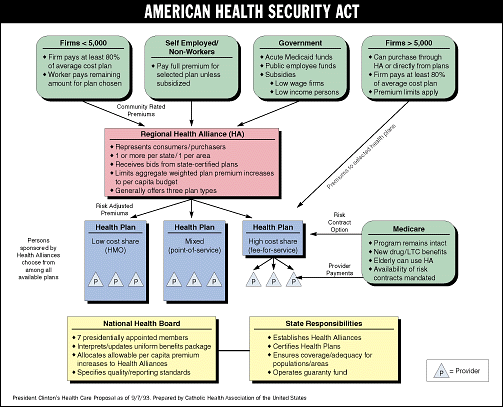
State Politics and Responsibilities
The politics of healthcare reform, however, extend far beyond Washington, DC. A key facet of Clinton's plan involves high-level responsibility for the states–most notably in ensuring healthcare coverage for all residents. A number of states have already taken steps to achieve greater healthcare coverage for their citizens (see October's column, "States Lead Way in Healthcare Reform," pp. 10-12, 47). Indeed, in the short term, state reform activities should not be overlooked in the furor of healthcare reform surrounding Washington. "Anything that can be done without costing [the federal government] money will be done this year. That makes the states very interesting," said Dan Fox, president of New York City—based Milbank Memorial Fund, in a conversation. Fox has written extensively on Oregon's healthcare reform plan and currently helps arrange meetings among state leaders to discuss healthcare reform issues.
State Responsibility According to the September 7, 1993, working group draft of the president's plan, the American Health Security Act of 1993, "States assume primary responsibility for ensuring that all eligible individuals have access to a health plan that delivers the nationally guaranteed comprehensive benefit package."2 Under the Clinton proposal, each state must submit to the National Health Board a plan for implementing healthcare reform, based on federally set requirements. By January 1, 1997, each state must establish one or more regional health alliances to provide healthcare coverage to all its residents. States also would qualify healthcare plans to participate in the alliances and would perform various other functions.
Each state must designate a state agency or official to coordinate its healthcare responsibilities among the appropriate state agencies. In many states responsibility for healthcare coverage overlaps, necessitating streamlining or even overhauling of state structures.
The road to reform will not be smooth or without controversy. Even in Florida, a state whose political leaders are committed to pushing healthcare reform, the idea that a single state agency be given responsibility for reform was controversial. This proposal was narrowly approved by the state's Task Force on Government-Financed Health Care in March 1991 only because the task force agreed to make known that 8 of the group's 17 members (including all three of its hospital representatives) expressed dissenting views on the proposal for a single state agency to be given responsibility for reform of the state's healthcare system.3 Not only would entrenched political structures change under Clinton's plan, but healthcare providers accustomed to dealing with multiple layers of agencies, perhaps with more diluted power, would have to work with one powerful state agency or official coordinating local healthcare reform.
According to the president's draft proposal, each state plan must also show how the state will carry out the following functions:
- Administration of subsidies for low-income persons, families, and employers
- Certification of health plans
- Financial regulation of health plans
- Administration of data collection and a quality management and improvement program
- Establishment and governance of health alliances, including a mechanism for selecting members of boards of directors and advisory boards for alliances
Health Alliances: Ensuring Access to Care The establishment of regional health alliances is states' primary responsibility under Clinton's managed competition strategy. These alliances (formerly called health insurance purchasing cooperatives, or HIPCs) are the point at which universal access to healthcare is ensured. "Because there are substantial variations across the country in the ecology of the medical care delivery system and in the preferences of providers, patients, and politicians, it makes sense to give the states substantial discretion in how HIPCs should be appointed and administered," explained White House task force adviser Richard Kronick,4 an assistant professor at the University of California, San Diego.
According to Clinton's draft plan, "The state ensures that all eligible individuals enroll in a regional alliance and that all alliances offer health plans that provide the comprehensive benefit package. The state also ensures that each alliance enrolls all eligible persons in the geographic area covered by the alliance." In areas with inadequate access to healthcare, such as some rural and urban areas, it is the alliance's responsibility to build healthcare networks to increase access to care. Individuals not covered through a health alliance are those with healthcare coverage under Medicare, the Indian Health Service, the Department of Veterans Affairs, or the Department of Defense. Medicaid beneficiaries would receive their healthcare coverage through the new alliances.
A health alliance may be structured in several ways–as a not-for-profit corporation, an independent state agency, or an agency of the state executive branch. An alliance would hold an annual open enrollment period to register everyone in its region, including low-income and unemployed persons. A regional alliance would automatically assign a healthcare plan to those persons who do not sign up during the enrollment period.
Each alliance contracts with approved health plans that meet national quality standards and that offer the guaranteed benefit package set at the federal level by the National Health Board. A large corporation (more than 5,000 employes) may form its own "corporate alliance" to cover its workers.
Budgets: Controlling Rising Costs To hold down rising healthcare costs, Clinton's reform plan would set a national healthcare budget. According to the draft plan, the budget centers on annual premium increase targets based on a weighted average premium for the nationally guaranteed benefits package in regional health alliances. Whether these targets become legislated premium "caps" will be a matter of debate. The target premium increase rates in the draft are the Consumer Price Index (CPI) plus 1.5 percentage points for 1996; CPI plus 1 percentage point for 1997; CPI plus 0.5 percentage points in 1998; and the projected rate of increase in the CPI by 1999.
The National Health Board would calculate the per capita insurance premium target for each health alliance, adjusting for regional variations. To help achieve this, the president's task force on healthcare reform asked the Health Care Financing Administration (HCFA) to publish new estimates of healthcare spending by state–for the first time in nearly a decade.
"Task force members were concerned about the quality of estimates that could be produced with existing data, and whether these estimates were sufficient to set global budgets at the state level under a reformed health system," write HCFA analysts Katharine R. Levit and colleagues.5 "At the same time, state governments requested similar information as they embarked on separate reform initiatives," they continue.
The new HCFA estimates show that the New England and Mid-Atlantic regions spend consistently more for hospital care, physician services, and retail purchases of prescription drugs than do other regions. The Southwest and Rocky Mountain regions spent the smallest amount (as much as 17 percent below the national average). Two states–California and New York–account for 20 percent of state spending on hospitals, physicians, and drugs. The annual growth rate for these state healthcare spending categories averaged 10.5 percent between 1980 and 1991.
State Flexibility President Clinton's health proposal allows for some state flexibility in meeting the overall goals of universal healthcare coverage and cost control. For instance, a state may establish a single-payer system rather than health alliances that offer multiple plans. A state may also set up a single-payer alliance to serve part of its state. This option may be used in rural areas where multiple plan competition is not feasible.
Vermont is already pursuing a single-payer option. The Vermont Health Care Authority is charged with designing two alternative health systems (single payer and multipayer) by November 1993. "Both plans should offer universal coverage by October 1994, including provisions for global budgeting, uniform health benefits for all residents, centralized planning, incentives to contain costs, reimbursement mechanisms for providers and recommendations for incorporating long-term care," notes a recent report on state reform activities.6
State Capacity Health alliances represent a new venture for most states. Only California and Minnesota have had some experience with entities similar to Clinton's proposed health alliances. Likewise, state data capacity for creating and monitoring healthcare budgets is uneven and will need considerable upgrading, although HCFA's new estimates offer a good start. Whether all states have the political expertise and the financial capacity to establish health alliances and carry out the other responsibilities laid out in Clinton's health plan is debatable.
Looking Ahead
State responsibility and capacity represent but one facet of President Clinton's plan under discussion. This complex and massive legislative proposal will lead to major debate on many fronts and engage many participants–providers, policy analysts, politicians, businesspersons, and citizens. Although the president's plan contains much to argue about, one thing is unarguable: Clinton has squarely placed healthcare reform on the nation's agenda. The plan is a serious effort. It is now time to get down to serious negotiation.
NOTES
- Dan Balz, "Vying for Public Trust," Washington Post, September 23, 1993, p. 1.
- "Preliminary Draft of the President's Health Reform Proposal," September 7, 1993.
- Lawrence D. Brown, "Commissions, Clubs, and Consensus: Florida Reorganizes for Health Reform," Health Affairs, Summer 1993, p. 12.
- Richard Kronick, "Where Should the Buck Stop: Federal and State Responsibilities in Health Care Financing Reform," Health Affairs, Supplement 1993, pp. 87-98.
- Katharine R. Levit et al., "Health Spending by State: New Estimates for Policy Making," Health Affairs, Fall 1993, pp. 7-26.
- The States That Could Not Wait: Lessons for Health Reform from Florida, Hawaii, Minnesota, Oregon, and Vermont, Milbank Memorial Fund, New York City, 1993.
