BY: D.W. DONOVAN, DBioethics, MA, MS, BCC
The chaplain's role in ministering to the ill, injured and suffering, as well as to their caregivers, has been acknowledged as critical for as long as hospitals have been built and staffed, as long as prisons have housed men and women and as long as people have been sent into battle.
Some of us remember growing up watching episodes of "M*A*S*H," where Fr. Francis Mulcahy introduced the role of the chaplain to many of us for the first time. Despite being the only chaplain assigned to the 4077th Mobile Army Surgical Hospital and appearing to be quite busy, Fr. Mulcahy struggled with his own sense of personal contribution. In the seventh season's popular episode "Dear Sis," Fr. Mulcahy worries that "When you're faced with such overwhelming misery, it just doesn't seem enough to offer spiritual comfort. … I hang around on the edge of effectiveness."1
To his credit, Fr. Mulcahy would have represented that innovative group of Catholic chaplains who sought to expand the role of chaplaincy beyond the provision of sacraments and the offering of traditional worship services. Unfortunately, with very few exceptions, our profession has not made much progress in our ability to evaluate and benchmark modern-day chaplaincy.
"I do give last rites to the dying," muses Fr. Mulcahy, "but if only there was something I could do for the living. … No one comes for confession. I have no one to grant absolution to. … At times like this, I head straight to the bar at the Officer's Club." We see him at the club serving drinks and listening to two different staff members express their distress over difficult relationships.2
This short scene not only illustrates Fr. Mulcahy's personal fears about being pastorally ineffective, but it also raises important questions about the best metrics for measuring the value of professional chaplaincy.
As the episode comes to an end, Fr. Mulcahy is toasted by his friends for his tremendous pastoral work and unique place within their community. His failure, such as it is, rests in his inability to recognize that although his ministry's setting and form may have changed since he joined the 4077th, the substance of what he has been called to do is the same — and he is quite effective at doing it.
MEASURES OF EFFECTIVENESS
So to put it in modern terms, Fr. Mulcahy has been using the wrong metrics. The episode points out the challenges of recognizing and measuring our own effectiveness.
In the past few decades, the profession of chaplaincy within the Catholic Church has shifted from care primarily provided by Catholic priests and sisters to care offered by board-certified chaplains from a variety of faith traditions. In turn, the importance of pastoral counseling and the ability to advance the plan of care for each patient as a fully integrated member of the health care team has grown.
Any director of pastoral care or mission leader who has experienced a finance and quality review session would recognize the avalanche of data that measures such things. Our country's movement towards affordable health care has focused our attention on fiscal processes, with a laser-tight focus on controlling salary and supply expenses and maximizing productivity.
This brings us to a unique place in the history of hospital chaplaincy. At precisely the time that our medical colleagues are using data more and more effectively, and at precisely the time when administrators depend upon productivity measures to establish and defend staffing levels, our profession has been slower to adopt such approaches.
It may be that chaplains have a resistance to talking about such sacred work in such secular terms. It may be that much of the world still equates chaplaincy with a priest performing the "last rites." It may be that the sheer diversity of staffing models within chaplaincy and the wide variety of ways in which chaplains are engaged in the life of a particular institution make any kind of standardized productivity measure nearly impossible.
AT AN IMPASSE?
This theoretical dilemma quickly has become a practical impasse for the many directors of pastoral care and mission leaders attempting to defend positions from elimination or, even more challenging, to add a position in the midst of tightening budgets and reductions in force. Many leaders at the local level have reached out to our national associations for guidance. Hoping to find clear answers based on whatever data points might be needed, callers instead learned that the National Association of Catholic Chaplains and the Catholic Health Association have been collaborating on the issues in a focused way since the 2007 Joint Pastoral Care Summit in Omaha, Nebraska. Their work to date was summarized in an article by Brian Smith in the September-October 2014 issue of Health Progress. Although the research reported there gave an emerging framework for effective spiritual care staffing, it fell short of the hoped-for algorithm that could lead to
national benchmarks.3
At a 2013 NACC meeting in Pittsburgh, the reasons why a formula or algorithm would not work were summarized as follows:4, 5
- The foundation of such systems is what is not working now: namely, a ratio approach of chaplains to beds that does not take into account acuity or account for staff care
- Because there is such diversity not only in what we do, but in what hours we cover, no one really knows how to compare apples to apples to see if we are staffed in numbers that are better, worse or equal to others
- We need to develop metrics that move us from pure volume to value. Correspondingly, our metrics need to be focused primarily on quality outcomes rather than on process measures
Experts in the field, with many years of experience, reached these conclusions after significant study of the issue. It clearly represents a consensus statement by many of the best and brightest of our leaders in chaplaincy today.
A STAFFING MODEL
With due respect to my colleagues, perhaps there is an opportunity for a minority opinion. I am driven by the belief that if products like "TurboTax"™ can account for the millions of intricacies within our tax code and still produce a result with high reliability and internal consistency across an entire nation, surely we can take some small steps in the same direction.
Therefore, with thanks to Intuit Inc. for the concept, I would like to present one example of how we might use an acuity-based model with adjustments to account for the various miscellaneous duties that chaplains often are assigned or take on voluntarily.
I created a chaplain staffing model that asks the user a series of questions in an easy-to-read format, with each section carrying a brief explanation of the work to come and providing hints to consider. Most of the calculations will be done behind the scenes, with a summary and recommendations presented to the user on a separate page.
Primary users (presumably directors of pastoral care) can use the tool to generate a meaningful discussion with their immediate supervisor regarding the most appropriate staffing for their department at that time.
Embedded in this article are some screenshots of the tool to give a sense of what I designed.
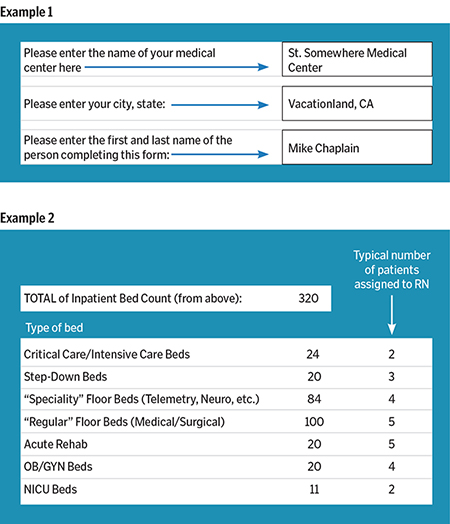

After a brief introduction (see Example 1), we begin by asking the user a series of questions for some basic information — the number of beds within the medical center, how they typically are classified and the nursing ratios typically used within them.
This is the information used to make calculations in the background as to the recommended number of chaplains (see Example 2).
As we start to move into the main part of the program, it is helpful to think of two different models of chaplaincy. The coverage model means one chaplain is assigned around the clock (it may or may not be an on-call or standby role). He or she responds to the major emergencies and receives specialized training to serve as a member of the Trauma and Blue teams, as well as to respond to deaths and to manage multiple traumas simultaneously. By artificially isolating this role for emergencies, for the moment, we can identify the remaining staff needed for the integration model.
In the integration model, we look to the chaplain as an integrated member of the team, contributing to many patients' plans of care and directly attending to those identified as needing the chaplain's specialized care.
Just like tax preparation software, my program offers helpful hints to prepare the user for each major section. The hints are designed to be respectful of the current variation that exists within local practice, but also to explain why the current best practices are recommended (see Example 3).
After thinking through how to select emergencies to be covered and looking at departmental standards, the next step is to identify the clinical situations that will trigger an automatic pastoral care consult on an emergency basis.
A MODEL FOR COLLABORATION
The conversation about covering emergencies sets an important precedent for how this tool can be used. Chaplaincy has a history of scheduling and pay practices that other professionals might not consider reasonable. However, the solution is not to use this or any other tool to wage war on behalf of the profession. The model here is one of professional collaboration, whereby the director of pastoral care is able to invite senior leadership into a conversation that respectfully seeks to find the best possible way of providing coverage based on the particulars of the specific setting and certain nearly universal standards.
For example, such a discussion might center on a chaplain's presence at the death of a patient. If the chaplain's callback time is 45 minutes, that time frame seems reasonable compared with callback times in the rest of the facility and if it also appears to make it possible for the chaplain to minister to the majority of families, the 45-minute time frame is likely to continue.
However, if the facility's data indicates that the average family arrives within 15 minutes of a patient's time of death and leaves after spending an average of 35 minutes in the room, but the chaplain on call typically arrives 35 minutes after the patient's time of death and has, on average, only 10 minutes with the family, there clearly is an opportunity to greatly improve the quality of care offered at the bedside for the family of the deceased.
By reducing the callback time to 30 minutes and arranging for a room on-site where the chaplain waits during his or her on-call shift, you decrease the chaplain's average response time to 15 minutes and give him or her a secure place to stay, avoiding a drive to the medical center during rush hour or in the middle of the night. Having a call room in the hospital means that in many cases, the chaplain can be present in the patient's room to greet the family as they arrive.
The last major section of the input side of the chaplain staffing program asks about other duties the chaplain tends to in his or her ministry. The software program asks about time spent on some standard tasks and provides fill-in-the-blank space for others.
These hours will be calculated behind the scenes to translate to part of the total FTE package that then can be part of the discussion for what should be included in the pastoral care budget. (see Example 4).
After a brief look at leadership roles, we turn to the output page, which provides information for a second major discussion.
STAFFING BASED ON PATIENT ACUITY
Staffing based on the acuity of the patient has a long history within medicine. It is typically acknowledged that the sicker patients are, the more time and attention they require. Far more often than not, this is true not only of the medical treatment, but also of the pastoral interventions that have become an integral part of their overall care.
Thus, the tool looks to the same ratios that guide nursing care, but multiplies them to an appropriate level. Although a critical care nurse typically has a 1:2 ratio and would be assigned to two patients each shift, my own experience suggests that for a chaplain, the appropriate multiplier is 15, and that the typical chaplain — relieved of any other responsibilities for that day — reasonably could cover a 30-bed intensive care unit.
By using the nursing ratios you already provided, we can add a reasonable multiplier and determine a recommended number of chaplains to staff the medical center. As noted repeatedly, the intent is not to force a number here, but to invite another conversation between the director of pastoral care and senior leadership in order to arrive at what seems to be a fair number for staffing. Experience will tell if a midcourse correction is necessary.
In the staffing tool (see Example 5), each subsection leads towards a greater whole. The summary page (see Example 6) pulls together "current state" information and "best case" information to project a scenario for discussion.
The more diehard M*A*S*H fans among you might remember how the "Dear Sis" episode ends. The whole camp is suffering from Christmas blues and homesickness. Overhearing the sour Major Winchester talking about past Boston Christmases, Fr. Mulcahy secretly suggests that Radar contact the surgeon's family for Winchester's childhood tobogganing cap. Winchester is deeply touched. Weeping openly, he says to the chaplain, "You saved me, Father. You lowered a bucket into the well of my despair, and you raised me up to the light of day."
Perhaps it is time for a new day for us as well.
D.W. DONOVAN is director, mission and spiritual care at Providence Holy Cross Medical Center in Mission Hills (Los Angeles), California. If you would like to experiment with the staffing tool, please contact him at itsjustdonovan@gmail.com.
NOTES
- "Dear Sis" episode of "M*A*S*H," CBS television series. Season seven, episode 15, premiered Dec. 18, 1978. Written and directed by Alan Alda.
- "Dear Sis."
- Brian Smith, "Looking Back at a Decade of Collaboration with CHA," National Association of Catholic Chaplains website. www.nacc.org/vision/march-april-2017/looking-back-decade-collaboration-cha/.
- Jennifer W. Paquette, "Multiple Models Suggested for Determining Adequate Chaplain Staffing," Vision 23, no. 4 ( July-August 2013). www.nacc.org/vision/2013-jul-aug/multiple-models-suggested-for-determining-adequate-chaplain-staffing/.
- Tim Serban, Julie Jones and James Letourneau,
- "Models for Determining Adequate Staffing," PowerPoint presentation, National Association of Catholic Chaplains Annual Conference 2013. slide presentation: www.nacc.org/docs/conference/2013/M1-Presentation,%20Models%20for%20Determining%20Adequate%20Staffing.pdf.
