BY: PAMELA M. DUCHENE, PH.D., APRN, CNAA, ACHE
From the first moment I walked onto a nursing unit as a student, I knew this was the environment in which I wanted to work. Although nursing has not been a perfect employment situation, it has been a great career. It has always offered challenges for me and has continued to provide tremendous fulfillment.
So why would there ever be a shortage of nurses?
As a career, nursing shows much promise. The hours are flexible, the work is considered honorable and nurses are able to find jobs in most any location. For the past eight years, nurses were voted the most trusted profession for their honesty and ethical standards in the annual Gallup survey of professions.1
Though many consider nursing a calling, the work is filled with frustrations and difficulties. Nurses leave in significant numbers, citing poor working conditions. Nursing also has been called a profession that eats its young, one that results in many choosing to seek out less stressful opportunities.2
Though the economic recession has helped stabilize the nursing workforce in the short term as more nurses hang onto their jobs, add hours, put off retirement plans, etc., the national nursing shortage is expected to escalate to 500,000 by 2025, according to Dr. Peter Buerhaus of Vanderbilt University.3, 4 A change in workforce stabilization is only a positive trend if the nurses choose to stay because they enjoy their work, not because they lack other opportunities.
THE MAGNET RECOGNITION PROGRAM
The Magnet Recognition Program, through the American Nurses Credentialing Center (ANCC), is directed at attracting and retaining great nurses by creating environments in which nurses choose to practice.
At present, 350 organizations in the world have achieved Magnet designation, most of them in the United States. Of the 5,815 hospitals in the U.S.5, only about 6 percent are Magnet-designated.
The perception is that Magnet hospitals are an elite group. Magnet organizations are reported to have higher levels of quality, with stronger nursing satisfaction, richer RN ratios, fewer work-related injuries, lower mortality rates, fewer patient complications and higher overall patient satisfaction.6, 7 Some of these attributes may accompany nurse retention, but the Magnet program helps ensure the nurses retained are of the highest quality — those who are motivated and engaged, with a commitment to the organization, interdisciplinary collaboration and patient advocacy.
To be sure, the journey to Magnet is arduous and expensive, with those desiring to achieve it spending thousands of dollars for the application and process, including costs associated with making changes in programs, organizational structure and nursing benefits.
Within most Magnet organizations, nurses play a powerful role, with extensive involvement in committees, governance and organizational decision-making. Nurses are expected to be represented at the senior executive level and to be able to participate in organizational governance meetings. Although it is not a Magnet mandate, it would be almost impossible to achieve Magnet status without giving nurses a share in governance, thus an organization must be willing to support nurse attendance at committee and council meetings. This may be one of the most significant expenses of the process, given the cost of labor. It is, however, one of the most successful strategies behind the Magnet promise of higher nurse retention rates.
The Magnet application places a strong emphasis on nursing research, advanced practice, continuing education and strong staffing patterns. All of these require a healthy financial investment in nurses and nursing practice through continuing education and tuition reimbursement.
Magnet developed in response to a significant paradox. During an extreme national shortage of nurses in the 1980s, there were a few hospitals not clamoring for nurses — instead, they had lists of applicants clamoring to fill open nursing positions. A team of researchers from the American Academy of Nursing studied these 41 hospitals in 1983 and found key characteristics that correlated with an environment magnetic to nurses.8 These qualities became known as the Forces of Magnetism. They measure such things as the quality of nursing leadership; the hospital's organizational structure, personnel policies, management style and positive view of nurses; nurses' input, autonomy, accountability for the care they provide, access to clinical experts and continuing education opportunities.
In a recent study comparing 39 of the original Magnet hospitals with current Magnet organizations, many aspects of the original study held true.9 Nurses in Magnet organizations have a higher level of education, nurse-patient ratios are lower, the clinical environment is more likely to be characterized as autonomous, and quality of care is rated more highly. In the almost 30 years that have lapsed since the original study, the results continue to hold true: Nursing environments that reflect the magnet forces are ones in which nurses choose to practice.
AN UNLIKELY MAGNET
At St. Joseph Hospital in Nashua, N.H., we began our journey toward Magnet more than 11 years ago. We had a nurse turnover rate of 24 percent; more nurses were leaving than entering the organization. Peter Davis, our chief executive, suggested we consider becoming a Magnet organization.
The odds of attaining designation were against us. At the time, there were only 28 ANCC Magnet-designated hospitals in the country, most of which were teaching organizations, and only two were located in New England. How likely was it that our small hospital could achieve Magnet designation before the major teaching facilities would? Our nursing staff was predominantly diploma-prepared; we had significant leadership vacancies and there was no discernible interest in or evidence of nursing research within the organization. A change in each of these variables was essential for a successful Magnet journey.
We nevertheless hoped that aiming for Magnet certification would help us create an environment that nurses would never choose to leave. Davis' encouragement and endorsement was the first step. The second step was to develop a sense of empowerment within the nursing staff. In order to do that successfully, we needed to be certain that the organization would support the journey.
As I noted, our turnover rate in 1999 was a staggering 24 percent. The organization had just "demerged" from two other, larger hospitals that had received funding priority. St. Joseph Hospital was experiencing a rebirth, but it badly needed equipment, staff development and nurse leaders.
OPEN FORUMS
In a nursing staff satisfaction survey completed in May 1999, as a baseline for our Magnet journey, our nurses reported poor communication was the single most dissatisfying aspect of their work environment. Nurses said they seldom saw nurse leaders — logical, since there were few nurse leaders in the organization.
To address this, we decided to follow the Hewlett-Packard example described in the hugely influential business management book, In Search of Excellence — we would manage by walking around.10 We implemented open forums, monthly sessions held for all shifts, only to find they were sparsely attended because nurses were unable to get away from patient care. So I took the sessions to the nurses. With a traveling cart, and some snacks, I was able to capture the nurses' attention long enough to hear what was on their minds and to learn of their needs. The open forum system continues to this day.
Many, many changes within the system have resulted from this method of informal communication, including staffing questions and equipment and supply issues. During a recent open forum, for example, a nurse on the night shift expressed concern regarding a change in bed-making policy. The linen committee had recommended not using fitted sheets. This seemed like a good way to reduce costs on the psychiatric unit, since the patients were out of bed most of the day. The nurses on nights, however, had a totally different perspective, because they saw patients unable to rest comfortably — the flat sheets tended to come untucked. We corrected this change, thanks to the open forum system that gives nurses a way to communicate effectively and spontaneously.
SHARED GOVERNANCE
Although the Magnet application does not specify how to achieve shared governance, it is not possible to attain the designation without an empowered, engaged nursing staff who are integrally involved in organizational decision-making. This was a novel concept for St. Joseph Hospital. We decided to model ourselves after the system used at Rush University Medical Center in Chicago to give clinical nurses a voice in determining nursing practice, standards and quality of care.11
We got our first chance to try it when the nurse manager for the operating room happened to resign her position. Since there was little understanding of the operating room outside of that highly specialized clinical environment, it made great sense to start there, with a unit advisory committee formed to provide larger councils with input from operating room clinicians.
The system worked, and it has grown. Nurses throughout the organization are empowered to address practice issues and concerns, and they are integrally involved in decision-making. At St. Joseph Hospital, we have found shared governance and nursing satisfaction are directly linked. Nursing satisfaction levels have risen to the top quartile as monitored by the National Database of Nursing Quality Indicators.
No matter how the system is set up, leaders must be involved in the process. The point is to have shared, not delegated, governance. At St. Joseph Hospital, we follow these principles:
- Resist unilateral decisions. Leaders must avoid temptation to make quick decisions that affect staff.
- Schedule nurses to permit meeting attendance. Nurses can't be involved in decision-making if they can't be relieved of assignments in order to attend their committee or council meetings.
- Support the committees. Nurse leaders need to be involved in facilitating committees' work by helping to develop agendas, record actions and assure financial support, if possible, for decisions the committees make.
- Watch groups for signs they are on track. Councils can get into trouble through disorganization or apathy. Change is often difficult. Nurse leaders need to be ready to ask for assistance and identify strategies to help keep committees involved.
- Reinforce authority. Make sure decisions result from shared governance councils'/committees' recommendations, and give the council or committee credit and accountability for its decision.
NURSING SATISFACTION
We set as a goal never to give a nurse a reason to leave St. Joseph Hospital. We worked both to address long-standing satisfaction issues and to hardwire nursing satisfaction into all aspects of nursing leadership. Because surveys and turnover rates can empirically measure nursing satisfaction, St. Joseph Hospital took care to run surveys every six months until the organization enrolled in the National Database of Nursing Quality Indicators. By joining the database, the organization was able to participate in annual, national nursing satisfaction surveys that provide a comparison with other organizations across the country. Nursing satisfaction survey results also are part of nursing leadership evaluations, thus placing appropriate emphasis on satisfaction.
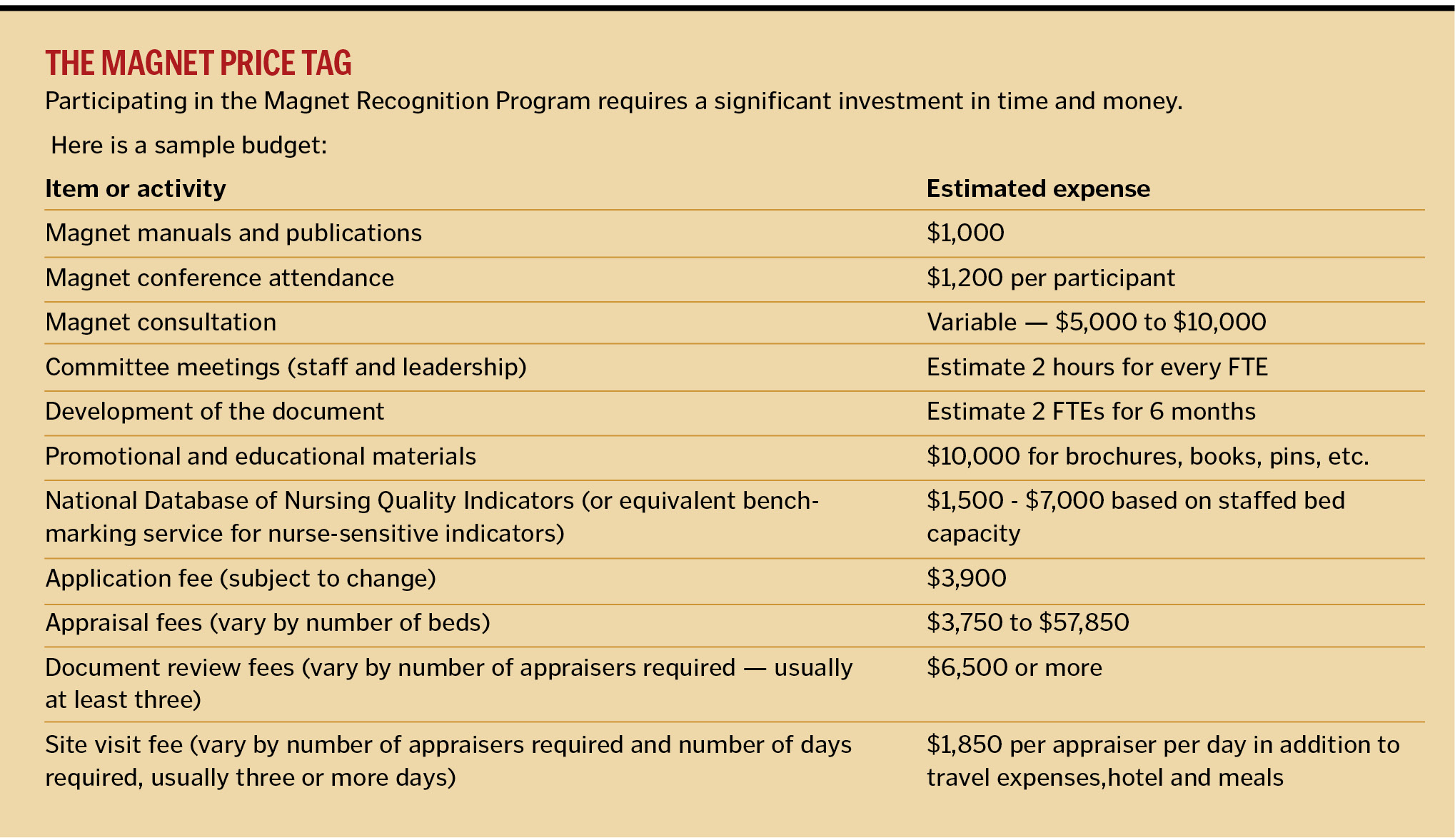
THE COST OF MAGNET STATUS
Pursuing Magnet certification is expensive. The firm costs of the program include thousands of dollars in fees for the application, appraisers and site visit. There also are many "soft costs" such as committee time and educational conferences that can easily exceed the firm costs.
Yet, at St. Joseph Hospital, our designation as a Magnet organization has resulted in many direct benefits to the hospital and to the community. Our nurse turnover rate is the lowest it has been in over 11 years, declining from 24 percent 11 years ago to 5 percent in 2009 (and trending down). From a time when we were losing more nurses than we hired, the average length of tenure has risen to 11 years, and last year there were more than 100 applicants for the 10 positions available in our nurse residency program.
These statistics directly affect the cost of care, since retention of experienced, satisfied nurses directly contributes to the patient-care experience. Our scores in patient satisfaction and quality continue to climb. It is relatively easy to implement improvements with a highly engaged nursing staff that is committed to the organization's mission.
Nurses will go the distance to assure that patient needs are met, both within the hospital and in the broader community, and are asking how they can make an even stronger impact on patient care. That goes a long way toward assuring that the organization is able to achieve its intended mission.
As Margaret Mead stated, "Never doubt that a small group of thoughtful, committed citizens can change the world. Indeed, it is the only thing that ever has." The true value in the Magnet Recognition Program is in the journey and the culture it creates, through which nurses realize they can change their world and the world of their patients. A hospital that creates a Magnet environment assures that nurses will remain in nursing practice and that patients will never lack a great nurse at their bedside.
PAMELA M. DUCHENE is vice president and chief nursing executive at St. Joseph Hospital, Nashua, N.H.
NOTES
- American Nurses Association, "Gallup Poll Votes Nurses Most Trusted Profession," www.nursingworld.org/FunctionalMenuCategories/MediaResources/PressReleases/2009-PR/Gallup-Votes-Nurses-Most-Trusted-Profession.aspx
- M. Rowe and H. Sherlock, "Stress and Verbal Abuse in Nursing: Do Burned Out Nurses Eat Their Young?" Journal of Nursing Management 13, no. 3 (2005): 242-248.
- P. Buerhaus, et al., The Future of the Nursing Workforce in the United States: Data, Trends and Implications (Boston: Jones and Barlett, 2009).
- American Association of Colleges of Nursing, "Talking Points: Impact of the Economy on the Nursing Shortage," www.aacn.nche.edu/Media/pdf/TalkingPoints.pdf.
- American Hospital Administration, "Fast Facts on U.S. Hospitals," www.aha.org/aha/resource-center/statistics-and-studies/ fast-facts.html.
- L. H. Aiken, "Superior Outcomes for Magnet Hospitals: The Evidence Base," in M. L. McClure and A. S. Hinshaw, eds., Magnet Hospitals Revisited: Attraction and Retention of Professional Nurses (Washington, D.C.: American Nurses Publishing, 2002).
- K. Drenkard, "The Magnet Imperative," The Journal of Nursing Administration, 39, no. 7/8 (2009): S1-S2
- American Nurses Credentialing Center, "Forces of Magnetism," http://www.nursecredentialing.org/Magnet/ProgramOverview/ForcesofMagnetism.aspx.
- L. Aiken, D. Havens and D. Sloane, "The Magnet Nursing Services Recognition Program: A Comparison of Two Groups of Magnet Hospitals," Journal of Nursing Administration 39, no. 7/8, (2009): S5-S14.
- T. Peters and R. Waterman, In Search of Excellence: Lessons from America's Best-Run Companies (New York: Warner Books, Inc., 1982).
- H. Shidler, M. Pencak and S. McFolling, "Professional Nursing Staff: A Model of Self-Governance for Nursing," Nursing Administration Quarterly 13, no. 4 (1989):1-9.
American Nurse Credentialing Center Magnet-Recognized Organizations
CHA MEMBER ORGANIZATIONS
Alegent Health Mercy Hospital
Council Bluffs, Iowa
Avera McKennan Hospital & University Health Center
Sioux Falls, S.D.
Bon Secours Memorial Regional Medical Center
Mechanicsville, Va.
Bon Secours St. Mary's Hospital
Richmond, Va.
CHRISTUS Hospital – St. Elizabeth
Beaumont, Texas
CHRISTUS-St. Mary
Port Arthur, Texas
Carondelet Health – St. Joseph Medical Center
Kansas City, Mo.
Carondelet Health – St. Mary's Medical Center
Blue Springs, Mo.
Good Samaritan Hospital
Dayton, Ohio
Holy Cross Hospital
Fort Lauderdale, Fla.
Holy Name Hospital
Teaneck, N.J.
Mercy Health Center
Oklahoma City, Okla.
Mercy Hospital
Miami, Fla.
Mercy Medical Center, Dubuque
Dubuque, Iowa
Our Lady of Lourdes Memorial Hospital, Inc.
Binghamton, N.Y.
Our Lady of the Lake Regional Medical Center
Baton Rouge, La.
Providence Holy Cross Medical Center
Mission Hills, Calif.
Providence Portland Medical Center
Portland, Ore.
Providence St. Vincent Medical Center
Portland, Ore.
Saint Elizabeth Regional Medical Center
Lincoln, Neb.
Saint Joseph's Hospital of Atlanta
Atlanta
Saint Joseph's Hospital/Ministry Health Care
Marshfield, Wis.
Saint Joseph's Regional Medical Center
Paterson, N.J.
Seton Medical Center Austin
Austin, Texas
Seton Northwest Hospital
Austin, Texas
St. Alexius Medical Center
Bismarck, N.D.
St. Cloud Hospital
St. Cloud, Minn.
St. Elizabeth Health Center of Humility of Mary Health Partners
Youngstown, Ohio
St. Elizabeth Medical Center
Edgewood, Ky.
St. John Medical Center
Tulsa, Okla.
St. Joseph Health Center of Humility of Mary Health Partners
Warren, Ohio
St. Joseph Hospital
Nashua, N.H.
St. Joseph's/Candler – St. Joseph's Hospital
Savannah, Ga.
St. Peter's Hospital
Albany, N.Y.
St. Peter's University Hospital
New Brunswick, N.J.
UPMC St. Margaret Hospital
Pittsburgh
Wheaton Franciscan – St. Joseph Campus
Milwaukee
