BY: MEGAN MAHNCKE, MA
Almost a year ago at SCL Health, we launched an assessment of philanthropy across the organization. When it comes to fundraising, here's the vital question: "Are we raising as much money as we possibly can?"
Sometimes people feel squeamish about linking money and ministry, even though intellectually they know better, and even though history has shown them the way. For example, in our health ministry, philanthropy always has played a significant role. The Sisters of Charity of Leavenworth were our first fundraisers; they persistently raised money to build sites within our organization that now comprises 11 hospitals and includes ambulatory centers, home health care, hospice, mental health and safety net services across Kansas, Colorado and Montana.
As the transition from sisters to lay administrators took place over the past several decades, the role of philanthropy shifted, too, often becoming an afterthought buried amid larger hospital operations.
For those of us who have spent our careers in fundraising, we know there are important underlying questions to be answered and best practices that need to be in place before you can gauge the effectiveness of philanthropy. You need to know: 1) How efficiently are you raising current dollars? 2) Have you invested in the appropriate infrastructure and staff? and 3) Have you focused time on the most impactful programs, namely, major giving as opposed to events?
GATHERING DATA
At SCL Health, these questions spurred our evaluation and drove us to create a strategic approach that would transform philanthropy throughout the ministry. As we began to gather financial data to understand where each of our foundations stood, we quickly realized we were not comparing apples to apples.
We had nine different staffing models using six different kinds of database software and encountered great variations in financial reporting and definitions. Each foundation was isolated from the others, regardless of geographical proximity. There was limited collaboration, meaning basically no exchange of knowledge or best practices, and individual hospital foundations often were approaching the same funders. We couldn't put together a meaningful report that would inform our health system board and leaders how effective our fundraising was.
It became clear that we needed outside experts to help us evaluate each foundation and to attempt to compile data in a standard format with comparable categories. Only then could we set a benchmark for each foundation and roll up data for review at a system level. We chose a third party to examine each foundation's return on investment, staffing structure, board management and development, alignment with senior management of each hospital and overall impact to mission.
We surveyed donors, board members, hospital leaders and foundation teams to gain a full understanding of how our foundations were perceived and then compared that information to performance at each site. The process took almost six months from start to finish. The outcome was a detailed, comprehensive report of recommendations divided into actions that were system led, regionally led and led by the local care site. The first overarching recommendation we took action on was establishing a chief development officer position for the health system — the position I now hold — to support and elevate philanthropy across all of our regions.
STRENGTHS AND WEAKNESSES
The assessment's overall findings and observations indicated our strengths at SCL Health Foundations include high patient satisfaction for our hospitals — a key indicator of both current success and potential fundraising opportunity. Patients satisfied with the care they have received are much more likely to give back and to advocate for your hospital within the community.
Another key strength was our strong community volunteer leadership within hospital and foundation boards. On the financial side, we saw an upward trend over the preceding several years and a 7 percent increase in philanthropy over the preceding two years. The assessment also pointed to some successful existing programs, including associate giving, grants and low-cost, high-return events.
The findings revealed that our greatest need was to dramatically increase collaboration and use of shared intelligence among our foundation teams. We also learned there were areas of opportunity to improve unrealized philanthropic potential based on a community capacity assessment.
SHIFT IN FOCUS
The recommendations and findings showed SCL Health needed to shift its focus to building or strengthening high-return programs, such as major giving, gift planning and grateful patient giving. We learned many of our foundations had spent the majority of their efforts on grants, soliciting SCL Health associates, and putting on fundraising events. All three are necessary components to a robust fundraising program, but they are not sustainable without the major giving component. We also discovered that we needed to engage our physicians in order to increase grateful patient referrals. Physicians and nurses are the first to build a relationship with a patient and their family. It is important for them to understand the impact of hospital foundations so they can endorse and refer grateful patients. We had not spent the time to educate our larger physician community on the impact of our foundations, nor had we taught them how to connect patients to us directly.
Another area of weakness was the lack of metrics for philanthropic work. Foundations were a small line item in the large hospital consolidated financials. There were no consistent measurements or benchmarks for our fundraising operations that would allow us to determine success or failure.
RECIPE FOR FOUNDATIONS
These high-level strengths and weaknesses helped us prioritize the first course of action: getting the nine foundations to work together so that each one could be more successful. Drawing on my experience raising money in large systems within health care and higher education, I knew we needed to maintain a high level of autonomy at the hospital foundations, and we needed to improve the business functions that support fundraising and stewardship. We needed to increase accountability and share best practices for fundraising, consistent reporting and metrics to all of our foundations.
I engaged with each foundation leader to determine and understand what strategies and tactics needed to remain local and what support could be provided at the system level. We determined that each hospital would retain autonomy by having its own board, local fundraising priorities set by hospital leadership and boards, and retention of all dollars raised.
Most importantly, we discovered the foundations needed more time to focus on community relationships. Our foundations ranged in staffing from teams of two to 12, but no matter the size of the team, each was responsible for everything from gift processing to raising major gifts. It became apparent that if we could provide "back of house" support and resources at a system level, the foundations could concentrate on the "front of house" duties, i.e. fundraising, board management and successful events that are the direct business of raising money in individual communities.
At the system level, we created supportive efficiency by taking on the functions for accounting and finance, converting to one single donor database, annual fund and grants strategy. By relieving our foundations of some of the administrative work, they are able to focus and pay the appropriate attention to donors while still having the autonomy they need to build a unique relationship with their community. Over time, each foundation will be able to shift focus to major and planned gifts.
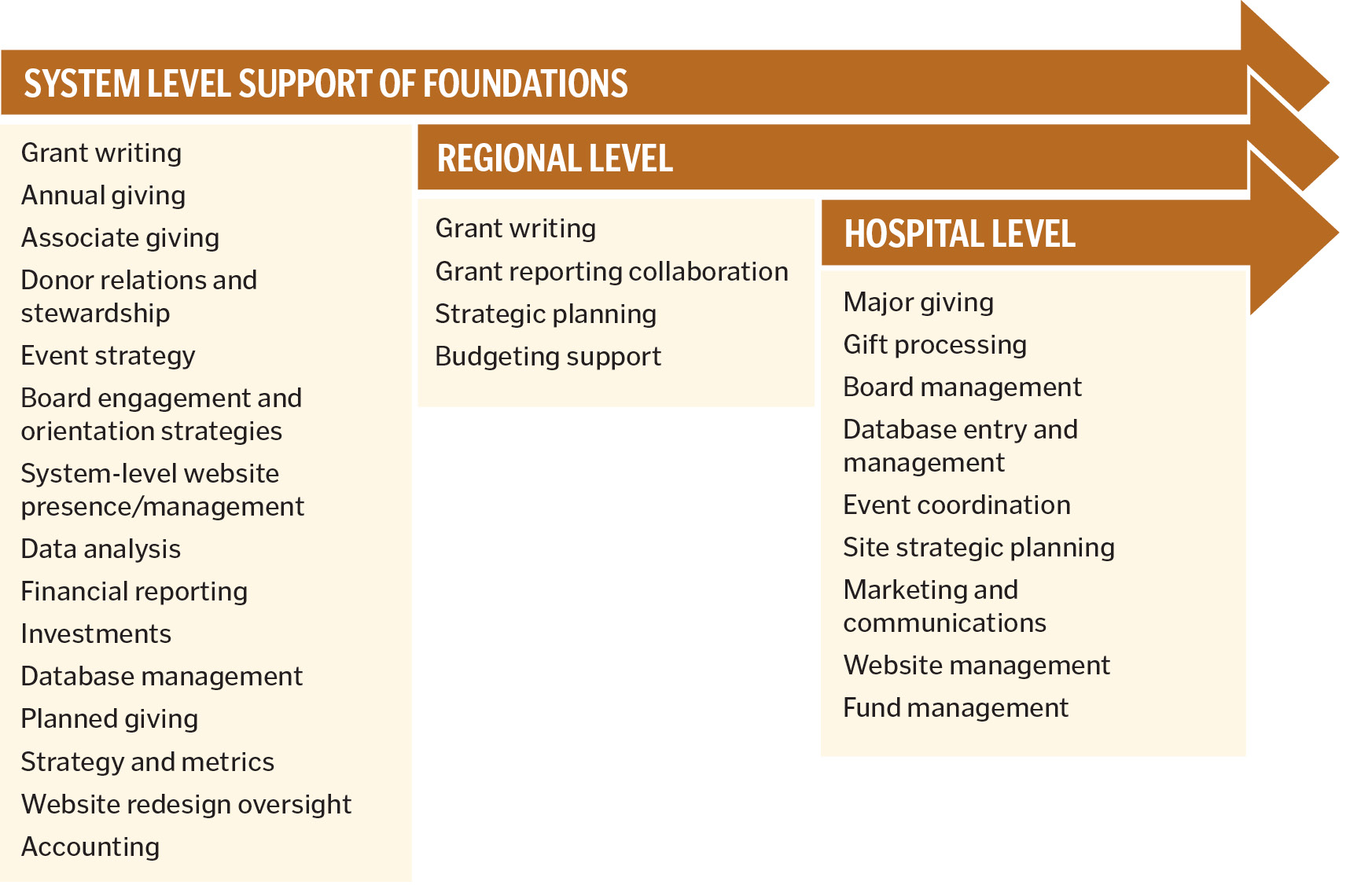
LEVELS OF SUPPORT
Fundraising is based on internal organizational relationships, relationships with donors and the overall relationship that hospitals have within the community. Our undertaking was designed to provide system-level support for back-office activities that had been handled at the local care sites without disrupting successful local practices and processes already in place.
I assembled a small team to review every function or lack of function within our foundations to determine which level of support would improve our ability to raise more money. We asked these questions before each step:
- Can this function or recommendation be implemented at a system level? If yes, why is this a better solution for improving philanthropy?
- Should this function/recommendation be implemented at a regional level? If yes, why is this a better solution for improving philanthropy?
- Does this function/recommendation need to remain at the local care site?
- In the business of philanthropy, we base everything we do on the relationships we have with our donors and the overall community. We cannot raise the necessary support if we do not cultivate and steward these relationships in and outside our organizations.
It takes many hours, even years, to cultivate donors who support our healing mission. The competition grows annually for philanthropic dollars as more and more nonprofits start up within the communities. The competitive environment demands us to become even more accountable and transparent regarding the exact impact the donors' dollars are having on the work they are supporting. We owe it to our patients and donors to ensure efficiency in the back-of-the-house operations so that we can direct dollars to the cause with as little overhead cost as possible.
REPORTING BENCHMARKS
To that end, SCL Health now has nationally recommended benchmarks to which we would hold each foundation annually accountable:
- Cost per dollar raised
- Gift income per full time employee
- Gift income per salary dollar
These simple data points help us focus on how efficiently we are raising money. None of the benchmarks is new, but it was a culture shift to report the numbers on a regular basis, and it created transparency and accountability for each foundation. Some foundations' board members were shocked to discover it was costing more than a dollar to raise a dollar. Others were impressed to see how a small team had been raising millions.
With these data points and the insights and perspectives gained from our assessment, all foundation leaders, foundation boards of directors, hospital leaders and system executives reviewed the recommendations on how to improve fundraising throughout SCL Health.
I worked with many leaders throughout the health system to come up with a two-year plan. Its key priorities were to increase philanthropy and efficiency, build infrastructure and develop programs, and we assigned goals and strategies to each priority.
CONCLUSION
It took hours of relationship-building and discussion to improve how we are raising money within our health system. These conversations were made possible by our shared mission and values — we are here to raise the greatest amount of money and support for the hospitals to provide excellent patient care. Starting with this shared premise allowed us to elevate our conversations to focusing on possibilities of improvement versus control of function. The other critical component is the investment and support from the top executives, including the health system board.
Too often in large nonprofits like health systems or universities, we move to implement efficiency but sacrifice truly improving the quality of the work, or, in this case, the amount of support we are receiving from our communities.
We have discovered that as you shift focus, there are gaps in skills that need to be addressed. As much of our work is based in the community, we also are learning of the need to improve the culture of philanthropy throughout our system. Every aspect of health care is evaluated on a certain standard of metrics. It became clear to us that we needed to create a standard set of metrics that we report on monthly to our leaders to show philanthropy's impact and to prove that it has strategy-driven outcomes like anything else in health care.
So far, this work has resulted in creating a culture of shared knowledge among philanthropic leaders. Metrics are driving a culture of major giving and transparent fundraising outcomes, both internally and externally. We have found efficiencies in working together so that we can deliver greater impact for the philanthropic dollars that are invested in our SCL Health hospitals across Colorado, Montana and Kansas.
MEGAN MAHNCKE is vice president, chief development officer for SCL Health, Denver.
