BY: ALAN ZUCKERMAN
Mr. Zuckerman is director, Health Strategies & Solutions, Inc., Philadelphia.
"Catholic Healthscan 2004" Reveals the Views of 175 Ministry Leaders
No providers are exempt from the enormous difficulties facing U.S. health care, but Catholic organizations face special challenges. Dwindling memberships of sponsoring congregations; problems involved in balancing values and financial performance; and uncertainties concerning emerging genomic medicine, on one hand, and end-of-life issues, on the other-all these continue to dominate the agendas of the nation's largest group of not-for-profit health care organizations.
What are the most important issues likely to affect Catholic hospitals over the next five years? In 2004, CHA and Health Strategies & Solutions, Inc., a Philadelphia-based management consulting firm, conducted a survey called Catholic Healthscan 2004. Our survey was intended to accomplish three objectives:
- Identify the degree of concern among executives in Catholic health care about the key current and future challenges
- Clarify the nature of each challenge and discuss potential approaches to employ in addressing it
- Encourage study and dialogue about successfully managing the most important challenges
Having received input from an advisory panel of 13 senior executives of Catholic health care organizations, we selected 25 critical issues for the survey, which employed a seven-point Likert scale. We then solicited survey responses from some 650 people, representing each of CHA's member hospitals and systems. We received 175 responses, a 27 percent response rate.
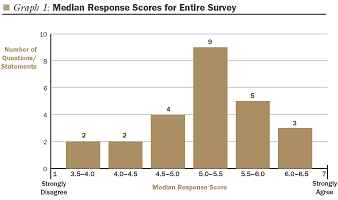
Our survey questions were posed in the form of statements to which we asked respondents to say whether (and how strongly) they agreed or disagreed. Five general themes seemed to emerge:
- Economic/financial issues
- Legislative/regulatory issues
- Physician/staffing issues
- Capital needs/growth issues
- Catholic-specific issues
Although most of the issues cited were of great importance to survey respondents, they revealed exceptionally strong agreement in their responses to three particular predictive statements:
- U.S. employers will compel employees, dependents, and pre-Medicare retirees to share an increasing amount of the costs of their health benefits through higher copayments and deductibles and/or shift to defined contributions (6.28 median score).
- State and federal budget deficits will result in Medicare and Medicaid payments falling further behind health care cost increases (6.06 median score).
- Hospitals with access to capital will build replacement hospitals and ambulatory
care facilities and acquire the latest technology; hospitals without access
to capital will fall further behind their competitors (6.06 median score).
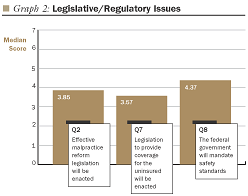
Conversely, two statements generated strong disagreement, suggesting that survey respondents see little likelihood of government action: - Concerns about the medically uninsured will result in legislative reform to provide coverage for the large majority of this group (3.57 median score).
- Effective malpractice reform legislation that sets limits on awards will be enacted (3.85 median score).
None of the seven statements in the Catholic-specific section of the survey generated agreement or disagreement as strong as those in the other sections. The strongest agreement (5.68 median score) was elicited from the statement "Strong financial skills will be as important as Catholic values in selecting future executives and senior managers of Catholic health systems." The strongest disagreement (4.37 median score) came in response to the statement "Catholic health systems will expand by adding more elements of the continuum of care to efficiently and effectively move the growing volume of patients through the system."
Economic/Financial Issues
Gradually improving financial performance, in both the general economy and the
health care sector of it, has not allayed concerns generated by years of turbulence.
"Vulnerable" is the word that best describes health care providers,
according to our survey's respondents. They forecast, over the next three to
five years, worsening state and federal budget deficits, increasing consumer
responsibility for payment of health insurance and services, and further deterioration
of margins.
However, although respondents are cautious in their outlook, they seem to be optimistic in their behavior; the survey shows a "disconnect" here. Respondents are, for example, dramatically escalating their capital spending in reaction to rising patient-care demands. And they forecast continued high levels of capital spending over the next three to five years. Time will tell whether survey respondents are being overly aggressive or exercising the right balance of fiscal conservatism and sound growth strategies.
Legislative/Regulatory Issues
In recent years, the federal government has focused narrowly on Medicare reform
and prescription drug costs. At the state level, budget deficits have dampened
activism. Survey respondents are pessimistic about the likelihood of broad-based
legislative initiatives in the areas of malpractice reform, coverage of the
uninsured, and the establishment of safety standards. Survey questions concerning
these issues yielded the lowest median scores and the least agreement about
the likelihood of action in the next five years.
Physician/Staffing Issues
After the downsizing efforts of the late 1990s, today's labor shortages have
caught most hospital leaders by surprise. Declines in job satisfaction among
nurses and physicians, caused in large part by compensation constraints and
deteriorating work environments, are-when combined with the shortages of physicians
and nurses-creating crisis situations for many providers. Survey respondents
tended to agree that physician and staffing issues could translate into a national
crisis, particularly for emergency-department services.
Respondents also expect deterioration in hospital-physician relationships because of increasing head-on competition between them (as indicated by a median response score of 5.27). On the other hand, many respondents were hopeful (median score 5.80) that hospitals will engage physicians in quality initiatives and a culture of service excellence.
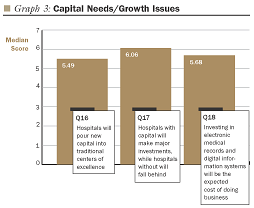
Capital Needs/Growth Issues
After more than a decade of volume declines and downsizing, hospital volumes
began to rebound at the turn of the new century and have shown strong growth
since. Financial performance improvement appears to have led to a capital spending
boom among survey respondents, with healthy increases forecast for the next
five years. The need to maintain and improve bond ratings, cited as very important
by respondents, may have a chilling effect on spending. Our respondents (by
a median score of 6.06), together with many experts in the field, believe that
capital access will divide U.S. health care into "haves" and "have
nots," leaving those without needed capital to wither, expire, or be absorbed
by stronger organizations.
Catholic-Specific Issues
Seven questions in the survey focused on issues of particular concern to Catholic
providers. Our respondents seemed to take these challenges-involving genomics
and other technological advances, the decline in membership of sponsoring congregations,
the balancing of values and financial performance, and caring for the indigent-in
stride. None of the agree/disagree questions in this section of
the survey generated as much agreement or disagreement as those in other sections.
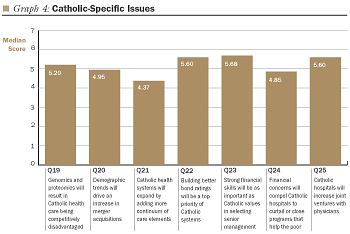
Respondents' particularly strong responses to financial performance and position questions indicate that fiscal issues remain at the top of their list of concerns. The survey responses suggest that the key concerns of Catholic and other-than-Catholic organizations are similar. Executives in Catholic health care appear reasonably confident that they can handle the special challenges they face, although their varied responses to a survey question about curtailment of services to the poor may indicate some ongoing concern about managing what for them is a core mission.
Looking Ahead
The Catholic Healthscan 2004 survey results indicate that financial challenges
are respondents' number one concern. Reimbursement shortfalls, rapidly escalating
costs, and the increasing burdens of indigent care create a confusing puzzle
with possibly devastating consequences, all aggravated by a growing need for
capital and possible difficulties in gaining access to it.
Physician relationships rank as the second highest issue of concern, based on survey responses. Physician ventures that directly compete with hospitals, the increasing pressure on physician incomes, declining morale and professional satisfaction, and the accompanying drift of physicians away from hospitals-these will add up to monumental challenges for all hospitals and systems. Shortages of other health care workers will only further aggravate the situation.
Although survey respondents express some confidence in their ability to manage mission commitments and ethical issues, they expect new challenges to arise; an example is the March 2004 papal allocution on patients in a persistent vegetative state.1 The next five years will be a watershed period for Catholic providers, respondents suggest. Closures, consolidations, and other complex and difficult decisions are inevitable as providers adapt to harsh financial realities. But they also see great opportunities for Catholic health care organizations in addressing such issues as the nation's growing uninsured population, quality and safety standards, physician-hospital relationships, and developments that have ethical consequences.
Catholic Healthscan 2004: A National Survey of Health Trends Affecting Catholic Health Care Organizations from 2004 to 2005, St. Louis, 2004, is available from CHA, 4455 Woodson Road, St. Louis, MO 63134 ($10 members, $20 nonmembers).
NOTE
- Pope John Paul II, "Life-Sustaining Treatments and the Vegetative State: Scientific Advances and Ethical Dilemmas," March 20, 2004, available at www.vatican.va/holy_father/john_paul_ii/speeches/2004/march/documents/hf_jp-ii_spe_20040320_congress-fiamc_en.html.
SURVEY SNAPSHOTS
Health Strategies & Solutions saw Catholic Healthscan 2004 responses as
predicting the following over the next five years:
Economic/Financial Issues
- Another significant industry downturn will occur.
- More hospital closures and consolidations will occur.
- Major changes in payment mechanisms are likely.
Legislative/Regulatory Issues
- Reimbursement reform is likely, with continuing budget deficits that will in turn cause across-the-board reimbursement cuts.
- Possible federal legislative priorities include patient-safety regulation and the creation of incentives seeking to increase the number of medical and nursing school graduates.
Physician/Staffing Issues
- The physician and nurse shortage crisis is likely to grow worse.
- Quality improvement initiatives will develop slowly unless physicians are compensated for these efforts.
- There will be a continued migration of outpatient services to physician offices; physician-hospital joint ventures will increase.
Capital Needs/Growth Issues
- Increased capital spending by strong providers will help accelerate the decline of already vulnerable hospitals and systems.
- Rapid capital expenditures will weaken even the strongest hospitals and systems; health care, an overleveraged sector of the economy, will see a decline in financial performance and creditworthiness by 2009.
Catholic-Specific Issues
- Increasing turbulence will occur, with fewer, but larger, hospitals and systems remaining.
- Major organizational redirection will be necessary to offset competitive threats from for-profit firms and physicians.
- Managing moral and delivery-related challenges from proteomic and genomic therapies will be become more difficult.
- One or two major sponsoring congregations may relinquish day-to-day responsibility for system operations.
