BY: JOYCE BATCHELLER, RN, and KAREN BURKMAN, RN
As a Healthcare Network Expands, Nurses Play Key Role in Developing Practice Management
Ms. Batcheller is senior vice president/network chief nursing executive, and Ms. Burkman is director, nursing practice, Seton Healthcare Network, Austin, TX.
Fueled by a booming economy and explosive growth of high-tech business, Austin and the central Texas region have enjoyed a growth rate among the highest in the nation for several years. The Seton Healthcare Network's own growth has accompanied this surge. In 1994 the network consisted of two acute care facilities and a clinic for the working poor in Austin. Seton now encompasses a regional complex of 30 sites located throughout the greater Austin area and the surrounding rural communities. An ambulatory care center and another community clinic are scheduled to open in late 1999 and early 2000.
The growth of the Seton network has presented a new set of challenges to the nursing management team. Nursing leaders have had to find a way to coordinate nursing practice among 2,600 nurses in a complex, evolving, and geographically dispersed system, while giving them a professional identity and a sense of being part of a team.
Coordinating Mission, Values, and Nursing Practice
To successfully align the nursing practice with the mission, philosophy, values, and goals of Seton, nursing leaders focused on the following areas:
- Communication across the network. With a single chief nursing executive and one board of trustees for the entire network, we knew managing communication across a multicounty network would be a challenge.
- The lack of shared values and philosophies between cultures. In 1995 Seton leased two public facilities, Brackenridge Hospital and Children's Hospital of Austin, from the city of Austin. Merging the public hospital culture with the Catholic not-for-profit culture proved to be a challenge. At the same time, we had to address staff fears for job security and the maintenance of benefits.
- Structural inconsistencies across sites. Although Seton's organizational chart has changed several times in the past five years, its structure has remained relatively flat. In contrast, some facilities that joined the network had many structural layers. Nursing leaders' titles and responsibilities varied from site to site.
- Ways to foster "team spirit." With multiple sites in distant locations, it was important to establish a sense of community and identity among the nurses.
- Variation in practices. Variations were an obstacle to flexible staffing among the 30 network sites. Without consistency in nursing practice, a uniform level of care would be virtually impossible to attain. Rather than focusing on differences, we wanted to build on what we had in common.
Early on, we began developing a shared nursing philosophy and a framework for what has become Seton's network nursing shared governance model. We knew that shared values, a consistent nursing philosophy and practices, and a uniform clinical ladder for the four Austin hospitals would be the keys to successfully integrating new sites. We believed that enhancing professional identity was the key to integrating care delivery. Professionals tend to align with the values, practices, and culture of their group rather than with the overall organization.
The Nursing Executive Committee
We ultimately built a four-component governance model, consisting of a Nursing Executive Committee, the Nursing Congress, eight specialty councils, and support councils (see "Shared Governance Model" below).
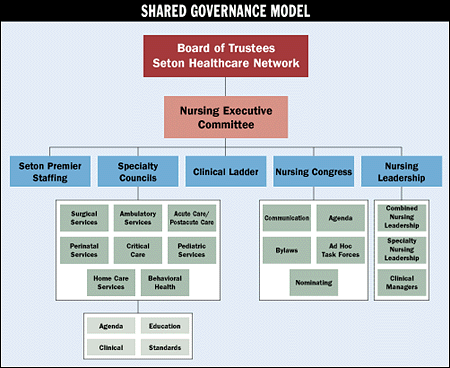
At the helm of our nursing governance is the Nursing Executive Committee (NEC), which provides strategic and operational direction for nursing and integrates processes for improved alignment and empowerment into the practice environment. Chaired by the chief nursing executive, the NEC works through the Nursing Congress and the specialty councils. The NEC also works collaboratively with network medical executive committees and the Clinical Quality Committee of the board, which oversees quality improvement activities.
The Nursing Congress
In May 1996 the Nursing Congress was formed to define, promote, and evaluate nursing practice and ensure consistent nursing practice and standardization across the network. We began by focusing on what we had in common across facilities.
Integral to the shared governance approach, the 65-member Nursing Congress draws participants from every constituency of the nursing environment to ensure that clinical decisions are made at the point of care. Congress members represent a defined constituency, and every nurse in the network may participate in decision making through his or her representative. In addition, 15 representatives from various other disciplines, as well as experts from infection control, materials management, human resources, and other areas, serve on the congress. The point is that we have all key stakeholders participating in the congress to make timely, collaborative, and informed decisions about patient care.
The congress meets monthly for no more than an hour and a half. Meetings are designed as executive sessions; hands-on work is carried out by task forces and councils. Each month at the congress meeting, the chief nursing executive gives an NEC and practice update. Meetings are open to staff members from the represented disciplines. Guests may participate, but only congress members may vote.
Standing Committees
Standing committees carry out much of the Nursing Congress work. They are:
- Communication Committee. This committee creates and maintains communication tools (such as informational notebooks) for constituents and coordinates ongoing evaluations of the communication process. A congress communication team developed a process to identify and communicate roles and responsibilities for congress specialty council representatives, their constituency members, and department leaders.
- Agenda Committee. This committee ensures appropriateness and readiness of agenda items. Requests for feedback or decisions on agenda items are based on the defined scope of the congress.
- Nominating Committee. Officers serve one-year terms; representatives, two-year staggered terms. The congress's officers and parliamentarian usually come from different sites and specialties. The chair and vice chair of the congress are NEC members and attend network leadership retreats.
- Bylaws Committee. The Bylaws Committee developed the initial bylaws and updates them as needed.
- Ad Hoc Task Forces. These groups, limited to five task forces at a time, have been key in the development of new initiatives. For instance, one task force did a study of supply purchases; implementation of its recommendations resulted in a $500,000 savings for the network.
Scope of Governance
The Nursing Congress focuses its attention on practice issues that affect more than one specialty. For example, in one case the congress found that we had a policy and procedure that required two people to check insulin injections. Investigation showed it to be a long-standing, national nursing practice that had not been updated since the 1950s. We have now adopted new procedures for insulin administration in acute care, home care, and primary care settings that save staff time while not diminishing the quality of care.
Congress also provides feedback on other issues outside the scope of its decision making, such as human resources or administrative concerns. For instance, representatives have been asked to give feedback on the cross-campus floating guidelines.
Caucuses are another valuable avenue for input from the congress. Topics addressed at the caucus level include how to improve patient, staff, and physician satisfaction; issues the NEC and congress should focus on when developing annual goals; representatives' educational needs; and clinical ladder processes. Caucuses also provide a forum for feedback on priorities.
From Congress to Specialty Councils
By summer 1996, the Seton Nursing Congress was well under way. The next step was establishing seven specialty councils, whose scope includes issues that affect more than one department within that specialty across the network. Councils represent surgical services, ambulatory services, acute care/postacute care, perinatal care, critical care, pediatrics, and home care. When a behavioral health facility joined the network, a specialty council on behavioral health became the eighth council in March 1999. Functioning essentially like the congress, the councils are composed of representatives with regulatory and practice similarities.
Like the congress, the specialty councils have a voice up the chain of command within the Seton network. The liaison director is the councils' spokesperson on the NEC. The chairs of the councils also report quarterly to the NEC. Their reporting schedule aligns with that of Seton's board of trustees, so quarterly reports can be incorporated into the chief nursing executive's report to the board.
Support Councils
Six support councils form the fourth spoke in the shared governance wheel. They provide a process for alignment within the network, support to the staff, mentorship, and organizational navigation. Support councils represent each major process and play a valuable role in eliminating barriers to projects' completion.
Four support councils — practice, operations, organizational development/education, and quality management — have representation on the NEC, Nursing Congress, and specialty councils. Representatives from information systems and research are members of the Executive Committee and serve as ad hoc consultants to the congress and specialty councils.
Evaluating Success
From the outset, we focused on outcomes to demonstrate value, particularly since we expected the model could be perceived as a costly undertaking (see "Supporting Positive Outcomes" below). Among our evaluation tools, we rely on staff measurements, clinical indicators, and customer satisfaction surveys of both patients and medical staff. In light of the growth and cultural differences throughout the network, we were pleased with the results of our 1999 communication survey, in which we asked the nursing leaders and staff to rate the effect shared governance has had on the nursing practice environment at Seton. Their responses indicated a distinct preference for the shared governance model over previous models of leadership. They also rated it highly for providing a consistent vision among nursing leaders, increasing their sense of connection to the network, increasing the consistency of nursing practice, and making decision making collaborative.
SUPPORTING POSITIVE OUTCOMES
Changes implemented by Seton's nursing practice shared governance model enable the delivery of high-quality nursing care across the network.
- One clinical ladder. In the past, we had two philosophically different clinical ladders. In 1996 a team of nurses developed an outcome-driven clinical ladder that recognizes significant accomplishments. It is being evaluated for non-acute care specialties.
- Standardized nursing leadership. After the addition of new facilities over the past five years, there were six different nursing leadership titles and a wide variation among organizational charts. The NEC standardized the organizational charts, decreased the number of layers, and made titles and job descriptions consistent across the network.
- Redesign. Through time studies, we identified the four top time-consuming activities — documentation, communication, medication administration, and activities of daily living — and consequently initiated several major work redesign initiatives. Today, redesign thinking is incorporated into all our work.
- A staffing center. With network growth came distinctly different staffing philosophies, making staffing the network's 30 sites inefficient and expensive. We created Seton Premier Staffing Center, an internal employment agency that currently employs 180 RNs, LPNs, assistive personnel, and RRTs. The center enables us to offer higher salaries, since we bypass the fees normally paid to recruitment firms and pass those savings on to the employees. At the same time, we maintain better quality control and ensure consistency of care across our sites.
- Reduced documentation time. Coordinating documentation was a challenge, as each site had its own forms. A steering committee led the process to reduce and standardize nursing documentation, which resulted in substantial cost savings to the network. In medical-surgery areas, for instance, documentation time fell by almost half, saving $33 per shift per nurse.
Another of our key measures — patient satisfaction — has improved since implementation of the shared governance model. Measured weekly, quality of care and service inpatient ratings climbed slowly but steadily in all four of the Austin hospital sites from July 1997 through December 1998.
Physicians also perceive an improvement in the hospital environment with regard to nursing. This year almost three out of five physicians rated nurses' efficiency and accuracy in carrying out physician orders excellent or very good, a 31 percent improvement over the baseline period. A letter to the medical staff from the president of the network's medical executive committee directly credited the Nursing Congress in identifying barriers to improvement in this area.
Lessons We've Learned
As Seton's nursing leaders, we have learned to involve the people whose work will be affected in decision-making processes. We have learned the value of visibility and recognition. Photographs of the nurses who chair the Nursing Congress and specialty councils now hang on the wall next to photos of the medical executive committee chiefs. Positive comments on this change have come as much from the physicians as from other nurses and visitors. We give frequent awards and use special opportunities like Nurses' Week to highlight our staff. The chief executive officer and chief operating officer make regular appearances at congress meetings, an expression of the value the management team places on this group.
We have learned to let others know what we're doing. Immediately following each congress meeting, minutes are e-mailed across the network. Our monthly newsletter on nursing issues, Network Nursing News, recognizes contributions of teams and individuals and reports on best practices and congress/specialty council activities. A Web page on Seton's intranet, now under construction, will serve as another source of information. We hold orientation sessions for new Seton directors, vice presidents, new congress representatives, and clinical managers, and encourage involvement from all disciplines. Perhaps most important, we have learned that if you start with the best and brightest, the possibilities are limitless. Each leader who completes a term in office has a vested interest in recruiting other bright, creative leaders to carry on the work and make even greater contributions in the future.
The saying goes that the whole is only as strong as its parts. Through three years of shared governance in our nursing program at Seton, we can say from experience that we have not only strengthened the whole network, but that each part is better for having gone through the process.
For more information, contact Joyce Batcheller at 512-324-1943.
