BY: STEPHEN C. SCHOENBAUM, MD, M.P.H., and KAREN DAVIS, Ph.D.
Dr. Schoenbaum is executive vice president for programs, and Dr. Davis is president, both at The Commonwealth Fund, New York City.
The strength of the United States depends upon having a healthy population. In order to achieve exceptional health outcomes efficiently for all Americans, it is essential to have a high performance health system. However, the current performance of the U.S. health system is far from optimal.1 Recently, the Catholic Health Association's Our Vision for U.S. Health Care has adopted the principle that "health care in the U.S. should be health and prevention oriented, with the goal of enhancing the health status of communities."2 This article reviews evidence about current prevention performance, reveals key strategies for achieving higher performance set by The Commonwealth Fund's Commission on a High Performance Health System, and assesses how those strategies will lead to better preventive care and a healthier population.
Prevention Performance
Preventive care is designed to reduce the occurrence of disabling and fatal conditions. The most obvious example is immunization. In the past, vaccine-preventable conditions such as measles caused a significant loss of school days for almost all children and a loss of workdays for parents. Although the incidence of major complications such as measles encephalitis was relatively low, measles itself was so common that the aggregated disability and even deaths from the disease were substantial. Those problems have almost disappeared. Though a vaccine to eradicate hypertension is not available, effective detection and management of the condition leads to less morbidity and mortality from strokes, and to better outcomes for diabetics with hypertension as a co-morbidity.
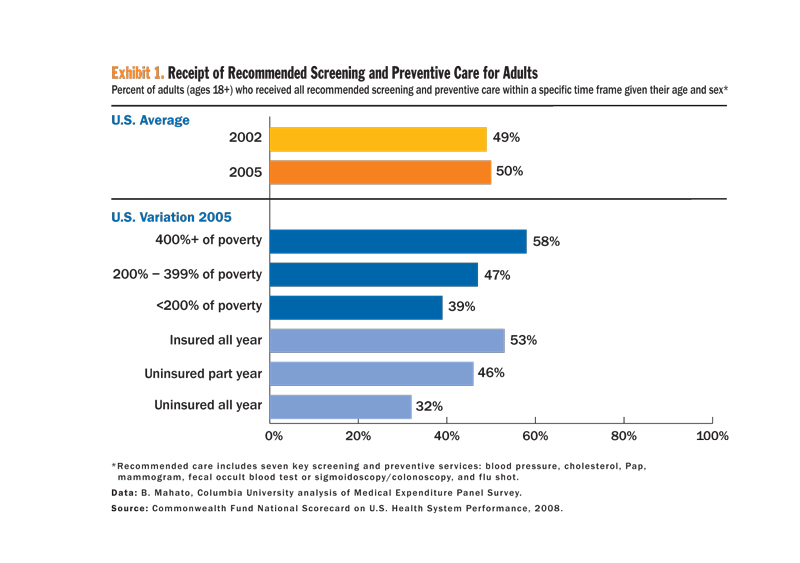
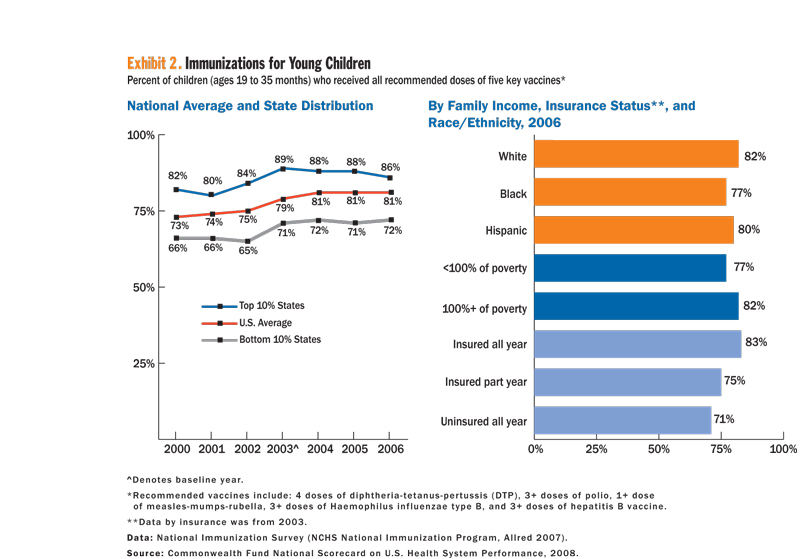
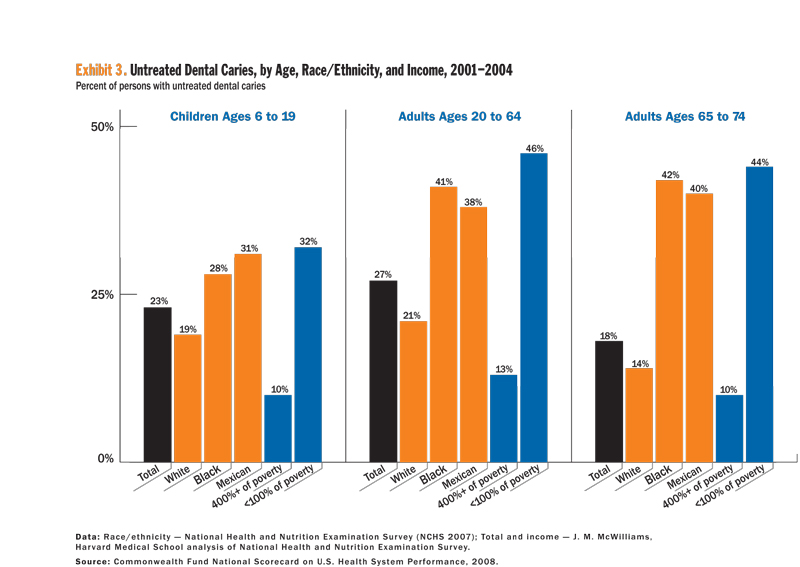
Exhibit 1 shows that adults in the United States, as of 2005, received only 50 percent of the recommended screening and preventive care for their specific age group. Furthermore, persons who are poorer, uninsured or have unstable insurance coverage — the latter two groups include roughly 70 million Americans — are much less likely to receive the recommended care. Ideally, performance would be close to 100 percent since few contraindications to the particular recommended practices exist. Similarly, Exhibit 2 shows that one in five American children has not received preventive care as basic as a complete set of recommended childhood immunizations. Again, significant differences by insurance status and major differences in performance by state are evident. Furthermore, Exhibit 3 indicates that preventive dental care is less than optimal for Americans of all ages, particularly those who are non-white or poor.
These performance deficits are consistent with what occurs across the spectrum of care — preventive, acute, chronic and long term. In all instances, performance on quality, efficiency and equity could be much better for the "average" American, and, in all instances, a lot of variation in performance exists. Each of these types of care contributes to a healthier, more productive population.
Also, an interrelationship between dimensions of performance within the United States exists. For example, quality of care tends to be higher in states with greater coverage and access to care;3 and this country's high rate of uninsured — unique among developed countries — is itself a major performance deficit. Thus, it is critically important to consider how all dimensions of performance and all types of care might be improved.
The Five Strategies for Improved Performance
Just as CHA's Our Vision for U.S. Health Care puts forth a set of principles, the Commonwealth Fund's Commission on a High Performance Health System has developed the following five key strategies for achieving broad-based performance improvement:4
- Extend affordable health insurance to all
- Align financial incentives to enhance value and achieve savings
- Organize the health care system around the patient to ensure that care is accessible and coordinated
- Meet and raise benchmarks for high-quality, efficient care
- Ensure accountable national leadership and public/private collaboration
How Can These Strategies Help?
Now, health insurance coverage for all isn't sufficient to assure exceptional care for all; it isn't even sufficient to assure access to the health system. But, health insurance coverage for everyone is a necessary condition for assuring access to the health system and achieving excellent care for all. Further, it is critically important that health insurance be comprehensive and cover necessary medical and surgical care, including preventive care, with little or no cost-sharing. Affordable coverage with comprehensive benefits is the foundation for performance improvement, including improvement of preventive care.
Comprehensive coverage of preventive services began with development of federally qualified Health Maintenance Organizations in the 1970s. Indemnity insurers adapted through the years, but even Medicare has been slow to respond. Only with the enactment of a new law in July 2008 (overriding a presidential veto) is the Secretary of Health and Human Services now empowered to make coverage decisions for Medicare involving "A" and "B" recommendations of the U.S. Preventive Services Task Force, an activity of the federal Agency for Healthcare Research and Quality.5
Payment for care in the United States is largely fee-for-service, an incentive that rewards more care, not necessarily better care. So, payment reform is an essential element of performance improvement, including improvement of preventive care. Achieving first-rate preventive care requires more than providing the service, including at a minimum outreach to persons who need the services and follow-up when some preventive services (e.g., screening tests) are positive. These activities are generally not "reimbursed" in current fee-for-service payments. Not surprisingly, only 52 percent of all adult Americans report receiving routine reminders for preventive care.6
Persons who have a regular source of their primary care — a clinician who knows and respects them or helps make care available to them when they need it by coordinating off-hours and weekend care — can be said to have a "medical home," an organized form of primary care that is patient-centered. Persons who have such a medical home are more likely to get appropriate preventive care. Even uninsured persons, who are fortunate enough to have a medical home, are more likely to get appropriate preventive care.7
In the United States, average performance across a set of 37 indicators tends to be about two-thirds of "benchmark" performance, e.g., the top 10 percent of performers (for some of the indicators, these are the top 10 percent of states; for others they are the top 10 percent of hospitals or health plans, etc.).8 Encouragingly, average performance for some of the indicators of preventive care is better than two-thirds of benchmark. Exhibit 2 shows that with respect to childhood immunization, the U.S. average for full immunization by age three is 81 percent, and 86 percent in the top 10 percent states. Though the results could be even better, they are as good as they are for several important reasons, including the following: The goal is clear — 100 percent immunization. Meeting the goal is relatively simple since it requires administration of a defined set of vaccines, a specific number of shots. Since 1993, measurement of childhood immunization performance in health plans has been in place through its incorporation in the Healthcare Effectiveness Data and Information Set performance measurement data set by the National Committee for Quality Assurance. Public programs subsequently adopted measures of childhood immunization and supply vaccine for poor children and electronic immunization registries. Widespread quality improvement efforts in public and private programs ensued. Theoretically, it should be possible with many aspects of preventive care to achieve near 100 percent performance by establishing clear goals, developing effective programs to achieve them, and supporting those programs with an appropriate health care infrastructure that includes electronic information systems to facilitate reminders for patients and clinicians and to support the implementation of the programs.9
Furthermore, in an analysis of several specific options that could help achieve net savings in health care expenditures in the United States during a 10-year period, three promising ones related to prevention emerged. These included reduction in tobacco use through an increase in taxes, which would be invested in smoking cessation programs; reduction in obesity through a new tax on sugar-sweetened soft drinks, which would be used to finance obesity prevention programs; and use of government and private funds to create positive incentives for individuals to engage in wellness programs. Estimated 10-year savings for these three options were $191 billion, $283 billion and $19 billion, respectively.10
Finally, national leadership is essential for achieving high performance. Some aspects of preventive care again provide examples: National groups establish guidelines for prevention such as the previously mentioned U.S. Preventive Services Task Force. In some areas, multiple national groups — private and public — exist. For example, the Centers for Disease Control's Immunization Practices Advisory Committee and the American Academy of Pediatrics' Redbook Committee develop recommendations on the use of vaccines for children. Given the pluralistic system in this nation, it is fortunate these two committees and organizations have long sought to "harmonize" their recommendations to minimize confusion for those who have to implement them. Electronic immunization registries have often been organized at the state level, generally under the leadership of state health departments. The nationally used Healthcare Effectiveness Data and Information Set, which includes several performance measures related to prevention, started as a private effort among health plans and some key employers, who were customers of those plans. The measures have now been endorsed by the National Quality Forum, a public-private collaboration that provides national leadership for quality measurement, and some measures are used not just by health plans, but also by government programs (e.g., Medicaid).
More national leadership for better preventive services is needed — for instance, leadership to help establish better incentives for development of medical homes, for supporting the implementation of health information technology and facilitating information transfer for purposes of achieving higher performance and measuring it, and for bolstering public health efforts related to prevention and better coordinating them with health care delivery efforts (e.g., around prevention and management of obesity).
Conclusion
The five key strategies for achieving higher performance of the U.S. health care system include preventive services, and almost everyone involved in the system can play a significant part in improving it. Particularly necessary is national leadership to achieve universal health insurance coverage and to help coordinate the many disparate parts of the system. The beginning of a new administration in Washington, D.C., provides an opportunity to achieve more effective, efficient and equitable health care for all Americans. We must take advantage of that opportunity today.
NOTES
- Commission on a High Performance Health System, Why Not the Best? Results from the National Scorecard on U.S. Health System Performance (New York: The Commonwealth Fund, July 2008). Available online at www.commonwealthfund.org; Karen Davis et al, The Commonwealth Fund, Mirror, Mirror on the Wall: An International Update on the Comparative Performance of American Health Care (New York: The Commonwealth Fund, May 2007). Available online at www.commonwealthfund.org.
- Catholic Health Association of the United States, Our Vision for U.S. Health Care, available online at www.catholichealthcare.us/OurVision.
- Joel Cantor et al, Commission on a High Performance Health System, Aiming Higher: Results from a State Scorecard on Health System Performance (New York: The Commonwealth Fund, June 2007). Available online at www.commonwealthfund.org.
- Commission on a High Performance Health System, A High Performance Health System for the United States: An Ambitious Agenda for the Next President (New York: The Commonwealth Fund, November 2007). Available online at www.commonwealthfund.org.
- Note: "A" and "B" recommendations of the U.S. Preventive Services Task Force are distinguished from "C" and "D" levels of recommendation by having strong supporting evidence.
- 2006 Health Care Quality Survey, The Commonwealth Fund (unpublished data).
- Anne Beal et al, Closing the Divide: How Medical Homes Promote Equity in Health Care: Results From The Commonwealth Fund 2006 Health Care Quality Survey (New York: The Commonwealth Fund, June 2007). Available online at www.commonwealthfund.org.
- The Commonwealth Fund Commission on a High Performance Health System, Why Not the Best? Results from the National Scorecard on U.S. Health System Performance.
- Mary Barton and Stephen Schoenbaum, "Improving Influenza Vaccination Performance in an HMO Setting: The Use of Computer Generated Reminders and Peer Comparison Feedback," American Journal of Public Health 80, no. 5 (1990): 534-536. Available online at www.ajph.org; Stephen Schoenbaum, "Implementation of Preventive Services in an HMO Practice," Journal of General Internal Medicine 5, supplement 5 (September 1990): S123-S127.
- Cathy Schoen et al, Commission on a High Performance Health System, Bending the Curve: Options for Achieving Savings and Improving Value in U.S. Health Spending (New York: The Commonwealth Fund, December 2007). Available online at www.commonwealthfund.org.