Pandemic took heavy toll on patients in New York City eldercare facilities
By JULIE MINDA
This spring, New York City was one of the world's coronavirus hotspots — and the city's nursing homes bore the brunt of the virus' blow. According to data from The Atlantic's COVID Tracking Project, 6,697 — or about 26 percent — of the 25,618 people who have died of COVID-19 in New York State were in long-term care facilities. Roughly half of the state's confirmed and probable COVID deaths that happened in nursing homes were in New York City, according to data from the New York State Department of Health.

LaRue
During the worst of the spring onslaught, Scott LaRue, president and chief executive of the ArchCare long-term care system, spoke to Catholic Health World about the devastation the pandemic had wrought in long-term care in the city. Sponsored by the Archdiocese of New York, ArchCare has facilities in New York City and Upstate New York including five nursing homes, a specialty hospital for medically fragile children and a residential care home for people with Huntington's disease.
ArchCare has had 638 residents test positive for COVID and its facilities cared for an additional 259 patients who were COVID-positive at the time of admission. It has recorded 295 patient deaths from COVID.
In a March 28 interview, LaRue said ArchCare and other long-term care facilities were desperately searching for personal protective equipment for staff and they had been challenging state government actions that placed COVID-positive patients discharged from hospitals among vulnerable long-term care populations.
This summer COVID case numbers sharply declined in New York City. LaRue spoke with Catholic Health World on Oct. 5 as new hotspots were emerging.
How are ArchCare staff doing, seven months in?
It is very hard for our staff, and that is partially due to the vilification of nursing homes by some of the media. And nursing homes have become a political football. This (treatment) is not based in fact or a desire to find out the truth and how to help prevent problems. It's political and it is very disheartening to people who literally put themselves and their loved ones at great risk in order to serve our residents.
How have the caseloads changed at ArchCare?
The peak for us was around Easter weekend, then things calmed down toward the third week of May. And then it was relatively stable until the third week of September. We had very few positive cases this summer. Our last death from COVID was July 2. We have spent this time preparing for the protracted response to COVID-19 and the possibility of a second wave.
What was ArchCare's focus during the summer reprieve?
We have created a program called "Protect." It includes increasing infection control staff and training, enhancing our infection control protocols and policies, and investing in new protective equipment. (See sidebar.)
I was not going to leave a single stone unturned in protecting our people, and that is what we have done.
Can you attribute the declining rates of COVID in your homes to these proactive changes at ArchCare?
Our rates of COVID infection have been declining, but I don't believe that is primarily because of these changes we've been making — some of these changes have been pretty recent. The virus spread in the spring because we were not provided access to the testing and the personal protective equipment we needed because the decision was made in our state to give acute care the higher priority for resource allocation. As soon as we were given access to the testing and the personal protective equipment, and we were able to test employees and patients regularly, the spread almost ceased.
ArchCare has been involved in advocacy efforts in the state to ease visitation restrictions. Could you explain those efforts?
I supported the restrictive visitation policies in New York when there was no access to testing and shortages of personal protective equipment and high rates of infection in our communities.
But we now have ample access to testing and personal protective equipment and until two weeks ago, the caseload was low.
There has been harm done to families and residents who are not able to see each other in person, and window visits are not the same. People with dementia, for instance, do not understand window visits.
We've demonstrated we can control the spread with a variety of options. Our testing has a high reliability and we think we can do the visits safely and that the visits are necessary for the well-being of our families and residents.
Has this advocacy by you and others in New York had an impact?
There has been some success. The old policy was that long-term care facilities had to go 28 days with no positive COVID test among residents and staff (before visitation was allowed). Well, that is not possible — at ArchCare we have 4,300 employees. The policy has since been reduced to 14 days and two of our homes qualified for visitation. I still think the policy is too strict.
So do you anticipate your homes now can expand visitation?
Unfortunately (in late September and early October) New York has seen a handful of positive cases in communities where some of our homes are. And the community infection rate has grown in parts of New York. So the city is starting with lockdowns for specific ZIP codes. This rate increase could be the indication of a second wave. But I am glad this is a targeted closure — we are not closing everything.
We will have to continue to balance the rate of spread with the ability to manage and control openings in a prudent and responsible way.
The good thing is we know what we are dealing with, we know how to manage the spread, we know more about the virus, and testing is identifying asymptomatic individuals. We have the resources and a better understanding, so I don't anticipate a return to the caseload of the spring.
What have been the most challenging aspects of the pandemic for you as the head of an eldercare system?
What was most concerning to me was asking staff to go in and care for patients who had COVID, even though the staff did not have the full protective equipment that they should have had. We were responsible to care for these patients, but to do so we were having to ask staff to put themselves and others at risk, and it was extraordinarily difficult to do that.
The other most difficult aspect was witnessing the suffering of the families of loved ones we had cared for. We had cared for some of these residents for many years, and it was just heartbreaking to see the suffering and, then in some cases, to lose them.
ArchCare bolsters its infection control staff, protocols, technology
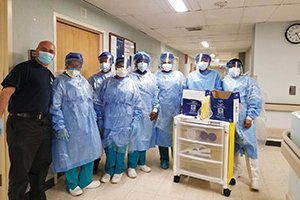
ArchCare spent the summer strengthening its infection control protocols and increasing its inventory of personal protective equipment in preparation for a possible resurgence of COVID-19. Here, colleagues at an ArchCare facility gather in their protective gear.
The New York-based ArchCare long-term care system has made many enhancements to help prevent viral spread in case of a resurgence of coronavirus. Through a program called "Protect," ArchCare has been increasing its staffing, improving its protocols and installing new technology.
This includes:
- Hiring an infectious disease medical director who is responsible for overseeing infection control practices.
- Hiring a systemwide infection control preventionist.
- Working to recruit and employ an infection control expert at each ArchCare facility.
- Assembling at each ArchCare site a trained and certified infection response team. These staff are prepared to care for residents with COVID-19.
- Improving and expanding infection control policies and protocols. This includes ensuring ArchCare has a 60-day supply of personal protective equipment on-site at each of its programs. The system has an additional 90-day supply of PPE at a warehouse in New Jersey.
- Installing thermal scan cameras at each entrance of every ArchCare facility. With this technology, temperatures are taken automatically, and there is an alert if the temperature is at or above 100 degrees. The thermal scans also can identify people not wearing a mask. A front desk attendant prevents those not wearing masks from entering.
- Purchasing portable HEPA negative air pressure machines so that ArchCare sites can contain airborne virus in the rooms of COVID patients.
- Purchasing robotic ultraviolet lights to disinfect patient rooms after discharge.
- Upgrading facility filters to have a higher MERVs rating. (Minimum Efficiency Reporting Values, or MERVs, are a measure of a filter's ability to capture larger particles between 0.3 and 10 microns.)
Scott LaRue, ArchCare's president and chief executive, notes that it has been difficult to make such investments during an economically challenging time.
He says of the investments, "It's had an extraordinary fiscal impact. Our census is down 20 percent and I don't see it going up until mid-next year. We've taken a revenue hit, but we are still investing in our staff and in our equipment.
"We believe this will set us apart in terms of how prepared we are in the future," he says.
— JULIE MINDA