By LISA EISENHAUER
At the start of the pandemic, when patients with COVID-19 who walked into emergency departments began to deteriorate so rapidly they were intubated and placed on ventilators within hours, Bon Secours Mercy Health kicked its advance care planning efforts into overdrive.
"While ACP has always been part of Bon Secours Mercy Health's mission, the onset of COVID catapulted us into more urgent and innovative action," said Rebecca Gruszkos, the director of advance care planning for the Cincinnati-based system that has facilities in seven states.

Gruszkos
Starting in March 2020, Gruszkos and her colleagues set up trainings and developed guides on how to initiate conversations with COVID patients and their loved ones about documenting care preferences and designating a surrogate to make health care decisions in the event the patient were to become incapacitated.
The system also created specific roles that were taken on voluntarily by staffers in emergency departments and inpatient units to identify patients who didn't have advance directives and to coordinate immediate outreach to them or their relatives.
Early on, only 30% of patients who died from COVID at Bon Secours Mercy Health hospitals had a documented health care decision-maker. Within a few months, that number had climbed to 60%.
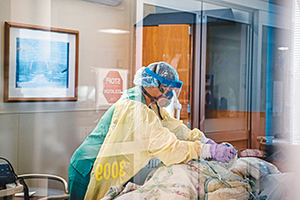
A nurse in the intensive care unit of a Pennsylvania hospital disconnects medical equipment after the death of a COVID-19 patient in December 2020. Studies show that while most Americans say they would prefer to spend their last days at home, a majority die in hospitals, nursing homes or hospice facilities.
Alexandra Wimley/Pittsburgh Post-Gazette via Associated Press
In May 2020, the system ramped up its advance care planning efforts in the ambulatory setting too. It hired full-time staffers to handle outreach to patients seen at clinics who had not designated surrogates for health care decisions in the event they were incapacitated or filed advance directives. It launched an online portal for patients with a MyChart account to access information in English and Spanish about advance directives, learn about the system's process for ascertaining goals of care, get state-specific documents and upload completed forms.
In March 2021 alone, 43,839 patients accessed the portal. Over the course of a year, the system received 26,000 updates from patients related to their advance care planning wishes via the portal.
Uneven uptake
Gruszkos discussed how Bon Secours Mercy Health supercharged its advance care planning at the start of the pandemic during a session at CHA's Theology and Ethics Colloquium in mid-March and in a later interview. She said the revised process brought solace to patients and family members who were separated because of COVID protocols and to frontline care providers ministering to a high volume of COVID patients in steep decline with little time to initiate complex end-of-life conversations.
Gruszkos pointed out that well before the pandemic, studies had shown a disconnect in the United States between what patients say they want at their time of their deaths and what actually happens. While a majority of Americans prefer to die at home, only about a third do. Most everyone else spends their last days in hospitals, nursing homes or hospice facilities.
The National Institute on Aging says that people who have advance directives are more likely to get the care they prefer at the end of life than those who do not. Nevertheless, only about one-third of Americans have completed such directives, a study published in 2017 found.
Gruszkos said individuals with advance directives tend to be white, older, wealthier, more educated, suffering from a chronic condition and getting regular health care. "As you see, many patients whose lives we touch are not represented here," she noted.
Gruszkos said the uneven use of advance care planning is the result of various barriers. One is access to health care, which remains a challenge for the millions of Americans who are uninsured. Another is the legal hurdles some states have in place. In Ohio, for example, the forms that constitute advance directives — a health care power of attorney and a living will declaration — number 20 pages and require signatures from two witnesses unrelated to and not providing care to the signatory or from a notary public.
Another factor is that some care providers are uncomfortable broaching the topic of end-of-life planning. "The most obvious reason and maybe the most problematic is the diffusion of responsibility," she said. "Everyone hopes or even expects that someone else will have this conversation with the patient."
Legacy of commitment
Bon Secours Mercy Health's commitment to advance care planning goes back to its legacy organizations. In 2014, Gruszkos said what was then Bon Secours Health System joined other major health care organizations operating in the Richmond, Virginia, area in vowing to normalize advance care planning conversations; provide formal training on how to talk to patients about their goals, values and preferences instead of just urging them to complete forms; and devise ways to store and retrieve related documents.
The commitment continued after the system's merger with Mercy Health in 2018 and provided a foundation for the revamp that was kick-started by the pandemic.
The revamp began with a directive from Bon Secours Mercy Health's leadership. The directive called for Gruszkos and others to lead the process of standardizing advance care planning across the system's footprint, in alignment with its intention to provide care oriented to each patient's goals.
That was followed by a ministry commitment statement that pledged an approach to advance care planning that "is easy for patients to access and efficient for clinicians to complete" and "achieves clearly defined outcomes consistent with national standards and the ministry's mission and strategic plan."
Next up was the creation of an advance care planning executive leadership team to oversee workgroups focused on planning, informatics and transformation among the medical teams.
"We had a systemwide model, a training program, new patient engagement tools and conversation guides in place within three months," Gruszkos said. "I've never worked harder in my life."
New policies
As part of the revamp, Bon Secours Mercy Health adopted several new advance care planning processes, including allowing virtual or telephone conversations about goals of care, letting patients access online platforms to designate surrogates or make their care preferences known, and approving the use of E-signatures and E-notarization for directives, at least where allowed by state laws. The uploaded documents go into the system's electronic medical records, making them easily accessible.
The system also created a dashboard with the informatics on referrals, online document filings and other related data to track the progress of its advance care planning initiatives. "We've been very pleased with the outcomes," Gruszkos said.
"I've experienced over 25 years the power of advance care planning when it's done well. Patients and families cope so much better, there are better bereavement outcomes," she said.