Resourcefulness has helped many ward off crises
By JULIE MINDA and LISA EISENHAUER
May 13, 2020
When COVID-19 showed up in Bogalusa, Louisiana, the deadly virus delivered a fast and mighty blow. All six ventilators in the intensive care unit at Our Lady of the Angels Hospital were being used for patients with the virus at one point in early April and the hospital had to divert other infected patients to ICUs at hospitals elsewhere.
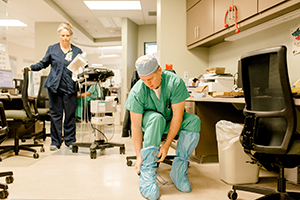
Bill Kuhn, a nurse anesthetist, dons protective gear as he prepares to intubate a patient who is believed to have COVID-19, as Jean Fortenberry, a registered nurse, looks on at Our Lady of the Angels Hospital in Bogalusa, Louisiana.
"That was the peak and within about five days the state of Louisiana sent us an additional five ventilator units that we were able to bring online quickly," said Rene Ragas, the hospital's chief executive.
By mid-April, the hospital in a city of 12,000 that is about 75 miles north of New Orleans had treated 60 patients for COVID-19, one-third of them as inpatients. Despite the sudden surge in demand for specialized care at a hospital that staffs 45 beds, Ragas said early preparations and assistance from its parent, the Franciscan Missionaries of Our Lady Health System, as well as local and state health and emergency preparedness officials kept the hospital from being overwhelmed.
While most of the about 1 million confirmed cases of COVID-19 in the nation have been concentrated in metropolitan areas, data compiled by the nonprofit USAFacts show that the pandemic has reached almost every county or, for Louisiana, parish. In rural areas, hospitals generally lack the breadth of clinical specialization, ready access to more advanced technology and — especially for those that are not part of a large system — a sufficient amount of critical supplies, as compared to their urban and suburban counterparts.

McGee
Executives from a sampling of rural hospitals in the Catholic health ministry told Catholic Health World that while they are concerned about these vulnerabilities, they have been able to use the time between when COVID-19 created urban hotspots and when it began moving into rural communities to prepare. They've been adjusting operations, cross training staff, coordinating with health care facilities and agencies to get supplies and identify potential community sites for extra treatment space. Hospitals that are part of big systems are tapping into the expertise of infectious disease doctors and other specialists within their parent systems to ready for worst-case scenarios.
Emily McGee, nursing director of intensive care, progressive care and respiratory care for St. Bernards Medical Center of Jonesboro, Arkansas, said that "while there are many challenges that rural areas face, when it comes to supporting a cause and helping others, we have a very strong community."
Same issues, big or small
Richard Morin, interim president for CHRISTUS Spohn Hospital Alice and CHRISTUS Spohn Hospital Kleberg in Kingsville, said the two south Texas hospitals, which together have about 90 staffed beds, have faced the same challenges as much larger ones across the nation in caring for patients with COVID-19. Those challenges have included stretching supplies of personal protective equipment for staff, long delays in getting test results, and setting up quarantine units and segregating patients to contain the contagion.

From left, Cole White, chief financial officer for Providence Seward Medical & Care Center; Stephanie Kaiser, a nurse with Seward Community Health Center; and Cristan McLain, director of quality & infection prevention for Providence Seward, staff the first drive-thru testing site in Seward, Alaska. Photo courtesy of Providence Health & Services Alaska
"Through good stewardship of resources, we've been able to make it work," Morin said, in mid-April, noting then that data collected by health officials showed the pandemic to be leveling off in Texas.
He gave credit to the leaders of the CHRISTUS Spohn region, who he said have emphasized consistency in practices and processes and open communication, and to his staff, who he said have given outstanding care to patients with the highly contagious illness while adapting to and enforcing restrictions to protect themselves and their communities.
"It's historic times. And in these times, it can bring out the best in people or the worst in people," Morin said. "I would say that for us as a ministry, it's brought out the best in our associates. Their courage, hard work and dedication has been a blessing to the communities served."

Smith
Exploiting lag time
Angie Smith is vice president of nursing St. Bernards Medical Center, the 386-bed flagship hospital that is part of St. Bernards Healthcare in Jonesboro. That system also includes a 15-bed medical center in Wynne, a 50-bed hospital in Pocahontas and an affiliate 25-bed hospital in Walnut Ridge. She said the system set up an incident command center in March, shutting down nonessential medical services and putting in place restrictive visitor policies. The first COVID-19-positive patient in the four hospitals presented four weeks after the planning began.

Thurmer
Smith said this lag allowed time for learning from other facilities going through the surge, and from CHA and other hospital associations. Arkansas State University in Jonesboro also has helped St. Bernards with disaster planning.
DeAnn Thurmer is president of the 25-bed Waupun Memorial Hospital in Waupun and the 17-bed Ripon Medical Center in Ripon, both in Fond du Lac County. The county reported its first COVID-19 cases March 11. Officials there were quick to recommend social distancing and other infection-prevention precautions. Thurmer said in large part because local people adhered to the recommendations, the county was spared a fast escalation of cases, and the three SSM Health hospitals in the county were spared a patient surge. The 139-bed St. Agnes Hospital is the third SSM hospital in that area.
SSM Health's Waupun and Ripen hospitals have ICU beds. Their crisis planning included potentially using St. Agnes as a release valve by transferring some patients requiring critical care for COVID-19 to St. Agnes. St. Agnes has cardiologists and intensivists, while the rural hospitals do not. The rural sites in turn would be available to admit St. Agnes patients coming out of critical care but still needing inpatient services.
The Waupun hospital also has been in close communication with the Wisconsin Department of Corrections to plan for how to handle a potential coronavirus outbreak at one of the four prisons in the hospital's service area. There are upwards of 5,000 prisoners living in those facilities, and the prisons are not equipped to care for prisoners needing critical care, said Thurmer.
Cross-training staff
"There are worries for small rural hospitals like ours of whether we'll have enough providers and staff if there is a surge," Thurmer said. "In our planning, we asked staff and providers whether they'd be willing to retool. The response was fantastic."
At the central Wisconsin sites — and at the Jonesboro-area St. Bernards sites — physicians displaced from closed clinics or practicing in low-volume departments got up to speed to work in emergency and critical care departments. Clinicians already trained to use ventilators, helped train colleagues. Clinicians also learned how and when to use bilevel positive airway pressure and continuous positive airway pressure machines to delay patients' need for a ventilator or decrease the chances they'd need one.

A clinician with St. Bernards Healthcare of Jonesboro, Arkansas, conducts her work while wearing personal protective gear.
St. Bernards' McGee said that system's nurses with critical care expertise have been pairing with nurses in other departments, to cross-train them to care for critical care patients. To limit exposure of staff to COVID-19, bedside nurses are drawing blood for labs and cleaning the rooms of their patients with COVID-19 — tasks normally performed by housekeeping staff and phlebotomists. Housekeepers clean and sanitize rooms after patients are discharged.
Vigilant in Alaska
Robert Rang, administrator of Providence Seward Medical & Care Center in Alaska, said his hospital has treated a few patients with COVID-19, all as outpatients. He said while state data indicates the pandemic is waning, his hospital and the 16 others in the state are not letting their guard down.
In coordination with state officials, all of the hospitals report a range of daily tallies, including intensive care patient census and personal protective equipment inventory levels. If there happened to be a surge of COVID-19 patients in one community, resources could be allocated from across the state, Rang said.
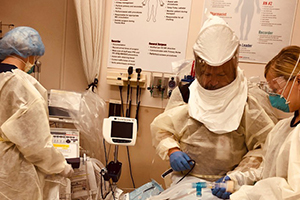
Dr. Jamie Quezada, center, a Waupun Memorial Hospital emergency department physician, completes intubation training alongside registered nurses Natasha Mueller, right, and Julie Jones Werner in April as the hospital continued its COVID-19 pandemic preparations.
"That peace of mind helps me sleep at night, knowing that if I did see something here that I would definitely have the rest of the state helping me out," he said.
Rang said Providence Alaska set up an incident command center to shift supplies and labor pools, if needed, among its five hospitals. Its parent, Providence St. Joseph Health, has shared best practices in such areas as PPE use and staff education related to the virus.
Moving toward a new normal
In Louisiana, Ragas said that the crisis had eased by mid-April. State data show the pandemic has leveled off, test results that had been taking up to nine days are coming within one and hospitals are slowly returning to normal functions, including resuming the nonelective surgeries that had been on hold for weeks.
While he is hopeful that the worst of the pandemics over, at least in the first wave, Ragas is confident that hospitals are prepared for whatever comes next. "While our nation, our industry and our local communities are challenged more than they have been in a very long time, we absolutely can handle this," he said.
In Avera's rural hospitals, primary care practitioners care for COVID patients with e-Care back-up
With nearly 30 rural, critical access hospitals widely dispersed across its five-state service area, Avera Health has made it a strategic priority for decades to develop and bolster its eCare telehealth services. Those services have helped to provide the system's rural facilities with a broad array of clinical services that they normally would not be able to offer, due to the difficulty of hiring certain physician specialists in rural areas.
Avera's investments in telehealth have been paying off amid the COVID-19 pandemic, said Dr. Kevin Post, with the system using virtual connections to provide the clinical expertise that is vitally needed to treat the most severely debilitated COVID-19 patients.
Post, who is chief medical officer of Avera Medical Group, said that all hospitals within the Avera system — including its small, rural hospitals — have created detailed staffing plans that hinge on flexibility, cross-training, shared knowledge and collaboration among staff members at all system facilities. Despite thorough planning, he said, sometimes gaps arise. He said in cases in which there is a physical shortage of doctors and nurses, Avera can bring in "virtual support and relief."
He said that while Avera's rural hospitals rely heavily on their primary care providers to care for patients, those hospitals have access to specialty providers for virtual consults and other telehealth services, when there is a patient need that falls outside of the primary care providers' expertise.
Throughout the pandemic primary care physicians and advance practice providers and nurses have been tending to COVID-19-positive patients in rural hospital. But those providers "can be assisted at any time with specialty consults, for instance, with pneumonia, by our pulmonary and infectious disease experts" available through telehealth, said Post.
He said such services are "allowing us to serve and support our patients and communities in even the most remote areas."
— JULIE MINDA