AMITA's Saints Mary and Elizabeth connects emergency department patients to social services
The realization that not only were they seeing the same social needs, but probably even the same people with those needs, over and over in their emergency rooms brought four hospitals on the west side of Chicago together, say people who helped start a collaborative called West Side ConnectED.

One of those people is Cody McSellers-McCray, executive director of community health for AMITA Health, a joint venture between Ascension's Alexian Brothers Health System and Presence Health, and Adventist Midwest Health. AMITA is based in the Chicago suburb of Lisle, Ill., and has 19 hospitals. Its Saints Mary and Elizabeth Medical Center operates one of the busiest emergency rooms on Chicago's west side.
McSellers-McCray, who was in CHA's 2019 class of Tomorrow's Leaders, said the idea of AMITA collaborating with other hospital systems that it normally competes with made sense within the parameters of a project to identify and address socioeconomic needs that factor into health outcomes for vulnerable patients.
"We wanted to learn, just like the rest of the hospitals, what are we seeing and then what can we do about it," she said. AMITA also wanted to use the model created through the collaboration to build an overall strategy that could be used in all of its hospitals, even outside of the emergency department.
With those goals in mind, staff from Saints Mary and Elizabeth Medical Center have partnered with their counterparts from the University of Illinois Hospital, Rush University Medical Center and Mount Sinai Hospital to develop and use a screening tool to assess and address the needs of patients who get care in their emergency departments.
Seven questions
The tool has taken the form of a set of seven questions that ask about needs such as primary care, housing and food.
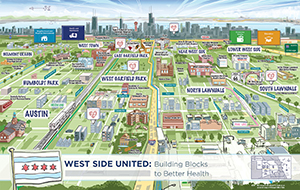
Representatives from the hospitals drafted the questions in a series of sessions that went on for several months. The screening is specifically meant to get at the needs of residents of 10 neighborhoods on Chicago's west side — places where rates of infant mortality and chronic disease far exceed the national average and residents face inequities in education, employment, food access, violence and access to transportation. Rates of diabetes, asthma and hypertension are of particular concern in these west side neighborhoods.
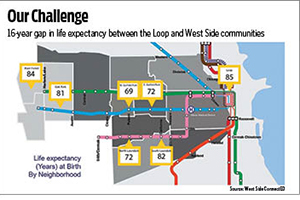
In one of those neighborhoods, West Garfield Park, the life expectancy of 69 years at birth is 16 years below that of residents in affluent neighborhoods on the lakefront just 2 miles to the east. The average life expectancy at birth for the city of Chicago as a whole is 77.3 years.

Kathy Donahue, acting administrator, president and chief executive at Catholic Charities of the Archdiocese of Chicago, said some people might see statistics like that and assume that violence is the root cause of the shortened life expectancy. But she said many factors are at play, including a lack of preventative care and health screenings.
"There's a lot of reasons why people don't get the preventative care that they should get," Donahue said. "It's women with cancer who never follow through with getting a mammogram because they're working three jobs, for one example."
United effort
Catholic Charities is the convening agency that brought the hospitals together and linked them with partner agencies that provide the social services needed by so many patients.
Part of the funding to cover Catholic Charities' costs for coordinating West Side ConnectED is coming from West Side United, a broader nonprofit initiative aimed at improving the health as well as the economy, educational opportunities and physical environment of west Chicago neighborhoods. Other funding is coming from the Illinois Health and Hospital Association.
Donahue said the fact that the hospitals were willing to collaborate for West Side ConnectED is telling as to how important they view the need for identifying and addressing socioeconomic needs that impact the health outcomes of their emergency department patients.
But she was among those who felt strongly that the screening was best done in emergency departments. Patients with low health literacy may repeatedly rely on ERs for primary care, she said.
"If you fix a problem in the emergency room, you've made a difference and you've saved the hospital so much money and you've saved those patients from repeated trauma," Donahue said.
Building support
One of the keys to getting all the hospitals to agree to ask the questions in emergency rooms was having the support of three of the four hospitals' medical directors, including the medical director from Saints Mary and Elizabeth Medical Center.
"They said: 'We have people sleeping in our waiting rooms who are homeless. We're becoming the de facto shelters for the city of Chicago,'" Donahue recalled. "That doesn't help your workflow, when you have nurses having to deal with people who haven't eaten and are sleeping alongside patients who have the flu. Somebody needs to be intervening in the social needs of patients who are multiple visit users."
The patient care managers at the hospitals, some of them nurses and some of them social workers, are doing the emergency department screening.
At all four of the west Chicago hospitals, the information from the screenings is assessed and matched with services from social service agencies listed in social service platforms used by the respective hospitals. The care managers then connect the patients with those agencies. In some cases, the screeners make calls and in some cases they pass along the contact information from the agencies to the patients.
Finding partners
Catholic Charities helped set up links with about 30 partner agencies that were ready to take the handoff from the emergency departments and provide services. The hospitals then established their own relationships with the partner agencies.
McSellers-McCray said Saints Mary and Elizabeth Medical Center taps additional agencies whose services are listed in the platform it uses, AMITA Health Community Connect, which is powered by the human services database Aunt Bertha. The platform vets all the programs that are included. All of the programs in the platform are either free or low cost to the user.
Courtesy Rush University System for Health
She said AMITA saw Aunt Bertha as the best option to spread the screening across its system and is using it as part of its Accountable Health Communities project (see sidebar). The other three hospitals are using a platform called NowPow.
The launch dates for using the screening questionnaires varied. It was September 2017 for Rush University Medical; mid-August 2018 for University of Illinois Hospital; March 2019 for Saints Mary and Elizabeth Medical Center; and April for Mount Sinai Hospital. Donahue said Catholic Charities is collecting information about the screenings — such as how many patients each hospital is screening and what needs are being identified.
Closed loop
The goal is for the screenings to be a closed-loop process, with the participants confirming to care managers that services were provided and thus needs were met. "It's important to ask the questions, it's important to have a resource and to follow up and to see if it's improving health," Donahue said.
Just based on anecdotal information from early in the process, the screening appears to be having some success, with patients reporting that they are getting help from the agencies with whom they've been connected.
McSellers-McCray said the mission of the collaborative goes beyond meeting the health needs of the individual patients and reducing the costs of their care to helping policymakers figure out how best to address the community's needs.
"Having this data, we can say, hey, there's a shortage on the west side of Chicago for housing or food," she said, "and so what policy changes should be made at the state level or the city level to influence that so there is better access to whatever that need is versus (the hospitals) trying to navigate and do all things for everybody?"
West Side ConnectED questions assess sociomedical need
These are the questions that are being asked of emergency department patients at the four hospitals that are part of the West Side ConnectED collaborative.
1. Do you have a doctor (primary care physician) or nurse that you see regularly?
___Yes ___No ___Declined to Answer
2. Do you have health insurance or a medical card?
___Yes ___No ___Declined to Answer
3. A. Do you currently have a place to stay/live?
___Yes ___No ___Declined to Answer
B. In the next two months, will you have a place to stay/live?
___Yes ___No ___Declined to Answer
4. A. Are you worried that your food will run out before you have money to buy more?
___Yes ___No ___Declined to Answer
B. In the last 2 months, have you run out of food that you bought, and didn't have money to get more?
___Yes ___No ___Declined to Answer
5. In the last 2 months, have you had difficulty paying your electric, gas, or water bill?
___Yes ___No ___Declined to Answer
6. Do you have a hard time finding transportation to and from your medical appointments?
___Yes ___No ___Declined to Answer
7. Is there anything else in your life that's impacting your health that you want to share?
___Yes ___No ___Declined to Answer
AMITA is helping CMS identify social needs in the frail elderly population
The screening for social determinants of health being done in the emergency department at Saints Mary and Elizabeth Medical Center is not new to AMITA Health, the hospital's parent company.
The use of questions to determine the social needs of vulnerable patients actually got started when the Alexian Brothers Health System (which formed a joint operating company with Adventist Midwest Health in 2015 to become AMITA) was awarded an Accountable Health Communities Model grant from the Centers for Medicare and Medicaid Services.
Thirty organizations got the federal funding to help figure out how addressing social needs can improve health outcomes and reduce costs. The five-year Accountable Health Communities initiative started in 2017.
AMITA is using its grant to screen patients who qualify for either Medicare or Medicaid, or both. People insured by both Medicaid and Medicare are often in poorer health than the general population. The pilot program is intended to develop effective ways to identify and assist "high-risk beneficiaries with accessing services to address health-related social needs," according to the CMS website.
That process is underway at the same time Saints Mary and Elizabeth Medical Center is collaborating in West Side ConnectED, which means a subset of patients there may be screened twice on social determinants of health.
— LISA EISENHAUER
