By JULIE MINDA
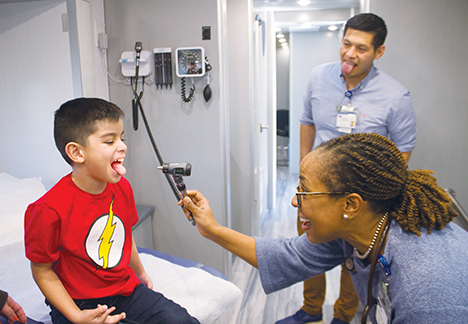
Even for people born and raised in the U.S., the fragmented health care and social service systems can be very difficult to access and navigate. Refugees and immigrants of little means can have the added obstacles of limited English language proficiency and cultural, social and financial barriers when they are sick or struggling to meet their family's basic needs.
It's no wonder that many economically vulnerable immigrants are not getting preventative health care or timely care for major health conditions.
According to the Immigration Policy Lab, unauthorized immigrants who are excluded from participating in publicly funded insurance and health care programs are among the most medically marginalized groups.
The issues aren't new. A study published in the September/October 2005 Health Affairs and funded by the Robert Wood Johnson Foundation found that "immigrants in general and the undocumented in particular use relatively little health care." The authors of the study gave another reason certain immigrant populations don't access health care: immigrants were more likely to report health care discrimination and stigmatization than were U.S.-born patients.
Some Catholic health systems have taken on these disparities by providing culturally sensitive outreach to refugee and immigrant groups. Some of the efforts go back decades. They have tailored services and staffed facilities to welcome medically underserved refugee and immigrant populations in their communities.
The programs highlighted here are building trust within immigrant communities and making inroads against preventable disease.
New Life in Lewiston

The closure of its textile mills beginning in the 1970s set off an industrial decline, depopulation and poverty that had a major impact on Lewiston, Maine, in the last decades of the 20th century. But at the turn of the millennium the unexpected happened. Word went out over the dispersed and informal network of Somali refugees in the U.S. that the Lewiston area was a safe, affordable place to raise families and that attracted several thousand Somali refugees to the area starting in the early 2000s.
Currently more than 60,000 people live in Lewiston and the adjacent community of Auburn. Over 22% of Lewiston's population are people of color and 15% are refugees/immigrants. In Auburn, 14.6% of residents are people of color, according to statistics from Kirsten Walter, who directs St. Mary's Nutrition Center, part of Covenant Health's St. Mary's Health System in Lewiston.
She says the first people to arrive were ethnic Somalis, mostly from Somalia, Kenya, Djibouti and Ethiopia, soon followed by Somali Bantus, an ethnic minority. Attracted by the low crime and affordable housing, they relocated from other U.S. cities. Over the next 15 years, people from other countries including the Democratic Republic of Congo, Angola, Zambia, Sudan, Iran, Syria and Afghanistan followed. A reflection of the diversity can be seen in the Lewiston Public Schools, where there are now 34 languages spoken, she says.
The arrival of immigrants, asylees and refugees during the last 20 years has brought the region diversity, energy, growth and challenges. Many immigrants in Lewiston and elsewhere endure systemic racism and Islamophobia. Recently arrived immigrants in Lewiston also face poverty, housing insecurity, food insecurity and language barriers, says Walter.
St. Mary's laid the groundwork for the nutrition center's core programs in 1999 and formally opened the center in 2006. The center addresses food insecurity in one of Maine's poorest cities and has evolved into a catalyst that works with community partners regionally to take on a range of socioeconomic concerns for immigrants and the greater community.
With a staff of 12, the nutrition center's food pantry works to provide culturally preferred food, along with other meat, dairy, fresh produce and dry goods. It offers cooking education programming, highlights locally grown foods that may be unfamiliar in African and Middle Eastern diets and supports community members in navigating fresh food access programs at a farmers' market and mobile market.
St. Mary's work in immigrant health has a partner in a federally qualified health center in Lewiston. The B-Street Health Center opened in 2010 in a neighborhood populated with refugees and immigrants. Both the nutrition center and health center have staff who speak two or more languages and who provide cultural brokering support as part of their job duties. The health center has three full-time community health workers who are fluent in English and Somali. There are 32 languages spoken by patients. On the health center's staff, Somali, Portuguese and French are the main non-English languages spoken.
Walter says at both the nutrition center and the B-Street Health Center, the focus is on addressing root causes of disease. She says inequity is at the heart of many of the health and socioeconomic concerns that immigrants and other vulnerable patient populations in the community face.
And she adds that within the last five years or so St. Mary's has been more intentional about deepening its equity and cultural competency work and creating a deliberate feedback loop with the community.
The St. Mary's system is part of a consortium putting together public and private financing for a redevelopment project in a downtown Lewiston neighborhood where the health center is located and where many immigrants of African and Middle Eastern descent live. The plan includes construction and rehabilitation of affordable housing, expansion of Head Start preschool and improvements to recreation and park spaces in a residential downtown area.
St. Mary's Nutrition Center staff are supporting a cooperative that plans to open in the redevelopment area a community food center. That facility will include a low-cost grocery store as well as a commercial kitchen, food storage and other facilities for use by food business entrepreneurs and other community members. As part of the downtown redevelopment project, the health center is expanding primary care, dental care and mental health care services.
Navigation assistance

Until relatively recently, many people from Bergen County, New Jersey's sizeable Asian-American community steered clear of traditional Western medical care. And their health suffered, said Dr. Hee Yang, chief medical officer for Asian Health Services at Holy Name Medical Center in Teaneck, New Jersey.
"We're in the middle of some of the best medical facilities in the world and yet these community members were not going to them," he says. "There were people who wouldn't come in until they were nearly on their death bed."
Holy Name's answer to that reticence came in the form of its Asian Health Services patient navigation program. Its charter includes educating physicians and other Holy Name caregivers and staff on how to provide culturally sensitive care to people of Korean, Chinese, Japanese, Filipino and Indian background, says Yang.
A paid concierge staff that includes six Korean-Americans, two Chinese-Americans and one Japanese-American are the mainstay of Asian Health Services. They help patients find their way through the web of health and social services to connect with the right provider and they sometimes accompany a patient into an exam room, where they can provide medical translation services. Under Yang's direction, program staff do outreach and education in the Asian community.
When the pandemic prevented family members from accompanying their non-English speaking relatives to medical appointments at Holy Name facilities, Asian Health Services concierges and volunteers identified patients scheduled for medical appointments who had used the concierge service before or had Asian-sounding names. They offered to help them prepare for their visits and to provide an escort from the health facility's entrance to a medical office. They stayed with patients throughout their appointment, if the patients so desired.
With COVID-19 restrictions lifted, patients still can request on-campus navigation assistance from the Asian Health Services team.
Yang says members of distinct Asian immigrant subgroups settled together in neighborhoods where they have retained their native language, culture, beliefs and traditions. This is especially true of older, first-generation immigrants of Japanese and Chinese heritage, he notes, with Filipinos generally being more assimilated.
Asian Health Services staff reaches out into these enclaves including through word of mouth and media outlets aimed at the ethnic subgroup to offer health and social services navigation.
About a dozen years ago, Holy Name clinicians connected informally through Asian Health Services documented a high incidence of aggressive breast cancer among Korean-Americans. Yang says historically Koreans have had very low breast cancer rates in part because of healthy diets and lifestyles. But Koreans who adopted American diets and lifestyles raised their risk for breast and other cancers.
Since many Asian women at the time were not getting preventive care or cancer screenings, their cancer progressed unchecked. Asian Health Services started a breast cancer awareness, screening and service referral campaign for Korean Americans, spreading information through word of mouth and through Korean newspapers and radio and television shows. Asian Health Services helped uninsured women who screened positive for breast cancer find a payer source or apply for financial aid. Yang said as a result of that campaign, women were able to be diagnosed and start treatment earlier in the disease process.
Asian Health Services launched a diabetes prevention and healthy living program that set out to influence the food choices of Korean, Chinese, Japanese and Indian families with diets high in carbohydrates, particularly rice and noodles. Yang and his team encourage healthy eating, increased exercise and healthful lifestyle choices as they raise awareness about the link between carb-heavy diets and chronic disease including diabetes.
Trauma-informed care
Hundreds of refugees are resettled in Boise, Idaho, each year. This year the city is on track to welcome more than 1,000 refugees.
During the 2000s, most of these new residents have come from Iraq, Congo, Burma, Bhutan, Afghanistan, Somalia, and Nepal, according to the Idaho Office for Refugees, the refugee resettlement administrator for Idaho state. More recently, refugees have arrived from Ukraine. More than 50 countries are represented among Boise's resettled population.
To ensure the new arrivals as well as immigrants who have come before them receive health and social services in a way that is individualized, culturally appropriate, linguistically responsive and trauma informed, the medical group of Boise's Saint Alphonsus Regional Medical Center launched its Center for Global Health & Healing about seven years ago. It provides women's health care and family medicine and runs a federally funded grant program for survivors of torture.

Elizabeth Rutten-Turner, a licensed clinical social worker at the center, says, "We build strong, trusting relationships with families. We help with wraparound care. We meet patients where they are. We address the social determinants of health."

Adds Sarah Mohr, practice manager of the Boise facility: "So often in western medicine, medical appointments are fast and driven by the goals of the providers." At the global health center, "we slow down and take our time with patients."
Dr. Chip Roser, the center's medical director, explains that most of the center's patients are refugees who fled war or other armed conflict. Many endured physical and mental trauma in their homeland and in refugee camps where they may have waited months or years for immigration documents.
Rutten-Turner adds that once resettled in the U.S., refugees typically have difficulty securing affordable housing, transportation, food and good jobs.
The job market has brightened in recent years, Rutten-Turner says, as more factories and plants have opened in and near Boise and families who arrived years ago are opening their own businesses and hiring members of their community. Also, a nonprofit is helping immigrants who left professions to get recertified and hired in jobs that use their skills and education. "Employment opportunities have greatly improved, although wages are still quite low compared to cities of similar size," says Rutten-Turner.
Still, uprooting one's life and acclimating to a new culture is a high-stress proposition. "Many of our patients, no matter how long they've lived here, are struggling with adjustment issues, acute stress disorder as well as complex, compound trauma and stress disorder, major depressive disorder," says Rutten-Turner.
Roser puts it this way: "We work at the intersection of trauma and medical care."
The Center for Global Health & Healing works closely with all resettlement and refugee aid organizations in Boise.
Rutten-Turner says the cornerstone of the center's success is a team of 11 community health advisers who serve individuals and families who speak the same language and are from the same cultural groups. The advisers are alert to the needs of their communities, and they work alongside center staff to address those needs. They also spread the word about the health center in the refugee community.
All the advisers are certified in medical interpretation and provide language services at the center. All were hired for their interpersonal and leadership skills, says Rutten-Turner.
The center has 25 staff members, including physicians, nurses, licensed clinical social workers, the community health advisers and administrative workers. Every staff member receives ongoing training in delivering trauma-informed care.
The center's social workers provide counseling — they've been trained in cross-cultural therapy — and they can connect patients with other resources to address social determinants of health. The social workers are part of the center's team that is using the federal grant to offer tailored counseling, medical care and legal support to survivors of torture.
Mohr says while data shows the center helps improve health outcomes, some of the most poignant validation of its work comes anecdotally. Patients of the center say they feel staff treats them like family members. "They keep bringing their families back and they recommend us to their friends. To me this speaks volumes about the trust we've established," she says.
Hot topics in South Asian health

Saint Peter's University Hospital, a Catholic teaching hospital in New Brunswick, New Jersey, has honed its approach to providing clinical and wraparound services to first- and second-generation South Asians, especially those of Indian and Pakistani descent. It also is training physicians to understand how ethnicity and culture factor into heightened disease risk for these immigrant groups.
About six years ago, the facility partnered with the Hillsborough, New Jersey, Shri Krishna Nidhi Foundation to establish the SKN South Asian Diabetes Center at Saint Peter's. Founded by local pediatrician Dr. Naveen Mehrotra, the nonprofit SKN Foundation seeks to address health disparities and promote wellness and the prevention of many chronic illnesses in part by increasing people's understanding of the relationship between lifestyle choices and disease prevention.
The SKN South Asian Diabetes Center's specific focus in Central New Jersey's large South Asian-American community is reducing diabetes and heart disease. It offers diabetes prevention and self-management programs. The center points people of South Asian heritage to health screening sites including at Saint Peter's. The center's staff can assist patients who require follow-up care in making appointments with Saint Peter's clinical specialists. The center's patients receive care at Saint Peter's usual locations.

Dr. Meena Murthy is chief of the division of endocrinology, nutrition and metabolism at Saint Peter's University Hospital. She directs the SKN South Asian Diabetes Center. She says many immigrants moved to Middlesex County, where Saint Peter's is located, over the last several decades because it is close to New York City but much more affordable than that city.
Middlesex County's South Asian population is made up of many highly educated, wealthy people who work at universities, hospitals and information technology companies, along with South Asians who are not wealthy and may be culturally isolated. People from both these socioeconomic groups turn to the center for information and assistance navigating the health care system, Murthy says. And, she adds, center staff also guide people in navigating the social service system.
"We find rich or poor, people have unmet health needs." Murthy says that through health assessment and support the center can improve health literacy, self-confidence and the self-management skills of all its patients.
Murthy says research has shown that South Asians have a heightened incidence of diabetes and cardiovascular disease as compared with caucasians. These conditions occur for South Asians at a much earlier age and at much lower weight and body mass index scores than for caucasians. Murthy explains, "South Asian genetics seem to be highly vulnerable for diabetes and heart disease, with a demonstrable higher level of insulin resistance." She says the risks always are multifactorial, "from genetics to epigenetics which includes social determinants."
"This higher prevalence is not just in immigrant populations; this problem is also seen in South Asians living in their country of origin," Murthy continues. "The whole world has changed due to industrialization, urbanization, globalization, western influences, as well as from information technology overload, employment expectations, cheap fast food availability, sedentary and stressed living."
Murthy says in general neither South Asians nor many clinicians appreciate the heightened risk of diabetes and heart disease. The center aims to close this knowledge gap.
The center also helps clinicians better understand South Asian cultures. For instance, says Murthy, many but not all Asian Indians place a high value on spirituality and consume vegetarian diets. Indians have lower rates of smoking than Caucasians. She says, "For better outcomes, clinicians need to understand family background, beliefs, spiritual faiths and respect as well as depend on such strengths and culturally appropriate resources to enhance and support care."
In September, the center held a cardiovascular health conference that brought together medical providers, researchers, medical students, patient advocates, patients and family members and community leaders.
"South Asian researchers who were invited to speak included those who have done original work in South Asian populations around the world and have global reach for their research." Other presenters focused on the health status of South Asians who reside in the U.S., Murthy says. "Heterogeneity within subpopulation was addressed in various talks; currently this is a hot topic that is being talked about and being studied in research actively."
Artificial intelligence
Latinos with low family incomes make up the majority of patients who receive care at Saint Peter's Family Health Center, a federally qualified health center look-alike facility in New Brunswick, New Jersey, that welcomes the uninsured and underinsured along with insured patients. The center provides primary care and specialty services and its patient mix includes new immigrants and immigrants who have been in the U.S. for a long time. Some of its patients are undocumented.
As part of their intake registration, new patients are asked questions about socioeconomic factors that impact health status and treatment outcomes. Their answers might reveal whether the patient has a stable housing situation and can afford to stock the refrigerator with nutrient-rich foods.
The health center is using artificial intelligence — primarily predictive analytics — to mine and analyze census and other publicly available data to better understand and address community and individual needs.

Ishani Ved, Saint Peter's director of transformational population health and outcomes, says the Saint Peter's Family Health Center has been emphasizing with its staff that the AI population analytics are intended to be an entry point for deeper conversation and engagement with patients, not a substitute for that deeper learning about the patient.
When clinicians take the time to listen and get to know patients, the patients open up and provide information that could be important to improving their health outcomes, she explains. The health center is tracking data to verify that this improvement is happening.

Dr. Alma Ratcliffe, vice president and chief clinical transformation officer for Saint Peter's Healthcare System, says the combination of patient screening and predictive analytic data have revealed that the top socioeconomic and related concerns that patients are facing have to do with food insecurity, lack of access to transportation, language barriers, lack of housing and insufficient access to care for mental illness.
Saint Peter's Family Health Center has been increasing its attention to these concerns. This includes providing behavioral health services to the seriously ill or addicted. Patients who present with symptoms of mental illness in Saint Peter's emergency department are given referrals to community mental health services including follow-up behavioral health care at Saint Peter's Family Health Center.
Staff have begun connecting patients with a program that reimburses for Uber and Lyft rides for transportation to medical appointments and providing vouchers for purchases at a farmer's market.
Expanding choices
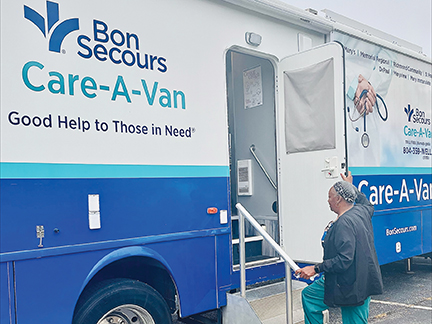
From its humble origins in Richmond, Virginia, nearly 30 years ago as a mobile vaccination provider for school-aged children, the Bon Secours Richmond Care-A-Van has evolved into a primary care clinic on wheels. Bon Secours Richmond recently supplemented the van's offerings by adding telehealth services and the system will open a fixed-site clinic in January.
Becky Clay Christensen, executive director of community health services for Bon Secours Health System's Greater Richmond Region, says more than 90% of the clinic-on-wheel's patients are Latino.
Many patients speak only Spanish. Most of the rolling clinic's physicians, nurses and social workers are fluent in English and Spanish and some of them are certified medical interpreters. When staff don't speak a patient's language, the Care-A-Van clinicians use a medical interpretation service that can provide translation in 200 languages.
Christensen says many Care-A-Van patients without legal immigration status steer clear of hospitals and fixed-base health care settings out of fear of coming to the attention of immigration authorities. From the start, the Care-A-Van built trust and came to be seen as a safe place by locating its stops at churches in immigrant neighborhoods.
In 2016, Care-A-Van staff started screening patients for housing and food insecurity and other needs associated with social determinants of health, documenting findings in patients' medical records and connecting them with social service providers.
Care-A-Van services include primary care, pediatric care, some lab services, chronic disease management and behavioral health care and referrals. Patients pay nothing for the services they receive. There were more than 7,300 patient visits to the van in the first two quarters of this year.
During the pandemic, the Care-A-Van began offering some services via telehealth. Many patients appreciate this ongoing service because they don't have to take unpaid time off work to travel to medical appointments.
Dr. Paula Young, Care-A-Van pediatrician and Bon Secours Richmond medical director of community health access, says hypertension, diabetes and cardiovascular disease are common conditions among Care-A-Van adult patients. It also is common for people to come in with acute conditions after they've tried natural remedies that were ineffective.
Many patients are migrant workers in physically demanding jobs. As they're traveling, they're not usually able to get health care services. Hard labor can exacerbate untreated injuries and disease.
Young adds that in some cases she has treated patients who had not sought care, or been unable to access care until their conditions became impossible to ignore. One teenaged patient wore diapers for his first appointment with Young. He needed corrective surgery for bladder exstrophy, a rare birth defect in which the bladder develops on the outside of the body. Another new patient presented with congenital heart disease so advanced that the person's finger tips were clubbing. The Care-A-Van was able to refer both patients to specialists.
All of the patients treated at the mobile clinic are uninsured or underinsured. Bon Secours offers a financial assistance program for uninsured patients who don't qualify for government-sponsored insurance and cannot pay for their treatment. The van refers patients needing specialty care to Bon Secours physicians and partners with Access Now. That Richmond nonprofit helps coordinate specialty medical care for patients without insurance at no cost to them.
Christensen says in recent years a growing number of patients with mental health concerns have been seeking care at the mobile clinic. Some experienced violence or trauma in their native countries or on the journey to the U.S. Adjusting to life in the U.S. carries its own significant stresses. The mobile clinic employs a part-time, bilingual licensed clinical social worker to provide mental health counseling and make referrals to partner organizations offering mental health services.
Starting in January patients will get an access option beyond the mobile clinic and telehealth. Bon Secours Richmond is leasing a space neighboring a nonprofit called CARITAS. The clinic site is in a Richmond neighborhood central to where many Latino immigrants live. The partnership is renovating a former tobacco warehouse into a health and social services hub. The new facility will house a Bon Secours Richmond clinic for the uninsured. CARITAS provides substance detoxification services, reentry services for former prisoners, job programs and other services.
Young says Bon Secours Richmond and its partners are making health care and social services more accessible for vulnerable people. "We meet them wherever they are" with the services they need.
"We are a safe place" for them, she says.
