Amid a satisfying career in nursing, Brandie Wilson wasn't necessarily looking for another job. But she was too intrigued about the opportunity at Covenant Medical Center in her hometown of Lubbock, Texas, not to check it out.

She's glad she did. The hospital's co-caring model of virtual nursing showed her a whole new way to practice. Working from home, she can respond to a patient's push of a button and join a streamlined, modern medical team.
"I did emergency room nursing for so long that in my mind, everything had to be stat and now and how many patients could I physically get to in one hour?" she explained. "It was just rush, rush, rush.
"When I got here, I had to learn to take a step back and realize that it was no longer that way. I could take the time to not talk. The patients didn't need to hear me talk. They just needed to be listened to and be heard. I didn't have to be rushed anymore."
Covenant Medical Center has been piloting the co-caring model, a hybrid with a virtual nurse splitting duties with a bedside team of a registered nurse and a nursing assistant, in an inpatient unit since 2021.
Covenant Medical Center's parent, Providence St. Joseph Health, is planning a wide expansion of the model this year.
By nurses for nurses
Sylvain Trepanier, chief nursing officer at Providence, says co-caring works because it was developed by nurses for nurses.
To develop co-caring, Trepanier said Providence invited nurses to reconsider how they go about their work and how to better meet the needs of patients. The system then handed off the nonessential work the nurses were doing to other staff members.

"By creating a new team that would share responsibility and accountability with a nurse that would be working virtually, we have people showing up every day doing the work that they love to do and removing some of the barriers that they had in doing it the old traditional way," he said.
Still, the co-caring model raised serious questions at first, about confidentiality and the human touch.
"All of a sudden there was a camera," Trepanier said, "and someone could see and hear what was going on in the room at all times. We were very quick to articulate that no one could listen unless the camera is on and if it looks their way.
"Sometimes, if you use the nomenclature 'virtual nurses,' it's almost like there's this perception an avatar has been created," he added. "The work itself is the same. What differentiates us is that we've completely deconstructed how we approach the work and we supplement it with virtual as well. Hence co-caring, where we're caring for patients, being both physically present and virtually present in a team effort."
By the numbers
The success of the co-caring model shows up in the numbers, Trepanier said, with turnover rates in the first year down by 73% for registered nurses and 55% for all staff in the pilot unit at Covenant Medical Center.
Trepanier said employee retention along with other efficiencies, such as a reduced need for costly travel nurses and shorter patient stays, added up to significant savings in the pilot's first year. "On a 30-bed unit, we ended up having a return on our investment of roughly $450,000," he said.
He added: "Our patients are happier, our nurses are happier, and we're decreasing our total cost of care, which is what everyone should be after."
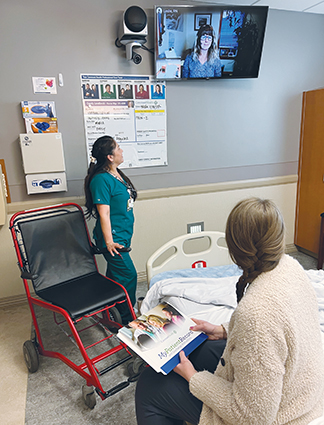
The co-caring teams at Covenant Medical Center in Lubbock, Texas, include a nurse working virtually with the bedside staff. The model, piloted in Lubbock, is being expanded to many other Providence St. Joseph Health hospitals.
The numbers point to efficiencies aside from cost savings. For example, in the past, once a doctor wrote a discharge order, it took four hours to get a patient ready to leave. In the co-caring model, the work is done virtually with the process starting the day before and the time needed cut to 80 minutes.
Such efficiencies help sell nurses on the co-caring system and working from home, Trepanier said.
"We know that the average age of a nurse has gone up and up and up, and many are starting to think about retirement in the next few years," he said. "What a great opportunity, to be able to continue to practice and to support patients where (they) don't have to be on (their) feet for 12 hours a day for three days in a row. That's what we need. We need to bring in more people and to retain those who are practicing today."
Following co-caring's success in Lubbock, Providence is expanding the model to 50 units across its seven-state footprint by the end of this year. Most of the units will be adult inpatient ones, such as medical/surgical, telemetry, step down and orthopedics.
Overcoming inertia
What has stopped hospitals from adopting models like the co-caring one with virtual caregivers until now? Trepanier said a lot of the problem has been simple inertia.
"I've been a nurse for 35 years this year," he said. "The world has changed. You have all sorts of widgets that we didn't have when I first started as a nurse, yet we still approach the work the same way. Nurses are given a group of patients, and they do their thing."
Given the intense current demand for their services, nurses need to practice at the top of their license and the best way to do that is to have support teams to take over some of the simpler chores such as checking vital signs, Trepanier said. Meanwhile, other duties now can easily be done remotely.
"All of the instruction, education, care coordination, all of that stuff can be done virtually," Trepanier said. "And it's oftentimes seen by the nurse at the bedside as an administrative burden. They need to have visual cues and access the patient, but accessing the patient virtually is equally effective. And we've been able to demonstrate that."
In addition to splitting duties with the bedside crew, the virtual nurses remote in for regular team meetings with charge nurses, case managers and physicians.
Team effort
From the nursing point of view, Wilson said, benefits from co-caring grow best when there is good teamwork between the virtual nurse and those who are working on the floor.
"It has to start with the bedside staff really taking the time to explain," Wilson said. "I have had patients as old as 101 years old that love this. Once the patients get to the room, as long as that bedside staff does a very good job explaining what we're going to be doing, it works."
Some patients, Wilson said, are simply lonely and scared and can benefit by knowing someone is as close as the push of a button. In some situations, she added, that button can be a lifesaver.
"There was a patient that was having a heart attack as I came into her room," she recalled. "I was able to immediately address her chest pain and we were able to get the chargers in quickly and immediately get the cardiologist there. There's no telling how much heart muscle we saved for her."
Working differently
The difference from co-caring has been pretty close to what managers like Trepanier envisioned.
"Quite frankly, when we embraced this, even if we could cover our costs and it would be cost neutral, it would be a great proposition," he said. "The pleasant surprise of this is that we're elevating the practice of nurses, the technicians feel a part of the team, and the patients are having a good experience. We're having great operational outcomes and decreasing the total cost of care."
That's good for the present, Trepanier said, and definitely bodes well for the future.
"If we don't do this, we are going to run out of time in health care," he said. "I recognize that not everyone has the resources and not everyone has the capability of pulling something off like that. I also am very cognizant that the status quo is not an option.
"For the sake of our patients and for the sake of the health of the communities that we serve, we all need to lean in and figure out how toapproach the work differently."
