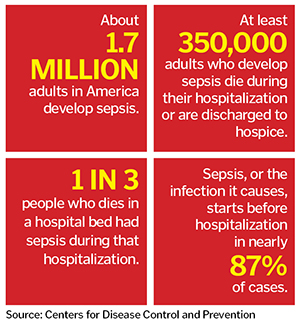
It took nearly 10 years to develop a rapid test for sepsis, the all-too-common, often deadly condition that hospitalizes 1.7 million American adults each year.
With the new test known as IntelliSep, which a team at Our Lady of the Lake Regional Medical Center in Baton Rouge, Louisiana, helped develop, doctors can diagnose sepsis in less than 10 minutes — a game changer for a condition that can become serious quickly but has been stubbornly difficult to detect.

"If your family's going to get one disease that has life-threatening potential, that one is sepsis," said Dr. Christopher Thomas, medical director of system quality and patient safety at Franciscan Missionaries of Our Lady Health System, Our Lake of the Lake's parent.
Dr. Mark Laperouse, medical director of Our Lady of the Lake's emergency department, added that the test is the first new one in a long time for use in emergency rooms, where patients with sepsis most often present.

"We're part of something groundbreaking and we have a test that never existed before," Laperouse said. "It's hard to really talk about that without getting goose bumps."
Threat to health, risk of death
The Centers for Disease Control and Prevention says sepsis is the body's extreme reaction to an infection. The CDC calls developing a protocol to deal with sepsis "essential to optimize patient care." The agency notes at least 350,000 patients who develop sepsis die or are discharged to hospice every year.
Patients who survive sepsis are at increased risk for negative health outcomes, for being unable to return to work and for death, the agency says.
An organization called the Sepsis Alliance, which provides information for health care providers as well as patients and their families, puts the cost of sepsis care for hospitals and skilled nursing centers at $62 billion a year. That figure is the highest for any condition, the alliance says.
Identifying the 'likely septic'
IntelliSep was developed by Cytovale, a San Francisco-based medical diagnostics company, in partnership with a quality and research
team at Our Lady of the Lake. The test, done through a blood sample, analyzes white blood cells and quickly classifies patients into three distinct bands.
Band one patients have the lowest probability of developing sepsis, while band three patients have the highest probability. In that case, hospital personnel can be mobilized with a sepsis alert.
"We're making the entire hospital more efficient by making sure we're treating the correct people," Laperouse said. "Instead of saying everyone is possibly septic, now we have people that are likely septic and likely not septic. It is amazing watching what's happening to the entire hospital because of the way we're focused on this disease process."

Mysterious illness
Despite the prevalence of sepsis, Thomas said, the condition can be a mystery to the general public.
"Over half of the United States, in terms of the patients, don't know what sepsis is as opposed to cancer or acute myocardial infarction, heart attack or stroke," he said. "On the provider side, it's the number one cause of hospitalization in the United States. It's the number one cause of readmission to the hospital in the United States."
Thomas almost lost his father to sepsis when, after a routine prostate biopsy, his father developed a fever and became acutely confused.
"I think they did a fantastic job at the time," he said, "but I often think about if the test had been there at that time, there would have been some trajectory for me to understand what I was dealing with."
For patients who survive sepsis, Thomas added, about half have some alteration of their life related to a complication called post-sepsis syndrome. That condition involves physical and emotional symptoms, such as fatigue and insomnia, that can last for months, the Sepsis Alliance says.
'An extra tool'
Thomas was giving lectures on sepsis about 10 years ago when he learned that a fast-working test was in development. He expressed interest in becoming involved in the research that led to IntelliSep and presented
the idea to Dr. Hollis O'Neal, medical director of research, and other medical leaders at Our Lady of the Lake.
Nine years of testing followed. The test got approval from the Food and Drug Administration in 2022. It was introduced at the hospital last summer.
Now that the rapid test is in use, Laperouse said, "We're watching patients benefit from it, both sick and non-sick patients. It's an extra tool that we've just never had to make decisions on patients that are presenting to the emergency department."
Thomas sees IntelliSep as an advancement in health equity. "If you look at sepsis numbers, disadvantaged groups have worse outcomes in sepsis because unfortunately, nationally, when you have to take a history or when you have areas that are underserved, they may delay in time of presentation or they may have more comorbidities," he explained. "So, by putting in an objective measure on a disease, that's the most significant diagnosis across our health system."
He added that use of the test has "allowed us to be very clear from a mission perspective that independent of environment, independent of background, every patient is going to get the same chance for optimal health, which is our definition of health equity: giving an optimal opportunity to achieve optimal health outcomes in the patients we're privileged to serve."
The use of IntelliSep began at Our Lady of the Lake, with plans to expand to other parts of the Franciscan Missionaries of Our Lady Health System. Laperouse said the wider use will create data that can be analyzed to maximize the effectiveness of the test.
"We're doing this unselfishly and we're making sure we take notes along the entire way, because not everyone's going to be able to expend the resources like we have done just since August first," Laperouse said, referring to the date when Our Lady of the Lake began using the sepsis test.
He added: "We're making sure any facility that ends up using this product will have the blueprints and the road map to be successful. And if we can do that one hospital at a time, one region at a time, one hospital system at a time, we're going to change the outcomes of so many people in this country and maybe the world, hopefully."
