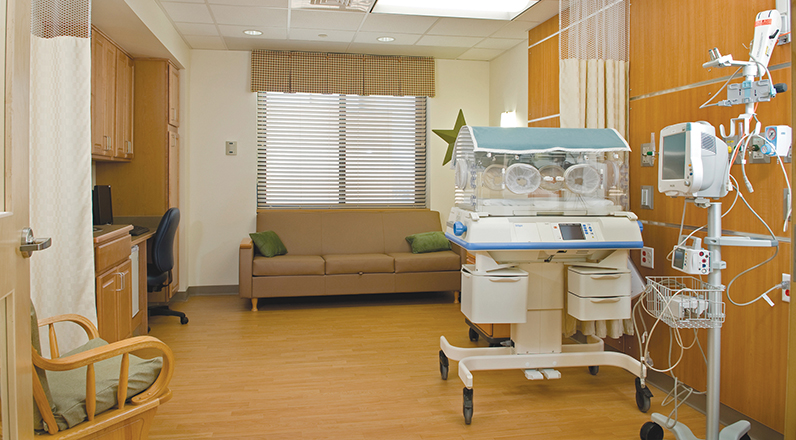
The suites contain the equipment needed to care for both mom and baby. Some of the equipment is in hidden storage areas of the suites.
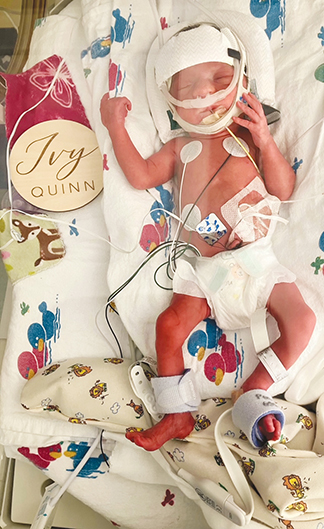
When Janelle Lorento gave birth to her daughter this summer at 30 weeks' gestation, she quickly knew she wanted to be transferred to a different hospital for what she anticipated would be an extended stay. She wanted to go where she and her family could "room in" with new arrival Ivy Quinn and spend as much time as possible bonding with the preemie.
About two weeks after Ivy's birth, mom and baby were transferred to the Neonatal Intensive Care Unit & Family Suites at Catholic Medical Center in Manchester, New Hampshire. Janelle says when she arrived at Catholic Medical Center, "I felt like I could take my first deep breath in weeks."

Unlike most NICUs across the U.S., the one at Catholic Medical Center exclusively offers family suites. Each is a private room with enough space for the baby and mom to receive care as inpatients and for other family members to stay. In the Lorentos' case, Janelle and her husband held, fed, changed and assisted with the care of Ivy in their hospital room. Ivy's brother and sister were able to stay in the room during daytime hours, spending time with their new sister and playing card games, completing homeschool work, eating meals and taking family photos.
Janelle, in a press release from the hospital, says the group enjoyed "making memories as a family of five — all in the comfort of our own, calm, private room."
"It created a sense of normalcy in a very abnormal situation," she says. Ivy was discharged October 30.
Nation's first
Catholic Medical Center says its family suites, opened in 2010, were the first NICU suites in the nation. Tanya Ricci, nursing unit director of the NICU & Family Suites, says a growing number of hospitals now have such suites and are adopting this model of care.
Catholic Medical Center has four suites designed for when moms are inpatients and four smaller suites for when just the infant is an inpatient. Each suite has an isolette or bassinette for the baby, a postpartum bed for mom and sleeping accommodations for one other support person. Each room has hidden storage areas containing the equipment required to care for the baby. The suites all get communal access to a sink, refrigerator, microwave, toaster and coffee maker; a washer and dryer; a private bathroom with a shower and locker; and a family lounge.
Ricci says the NICU suites' setup is "totally different" than what is the norm for most NICUs. What is typical is to have a bay, or a large open area, with the babies' isolettes and a chair or two next to each for parents or other visitors. There usually is a curtain to pull around each isolette for privacy.
Care for the whole family
Catholic Medical Center created the suites to offer not just a different type of space but a different type of care for NICU families. Called integrated care, couplet care, or mom-baby dyad care, it is focused on treating the mother and infant — as well as the other family members — as a unit. Key to the philosophy is that parents and family members should become the primary caregivers of their babies and collaborate with and work alongside the health care team.
The concept also calls for a different staffing model. Ricci says in standard NICUs, a team of nurses usually cares for the babies and most activity happens on a regimented schedule, with the nurses handling virtually all medical interventions. While moms are inpatients, they usually are on a separate hospital unit, cared for by a separate nursing team until their discharge.
In contrast, at Catholic Medical Center, mom and baby are cared for in one room and stay in that room virtually all of the time, with medical care delivered there. Just one nurse works with that family per shift. All of the NICU nurses have expertise in postpartum care of new moms and the care of high-risk infants.
The unit is equipped to provide babies with respiratory support, central venous and arterial access, supplemental nutrition, developmental care and bedside medical care, including eye exams. Trained nurses can provide the eye exams needed for premature babies at risk of retinopathy. The NICU is staffed by neonatologists and advanced practice providers from Darthmouth Health Children's.
Ricci says that in 2021 about 11% of the more than 1,100 births at Catholic Medical Center were to families that stayed in the NICU suites.
Around-the-clock bonding
At Catholic Medical Center family members are encouraged from the start to take an active role in their baby's care. They can hold their babies when they wish and they can change their diapers. Clinicians teach the parents to administer the routine medical care the babies need.
Renee Maloney, service line director of maternal, child and women's health for Catholic Medical Center, says it is usual for families to have to continue medical interventions at home after discharge. She says all the tubes and wires can be very scary to parents, so getting them acclimated to that medical equipment and its use from the start can make them feel much more in control and comfortable when discharge time comes.
Ricci says the essence of this integrated care is that families can spend as much time as possible bonding instead of being separated from their baby, which is typical for NICU families.

The suites in the NICU at Catholic Medical Center have room for mom, baby and family members.
"This speaks to our Catholic mission and values," says Maloney.
She notes that the same integrated care model is used in Catholic Medical Center's Mom's Place, the labor and delivery and postpartum unit of the hospital for moms and babies not requiring specialized NICU care.
Shift of control
The integrated care approach can be jarring for new team members used to other care environments, acknowledges Ricci. Ceding control of extremely fragile infants to parents who may not have a medical background can be difficult for clinicians to do. It helps, Ricci says, that Catholic Medical Center onboarded a team at the same time it opened the unit so all clinical staff "knew what they were getting into." Her team has consulted other NICUs experimenting with integrated care and the transition is more difficult when moving from a standard to integrated care approach, she says.
Ricci says the integrated care model has great potential to improve patient care. Research has shown that the approach can decrease new parents' anxiety and decrease the incidences of postpartum depression. It's also been shown that babies who are born to mothers with substance use disorder often require less pharmacological intervention when they are treated with integrated care. And, moms and babies have a decreased lengths of stay under this care model than those in typical NICUs.
"It's a whole different philosophy," says Maloney. "Our nurses are very good at building trust with families. It's a trusted relationship from the beginning. Our nurses do a lot of coaching."
"It's a unique, compassionate, caring place," she says.
