By JULIE MINDA
In October, for the first time in a decade, a dentist came to provide oral care to residents of St. Michael's Health & Rehabilitation Center in rural Virginia, Minn., and through the same contract the company will be providing quarterly dental hygienist visits.
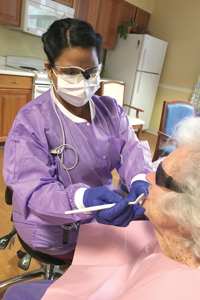
Prior to signing on with this company, said Cheri High, the facility's administrator and chief executive, finding dental providers had been a continual ordeal. She said it is "a challenge that's been going on for quite a few years in the industry, and it stems from the fact that Medicaid does not pay adequately and so many (dental) providers have fled. Many times there's just not a provider willing to take someone new," especially if that someone is an elder with complex dental needs.
While data on the oral health of the elderly and on residents of nursing homes in particular is spotty, broad national studies indicate that unmet dental needs are rising among low-income seniors generally.

Ministry long-term care providers and American Dental Association representatives who spoke to Catholic Health World said the majority of nursing home residents are insured by Medicaid. States can choose whether and to what extent they will cover oral health for adult Medicaid recipients. And, according to the dental association, the ability to find a dentist willing to treat long-term care patients directly correlates with the generosity of the Medicaid fee schedule.
"The reimbursement just isn't there" in every state when it comes to dental benefits for Medicaid recipients, and that causes access problems for low-income adults, said Dr. Steve Geiermann, senior manager, access, community oral health infrastructure and capacity for the American Dental Association. The dental association is advocating for better Medicaid coverage of dental benefits for all adults. The same fee schedule applies for all adults based on the state where they reside, regardless of their age and generally regardless of their outpatient treatment location.

In Minnesota, which has more limited Medicaid dental reimbursement than most states, the new dental services provider, In-house Senior Services, keeps its overhead down in part by using a single administrative staff to cover a suite of services it offers long-term care facilities. In addition to dental services it provides podiatry, optometry and audiology, according to Brad Elbers, co-founder and chief executive of In-House.
Gateway to the body
Wisconsin is among the states the dental association identifies as having relatively good Medicaid dental reimbursement. And yet, even there, according to Dr. Charles A. Hajinian, "The dentist does not even break even seeing Medicaid patients. We consider it an out-of-our-pocket donation to the resident and the state."

Alexian Village in Milwaukee has maintained a contract for decades with Hajinian's dental office. His daughter Dr. Stacy Michels also works in the practice. Hajinian said most Alexian Village residents use private funds for their dental needs. Hajinian estimated that about 5 percent to 10 percent of his Alexian Village patients are insured by Medicaid. (Campus-wide at Alexian Village, about 15 percent of residents are insured through Medicaid).
The dentists and their hygienist treat residents in a two-room operatory dental clinic near the lobby, or in the patients' rooms, if mobility is an issue.
Hajinian said neglecting dental health can lead to medical issues that can be life-threatening to seniors. For instance, he said, oral disease can cause or contribute to coronary heart disease, stroke and even aspiration-pneumonia.
Dental decay
The Administration for Community Living at the U.S. Department of Health and Human Services has said dental access and affordability are particularly problematic for older adults on fixed incomes. Even routine preventive dental care can be expensive when paid out of pocket, and few retirees have private dental insurance.

Analysis released Sept. 27 by the dental association's Health Policy Institute says that low-income seniors aged 65 and older had an untreated tooth decay rate of 42 percent in the 2011 to 2014 time frame, and that figure is up sharply from earlier studies. A 2014 institute brief on Medicaid reimbursement connects the current dearth of providers willing to accept patients with Medicaid coverage to a decline in "dental care use" among low-income adults. In another analysis also released Sept. 27, the institute said only 42 percent of seniors overall had visited a dentist in the prior year. For those who hadn't, 49 percent said cost was the top reason.
Limited access
Even in some states with more generous Medicaid dental benefits, high demand for services from Medicaid recipients can make it difficult to access oral care providers. A February 2015 Colorado Health Institute analysis indicated that while Medicaid expansion and an expansion of adult dental benefits by Colorado had tripled the number of adult Medicaid recipients with dental benefits, the number of registered dental professionals in the state had not increased at a commensurate rate.
While many older adults have difficulty accessing and paying for dental care, "accessing dental care can be especially difficult for nursing home residents," according to the Administration for Community Living.
Nursing home administrators and dental providers connected with Alexian Village; Elizabeth Seton Residence in Wellesley Hills, Mass.; St. Mary Health Care Center in Worcester, Mass.; and St. Michael's said it is usual practice in long-term care facilities that residents who do not resist brushing and flossing receive this preventive care daily; those who resist often receive dental rinses. Most often, certified nursing assistants perform this care.

Dr. Jane Grover, the dental association's director of the Council on Access, Prevention and Interprofessional Relations, noted there is insufficient data on the oral health status of nursing home residents and service availability because facilities are not required to track this aspect of resident health. The dental association is advocating to change that, and that data could strengthen their case for greater Medicaid reimbursement.
But, reimbursement is not the only hurdle to dental care for the elderly.
For some seniors with mobility issues or limited access to transportation, it can be a challenge to get to and from the dentist's office. That's true in spades for many residents of nursing homes that lack the services of a visiting dentist.
Before it set up its contract for in-house dental care, St. Michael's had some success sending patients to a local dental college for basic services. But, at times it has had to transport residents as far as 200 miles for advanced dental services, and that may be required in the future, albeit to a lesser extent. "That is really hard on residents who are compromised anyway — to put them in a medical van for three or four hours," said High.

Medical risk and complexities
The dental association's Geiermann said many general dentists are reluctant to treat the elderly because of the potential for added complexity.
An oral health fact sheet from the dental association says people aged 65 years and older who have preexisting medical conditions may:
- take multiple drugs that make them vulnerable to adverse reactions
- have physical, sensory or cognitive impairments that make communication with them or treatment of them difficult
- have certain dental conditions that are associated with aging that make them sensitive to dental drugs, including analgesics.
Suzanne Whitty, Alexian Village's administrator, said, "The dental providers must be creative and dedicated because in terms of physically working with the elderly, it's not routine, and it's difficult for most providers to do."
Reimbursement concerns, out-of-pocket costs curtail dental use by seniors The high cost of dental care is at the heart of the dental neglect issue among seniors. A 2016 report, "A State of Decay, Vol. III," from the nonprofit organization Oral Health America, said 58 percent of lower-income older adults have no plan in place to pay for dental care once retired and 52 percent of all older adults are either unsure or don't know that Medicare does not include dental coverage. While the report does not break out "older adults" beyond those 65 and older, it flags significant funding issues for oral health. According to a Kaiser Family Foundation issue brief, Medicaid is the main source of both coverage and financing for long-term care facility residents. States can choose whether and to what extent they will cover oral health for adult Medicaid recipients. According to a February 2015 Kaiser Health News article, almost half of the U.S. states either don't provide adult dental coverage through Medicaid or only cover emergencies. An October 2014 research brief from the American Dental Association's Health Policy Institute said that even in states that provide dental benefits, fee-for-service reimbursement rates have dropped in recent years. In 2014, the average Medicaid reimbursement rate for adult dental care services in those states was 40.7 percent of the usual and customary fee that a commercial insurer would pay for the same services. In part because of the reimbursement shortfall, in many states there is an insufficient number of dentists available to treat adult Medicaid patients, said the brief. Steve Geiermann, senior manager, access, community oral health infrastructure and capacity for the American Dental Association, said facilities can make some headway to secure reimbursement for medically necessary dental care for residents by requesting payment from Medicaid for "Incurred Medical Expenses." This payment mechanism often is used for eyeglasses, hearing aids and the like, but many facilities are unaware it can be used for some dental needs that are not covered by the standard Medicaid plan or other third party payer, he said. Dr. Greg Folsc is a member of the dental association's National Elder Care Advisory Committee. The dentist said the Incurred Medical Expenses reimbursement can be used, whether or not the recipient's state covers dental care under Medicaid. The dental association provides instructions on its website on using this reimbursement source. |
Coverage of dentures varies According to a 2002 analysis from the Centers for Disease Control and Prevention, the percentage of older adults who have retained their natural teeth has increased steadily in the U.S, and at the time of the report that trend was expected to continue. The CDC says about 25 percent of adults aged 60 years old and older no longer have any natural teeth. Healthcare Bluebook, a company that uses cost data to estimate the costs of health care products and services, says that complete dentures cost on average more than $1,300 in the U.S. For low-income people insured by Medicaid, the out-of-pocket expense for dentures varies by state of residence. A Kaiser Family Foundation resource says 37 states cover dentures through their Medicaid programs; eight of those states require a co-pay. The co-pay varies by state, with most of the eight states charging $3 or $5 per denture, or per visit or per episode of treatment. Florida and Missouri charge a percentage of the payment. For instance, Missouri recipients pay 5 percent of the payment for dentures and related services. |
