(Updated from the original version)
Editor's note: Since this story published, several other Catholic health care systems have announced that they will require vaccinations. PeaceHealth announced a vaccine mandate that goes into effect Aug. 31. Providence St. Joseph Health is requiring compliance by Sept. 30. St. Mary's Healthcare is requiring vaccinations by Oct. 1. CommonSpirit Health put a mandate in place that takes effect Nov. 1. SCL Health also is requiring proof of vaccination by Nov. 1. The Franciscan Missionaries of Our Lady Health System announced a vaccination mandate without specifying a date for compliance.
At least four Catholic health systems that together have about 350,000 workers have decided to require COVID-19 vaccines, citing studies that show the shots are safe and effective.
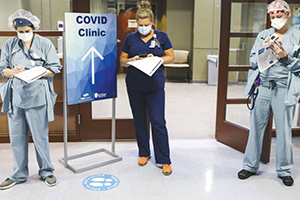
SSM Health announced its policy in late June; Mercy and Trinity Health announced theirs in early July; and Ascension announced its on July 30. The policies extend to volunteers, and at least for Mercy, Trinity Health and Ascension, vendors who work in the systems' facilities. The systems will allow people to request exemptions because of vaccine-related health issues or religious objections.
Representatives from several other Catholic health systems, including CommonSpirit Health, PeaceHealth, Providence St. Joseph Health, Hospital Sisters Health System, SCL Health and Benedictine, said that while they are strongly encouraging staff and volunteers to get vaccinated, they are not requiring immunization as a condition of employment.
In May, the U.S. Equal Employment Opportunity Commission issued guidance that said federal laws "do not prevent an employer from requiring all employees physically entering the workplace to be vaccinated for COVID-19." The guidance said the policies must provide reasonable accommodations to conform with other federal laws, such as the Americans with Disabilities Act and the Civil Rights Act.
The National Academy for State Health Policy reports that the federal guidance has prompted several states to pass or consider laws that ban COVID vaccination mandates.
Setting an example
For SSM Health, the decision to mandate vaccinations came down to three factors, said Dr. Shephali Wulff, the system's director of infectious diseases.
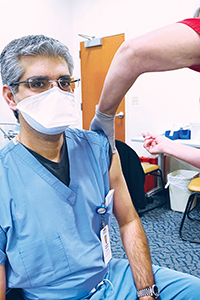
First was an evaluation by the system that showed the rate of serious side effects from the vaccines is extremely low while their efficacy is extremely high. Second was timing. Missouri, where SSM Health has its largest presence, was at or near the top of states in rates of new infections in late June and cold and flu season was nearing, which typically heightens demand for respiratory care.

The third factor was a desire to set an example for the communities SSM Health serves.
"We felt strongly that, as a health care organization, we show the communities that we take care of that we believe in the science of these vaccines," Wulff said.
Dr. Tammy Lundstrom, Trinity Health's senior vice president and chief medical officer, said safety was at the forefront in that system's decision to mandate vaccination. Safety is a core value for Trinity Health.
"We feel it's our responsibility to provide safe care and, for the common good in our communities, that we need to be vaccinated to prevent spread and prevent propagation of additional variants that may at some point escape vaccine," Lundstrom said.

All three systems said their requirements for proof of full vaccination include staffers working remotely.
Ready access
Trinity Health set a deadline of Sept. 21 for proof of full vaccination; for SSM Health and Mercy the deadline is Sept. 30; and for Ascension it is Nov. 12. The systems said the dates were picked to allow time for workers to get shots and for those inoculations to be in full effect.
Lundstrom said Trinity Health had given well over a million vaccines in the 22 states where it operates by early July. Access to vaccines is not an issue for staff, she said, noting that in many places, the shots are available on a walk-in basis.
Mike Hubert, vice president for communications at Mercy, said that he had recently been told by an epidemiologist studying the COVID-19 variant spread that because of the transmissibility of the delta variant, reaching herd immunity would require a vaccination rate or post-infection rate of over 90%. Hubert said that means there is almost no chance for someone who hasn't had a vaccine or the virus to avoid infection in a community where the delta variant becomes prevalent, which has now happened in most parts of the U.S. Some of those infected will be asymptomatic as has been the case with prior variants.
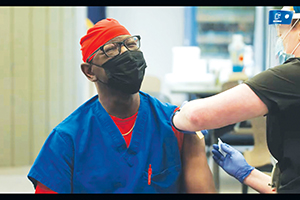
In its media release about its vaccination requirement, Mercy noted that most of the hospitalized patients the system was treating for COVID had not been vaccinated.
"What we are seeing aligns with the Associated Press analysis of CDC data," Dr. John Mohart, Mercy's senior vice president of clinical services, said in the release. "More than 95% of recent hospitalizations across the U.S. are people who aren't vaccinated. The data is clear. Vaccination is key to saving lives."
Ready for pushback
Since Trinity Health leaders expected some pushback on the new policy from workers, Lundstrom said the rollout was accompanied by plans for town halls to address workers' questions and concerns.
"We respect people's personal decisions and don't believe that everybody will be positive regarding this decision but with safety as a core value it was something that we felt compelled to do," she said.
Wulff said SSM Health has ongoing efforts to educate workers about the safety of the vaccines. Those efforts have included town halls, virtual meetings, videos and emails.
SSM Health managers also are making themselves available in person and by email to answer questions about the shots and the vaccination requirement. She pointed out that the system, like others, already requires proof of other vaccinations, such as those for measles, mumps and rubella and for diphtheria.
The system also requires annual flu shots, which have an efficacy rate far below what studies have shown for the three COVID vaccines approved for use in the U.S.
SSM Health did take into consideration that the vaccines have so far only been approved for emergency use, Wulff said, but the available data convinced the system's leaders of their safety and value.
Coaxing rather than requiring
Among the systems surveyed by Catholic Health World that said they were not requiring vaccines for staff, several declined to elaborate on their policies.
PeaceHealth shared a statement from Chief Physician Executive Dr. Doug Koekkoek. It acknowledged that the Pfizer, Moderna and Johnson & Johnson vaccines all have been shown to be "very safe and effective" and noted that most of the system's caregivers have been vaccinated.
Koekkoek went on to say: "While we are actively monitoring the regulatory environment, we have no current plans for mandatory COVID-19 vaccination and remain confident in our ability to provide a safe care environment with the high rates of vaccination that we have today."
SCL Health shared a statement that said in part: "COVID-19 vaccination remains voluntary at all SCL Health locations at this time. However, as health care providers, we have a more significant role and responsibility to ensure we are doing everything we can to slow the spread of COVID-19. This is why we strongly encourage our associates to get vaccinated to protect themselves, their loved ones, our patients, and the communities we serve."
Vaccine incentives
Benedictine, a senior care provider, is leaving the decision on whether to be vaccinated up to employees, but it is offering incentives. Workers at the system's 30 long-term care communities who show proof that they are fully vaccinated by Aug. 1 will be entered into a drawing for prizes, including $2,500 cash. Also, the communities that post the highest vaccination rates or the biggest jump in vaccination rates during the competition will win group meals. Winners will be announced in mid-August.

"I think for us it was one of those things where have we used every tool in the tool kit around encouraging vaccines," said Kathleen Murray, the system's training and development manager. "We thought, well, one of the things we haven't done is a vaccine competition so let's give this a try and see if it works."
At the start of the competition, the vaccination rate among communities ranged from 32% to 81%. Murray said that many employees who were vaccinated hadn't turned in proof. In the first weeks of the competition, the system's overall vaccine rate jumped by 4% to 62.6% due in part to people bringing in copies of their vaccination cards. "Just even that kind of movement, we are very happy with," Murray said.
To encourage the competition, Benedictine is emailing a leaderboard each week so communities can see where they stand along with stories from once-hesitant staffers who have changed their minds about getting vaccinated. Communities are posting their vaccination rates and fliers with the stories on bulletin boards.
Data backs decision
Wulff said that the data on the safety of the vaccines is overwhelming. She pointed to findings by the Centers for Disease Control and Prevention that of the 331 million doses of COVID vaccines given in the U.S. through early July, the rate of potentially related deaths was miniscule, at about 0.0018%. The CDC said that — at 2 to 5 incidents per million — the risk of developing anaphylaxis from any of the vaccines is low.
The CDC and the Food and Drug Administration reported that as of July 19, with 13 million doses of the Johnson & Johnson vaccine administered, 39 individuals developed thrombosis with thrombocytopenia syndrome. In mid-July, the FDA also warned that the J&J vaccine could lead to a slight risk of the rare neurological condition known as Guillain-Barre syndrome.
Wulff said her personal pitch to anyone still hesitant to get a COVID shot is that the vaccines are the best hope to end the lingering crisis.
"The only way for us to get out of this pandemic safely is for people to get vaccinated," she said. "The longer we wait, the more people that remain unvaccinated, the more time there is for variants to arise. The delta variant might be our scariest variant right now, but the longer we wait the more of these variants there will be until we really just don't have time to wait."
