 Our nation has a unique opportunity to reimagine long-term care, particularly related to the direct care workforce. Direct care workers — such as certified nursing assistants, home health aides and personal care aides — are the backbone of
the long-term care system, delivering hands-on care to older adults and individuals with disabilities. The COVID-19 pandemic shined a light on the essential care delivered by these workers and how the health care system and communities suffer when
that care is not available.1
Our nation has a unique opportunity to reimagine long-term care, particularly related to the direct care workforce. Direct care workers — such as certified nursing assistants, home health aides and personal care aides — are the backbone of
the long-term care system, delivering hands-on care to older adults and individuals with disabilities. The COVID-19 pandemic shined a light on the essential care delivered by these workers and how the health care system and communities suffer when
that care is not available.1
Research and resources from the FrameWorks Institute, a nonprofit policy research organization, are now available to help advocates of long-term care take advantage of this moment to deepen public understanding of direct care work and build public will to make the necessary investments in the long-term care system. By doing so, direct care workers will see structural changes — like better pay and working conditions — that reflect their immense value to the health care delivery system and society.
A WORKFORCE RUNNING ON EMPTY
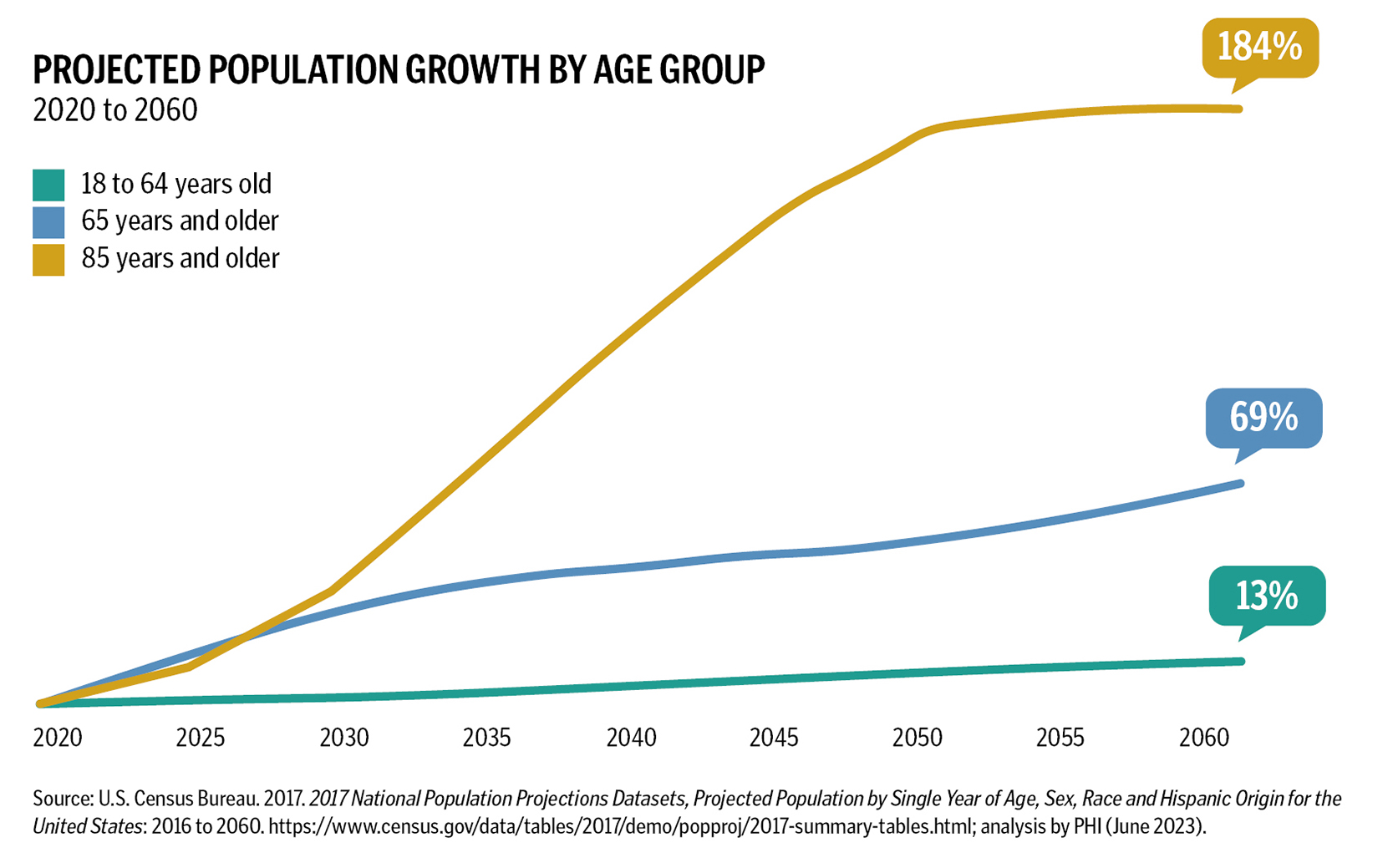
As the U.S. population continues to age rapidly, more direct care workers will be needed to provide care in the home, community and nursing homes. From 2020 to 2060, the population of adults age 65 and
older in the U.S. is projected to increase from more than 56 million to almost 95 million.2 The number of adults age 85 and older is expected to nearly triple over the same period from more than 6 million to 19 million.
In contrast to the rapid expansion of the older adult population, the population of adults ages 18 to 64 is expected to remain relatively static, which means that there will be fewer potential paid and unpaid caregivers available to support older adults. Currently, the ratio of adults ages 18 to 64 to adults age 85 and older is 30 to 1, but that ratio is projected to drop to 12 to 1 by 2060.3 (See figure on page 67.)
As a result, ways to address the long-term care workforce shortage are of special interest to policymakers. However, issues facing the direct care workforce are long-standing and entrenched. Chronic underfunding by public programs, a high rate of part-time work and limited career advancements make it difficult for long-term care organizations to attract and keep direct care staff. These shortages can contribute to burnout for existing staff as they work extra hours and multiple roles to care for residents. This often results in high turnover.4
As policymakers consider solutions, FrameWorks' resources can help advocates ensure that the responses are not crisis-driven — which can be fragmented and time-limited — but based on the understanding that direct care, as an integral part of a strong and thriving long-term care system, is always essential and valuable.
SHIFTING MINDSETS
The FrameWorks resources are based on a multiyear research effort conducted with the support of national aging organizations.5-7 The research on care work is part of a larger culture change project being
conducted by FrameWorks, which is exploring shifting patterns of thinking during this time of great societal change brought on by the pandemic and the racial justice protests. The research on care work is intended to help advocates take advantage
of this increased focus on direct care and nursing homes by equipping them with evidence-based advice to shift how the public thinks about care work, who provides it, and how we value and support it.
The resources, provided through the FastFrames: Aging & Care online series, provide specific guidance on framing issues around quality care, direct care and ageism.
How to frame quality care:8
1) Quality care means different things to different people, so it is important to describe quality by giving clear examples, things like residents having a say over when they wake, what they
eat and what they wear.
2) Keep people engaged by using clear language, explaining technical terms and spelling out acronyms, since most people will not have the same understanding of the issues and industry.
3) Offer examples of what is working, since the public rarely hears this side of the issue. Give examples of what quality looks like in practice, such as how interdisciplinary teams — including nurses, aides and social workers — work together to provide individualized care for their residents. Make sure to include nonmedical examples as well.
How to build support for our care workforce:91) Emphasize direct care work as skilled work, not just work done by caring individuals. People tend to think that good direct care is delivered by people who have innate caring traits versus a learned skill set. Therefore, it is important to describe the skills of direct care work, such as the ability to recognize when a resident with dementia is becoming agitated and how to de-escalate the situation. Showing policymakers that good direct care is the result of a trained workforce makes it easier to make the case for better pay and working conditions.
2) Talk about care work as a societal good, not something just needed in a crisis. As the acute impacts of the pandemic abate, the public needs to understand that a strong long-term care system with well-supported workers helps older persons, their families, the economy and society as a whole.
3) Identify specific and feasible solutions to support care workers. Advocates should help policymakers understand that care workers need jobs that reflect their skills and experience, such as higher wages, better benefits and career advancement.
How to talk about ageism:101) Explain what ageism is and its impact on how our care system is structured and funded. If older adults are not seen as valued members of society, what is the impact on the programs that should support them? For example, talk about how ending ageism means making sure that funding is available, so everyone has access to the care they need.
2) Make it about justice, not sympathy or charity for older people. Framing aging as a justice issue helps people understand that older adults are equal members of society and have the right to be full participants in economic and political life.
3) Emphasize how everyone benefits from addressing ageism. For example, when we end ageism, we can build a care system that provides person-centered care for residents and better pay and working conditions for the workforce. It also acknowledges that care for older adults is not the sole responsibility of families but should be shared with society.
TREASURING THE 'WEALTH OF YEARS'
The care system envisioned by FrameWorks' research — a system that is fair, just, serves all and is seen as a societal good — echoes a note issued by the Pontifical Academy for Life in
2021 titled "Old Age: Our Future. The Elderly After the Pandemic." Acknowledging the devastating impact of the pandemic, the Vatican document calls for a new attitude and approach to how older persons are viewed and cared for by not just institutions
but by families, church ministries and all segments of society, including young people, media and businesses.
The note states the new approach should be rooted in the view that being elderly is "a gift from God and a huge resource, an achievement to be safeguarded with care, even in case of disabling illnesses when the need emerges for integrated care and high-quality assistance. … the 'wealth of years' is a treasure to be valued and protected." The document also recognizes that these changes depend on new public health policies that address how to care for older persons that are based on "an ethic of the public good and the principle of respect for the dignity of every individual."11
As Catholic health care continues to partner with other long-term care advocates to reimagine care for older persons, it is more important than ever that it brings its core Catholic principles to policy discussions, especially as more and more nursing homes are sold to for-profit or private equity entities.12 A long-term care system shaped by human dignity, the common good, the dignity of work and solidarity will always prioritize and value the well-being of residents, their families, care workers and society.13
INDU SPUGNARDI is senior director, community health and elder care, for the Catholic Health Association, Washington, D.C.
NOTES
- Dave Muoio,"Hospitals Forced to Delay Patient Discharges as Nursing Homes and Rehab Center Face Major Staff Shortages," Fierce Healthcare, January 14, 2022, https://www.fiercehealthcare.com/hospitals/nursing-homes-snfs-facing-pandemic-labor-challenges-force-hospitals-to-delay-discharges;"Action Needed Now to Shore Up Aging Services Workforce: Finding from LeadingAge Snap Poll," LeadingAge, July 12, 2022, https://leadingage.org/action-needed-now-to-shore-up-aging-services-workforce-findings-from-leadingage-snap-poll.
- "Direct Care Workers in the United States: Key Facts 2023," PHI, 2023, https://www.phinational.org/wp-content/uploads/2023/09/PHI-Key-Facts-Report-2023.pdf.
- "Direct Care Workers in the United States."
- "Direct Care Workers in the United States."
- "Public Thinking About Care Work in a Time of Social Upheaval: Findings from Year One of the Culture Change Project," FrameWorks, October 28, 2021, https://www.frameworksinstitute.org/publication/public-thinking-about-care-work-in-a-time-of-social-upheaval/.
- "Public Thinking About Care Work: Encouraging Trends, Critical Challenges," FrameWorks, April 2023, https://www.frameworksinstitute.org/wp-content/uploads/2023/04/PublicThinkingAboutCareWork-April2023.pdf.
- "Communicating About Nursing Home Care: Findings and Emerging Recommendations," FrameWorks, March 2022, https://www.frameworksinstitute.org/wp-content/uploads/2022/04/Communicating-About-Nursing-Home-Care_2022.pdf.
- "Fast Frames Aging & Care: Episode 1 – How to Frame Quality Care," YouTube, November 28, 2023, https://www.youtube.com/watch?v=knoLWphjDqc&list=PLvvMeV06tVRfwFoXmx49DK32a9Ogt7Htm&index=2.
- "Fast Frames Aging & Care: Episode 2 – How to Build Support for the Care Workforce," YouTube, November 28, 2023, https://www.youtube.com/watch?v=O93TWlT5uS0&list=PLvvMeV06tVRfwFoXmx49DK32a9Ogt7Htm&index=3.
- "Fast Frames Aging & Care: Episode 3 – How to Talk About Ageism," YouTube, November 28, 2023, https://www.youtube.com/watch?v=_qIj9zpclas&list=PLvvMeV06tVRfwFoXmx49DK32a9Ogt7Htm&index=4.
- "Old Age: Our Future — The Elderly After the Pandemic," The Holy See, February 2, 2021, http://www.vatican.va/roman_curia/pontifical_academies/acdlife/documents/rc_pont-acd_life_doc_20210202_vecchiaia-nostrofuturo_en.html.
- Fr. Charles E. Bouchard and Alec Arnold, "Sponsors and the Crisis in Long-Term Care: Is This a 'Man from Macedonia' Moment?," Health Progress 102, no. 1 (Winter 2021): 5-10.
- Sr. Bernadette Matukas, MVS,"A Response to Challenges in Long-Term Care," Health Progress 103, no. 1 (Winter 2022): 13-15.
