Palliative care is core to the work of the Catholic health care ministry. By helping patients get relief from the symptoms, pain and stress of a serious illness, the care adds value beyond its ability to reduce health care costs, said speakers at a webinar
hosted by CHA.

"It is better quality care. It's the way we want to care for people," said Sarah Hetue Hill, the regional vice president for mission integration for CHRISTUS Santa Rosa Health System and CHRISTUS Children's.

Hill discussed palliative care along with Maria Gatto, chair of CHA's Palliative Care Advisory Council and a palliative care consultant. The webinar on July 26 was called "Palliative Care: Connecting Catholic Health Care's Mission & Today's Quality and Business Imperatives."
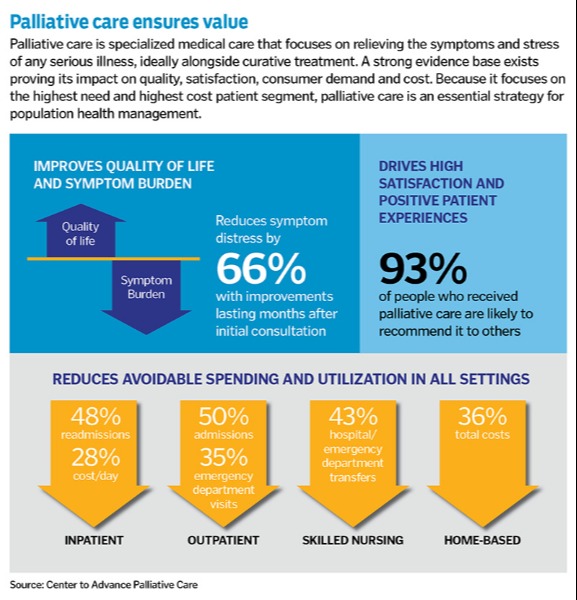
Palliative care treats the whole person – mind, body and spirit. It can be provided at any stage of the illness by a team of trained specialists that includes doctors, nurses, social workers, chaplains and other care specialists. Studies show that those who receive palliative care may spend fewer days in the hospital, have fewer emergency room visits, improve their quality of life, and may even live longer, according to the Center to Advance Palliative Care. The center offers health care professionals and organizations resources to provide high-quality and equitable care for people living with serious illness.
"Those of us who are very passionate about palliative care like to say that it's truly a hallmark of who we are, and that's because it stems directly from our history and our legacy," said Hill.
She pointed out that the word "palliative" comes from the Latin root of "palliare," meaning to cloak – like extra protection to shield people from harm. She noted that Jesus cared for the mind, body and spirit of lepers and a hemorrhagic woman by healing them not only physically but also spiritually by returning them to their communities. Many other groups and religious orders have followed suit over the years by attending to the whole person, she said.
Pope John Paul II, Pope Benedict XVI and Pope Francis have all spoken out and supported palliative care, she pointed out. Pope Francis said palliative care recognizes "the value of the person."
Who can use palliative care?
Gatto outlined case studies of those who could use palliative care:
- Mike, a family man diagnosed with head and neck cancer, needs help coordinating care so he can receive pain management for his symptoms alongside curative treatment.
- Anne, a young woman experiencing pain and disability after a mastectomy, needs coordination between close cancer monitoring and pain management so she can sleep through the night and return to the gym.
- Martha, who has worsening dementia and arthritis, needs support alongside her husband Bernard, who wants to care for her at home. Her team is managing her symptoms, assessing her home for fall risks and coordinating her care.
"It's an extra layer of support," Gatto said. "It doesn't take over the care, but it adds more support. ... It's about living well and being at home to get the best possible care to control your serious illness, and it helps to coordinate all your providers talking together."
Coordinating to fill a need
She pointed out that the Palliative Care Quality Collaborative is the only unified national registry of specialty palliative care data. Care providers can use the data to look at other programs to see
how their work measures up and where to focus resources, she said.
Palliative care is key to supporting an aging nation. The population of people aged 85 and older will more than triple by 2060, Gatto said. Surveys show that patients want palliative care once they are informed about it, she said.
"The Case for Hospital Palliative Care," a publication from the Center to Advance Palliative Care, says the care improves patients' quality of life and reduces health care costs, including by reducing the need for emergency and intensive care. For a midsized hospital conducting 500 palliative care consultations each year, the center says savings can add up to more than $1.6 million a year.
"So get out your calculator, because if you look at these numbers, that is the huge value of that business imperative," Gatto said.
She pointed out that more than 83% of U.S. hospitals with 50 or more beds had a palliative care program in 2020, up from just over 24% in 2000. Palliative care has been one of the fastest-growing fields as health care organizations, health plans and policymakers have recognized the improvement and quality that also reduces costs.
Gatto said health systems should focus on sustainability and growth strategies. Among the things they can do: work on quality standardization, improve financial coding and billing practices, identify patients sooner, improve staffing models, and focus on team health and resilience.
Hill said that while hospitals are struggling financially, it's imperative to remind senior leaders of the hospital's mission and the work of their founders. "This is the work that they started with. So, let's bring it back to this," she said.
