In the summer and fall of 2025, the Center for Applied Research in the Apostolate (CARA) conducted a survey of those working in professional spiritual care within Catholic health ministries in the United States. This study, commissioned by CHA and the National Association of Catholic Chaplains (NACC), sought to learn from those who lead and serve spiritual care through Catholic health care institutions and Catholic chaplaincy. This follows a similar effort in the fall of 2018, when CHA and NACC first commissioned CARA to bring a more scientific approach to studying trends in health care chaplaincy and spiritual care departments. For more than 25 years, CHA and NACC have partnered to study these trends.
The participants surveyed were employed by a CHA member ministry or were members of NACC. The survey was designed in three parts to assess participants based on their specific roles within the spiritual care team. Part One was for professional health care chaplains and those who support spiritual care and included questions on demographics, health care settings, roles and responsibilities. Part Two was for leaders who oversee spiritual care departments and included questions on organizational structure, staffing, professional standards, training and documentation. Part Three, solely sponsored by NACC, was intended for leaders who oversee spiritual care departments in partnership with their human resources leader, and asked questions on job requirements, compensation and benefits for spiritual care personnel and comparative data for social workers.
The 748 respondents included spiritual care workers and those with direct oversight of spiritual care personnel or a spiritual care department. The findings add to the insights gained in the 2018 survey1 and in-house surveys conducted in 1998 and 2008.
WHO SERVES IN SPIRITUAL CARE MINISTRY?
The survey sought to identify demographics of the "average" respondent, and slightly more than half are female (53%) and self-identify as non-Hispanic white (70%). Ninety-three percent indicate they use English primarily in their ministry. The average age of respondents is 57, with the youngest being 28, and the oldest is 96.
Many self-identify their faith as Catholic. Overall, 56% of respondents are Catholic and 32% are Protestant or some other Christian faith. Some selected some other faith, and among these respondents, many cited a specific Christian denomination. One percent of respondents self-identified as Jewish. One percent indicated they did not have a religious affiliation. Twelve percent are Catholic priests, 2% Catholic permanent deacons, 41% Catholic professed religious or lay people, and 45% other non-Catholic clergy or lay people.
The most common precursor to health care ministry is parish ministry. Prior to their current health care ministry, 46% indicated they were working full-time in parish ministry. Twenty-eight percent were working in education and 19% in a ministry outside of a parish or health care setting. Sixteen percent were working in the nonprofit sector, and 12% in some other health care profession. Twelve percent were in the for-profit sector and 5% in government. Three percent were involved in social work full time.
Respondents are most often certified for their positions and highly educated. Seventy-one percent of respondents are board-certified chaplains. Sixty-nine percent have 4 units of clinical pastoral education (the standard amount needed for board certification). Six in 10 have a bachelor's degree, 45% a master's in Divinity, 47% a master's in theology, spirituality or related field, and 24% some other master's degree. Twelve percent have a doctorate.
A call to ministry is most often cited as the reason for working in a spiritual care role. The factors selected as most important (or "very much" a factor in the survey's language) to the decision to enter health care ministry were: feeling called to this ministry (87%), always wanting to help others (77%), their superior or supervisor asked them to do so (71%), a feeling that this ministry would fit their personality (53%), and liking the work environment (50%).
Fewer than half of respondents cited the following as being "very much" of a role in their decision to enter their ministry: felt it would be a good step in their career (48%), wanting to develop a particular skill set (34%), felt that it offered good work-life balance (26%), wanting to try something new (25%), needing a change to another ministry setting (21%), without looking found the position was open (17%), wanting to earn a better salary (13%), and moving from being a volunteer chaplain to a full-time commitment (10%).
SETTINGS OF CARE
Respondents were asked to indicate the various settings in which they provide spiritual care and could select more than one setting. Seventy-three percent say they serve in a general, community or regional hospital. Fifty-one percent serve in hospice or palliative care. Other common places where chaplains serve are in academic medical centers (43%), outpatient clinics or emergency departments (41%), mental or behavioral health settings (38%), critical access or rural hospitals (34%), and pediatric hospitals (27%).
Respondents are most often certified for their positions and highly educated. Seventy-one percent of respondents are board-certified chaplains.
Sixty-nine percent indicate their work is at the local level and 17% say they work regionally. Five percent work at the state level and 6% work at the national level. Three percent indicate some other geography, including multiple states, citywide and international.
Eighty-two percent indicate their current employment is full-time, 14% part-time, 2% are on call, and 2% indicate some other arrangement. On average, respondents spend 54% of their time on patient and family care services and 26% on administrative work. Twenty percent, on average, is spent on staff support.
Two-thirds of chaplains say that a Catholic chapel is available in their facility. Forty-seven percent say an interfaith chapel or room is available. Three in 10 say they have a meditation room available in their facility. Thirteen percent have a multipurpose room available to them. Five percent do not work in a facility, and another 5% note the availability of some other facility.
On average, respondents have been serving in spiritual care in a health care setting for 11.8 years (median of 10 years). The minimum time served is less than one year, and the maximum is 44 years. Overall, the largest segment, 36% of respondents, has been serving for 10 to 14 years.
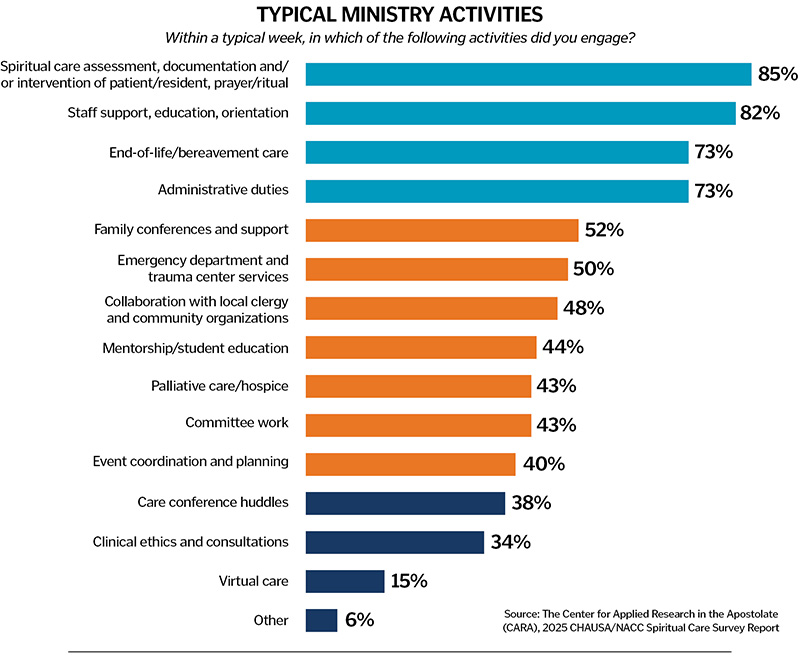
TYPICAL MINISTRY ACTIVITIES
The figure above shows the allocation of time reported by respondents by three frequency groupings. The first are those activities done by 73% to 85% of chaplains (in other words, most chaplains do these things). The second is done by 40% to 52% of chaplains (some chaplains do these things), and the final grouping is done by 38% or fewer (fewer chaplains do these things).
Eighty-five percent of chaplains engage in spiritual care assessment, documentation and/or intervention (including prayer and/or ritual). Eighty-two percent are involved in staff support, education and/or orientation. Seventy-three percent are involved in end-of-life and bereavement care. Also, 73% are engaged in administrative duties.
Fifty-two percent are involved in family conferences and support and 50% in an emergency department and trauma center services. Forty-eight percent are engaged in collaboration with local clergy and community organizations. Forty-four percent are engaged in mentorship and student education. Forty-three percent are involved in palliative care or hospice ministry. Forty-three percent engage in committee work. Four in 10 are involved in event coordination and planning.
Thirty-eight percent are involved in care conference huddles. Thirty-four percent are engaged in clinical ethics and consultations. Fifteen percent are engaged in virtual care.
CHALLENGES TO THE PROFESSION
Respondents were asked, "What do you consider to be the biggest challenge facing the profession of chaplaincy in health care?" Some 569 respondents wrote responses, which were grouped into eight broad categories (see table below). Examples in the respondents' own words are provided for the top three responses.
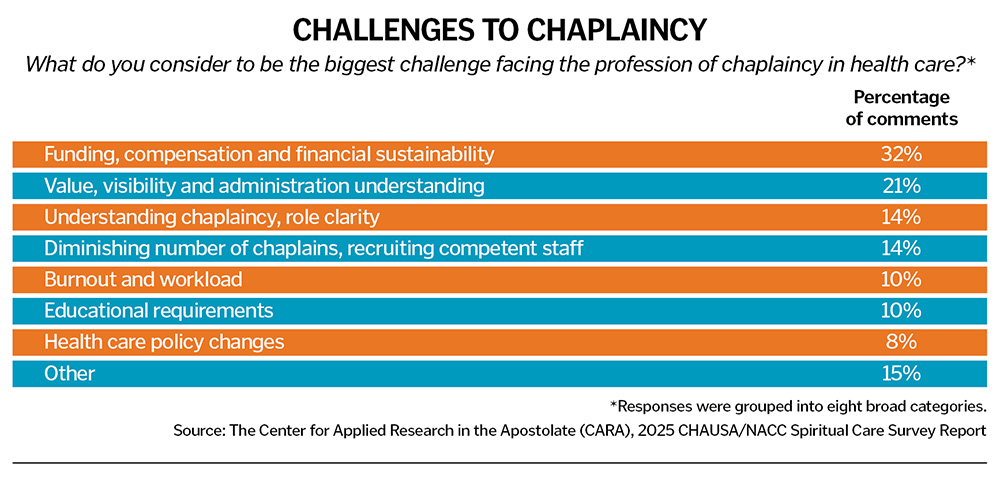
Nearly one-third of respondents identify funding, compensation and overall financial sustainability as the most significant challenges facing their profession. The following are selected excerpts from their responses:
- Low compensation. The amount of time, work and education required to become a chaplain is very high, but we remain significantly underpaid compared to similarly trained and skilled health care workers. We are highly trained professionals, but health care does not often recognize compensation commensurate with our education.
- Lack of funding will increase noncertified staff and weaken the need for certified chaplains. This will also have consequences.
- Financial constraints, dwindling funding — chaplaincy does not create a revenue stream directly.
About 2 in 10 respondents report concerns about their perceived value, noting a lack of visibility and a feeling of being undervalued or insufficiently understood by hospital administration. The following are a few of their comments:
- Compensation held down by historically low salaries, lack of hospital management's understanding of the importance of chaplaincy to the institution.
- Even in health care settings where chaplaincy is seen as beneficial, it is often 'looked down on' by administrators and is often one of the first programs to be reduced when budget changes are made.
More than 1 in 10 respondents report that patients, families and other hospital staff lack a clear understanding of chaplaincy and its role within health care settings. Following are a few of their responses:
- A general misconception among patients, families and other staff members that spiritual care is only for "religious" people.
- The other professions do not have proper understanding of the chaplain's ministry. There is constant education to staff members of other disciplines.
- I think that chaplains need to be able to move beyond the acute care setting and serve where patients are primarily located. I also think that chaplains need to recognize that fewer and fewer of our patients are connected to religious organizations and that we may be the sole provider of spiritual care to patients long-term.
- I think one of the biggest challenges is meeting spiritual and emotional needs of increasingly diverse populations. It requires cultural humility, interfaith knowledge and strong communication skills.
PROJECTED YEARS OF WORK
Three percent of respondents plan to work in spiritual care in a health care setting for one more year or less. One in 5 plans to serve two to five more years. Seventeen percent plan to serve six to nine more years. Twenty-one percent plan to serve 10 to 19 more years. Another 21% plan to serve 20 or more years. Eighteen percent have not made plans for how long they will work in spiritual care in a health care setting.
Thirty-five percent say they might leave their current role for growth opportunities. Thirty-four percent would leave for better pay. Twenty-eight percent might leave for personal reasons. One in 5 would leave because of burnout. Sixteen percent would leave for a career change. Eleven percent might leave to move to congregational ministry. Eight percent might leave to advance their education.
Fourteen percent indicate they are financially planned "extremely well" for retirement and 42% say they are "moderately well" prepared for this. Nine percent indicate they are "extremely well" set up for success for retirement because of the benefits and compensation they receive from their current system. Forty-seven percent are "moderately well" set up for success in retirement. Thirty-four percent say they are only "minimally well prepared." One in 10 say they are "not at all prepared."
MANAGERS' PERSPECTIVES
In total, 220 respondents indicated that they have direct oversight of spiritual care personnel or a spiritual care department (34%). The survey asked these individuals additional questions about their perspectives of spiritual care in a health care setting. Three in 10 oversee multiple spiritual care departments.
Managers, who were able to select all categories that applied in their response, reported that their chaplains are most likely to be staffed in acute care (72%) and hospice/palliative care (46%). The next most common areas staffed by chaplains are staff care (44%), cancer centers (40%), mental/behavioral health settings (40%) and outpatient clinics/emergency departments (39%). A smaller percentage of chaplains said they work in long-term care/PACE, the Program of All-Inclusive Care for the Elderly (24%), pediatric (19%), virtual care (15%), community care (12%), physician/clinical offices (6%) and home health (5%).
Forty-five percent of those managing a spiritual care department indicate that spiritual care coverage is provided on-site but not 24/7. Thirty-seven percent indicate spiritual care is provided on-site 24/7. Thirty percent indicate spiritual care is provided off-site or on call 24/7. Five percent say they provide spiritual care virtually 24/7. On average, 57% of chaplains are paid as exempt (salaried) and 43% are nonexempt, including PRN (pro re nata) chaplains (hourly).
Forty-six percent report that their department uses patient satisfaction tools to assess the quality of spiritual care provided. Among the 46% using these tools, the most common reason for this is to utilize The Joint Commission questions for chaplain involvement (50%), followed by utilizing the spiritual care Centers for Medicare & Medicaid Services codes (34%), assessing readmission rates (29%), managing alignment assessment (27%) and acquiring a net promoter score (21%).
Eighty-five percent say their system has a set of standards for spiritual care. Seventy-three percent say their department uses the Association of Professional Chaplains' Standards of Practice for Professional Chaplains.
Sixty-one percent have a clinical pastoral education (CPE) program in their spiritual care department. Among those using a CPE program, 94% say their CPE-certified educator is certified by the Association for Clinical Pastoral Education. Two percent indicated this was done by Clinical Pastoral Education International. Four percent indicated some other type of certification.
Seventy-seven percent of those managing a spiritual care department cite education requirements as at least "somewhat" of a barrier to finding qualified chaplains. This is followed by salary offered (75%), certifications required (73%) and experience required (65%). Lesser concerns are benefits packages offered (55%), compensation from other employers in the area (52%), that a specific religious affiliation is needed (39%), and limited support from religious institutions in the area (24%). Forty-four percent indicated some other characteristic of their location.
Twenty-one percent of spiritual care departments are now utilizing artificial intelligence (AI). Among the 1 in 5 spiritual care departments reporting AI use, the most common types of things done with it are: modifying or creating prayer reflections (52%), documentation (36%), patient referral (20%) and telespiritual care (20%). Sixteen percent use AI for CPE, 9% for aggregation of spiritual care requests/referrals and 7% for ethics.
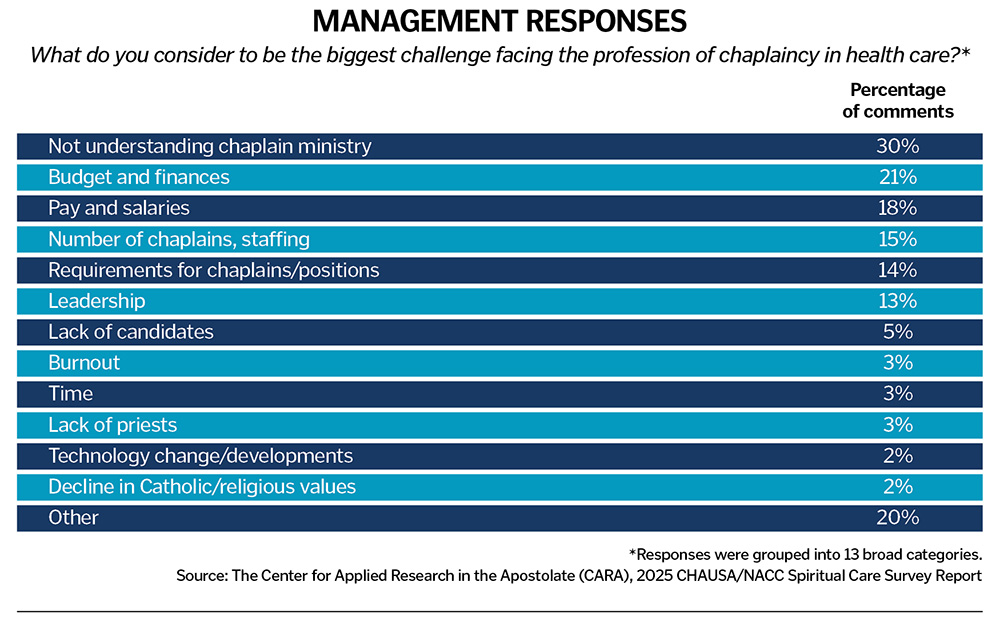
Similar to all respondents, managers were also asked specifically, "What do you consider to be the biggest challenge facing the profession of chaplaincy in health care?" Responses from 185 managers were grouped into 13 broad categories (see table above).
Three in 10 managers identify a lack of understanding chaplain ministry as the biggest challenge facing the profession. Following are selected excerpts from their responses:
- Acceptance by other departments as a critical part of the care team.
- Many still don't fully understand how to engage with spiritual care beyond the traditional perceptions of the role.
- Valuation of spiritual care in the overall well-being of the patient.
Twenty-one percent of managers identify budget and finances as the most significant challenges facing their profession. Following are selected excerpts from their responses:
- Getting funding for good board-certified chaplains.
- Maintaining paid chaplaincy positions as hospitals face severe financial challenges.
- The difficulty in relating spiritual care to financial metrics.
Eighteen percent of managers identify issues related to pay and salaries as the most significant challenges facing their profession. Following are selected excerpts from their responses:
- Chaplains are leaving due to better pay at either state hospitals or in different disciplines.
- No growth opportunities, lower pay, lean staffing.
- Outsourcing chaplaincy to volunteers.
- The imbalance between the education and experience required of chaplains and the remuneration for chaplains.
WHERE DO WE GO FROM HERE?
A deepened commitment to the essential role of spiritual care in Catholic health care remains a key priority for CHA and NACC. To be successful, we must rely on advocacy and support from all levels of ministry leadership to ensure the provision of spiritual care for patients, families and colleagues, and strategic integration of spiritual care with mission and interdisciplinary clinical teams. Together, we must stay faithful to what Catholic teaching instructs and what clinical evidence supports: Effective holistic healing must embrace a person's physical, psychological, social and spiritual dimensions.
In the coming months, CHA and NACC will continue to explore the implications and strategic priorities for spiritual care and spiritual care departments, based on ongoing analysis of survey findings. Interviews with survey respondents who serve as directors of spiritual care are not yet complete; more information is forthcoming.
Additionally, NACC will report further data on the survey's compensation and benefits review of chaplaincy and social work. To serve as a catalyst across the discipline, we will soon more broadly disseminate the current trends and future opportunities revealed by the survey. CHA also plans to publish a white paper this year on its website on the essentiality of spiritual care in the Catholic health ministry.
MARK GRAY is a research associate professor at Georgetown University and the director of CARA Catholic Polls at Georgetown's Center for Applied Research in the Apostolate (CARA). JILL FISK is director, mission services, for the Catholic Health Association, St. Louis. ERICA COHEN MOORE is executive director of the National Association of Catholic Chaplains.
NOTE
- Brian Smith et al., "Spiritual Care Survey Reveals Challenges for Ministry," Health Progress 100, no. 5 (2019): https://www.chausa.org/news-and-publications/publications/health-progress/archives/september-october-2019/mission-and-leadership---spiritual-care-survey-reveals-challenges-for-ministry.
