
Leanna Ross has trained hundreds of health care providers on the other side of the globe in the last two years without leaving her home in Missoula, Montana.

A nurse by training, Ross is a med/surg professional development specialist with the Providence Nursing Institute Clinical Academy of Providence St. Joseph Health. She volunteers with World Telehealth Initiative, a U.S.-based nonprofit that leverages technology to teach clinicians overseas.
"The cross-cultural connection has been heartwarming and bucket-filling for me," she says. "I'm connecting with people in such different parts of the world, but we have so much in common. I love finding that commonality."
At an event in February at Providence St. Patrick Hospital in Missoula, World Telehealth Initiative gave its inaugural Global Health Humanitarian Award to Ross. The organization said it honored "her exceptional volunteer service" and her commitment to going "above and beyond to make a measurable global impact."
Ross said mentoring overseas clinicians is needed "because of health equity. It's important that everyone has an opportunity for quality health care, regardless of where they live on the planet. And for health equity to be realized, we need health education" for providers worldwide.

Global aid cuts worsen situation
Half of the world's population lacks access to essential health care services and each year an estimated 8.6 million people worldwide die of treatable conditions, according to the World Telehealth Initiative. Sharon Allen, the organization's co-founder and CEO, said on a recent CHA networking call that there are gaping disparities in health outcomes worldwide due to myriad, complex factors, including "geography, workforce shortages and limited advanced training" that "leave many (overseas) clinicians without the tools they need to address local health challenges."
She added that "patients in rural and under-resourced regions often face preventable complications simply because specialized expertise is not available."
She noted that while these concerns always have been present in global health, "reductions in global aid have certainly intensified the need." Allen said when global aid funding declines, overseas hospitals often face staffing shortages, reduced training opportunities and limited access to specialty care. The current administration has been dismantling the U.S. Agency for International Development and significantly cutting overseas aid.
Virtual matchmaker
Allen said she and entrepreneur and inventor Yulun Wang founded World Telehealth Initiative because they recognized the power of technology to serve as a virtual matchmaker and connection between clinicians who lack expertise and resources and those who can help bridge that gap. The March networking call that featured Allen, Ross and others was called "Global Solidarity Through Telehealth."
World Telehealth Initiative seeks to help address global health inequities by increasing overseas clinicians' knowledge and ability to treat preventable illness. The organization connects health care providers across the U.S. with overseas clinicians over a telehealth platform. Since World Telehealth Initiative's 2017 founding, more than 1,800 physicians and nurses in the U.S. have volunteered their time to mentor, train, educate — and learn from — thousands of clinicians in 19 countries, most of them in the Global South.
World Telehealth Initiative is funded primarily by philanthropists, charitable foundations, corporate partners and voluntary memberships by the U.S. health systems that participate. In some cases, ministries of health in the countries where World Telehealth Initiative operates provide funding.
The organization works with overseas ministries of health and other partners to identify the health care facilities that are most in need and most able to benefit from telehealth. World Telehealth Initiative representatives meet with leadership at those facilities, explain the offerings and complete a technology review to ensure the facilities have basic infrastructure to support the telehealth technology. Those that sign on with World Telehealth Initiative get Teledoc Health equipment that will be their portal to their overseas mentors.
Cross-continental connections
World Telehealth Initiative has recruited, screened and trained physicians and nurses from across the U.S. to volunteer as mentors. Those providers fill out an electronic form indicating their areas of expertise and specialization. Contacts at the overseas locations request certain training, and then a notice goes to the U.S. providers, who can either accept or pass on each request. When the two parties are matched, they coordinate the date and time of the training and then connect over the virtual platform. U.S. providers also can proactively list the types of sessions they can provide, and their overseas counterparts can take them up on the offer. The two parties also can enter case-by-case consultancy-type relationships.
There is an almost limitless list of types of training, education, consultations, and mentorship opportunities available, but most revolve around about 50 specialties.

About two years ago, Ross saw one of these solicitations and signed on. She has fully embraced the role, conducting training sessions with providers thousands of miles away, primarily in Togo, Kenya and Bhutan. World Telehealth Initiative estimates Ross has trained more than 700 providers.
Providence partnership
Ross has worked at Providence for more than two decades. She began in direct care at St. Patrick, advanced to nurse leadership and education, and then transitioned several years ago to a system-level role supporting and educating new nurses and nurses moving into specialty roles.
Nearly from the time World Telehealth Initiative started, Providence has partnered with the organization. The health system often makes its clinicians aware of telehealth medical volunteerism opportunities with World Telehealth Initiative.
Live from Missoula
Ross has trained on many topics, including wound care, sepsis recognition and response, urinary tract infection prevention, stroke assessment and intervention, ostomy care and prevention of central line-associated blood stream infections.
She devotes several hours a month to medical volunteerism. With permission, she frequently uses the presentations she delivers in her Providence nurse educator role. She presents most of the sessions from her home office in Missoula, using a laptop.
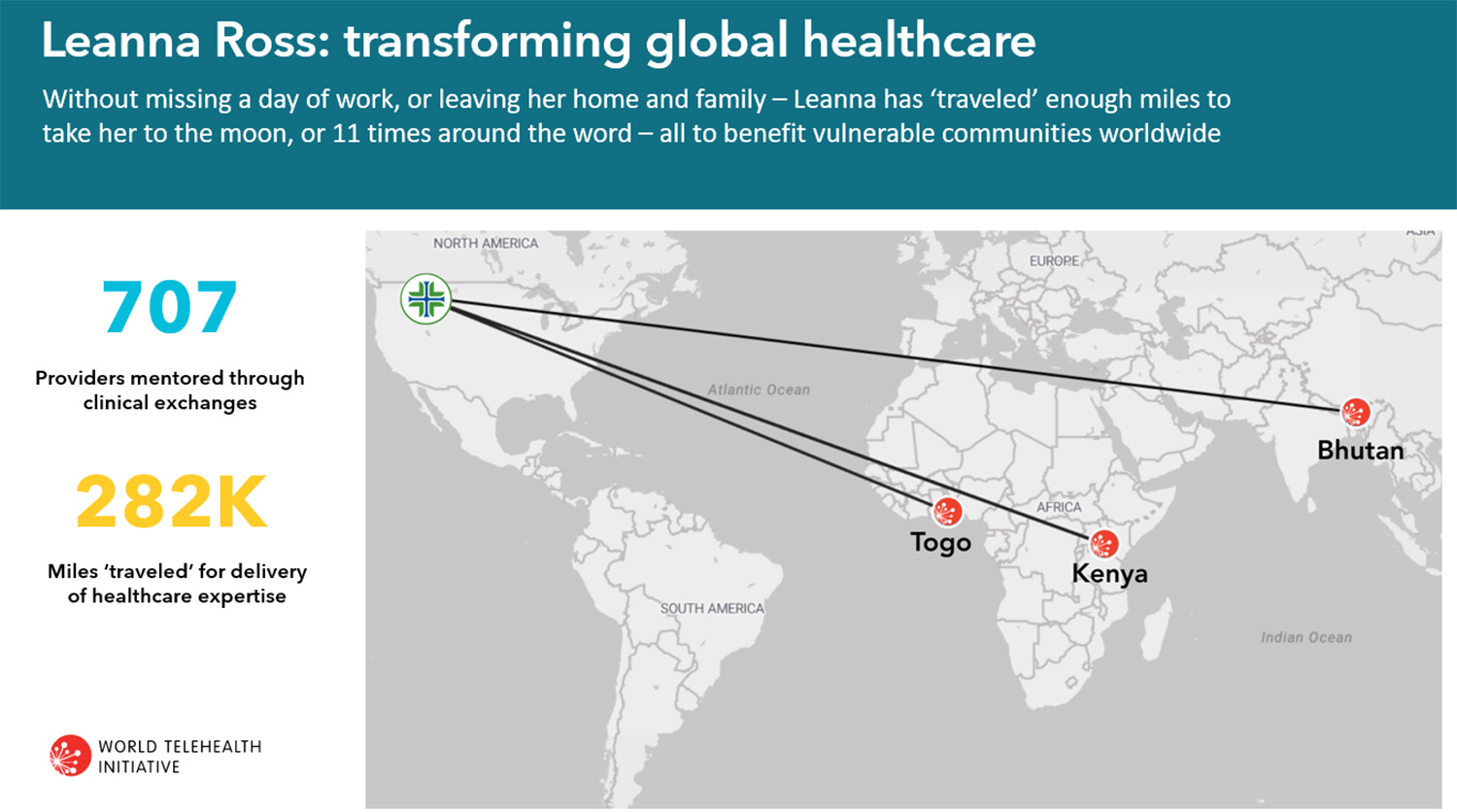
Ross' presentations are live. Most of the learners speak English. Class sizes vary greatly, from less than a dozen to several dozen participants.
Ross often begins with pleasantries and questions to make sure she knows what medical equipment the learners have access to and then starts the lesson. Her presentations involve conversation and back-and-forth questions and answers. She noted that often the learners have a broad knowledge of the topics she's speaking on — she's just providing new best practice information or detailing how to advance or deepen their skills.
Ross said one of the concepts that initially drew her to this medical volunteerism is the "idea of connecting with nurses from around the world." She recalled talking with a site coordinator in Togo at the exact moment they realized one of them was seeing the sun rise, and the other was seeing the sun set. They traded photos in real time of their vantage points.
She noted that she can see that this training is extremely valuable to the learners. Sometimes, they invite their town's mayor or other dignitaries to witness the session. The learning opportunities "empower them," Ross said. "They see this as really important to their community."
