Saint Peter's Healthcare System is using an artificial intelligence tool to better identify patients who need social services — such as transportation and food — and connect them with assistance. As a result, fewer of those patients are showing up in the emergency room with health issues.

The system, based in New Brunswick, New Jersey, reported that the use of the tool led to a 7.1% reduction in emergency department visits by high-risk patients at Saint Peter's University Hospital within a 90-day period. Those patients were identified through the tool, from Lightbeam Health Solutions, which describes itself as an "AI-enabled solutions and services leader in population health management."
The tool helps identify patients with a high risk of having needs related to social determinants of health and lists the top 10 risk factors for the patient, along with the top five recommendations to reduce the patient's risk. The care team at Saint Peter's reviews the risk factors and recommendations with the patients to determine the best way to help.
"While still early in the initiative, Saint Peter's has achieved promising results," says a case study from Lightbeam.
Clinicians and leaders anticipate that the tool will help reduce no-show rates at appointments and help them identify and document risk factors they may have missed before.

Ishani Ved, the system's director of transformational population health and outcomes, pointed out that Middlesex County, where the Saint Peter's University Hospital is located, is one of the most racially diverse counties in the nation. The population is 45.4% white, 30.3% Hispanic/Latino, 12.4% Asian, and 10.5% Black, according to a community health needs assessment. The hospital has more than 21,000 inpatient admissions, more than 260,000 outpatient visits and 67,000 emergency department visits each year.
Determining who to screen
Like many health systems, Saint Peter's vowed to address disparities in health care after those inequities became more apparent during the COVID-19 pandemic. The challenge was deciding which patients to screen for factors in those disparities, such as hunger and lack of housing. "We knew we had to do something," Ved said. She said the team asked themselves, "How do we risk stratify?"
The system had worked with Lightbeam before on projects, and the company came up with a tool that produced a risk score for patients based on known data, such as from the U.S. Census Bureau or the Environmental Protection Agency, with information from patients' medical records, such as their address.
"Your ZIP code is more important than your genetic code," Ved pointed out.
The system wanted to know who, exactly, to question to determine social determinants of health, which are responsible for up to 80% of health outcomes. The AI tool identifies those patients, by assessing factors such as whether or not a patient is more or less likely to have a car so they can get to an appointment, or whether they are more or less likely to have lead paint in their homes that might affect their health.
"We plotted that data so we know where to focus our effort," Ved said. "There's so many different applications of it, and I think the use of AI and population health is going to continue to evolve. But it helps us solve the problem of: Who do we reach out to first? Who do we screen when they're there?"
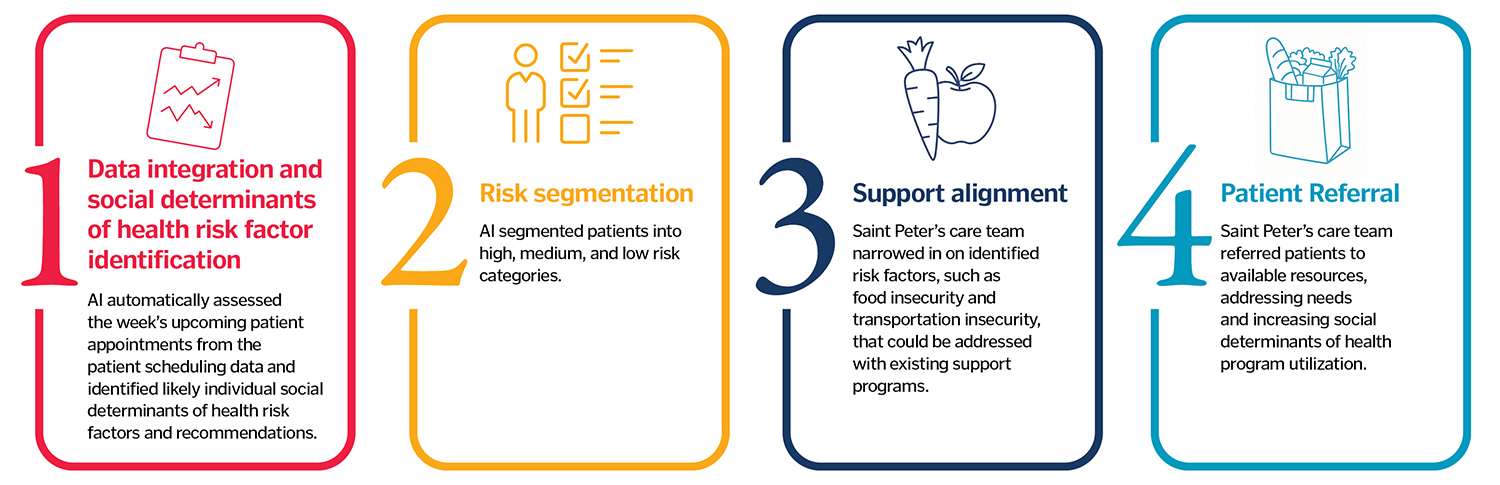
The AI tool reviews the week's upcoming appointments and identifies possible social determinants of health concerns faced by patients. If the tool identifies a patient who likely needs help, clinicians screen them during their appointment. They then refer patients who are in need of support to various resources, including services that Saint Peter's has expanded recently.
Meeting patient needs
Among the patients Saint Peter's is screening are those admitted to the hospital and those who go to Saint Peter's Family Health Center, which served children and adults during nearly 84,000 patient visits in 2025, an increase from 60,000 visits in 2023. In March 2024, the center completed a major renovation and expansion. Some of those renovations included more services to help those with risk factors based on social determinants of health.
In addition to primary and preventive health care, other offerings at the center include:
- The For KEEPS (Kids Embraced and Empowered through Psychological Services) program, a short-term acute partial hospitalization unit that offers mental health diagnoses and intensive treatment for children with emotional and behavioral issues.
- The Dorothy B. Hersh Child Protection Center, a multidisciplinary team of health care workers who offer help, such as crisis intervention, child abuse assessments and referrals, for children and families affected by child abuse and neglect.
- The Market at St. Peter's, a food pantry open to the center's eligible patients by appointment during weekdays. It features fresh produce, canned food, packaged goods, and baby care and personal hygiene items. The market includes a walk-in refrigerator and freezer and a demonstration kitchen that allows workers to teach patients different ways to prepare food. When it opened in spring 2024, the pantry served about 20 families each month, and now it serves around 50.
- A van that the center acquired at the end of 2025 and uses as a mobile food pantry. "It's beautiful, and will allow us to take the food pantry on the road," Ved said.

Ved said the idea is for individuals and families to become self-sufficient. "We don't want people to always rely on us. We want to give them the resources that they need to get out of a tough time," she said. "So that's where the whole team comes together."
She explained that a nutritionist with the food market will help patients make healthy choices, and social drivers of health coordinators will help people find affordable housing or a job, sometimes within the health system.
The key to Saint Peter's work in screening and identifying patients who need help is following through, Ved said, and that also includes building and maintaining relationships with outside agencies to update contacts and resources. "We can give you a number all you want, but if you're never able to get in touch with somebody on the other line, what good is that?" she said. "Intentionality is huge."
Ved, who practices Hinduism and Buddhism, says she is fascinated by the Catholic faith and takes one line of the Lord's Prayer to heart: Give us this day our daily bread.
People should have faith that God will provide, and the health system is, sometimes literally, the vehicle to get the daily bread to patients, she said. "That's the heart of the Gospel. That's what we're supposed to do: Help your neighbor."
