BY: JOE RANDOLPH
Few would deny the need for transformative change in U.S. health care across any spectrum — political, socioeconomic or otherwise. Declining reimbursements, rising costs, changing demographics and the sweeping effects of the Affordable Care Act all are realities driving health systems to seek new solutions for care and new revenue sources.
Increasingly, health care providers realize that incremental change and cost reductions are insufficient to make up the shortfall. Constraints and burdens on the current delivery model of health care are now so manifest, many industry leaders surmise that non-patient revenues will need to surpass patient revenues in coming decades as health systems look for new operating models and new revenue sources.
In an effort to get in front of this curve, many health systems are looking to the world of innovation as a potential lifeline for their future. The attractive promise of innovation offers solutions unburdened by the baggage of old processes and products. Speak with any leader in health care about the possibility of unlocked creativity leading to transformative care for his or her community, and you will find a willing ear. Yet, hospitals and health systems that seek to implement innovation initiatives are surprised when they face systemic organizational biases.
U.S. health care strongly rewards risk-averse organizations. A quick scan of health care providers' mission statements will find a core message centered on the improvement of and care for human life. Given that the protection of the people they serve is paramount, we should not be surprised when hospital cultures adopt blanket practices geared to avoid any risk, despite the costs. Who would not be dismayed to find his or her local hospital unconcerned about risky surgical practices? However, this very aversion to risk-taking — even intelligent risk-taking — is precisely what makes health care organizations so ill-suited to pursue innovation effectively.
LIMITED IMPROVEMENTS
Predisposed against the pursuit of any disruptive innovation, health care providers then look to the next logical source of solutions — standardization and the elimination of waste. "Lean" and "Six-Sigma" management programs often are used to standardize processes and reduce errors, thereby driving incremental change within the organization. These sorts of "inside the box" improvements can bring some good, and it is understandable that hospitals operate from this mindset and focus, because smaller changes seem more achievable.
However, process improvement remains fundamentally limited. For example, a local "Lean" improvement team might reduce the turnover time for an operating room, but they will never be able to identify, develop and commercialize a new medical device that will prevent or cure the medical condition that brought the patient into surgery in the first place. Waste elimination is not innovation, and it cannot provide the sort of widespread transformation that so much of health care needs.
Operating margins and short-term financial focuses present another substantial obstacle holding back innovation in health systems. Neither a thin operating margin nor three-year budget cycles allow organizations to focus on the long-term solutions. Instead, carving out dollars from the budget cycle for research and development of new ideas begins to be seen as a drain on the organization, especially since there is little to no return on investment within the short time being addressed. Innovation requires the relative expectations of the marathon runner, not the sprinter. Successful ideas almost universally have an incubation time of four to seven years from concept to usable completion — a maturation period that far exceeds the organizational patience of most health care providers.
Adding to this negative perception are the structural realities that come with large, complex organizations. Internal leadership teams, divided into diverse departmental structures, often seem to be competing for pieces of the same budget pie. Innovation spending can quickly become viewed by department leadership as detracting from their own effectiveness and as an easy target for financial cuts.
For innovation to thrive, you need to embrace failure. Thomas Edison famously said, "I have not failed … I've just found 10,000 ways that won't work." This attitude of the consummate innovator has influenced the world of business and technology since at least the beginning of the Industrial Revolution, and it is time to incorporate that same spirit into the culture of health care.
However, industrial innovation is not medical innovation. Health care needs an innovation model that better fits its unique mission to be a force for good in the world. An ethical model for health care improvement should be a collaborative one, bringing multiple health systems together to focus on the common good outside their day-to-day operations. We need a model where a wider community learns from intelligent, local failures and where the lessons learned from failures can be shared opportunities for all.
FINDING THE RIGHT MODEL
When I began my efforts to lead the launch of an innovation vehicle in 2013 for St. Joseph Health, a Catholic system based in Orange, California, I was not a newcomer to the realities of health care. I had 30 years in leadership behind me, including serving in both the CFO and COO capacities with nonprofit health systems. I was aware of many of the roadblocks facing us, as well as the existential need for growth and innovation.
Similar to other health systems across the country, St. Joseph Health was looking at major cost reduction initiatives. I realized that incremental change and cost reduction was not going to be enough to achieve the type of transformational change needed by the health care delivery system. I began to look at innovation as a potential solution and studied the different models in the market to determine the best approach.
The search for best practices within innovation across the country took us from nonprofit health care to for-profit health care to investment vehicles and to the tech sector. When we looked into the efforts of health care vehicles for innovation, we found a mixed bag — generally, however, innovation initiatives either were set up as a department or division within a health system, or they were set up as a stand-alone organization to function as an accelerator.
The initiatives that operated more like an R&D department than as an incubator or accelerator tended to prove inherently self-limiting in their thinking. As part of large, bureaucratic organizations, they would invariably get bogged down in annual budget cycles, politics and operations. There is a great deal of research that suggests incubators need to be independent in order to be successful.
We found from our research that a high proportion of stand-alone incubators failed in the first three years of operation. The cycle became a familiar story: The incubator would receive initial funding; it would invest in the most promising ideas/technologies; and then it would wait for the royalties from the promising ideas to generate enough cash flow to sustain itself. Since it takes four or more years for that to occur, it would return to its investors in about Year Three and ask for more funding. It was at this point that many of them failed.
Slowly, an evidence-based picture began to form of the kind of value-based organization we would need in order for innovation to thrive and be successful. Our new model would build on the available strengths in health care and shore up the weaknesses. This would become a collaborative, independent, self-sustaining endeavor, built to tap into physicians, clinicians, employees and industry partners to advance innovation.
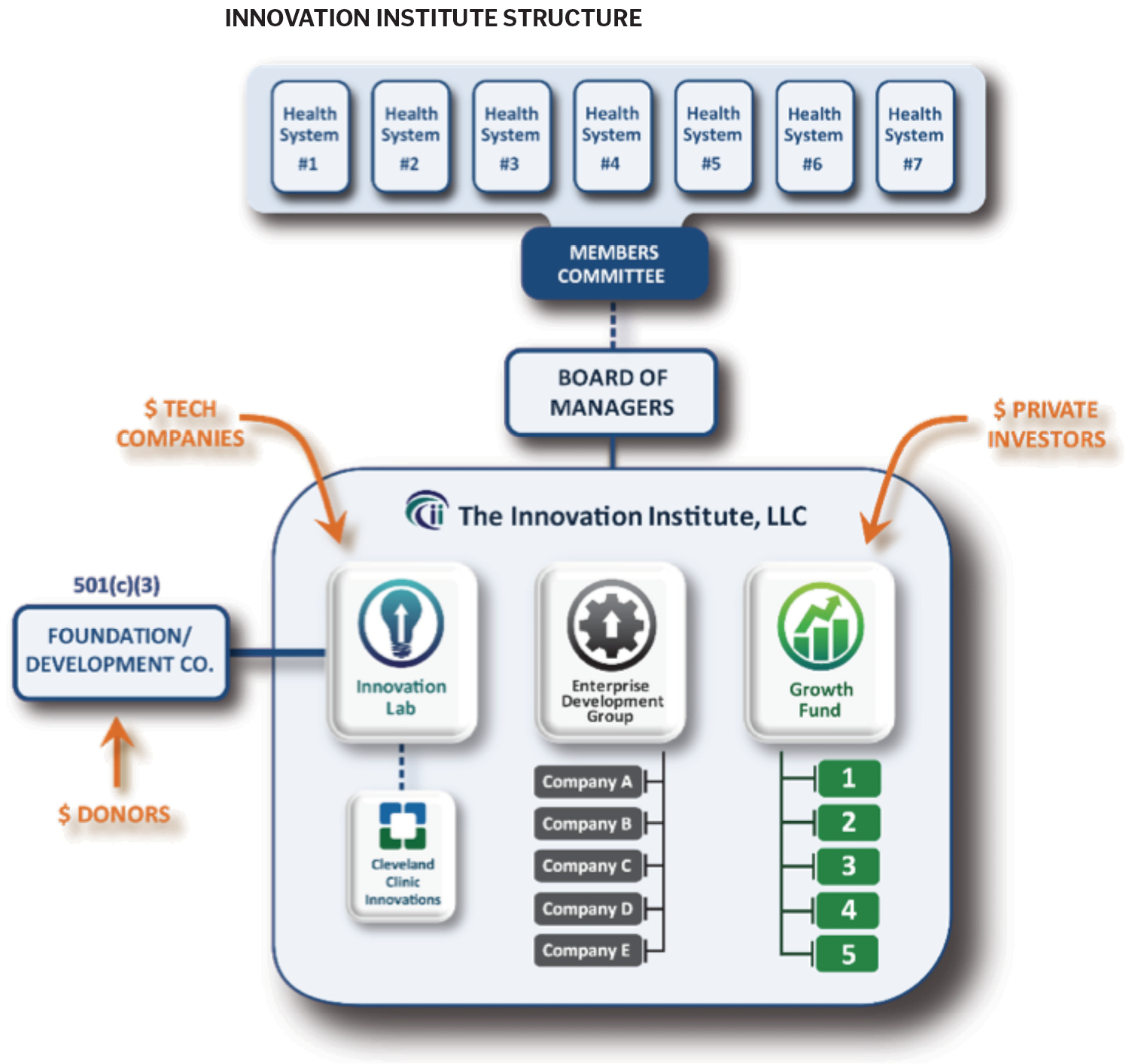
The best vehicle for innovation — our Innovation Institute — would need the following structural characteristics:
Independence: The ability to take risk, to "fail forward" and innovate, was critical. Our vehicle could not be part of the risk-averse cultures of typical health systems and subject to the vagaries of politics and short-term budget cycles.
Financial Viability: As an independent incubator/accelerator, our ability to be profitable almost immediately would also prove core to our success — we needed an economic engine. The model envisioned would hold multiple portfolio companies, all providing services within health care. Health systems outsource services all the time, and each time they do, they give margin to someone else. Our model captured this and reinvested it back into innovation.
Collaboration: Our intent was to break the cycle of internal blinders and bring people together to collaborate on innovation. The more minds you have working on a solution, the better ideas you are going to develop, so our model was designed to ultimately have seven health systems as member owners. There is an African proverb, "If you want to go fast, go alone; if you want to go far, go together."
Industry Partnerships: Health care has much to gain from partnerships with industry, especially in the technology sector. A diverse spread of partnerships that contributed to the innovation we sought, from the medical industry, finance and technology, would be instrumental in supporting the model we envisioned. These partners also could function as first adopters of appropriate innovations within their sectors, more rapidly increasing the impact of our work. This would likewise be consistent with our design as a collaborative, bringing people together to find solutions to problems we all face.
"Perpetual" Company: The company would need to be set up as a for-profit, limited liability company (LLC), for reasons of capital structure. Unlike the practices in other industries, however, we held no plan for an end date or a liquidity event — no sale, merger or initial public offering for our organization. Our intent was to work with nonprofit health systems for the long haul, where the need for innovation and growth was great. Therefore, the model required an LLC that would operate into perpetuity with no planned or "big payday" exit strategy.
Balanced Approach: Although it is important to provide a return on investment, the company also needs to focus on addressing issues that will have a positive impact on the community. There may be innovation investment opportunities that could have a significant benefit to the community and the underserved but may not hit a financial hurdle rate, that is, the rate of return needed for a project to get the go-ahead. There needs to be a balanced approach, where both ROI and the community's needs are addressed.
Incorporating the above elements into a single structure, The Innovation Institute was fully operational in 2013, existing in the structure illustrated on page 68. With a strong business plan structured to promote and embrace breakthroughs with vigor and resilience, we have experienced real success in our first two years. We are excited about what we're doing and confident that we have created a place that will allow health systems to flourish.
LESSONS LEARNED
Launching a healthy vehicle for innovation was not without its lessons. Located in California's Orange County, we quickly discovered the benefits that partnership with an experienced medical accelerator in another geographic region could bring. For our company, strategic partnership with the Cleveland Clinic in Ohio has increased our national reach and impact, and it reinforces the principle of collaboration threaded through our founding ideals.
Our growth is happening more quickly now that we have developed our infrastructure. Our first two years were focused on building out our physical lab, acquiring portfolio companies, and developing our innovation and idea submission software. The importance of having a plan of controlled growth is now apparent, so that we can follow through on our commitment to each of the health systems that invest in us. If growth is too rapid, infrastructure may be insufficient to keep up with the number of ideas coming in.
Place is a powerful tool in the utility belt of innovation. The right physical location can serve to bring people together and be the base for programs that enable them to transform care. Here, the inventor can be inspired, hone ideas and build connectivity with consumers and health care professionals and have the resources necessary to achieve commercial success. In our particular case, the Innovation Lab also provides a display space for innovations and successes and gives its investors and industry partners a meeting space for both small and large group innovation.
Perhaps the best advice for those passionate about bringing the capacity for innovation and growth to their hospitals and health systems is, never give up. The challenges are great in bringing needed transformation to health care, but such has ever been the case with truly disruptive change. Those we serve in our communities deserve our most focused efforts. In short, the time is right to infuse our ancient medical culture of "do no harm" with a healthy, modern dose of "fail forward."
JOE RANDOLPH is president and CEO of The Innovation Institute, La Palma, California, which is structured to cultivate solutions to transform health care delivery. He previously served as executive vice president and COO for the St. Joseph Health system in Orange, California.
