Facilities Grapple With Five Broad Issues, Including Changes in Leadership And AIDS
Ms. Westhoff is regional vice president for aging services, Sisters of Mercy Health Corporation, West Des Moines, IA; and Dr. Schaefer is a research assistant, Catholic Health Association, and a graduate student in health administration, Washington University, St. Louis.
Summary
The Catholic Health Association's 1992 survey of Catholic long-term care (LTC) facilities identified five broad issues LTC facilities face in the 1990s: leadership, system affiliation, community programs, resident issues, and care of persons with AIDS.
The transition to lay leadership presents new challenges to the relationship between LTC facilities and their sponsors. Despite the dominance of religious sponsors, an increasing number of laypersons are serving as healthcare administrators both in long-term and acute care.
Thirty percent of respondents reported being affiliated with a multi-institutional system. This percentage has changed little in the past few years, although the number of facilities that are system members continues to increase at the fastest rate of any type of LTC facility.
Only 27 percent of survey respondents said they provide educational or informational programs for persons in their communities. Thirty-nine percent of system-affiliated LTC facilities reported offering such programs.
One encouraging finding shows that 80 percent of facilities have written policies for living wills, 64 percent for designated proxy, and 86 percent for durable power of attorney for healthcare.
LTC providers are struggling to determine their role in caring for persons with HIV and AIDS. Only 3.6 percent of respondents care for residents with AIDS. A major problem LTC administrators face is a fear of potential infection of staff or residents.
To identify key issues Catholic long-term care (LTC) facilities face in the 1990s, the Catholic Health Association (CHA) asked them how they are keeping up with changes in sponsorship and leadership that affect Catholic healthcare organizations specifically and the United States healthcare system in general. Respondents identified issues of importance in five broad categories: leadership, system affiliation, community programs, resident issues, and care of persons with AIDS.
Survey Methodology
CHA surveyed 517 freestanding Catholic long-term care facilities (232 of which were CHA members) in April 1992. Of the 353 surveys returned (a 68 percent response rate), 337 were usable. Nearly half the facilities were located in the East North Central and Mid-Atlantic regions. A few were in the Pacific and Mountain regions. About 80 percent were in urban areas.
Changes in Leadership
The transition to lay leadership presents new challenges to the relationships between LTC facilities and their sponsors. For example, it may be difficult to maintain the organization's mission when the chief administrator is not a member of the sponsoring religious institute and may thus have a different focus and less contact with the sponsoring organization.
Religious institutes of women continue to dominate sponsorship of Catholic LTC facilities. Nearly 70 percent of the facilities reported religious institute sponsorship, 25 percent are sponsored by dioceses, 2.7 percent are private associations of the Christian faithful, and 1.2 percent are private juridic persons. Fewer than 7 percent of survey respondents said they expect changes in sponsorship or cosponsorship in the next three years.
Despite the dominance of religious sponsors, an increasing number of laypersons are serving as healthcare administrators in long-term and in acute care. Women and men religious accounted for about 43 percent of the total number of administrators responding (see Figure)—a 25 percent decrease since 1988 (see 1988 Annual Long-Term Care/Continuing Care Survey, CHA, St. Louis).
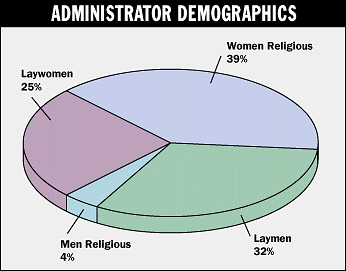
Of the laypersons serving in the administrative role, 32 percent are men and 25 percent are women. Women hold a higher percentage of administrative positions in LTC than they do in acute care, where chief executive officers are 76 percent laymen, 5 percent laywomen, and 19 percent men and women religious.
Because fewer than half the facilities contacted had women or men religious as administrators, a question about the expectation of leadership transition from religious to laypersons was often inapplicable. Of the facilities at which women or men religious were still administrators, 14 percent expected a change to lay leadership in the next three years. However, we question whether this small number accurately reflects reality. In any event, the trend of leadership passing from religious to lay will continue.
System Affiliation
Thirty percent of the respondents reported being affiliated with a multi-institutional system (see Figure). This percentage has changed little in the past few years, although the number of facilities that are system members continues to increase at the fastest rate of any type of LTC facility. Most religious institutes that sponsor only LTC facilities typically govern one or two independent facilities.

The extent to which Catholic LTC facilities are affiliated with systems differs considerably from Catholic acute care facilities. Approximately 74 percent of Catholic hospitals are system members. Although total profit margins for system-affiliated hospitals are slightly higher than for nonsystem hospitals, the difference is not statistically significant (CHA, A Profile of the Catholic Healthcare Ministry, 1992). However, a significantly higher proportion of financially sound hospitals belong to systems. Perhaps the financial benefits of system membership do not apply to LTC facilities and thus they are less likely to be affiliated with systems.
Community Programs
Few Catholic LTC facilities have developed educational or informational programs for persons in their communities. Only 27 percent of survey respondents said they provide programs to community members who live outside the facility (see "Community Programs" below). Continuing care retirement communities appeared to do slightly more programing in this area, perhaps as an outgrowth of their more diverse institutional programing. Systems may encourage their members to develop community programs: Thirty-nine percent of system-affiliated LTC facilities reported offering educational and informational programs to their communities, whereas only 21 percent of facilities not affiliated with systems did so.
Among those facilities offering community programs, volunteer programs (e.g., residents reading to preschool children) and family-resident counseling were the most frequently cited services. Nearly half the facilities offered adult day care, respite care, or both.
Five of the facilities indicated they offer care management services to their communities. One facility, the Bon Secours Hospital/Villa Maria Nursing Center, has instituted a program to call and visit residents after they are discharged to their homes (see "A Postdischarge Follow-Up Program" at the end of this article).
Resident Issues
More than 80 percent of the facilities either had an in-house ethics committee or consulted with an outside committee or ethicist (see "Resident Issues" below). Similarly, 85 percent had a written policy for dealing with elder abuse. Nearly all of them (97 percent) also had a code of residents' rights as mandated by the Omnibus Budget Reconciliation Act of 1987.
Eighty percent of survey respondents reported having written policies for living wills, 64 percent for designated proxy, and 86 percent for durable power of attorney for healthcare. This is encouraging and could have occurred in response to the Patient Self-Determination Act (PSDA), which became effective December 1, 1991. The PSDA requires facilities that participate in Medicare or Medicaid to inform adult residents of their right to accept or refuse medical treatment. The PSDA also requires facilities to inform residents of their right to prepare an advance directive for use should they become incapable of expressing their wishes regarding healthcare.
One survey finding shows that independent housing facilities—which are defined as facilities where residents care for their own personal needs and receive only usual tenant services such as maintenance and security—consistently lag behind other types of LTC facilities in addressing ethical issues. For instance, although they are not immune to cases of elder abuse, only 54 percent of the responding independent housing facilities reported having a written procedure regarding the matter.
Care of Persons with AIDS
LTC providers are struggling to determine their role in caring for persons with HIV infection and AIDS. The decision whether to assign residents with AIDS to designated units or to integrate them into the general population often distracts attention from the critical issue of establishing a range of options for the care of persons with AIDS.
As the AIDS epidemic progresses, the survival times from the point of diagnosis are steadily increasing. Current estimates show median survival times of 15 to 16 months (Alma L. Koch, "Long-Term Care for People with HIV/AIDS: Challenges and Opportunities," Journal of Health Administration, Winter 1992, pp. 115-137). And some experts believe 10 percent to 25 percent of persons with AIDS could benefit from care provided in a skilled nursing facility (SNF) (A. E. Benjamin, "Perspectives on a Continuum of Care for Persons with HIV Illness," Medical Care Review, Winter 1989, pp. 411-433). Some persons with AIDS recently discharged from hospitals, those near death, and those with serious AIDS-related dementia could appropriately utilize SNFs.
Despite this need, only 3.6 percent of facilities responding to the CHA survey care for residents with AIDS. We did not attempt to assess why this number is so small. However, a major problem LTC administrators face is a fear of potential infection of staff or residents. And many states' laws do not permit LTC facilities to accept residents with infectious diseases.
Sixty-five percent of the respondents said they expected to serve residents with AIDS within the next three years. Forty-one percent indicated they had written policies concerning HIV-infected residents, and 37 percent said they had written policies regarding HIV-positive employees.
Healthcare experts predict a shortage of LTC beds to meet future needs. The CHA survey results suggest that the majority of Catholic LTC facilities are not fully prepared to offer chronic AIDS care at a time when the need is dramatically increasing.
LTC facilities can play many roles in addressing the AIDS epidemic. These roles include providing nursing care to persons with AIDS and educating staff, residents, and families about HIV and AIDS to eliminate misconceptions that lead to intolerance. Staff must master proper infection control techniques. In addition, LTC facilities must develop policies that effectively address issues related to HIV-infected employees.
CHA's LTC members must adopt a proactive stance and take a leading role on this issue. Will residential facilities be reserved only for care of the elderly in the future? Will they be prepared to care for elderly residents with AIDS?
The survey also disclosed a lack of inpatient hospice in general. Only 10 percent of the facilities offered this type of care. Those which did often reclassified a regular nursing care bed on a per diem basis. The lack of hospice will also hamper LTC facilities' ability to care for persons with AIDS, since hospice is one of the best methods of caring for persons with AIDS when death is imminent.
Hospice care in this case, however, differs from the approach used for other terminal illnesses because people with AIDS are often treated for opportunistic infections until death. Many providers believe that any antimicrobial therapy directed against the opportunistic infections characteristic of AIDS is incompatible with hospice philosophy of providing palliative treatment only. This is another challenge some organizations face. Because of the significant need for AIDS beds, some organizations may find it beneficial to alter their philosophy of care.
Questions for Further Study
All levels of long-term care form an integral segment of the continuum of care that would be provided by integrated delivery networks (IDNs). These networks will offer comprehensive benefits and coordinate the delivery of healthcare services in specific geographic markets. IDNs' underlying concept is that all services are coordinated and focused with the aim of providing high-quality service to the patient. To prepare for involvement within an IDN, long-term care facilities would benefit from including a community service orientation in their programs.
The survey of freestanding LTC facilities identified certain issues and raised a number of questions that will require further investigation by CHA. The issues include leadership development for LTC administrators, management resources to evaluate how and why new programs are developed, and the role of LTC facilities in meeting the needs of persons with AIDS.
Questions for further study include:
- What policies do independent housing facilities need to address ethical issues as residents age in place?
- What types of programs will increase in LTC facilities? Will they focus on institutional programs (for residents only), or will they focus on programs for the community (e.g., adult day care)?
- How prepared are LTC facilities to participate in integrated delivery networks?
Photocopies of the 1992 Long Term Care Survey are available by calling Mary Luedloff in CHA's Division of Member Services, 314-253-3416.
COMMUNITY PROGRAMS
| Facility Type | Percentage Offering Community Programs |
| All respondents | 27% |
| Nursing facility | 27 |
| Continuing care retirement community | 32 |
| Independent housing | 15 |
| Other facility | 25 |
| System member | 39 |
| Nonsystem member | 21 |
RESIDENT ISSUES
| Program or Policy | Percentage of Facilities Offering |
| Ethics committee | 87% |
| Elder abuse policy | 85 |
| Code of residents' rights | 97 |
| Living wills | 80 |
| Designated proxy | 64 |
| Durable power of attorney for healthcare | 86 |
A Postdischarge Follow-up Program
Improving the health of residents once they have returned home after a stay in a nursing home is the goal of the Nurse Managed Family Follow-up program at Bon Secours Hospital/Villa Maria Nursing Center, North Miami, FL. The facility and the University of Miami School of Nursing have joined forces to train nurses to make follow-up telephone calls and visits to residents after they are discharged to their homes. The program was made possible through a three-year, $512,000 research grant from the U.S. Department of Health and Human Services' Division of Nursing.
"The program focuses on discharge planning to reduce re-entry into institutional care," explains Lois Blume, director of community services at Bon Secours/Villa Maria. Initial plans call for assigning a nurse to each resident participating in the program. The nurse oversees the individual's progress through four contacts: a phone call on the day of discharge, two home visits during the next four weeks, and another visit about three months after discharge.
All 28 nurses at Bon Secours/Villa Maria will be involved in the program during the next three years. Villa Maria has provided the space and funding to enable nurses to attend training sessions and make home visits. In addition to formal training, clinical coordinators accompany nurses on their initial home visits to provide on-site clinical training.
Nurses will take on many new responsibilities as the program progresses. In addition to monitoring former residents' progress, nurses will learn advocacy skills. For instance, a nurse may assist with the administration of a person's home health entitlement. Procedures are currently being evaluated to allow nurses to facilitate the transition from the institution's physician back to the resident's primary care physician.
When possible, nurses will instruct family members on patient care techniques, such as how to change a dressing. According to Blume, this is an important departure from the old practice of asking family members to leave the room when procedures were being performed. The goal is to restore the former residents' independence.
Nurses at Bon Secours/Villa Maria have reacted positively to the challenges the program has introduced. They were consulted before the Nurse Managed Family Follow-up program was put into place. The nurses indicated they had been getting a lot of calls from former residents long after discharge, so the program is filling a need.
The social work department at Bon Secours/Villa Maria also supports the program. Nurses had always been involved with social workers in discharge planning, although not as significantly as they are now. Rather than viewing the program as an "encroachment" on their service, the social workers feel they will now have more time to focus on persons' financial and community service needs. With the nurses visiting persons at home, social workers can now learn how their discharge plans are working and make adjustments as necessary.
Although the Nurse Managed Family Follow-up program is not the first of its kind, a couple of things make it unique. Blume believes this is the first such program to be introduced in an LTC facility. In addition, it is rare to assign one nurse to the resident throughout the entire program as does Villa Maria. And home visits are usually not the responsibility of the in-house nursing staff, as they are at Villa Maria.
