By LISA EISENHAUER
As COVID-19 was sweeping across the nation, Livonia Mayor Maureen Brosnan and the community's other leaders were unaware that the suburban Detroit city was getting slammed especially hard by the pandemic.
"We kind of thought that everybody else around us was dealing with the same dynamic that we were," recalled Brosnan.

Brosnan
What the city was dealing with was a patient load so heavy that St. Mary Mercy Livonia, the only hospital in the city, had nearly doubled the size of its 16-bed intensive care unit by early April to meet demand and added a "comfort care unit" for the dozens of patients dying from the virus.
When comparative numbers started coming in from the state a few weeks into the pandemic, Brosnan and others learned that the COVID case and death rates for Livonia were above those of any Michigan city except Detroit. At its peak, the death rate for people who contracted the virus in the city of 96,000 reached 18%, higher at the time than that of New York City.
Eye of the storm
The virus might have been even more devastating if not for the joint efforts of city officials and leaders of St. Mary Mercy, where Brosnan chairs the board of directors. The hospital is part of the Saint Joseph Mercy Health System, a subsidiary of Trinity Health.

Fire and police departments from Livonia and across southeast Michigan turn out in force April 16 to thank St. Mary Mercy Livonia staff caring for patients during a surge of COVID-19.
Working together, city and hospital leaders were able to find local companies to make personal protective gear for health care workers. As COVID spread rapidly in the city's long-term care facilities, St. Mary Mercy set up a task force to mitigate damage and invited participation from the city. The hospital consulted on setting up quarantine units at long-term care facilities for residents who contracted COVID and additional steps to protect other residents from contagion. The hospital and city worked together to identify potential sites for COVID wards outside the hospital. Fortunately, the broadside the city had taken from the pandemic eased by mid-May and the plans for those extra care spaces could be put on hold.
Nevertheless, Brosnan said: "We by no means consider ourselves out of crisis management mode."
The same is true for St. Mary Mercy, said Dr. Matt Griffin, the hospital's chief of medicine.
"We kind of feel that we're at a stable point," he said. "We're certainly not done with this and none of us anticipate that we'll be done any time very soon."
The hospital's tally of infected patients has been, however, trending downward. On its worst day, April 7, the hospital was treating 152 patients with COVID and diverting others to the five other southeastern Michigan hospitals in the Saint Joseph Mercy Health System.
Bracing for the blow
Before the pandemic hit Livonia, Griffin said he and the hospital's other leaders had had about a week to brace themselves as they watched the virus inundate Seattle and then New York. "Pretty quickly, in the first couple of days, we were convinced that we were going to face a very similar crisis due to our patient population," he said.
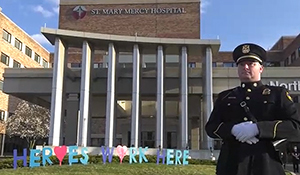
A police officer stands outside St. Mary Mercy Livonia as several police and fire departments take part in an event to honor health care workers caring for COVID patients.
Livonia's population has a high rate of comorbid conditions such as diabetes, hypertension, obesity and pulmonary disease and many residents are elderly, making them especially susceptible to a poor outcome from COVID.
Within three days of seeing its first patients with the infection, the hospital set up a screening site outside of its emergency department. Few of the people who came through were actually tested because of restrictions on who was eligible for testing; and, for those who were, the results took days to get. The screening staff nevertheless was able to identify those who might be infected, get patients in the direst conditions into hospital care and educate those who had signs of the infection on how to self-quarantine.

Griffin
Griffin said that outdoor screening site was one of several ideas pitched by staff and adopted by St. Mary Mercy's leaders that proved key in getting the hospital through its worst days of the pandemic. Another was to turn an area that had once housed the emergency department but was more recently being used for storage into a second ICU. At staff suggestion, the hospital repurposed what had been a ward for patients with chemical dependencies into a hospice care unit for patients with COVID, who themselves or whose families opted against aggressive medical intervention.
"Sad as it is that we needed it, I think one of our biggest successes during this event was our comfort care unit," Griffin said, referring to the unit for end-of-life care.
The unit's team of specialists — physicians, nurses and support staff — cared for more than 100 patients over the period of four to six weeks, providing them a peaceful end to their lives, Griffin said.
Community pitches in
As St. Mary Mercy was in the throes of the patient surge from the pandemic, concerns about supplies arose. Shortages of medical necessities were being reported across the globe and even Trinity Health's well-connected and reliable supply chain couldn't meet the need for goods like respirator masks and surgical gowns.

Spivey
Griffin said St. Mary Mercy's leaders paid close attention to ensure that protective gear was being conserved without violating federal guidelines; there was no easy way to replenish supplies.
That's one of the ways the collaboration with the city paid off. With the hospital providing prototypes, city officials were able to tap local companies to produce scarce items for the hospitals and long-term care facilities. Two firms made plastic face shields and others made gowns and surgical masks.
"The community really provided support through the manufacturing sector," hospital President David Spivey recalled.
Better together
St. Mary Mercy in turn shared its expertise with the community, including by offering advice from its infectious disease experts to help the 15 long-term care centers in Livonia contain the infection. The expertise was used to figure out burn rates on protective supplies and how best to set up quarantine units to keep patients with COVID away from those who weren't infected.
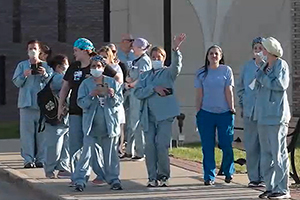
St. Mary Mercy Livonia staff react to a tribute to their heroism from first responders. Police and fire department vehicles ringed the hospital to show support.
First responders from Livonia and other localities in southeast Michigan turned out in force April 16 to honor and thank the frontline caregivers at St. Mary Mercy. The city's video of the tribute, which included prayers for the first responders and families impacted by COVID, can be viewed here.
Brosnan called her connection with the city and the hospital, one of Livonia's top five employers, "an ideal arrangement" because she was able to merge their expertise and resources. She has served on either the hospital's or St. Joseph Mercy's board for 19 years. She said she finds personal fulfillment in the spirituality-based mission of Catholic hospitals.
"The big part of how, as a leader, I was able to get through, and continue to get through, this crisis is having that background and having that foundation," she said. "And knowing that I had a Catholic hospital in my backyard to help me do it."
Three leaders of St. Mary Mercy Livonia hospital in Michigan share some thoughts on things they have learned during the pandemic.
Dr. Matt Griffin, chief of medicine at St. Mary Mercy Livonia
This has been a good example of a very broad and pervasive event that is going to force a change in our thinking on how we prepare for these kinds of things. We really have to expand our preparedness work in the sense of seeing way farther than what we would image or expect.
It was amazing the ideas that our teams were coming up with for how we were going to get done what we needed to get done. I think that's a good model for every day, for when things are normal, making sure that we're highlighting that perspective or that approach.
Maureen Brosnan, Livonia mayor and chair of the St. Mary Mercy Livonia board
The first set of resources that we really needed to get our arms around was our supply chain. And we did. The city quickly set up a donation center and contacted area businesses through a partnership with the Chamber of Commerce and Livonia Community Foundation to secure PPE, financial contributions, and commitments to produce PPE.
Second is people, in terms of the strength of your team. Understand that the hat they're wearing today isn't necessarily the hat they're going to be wearing tomorrow, and that they're capable of doing more with their skill set. One day the director of planning and economic development is talking with retail site selection teams and the next he's knocking on the doors of the 15 long-term care facilities offering to get them the resources they need to manage a growing crisis in their facilities.
Third is that we do have an immense amount of talent and skill and knowledge right here at the hospital. St. Mary Mercy established a long-term care facility task force that met weekly on a conference call. They invited a city team to participate to quickly understand why the virus was spreading so quickly through long-term care sites in our city and how we could mitigate the damage by sharing best practice around isolation and quarantine with the facilities.
David Spivey, president of St. Mary Mercy Livonia
We have a very strong foundation in terms of working with other providers in the community, the fire and safety group, the police and other community organizations. And I think we have, through this crisis, understood that as a health care provider within a community public health opportunities exist when you have a strong foundation. I look forward to building upon that foundation and set of experiences that we've had to further the health status of the citizens in and around Livonia.