By JULIE MINDA
More than a year and a half into the COVID-19 pandemic, a fourth wave of infection was driving new caseload spikes in communities across the U.S. this summer. Already taxed by the ravages of prior surges and shortages of essential staff, many hospitals were stretched up to or beyond their capacity.

A sampling of ministry leaders in early September said their facilities were exhausting every viable mechanism to shore up their staffing, expand capacity and leverage the resource allocation efficiencies of partnerships with other hospitals. Many of these leaders worried about the short- and long-term costs of the continual strain.

During a late August press conference, Dr. Steven Nemerson, Saint Alphonsus Health System's chief clinical officer, said, "We are losing the COVID battle. This fourth COVID surge is the worst we've seen. Patients are dying unnecessarily" as the vast majority of hospitalizations and fatalities are among unvaccinated patients. The Boise, Idaho-based system is part of Trinity Health.
'A pandemic of the unvaccinated'
Jennifer Burrows, chief executive of Portland's Providence St. Vincent Medical Center and of Providence St. Joseph Health's Western Oregon region, said capacity strains at Providence's two Portland hospitals resulted in part from rural Oregon facilities transferring patients in need of higher acuity care, most of them with COVID. She said many of these rural areas had lower rates of vaccination than Portland.

Oregon had locked down during much of the pandemic, but it had eased restrictions in late June before the highly contagious delta variant swept through the state. Gov. Kate Brown reinstated strict coronavirus restrictions in late August.
During a Sept. 2 press conference, clinical and administrative leadership of Dignity Health's Marian Regional Medical Center in Santa Maria, California, said their intensive care units were full of COVID patients. Many ventilator-dependent patients were dying. The hospital was treating a younger patient population with COVID than earlier in the pandemic, likely because older generations have higher vaccination rates, hospital officials said. Dignity Health is part of CommonSpirit Health.

When he spoke to the press in August, Saint Alphonsus' Nemerson said although Idaho had not yet hit a caseload peak, COVID patients were crowding emergency rooms. He warned of increasingly long waits and delayed emergency care for all patients. He called the latest surge "a pandemic of the unvaccinated and the young."
St. Joseph Regional Medical Center of Lewiston, Idaho, said almost 90% of the COVID patients it hospitalized between mid-August and mid-September were unvaccinated. According to media reports, data from the Idaho governor's office show that since January the unvaccinated have accounted for 98.6% of COVID hospitalizations and 98.7% of COVID deaths statewide.
In Baton Rouge, Louisiana, the 988-bed Our Lady of the Lake Regional Medical Center had 155 COVID patients in early August, with 55 of them in its 166-bed capacity intensive care units. It was admitting an average of one COVID patient per hour.

Jerry Carley is president and chief executive of the Benedictine long-term and continuum-of-care system. Its facilities are concentrated in North Dakota and Minnesota. In an interview in early September, he said that while many of the cities and towns where Benedictine operates were experiencing COVID caseload increases, he suspected the Upper Midwest was just at the start of its peak.
He added that while only a couple Benedictine campuses had residents who were COVID-positive, dozens of campuses had COVID-positive staff. Carley spoke to Catholic Health World before President Joe Biden announced Sept. 9 that he would mandate that health care workers within all Medicare- and Medicaid-certified facilities get vaccinated. Carley said about 85% of Benedictine facility residents and 65% to 75% of staff were vaccinated.
Anticipating problems
Ministry leaders said their systems and facilities have been collaborating with competitors to address surge complications regionally, and they've been making operational changes to stay ahead of emerging problems.

Saint Alphonsus participates in a statewide collaborative of health care providers that addresses labor and supply challenges related to COVID surges. Participants are in regular contact to deploy resources, including staff, to Idaho communities where health care capacity is strained.
To free beds at the tertiary level for very sick patients, smaller hospitals have been accepting transfers of patients who no longer require tertiary-level care, but are not ready to be discharged home, said Nemerson.
On Sept. 7, Idaho implemented "Crisis Standards of Care," protocols allowing hospitals in its panhandle and north central area to balance the needs of the community and the needs of individuals. On Sept. 16, Idaho expanded the application of those standards statewide. The designation permits hospitals to provide care outside of the usual standard if they exhaust their resources. For example, hospitals may conserve their supply of oxygen by using air for nebulizers, when possible, or reusing single use items after sterilization. The standards also allow hospitals to "allocate resources to patients whose prognosis is more likely to result in a positive outcome with limited resources."
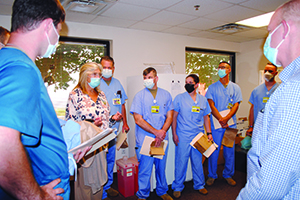
Lewiston's St. Joseph Regional Medical Center is in the affected area. A hospital spokesman said Sept. 13 that although it was operating at the very edge of its capacity and its COVID caseload was at its heaviest, it had not yet had to activate Crisis Standards of Care.
In mid-September, Saint Alphonsus was outside the area where the state authorized Crisis Standards of Care. Saint Alphonsus was delaying elective procedures in September as capacity levels dictated and expanding patient care into hospital classrooms.
Providence's Oregon region stood up a statewide logistics center early in the pandemic that was being put through its paces in the late summer surge. Burrows said the center uses data from a local university and internal Providence data to help predict and respond to surges.
An intensivist on the logistics center's staff provides consultation to rural critical access and rural community hospitals, including those outside of the Providence network, to help them safely treat patients in place instead of transferring them to a higher level of care.
In late August, in Roseburg, Oregon, CommonSpirit's CHI Mercy Health Mercy Medical Center partnered with primary care provider Aviva Health to triage COVID patients as they arrived at the hospital's emergency room. Working from a tent near the emergency department entrance, Aviva staff sent those with mild to moderate symptoms to an on-site mobile unit also operated by Aviva for an exam and follow-up care.
Clinicians with the Mercy health system of Chesterfield, Missouri, have been encouraging the use of its telehealth service to keep COVID patients from deteriorating to the point they require hospitalization. A team of emergency medicine physicians care for patients via phone, text and video links.
As of early September, all of Mercy's hospitals in four Midwestern states had experienced an influx of patients with the delta variant.
Uncertainty ahead
During the Marian press conference in early September, Dr. Barry Feldman, chief medical officer of the intensive care unit, said, "There is a lot of dying in our hospital now, and we're feeling really frustrated because this is preventable. It weighs on everyone. It's been a very, very long year and a half."
Providence's Burrows said, "It is humbling to realize we're a long way from beating this. It's humbling to realize that we have to stay diligent and keep learning. We have to practice self-care and be resilient because there's still work ahead of us."
