The COVID-19 pandemic has made the last year one like no other for health care workers. The scope of the illness has pushed hospitals' capacities to their limits and tested the endurance of their staffs.
The diligence of medical workers has kept the virus from taking an even more devastating toll and gotten more than 30% of Americans vaccinated by early May.
For many months, Catholic Health World has been profiling frontline health care workers and system leaders about their extraordinary efforts during the pandemic in a series called Rising to the Call. It can be found at chausa.org/rising. This spring, we invited eight more workers to reflect on the unique challenges of the past year. They shared how innovative thinking, collaboration and support from executive leadership, their colleagues and their communities helped them surmount hardships.
David "Puddy" Agans
Director of mission
Mercy Hospital Ardmore in Oklahoma

When the pandemic was hitting Ardmore, Oklahoma, hardest late last year and early this year, David "Puddy" Agans saw the demand for chaplaincy services at Mercy Hospital Ardmore shift from patients to staff.
Agans says that on the worst days, patients with COVID-19 made up 80% of the hospital's census. Tracking sites showed the rate of viral spread in the community of about 25,000 was the ninth worst in the nation.
The hospital's chaplains reported that three out of four of their requests for counseling were coming from staff. Previously, most of their requests came from patients or families.
"We were in a bad place," Agans recalls.
When a hospital survey found that workers wanted better communication and better support, Agans headed up the effort to address that need by stepping up outreach to staff. Employees voiced concerns and leaders shared information and encouragement at staff town halls. Executives scheduled regular events such as free meals to lift spirits and show their appreciation for the staff's perseverance.
The community pitched in, too. Churches held prayer services in front of the hospital. The Ardmore Chamber of Commerce got 25 businesses to sponsor hospital departments. The sponsors sent goody bags and arranged catered meals. Often, the gifts came with handwritten notes of gratitude.
"It was really cool just to see the reactions on co-workers' faces when they received them," Agans says. "They were blown away by how much time people spent letting them know they were cared for."
He says the dedication of his colleagues during the pandemic has reinforced his own faith in and commitment to his hospital's mission of service.
"There's been so many times when people have just given themselves selflessly to be the hands and feet of Christ," he says. "It's great when you work for an organization that lives its values."
Brianna Erickson
Intensive care unit nurse
Avera McKennan Hospital & University Health Center in Sioux Falls, South Dakota
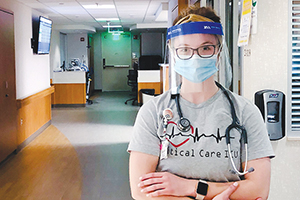
Brianna Erickson began her nursing career in February 2020, just as the novel coronavirus was beginning its deadly sweep across the globe. She chose intensive care to challenge herself and because she saw it as an opportunity for continuous learning. She got challenges and learnings aplenty in the last year.
"I've tried to look at COVID, as a new nurse, as a learning experience and as a positive experience more than anything, even though many of the days were hard," she says.
Erickson knew she would see death in the ICU but nothing prepared her for the number of lives lost to COVID. She arrived ready to comfort fearful and suffering patients but had not anticipated what it would be like to be the sole support at bedside for many patients in their worst or final hours.
"For a while, patients couldn't have family members in their rooms," she says. "We not only served as their nurse, but we served as their friend, their loved one and their family."
She recalls one patient who was on the upswing during a long bout with COVID. He couldn't talk but nodded yes when she asked if he was having a good day. She told him that made her happy. He mouthed back: "It makes me happy, too."
Erickson drew on the support of colleagues to endure such a trying year. "If I didn't have our teammates in the ICU to help me out, I don't know if I would have made it through this year," she says.
Erickson says she has had no second thoughts about her career choice. She says of her trial by pandemic: "I think it really made me a better nurse."
Dr. Varsha Moudgal
Infectious disease specialist and chief medical officer
St. Joseph Mercy Livingston in Michigan
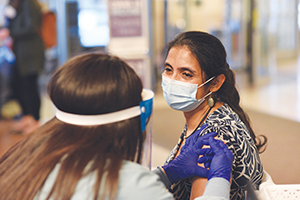
As a physician leader and infectious disease specialist, Dr. Varsha Moudgal has been a key decision-maker in how St. Joseph Mercy and other Saint Joseph Mercy Health System hospitals have revamped their operations and protocols in response to the challenges of COVID. Because there was no playbook early in the pandemic, sometimes those changes came fast and furious.
On occasion she has called people in the morning and told them, "'Can you please pass on to your colleagues that the protocol we're going to adopt for the day is XYZ?' An hour later it will change and I call them back. All of my colleagues have demonstrated extreme grace, extreme resilience and understanding in willingness to change."
Moudgal often explains the rationale behind revisions to hospital staff. She speaks not just as a leader but as a frontline colleague since she is in COVID wards providing care to sick and dying patients and bearing witness to the dedication of her colleagues. "No one said, 'You know what? I can't do this. I'm not going to do this.' Every single person said, 'How can I help?' And to me that single thing stands brightly."
Moudgal says she worries that the public and her fellow care providers are suffering from pandemic fatigue. She is continuing to advise that those not vaccinated wear a mask.
"How well we as a society can continue to keep these restrictions in place while the vaccine takes effect, that will determine when this pandemic will end," she says.
Omar Jome
Lead registered nurse for caregiver health services
Providence St. Joseph Health in Everett, Washington

Omar Jome's job is to care for caregivers at Providence St. Joseph Health. During the pandemic, he and his colleagues in caregiver health have worked with Providence St. Joseph Health system infection prevention specialists, pharmacists and human resources staff to give clinicians the latest information about personal protective equipment and COVID care protocols.
He has administered hundreds of vaccines, many of them to colleagues. One of the first was to Dr. George Diaz, the infectious disease specialist who treated the first known COVID patient in the nation.
"It's been a difficult situation for all of us, but we've worked so hard together to bring forth solutions and comfort to each other," he says. "While the pandemic has been challenging, it has also inspired us to do things differently and make changes to meet the needs of our patients and caregivers."
Lauren Landwerlin
Executive director of corporate communications
Saint Francis Health System n Tulsa, Oklahoma

"We often say that we do crisis well," Lauren Landwerlin says of the Saint Francis Health System. As the largest health system in Oklahoma, "people look to us in hard times for reassurance and trusted information," she says.
And that's been especially true during the pandemic when misinformation about the benefits of masking and social distancing and then anti-vaccine rhetoric blew up across the internet. Landwerlin's job as the lead communicator on the system's pandemic incident command team is to get the message out to 10,500 staff and the public that Saint Francis is committed to science and guiding the community through a public health crisis of epic consequence.
She wants the public to focus on the pandemic risk and take action, the way a blaring tornado siren on a stormy day can focus the mind on survival.
At her suggestion, the system took out a two-page ad in late October in the Tulsa World newspaper that warned: "We're headed in the wrong direction." A graphic showed the steady rise in the COVID patient population at the system's seven hospitals.
"It was around the time that there wasn't as much attention on COVID because people had started to get used to living in a pandemic," she says. "On the outside of a hospital, that may have felt OK, but on the inside, when our numbers were climbing, that was not reality."
The ad got attention, including a mention in the Washington Post. "I think it sparked more conversation about the seriousness of where we were headed and the impact the pandemic was having on health care workers, which obviously was significant and is significant," Landwerlin says.
Still, COVID continued to spread and at its peak in Tulsa, Saint Francis had 278 inpatients across four hospitals receiving care for symptoms and complications of the virus. As the COVID patient population has declined, Landwerlin has focused more of the system's communications on overcoming vaccine hesitancy.
One of the biggest lessons she has learned from the pandemic is this: "You have to understand your mission and actively choose to represent it every day."
Dr. Mary C. Raven
Medical director for palliative care
Mary Bird Perkins – Our Lady of the Lake Cancer Center in Baton Rouge, Louisiana

Dr. Mary C. Raven saw early on in the pandemic that demand for palliative care would be intense. National experts were worrying openly about potential shortages of pain and anxiety drugs used in compassionate end-of-life care.
Patients with COVID complications admitted to Our Lady of the Lake Regional Medical Center were deteriorating rapidly and dying quickly. Many of the overwhelmed care providers had little time and lacked experience to explain to patients and their families what was happening.
Raven and others on her palliative care team began collaborating with the ICU staff to help them provide compassionate care to dying patients and to comfort families who, because of COVID precautions, couldn't be at the bedside for final goodbyes. The care and comfort has included praying, hand holding and arranging phone or screen time to bridge the divide.
She and her palliative care colleagues have huddled with the care providers on COVID units to learn about the sickest patients. Afterward, they would call families to provide updates on their loved ones' conditions, tell them about the care being provided and sometimes ask difficult questions about treatment. They braced the relatives for the direness of the situation before hosting virtual visits.
"Most of these patients were intubated and many of them sedated but it gave the families some comfort to at least have their voices be heard" by the patient. "Sometimes it was to provide encouragement and sometimes it was to say goodbye."
Her team also saw to it that the care providers in the units had access to iPads so they could link patients with loved ones on video calls and they worked with hospital administrators to adjust visitation policies so families now can visit patients dying of COVID and other causes.
"I think that one of the things that's kept me going over this past year is knowing that in the face of such immeasurable grief and horrible tragedy, we are needed and we have a skill set that we can bring to the table and we can do something," she says.
Dr. Sriram Vissa
Vice president of medical affairs and chief medical officer
SSM Health DePaul Hospital in suburban St. Louis

Dr. Sriram Vissa recalls that there were many unknowns when the first wave of COVID reached St. Louis in spring 2020.
"Things were evolving very rapidly," he says. "There wasn't clear information in the beginning. Also, we had a significant shortage of treatment protocols and protective equipment such as masks, gowns and gloves."
A big part of Vissa's role has been to bridge the communication gap between workers and system and hospital leaders. By keeping the information flowing in both directions, he has strived to keep morale up and anxiety down.
"It was certainly, I would say, a challenging ask of leaders," he says. "In normal times we are dealing with various other safety, quality, credentialing and medical affairs issues, but 100% of our time during this pandemic was being the resource that connected the front line with the administration."
By this spring, the staff at DePaul Hospital was catching its collective breath after a surge of COVID patients that started late in 2020. To handle the load, the hospital had to shift clinicians from other departments to COVID care, expand its ICU capacity, add negative pressure rooms and open a temporary morgue on its parking lot.
"Personally, I saw the best of humanity in the people that work at DePaul Hospital," Vissa says. "I witnessed collaboration, collegiality and empathy. It just makes me feel that I'm at the right place."
Cassie Visser
Wellness Director, foundation director and spiritual care coordinator
Benedictine Living Community-Ada in Minnesota

Cassie Visser felt a bit like a jailer when she enforced precautions including social distancing to keep the coronavirus from spreading among the residents of Benedictine Living Community-Ada.
Before COVID, she delighted in planning all the fun social activities at the campus, now she had to tell residents to stay isolated in their rooms. "Honestly, I really struggled," she says.
It didn't take long before she and her colleagues were coming up with creative ways to keep residents amused and connected. For instance, for Mother's Day 2020 they arranged a car parade. Families drove around the building waving and holding signs while the residents greeted them from sidewalks or waved from windows. "That was a really bright spot," she says.
Another bright spot came this spring when the center was able to welcome back its volunteers. The first was a man who delivers activity calendars and menus to patients' rooms. "When I called to ask if he could come back, he was in tears," Visser says.
She continued to tap donors for contributions and found that the pandemic hadn't diminished the desire to give. Her appeals brought in enough that the center was able to buy headboards, footboards and nightstands for every room to finish a remodeling project started a few years back.
"Everybody could relate to isolation and being stuck in a room by yourself, so it was a good year to do that one," she says of the fundraising campaign.
By this March, even as Visser was rejoicing that the skilled nursing and assisted living facility had managed to avoid a COVID outbreak, she still worried that due to infection control precautions her job might never go back to being all about making residents' wishes come true. However, with volunteers beginning to return and the chapel reopening for in-person services, she was feeling hopeful.
"We are stronger than we would ever know and we're so fortunate to have our faith and have a spiritual belief that we will get through to something bigger and better," she says.
