By COLLEEN SCHRAPPEN
Since the passage of Title IX legislation in 1972, which increased athletic opportunities for female students, there has been a steady rise in the number of girls playing sports. Almost 70 percent of girls in the United States are, or have been, involved in organized sports, according to the Women's Sports Foundation.
But with more athletic participation comes a greater incidence of sports-related injuries. About 300,000 people in the United States each year suffer a tear to the anterior cruciate ligament, which stabilizes the knee joint. About two-thirds of those are not caused by contact or collision with another person or object, says Sue Barber-Westin, the director of clinical studies for the Noyes Knee Institute in Cincinnati.
Girls, in particular, are at high risk for this type of injury. According the Centers for Disease Control and Prevention, female athletes are four to six times more likely than males to suffer noncontact ACL injuries, which typically are caused by sudden movements such as changing directions, making quick stops, cutting or jumping. Sports such as soccer, basketball and volleyball are most stressful to the knee ligament.
ACL injuries often require surgery and up to a year of rehabilitation. The injury brings an increased risk of reinjury, or injury to the opposite knee, and can cause the early onset of osteoarthritis.
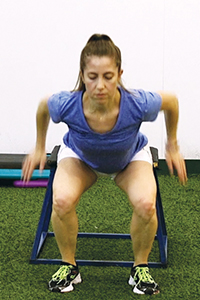
Land like a cat
"There are at least 20 different explanations and risk factors as to why female athletes disproportionately suffer such injuries," says Barber-Westin. "No one really knows how to predict an ACL injury, but a major risk factor is neuromuscular imbalance — where a female athlete lands from a pivot, cut or jump and has a wibble-wobble in the knee joint.

"That poor control puts the knee at risk to tear the ACL. That's the simplest explanation."
Female athletes are also more likely to have slower reflex times, land in a flat-footed position and have poor hamstring strength when compared to their male counterparts, says Barber-Westin.
Other risk factors include anatomical differences in females: a wider pelvis, smaller ACLs and more laxity in the ligaments than in males. Family history and the athlete's stature are also associated with increased risk.
"The main factor that can be modified is neuromuscular," Barber-Westin says. "You get them to land in a more balanced position that reduces the risk of injury, similar to landing like a cat."
Training makes a difference. "The beautiful thing is you can reprogram the girls to move like the boys do," she says.
Changing movement patterns
About three dozen intervention programs have been described in published literature since the mid-1990s, but only two have objectively shown significant improvement in changing risky neuromuscular movement patterns and reducing noncontact ACL injuries in female athletes, according to Dr. Frank Noyes, the president and medical director of the Noyes Knee Institute and a Mercy Health — Cincinnati orthopedic surgeon.

In a literature review, Noyes and his team identified factors that led to many programs' lack of success: the duration of the training was not long enough; training sessions were unsupervised or there was a lack of compliance in training; instruction on body positioning was not given during plyometrics, or jump training; and comprehensive strength training was lacking.
Noyes and Barber-Westin have published 22 articles in peer-reviewed orthopedic journals on ACL injuries in female athletes as well as two textbooks on the subject.
Noyes and his team presented findings on the two programs that have been proven effective, Sportsmetrics and Prevent Injury and Enhance Performance Program, in March at the annual meeting of the American Academy of Orthopaedic Surgeons.
The two programs can work in tandem, Noyes says. The six-weeks Sportsmetrics program is used prior to the sports season, and the injury prevention and performance enhancement program is used as supplemental training during the season.
But it is Sportsmetrics that is Noyes' baby. He developed it in 1996 with a team of athletic trainers, physical therapists and researchers, piloting a study with a girls' volleyball team. Three years later, the "big formal study" was done with girls' teams from 11 Cincinnati high schools. Half the athletes participated in Sportsmetrics training; half did not.
The ACL injury rate of the Sportsmetrics-trained female athletes dropped 72 percent, to the equivalent of male athletes.
"It was the first study that showed you could alter behavior," says Noyes. Since then, more than a thousand sites in the United States and worldwide have employed the program, with more than 1,200 individuals — usually physical therapists, athletic trainers and coaches — participating in two-day training sessions at the Noyes Knee Institute to become certified in Sportsmetrics training.
Since then, subsequent studies have found that Sportsmetrics improved athletes' muscle strength, decreased landing forces, decreased knee movement, improved body alignment and dynamic balance, as well as athletic performance indices such as speed and endurance.
Sportsmetrics is run as a nonprofit program. It is funded by the Cincinnati SportsMedicine Research and Education Foundation, which Noyes founded in 1985. In Cincinnati, 3,600 athletes from middle school through the professional level have undergone Sportsmetrics training. Mercy Health offers it as part of the comprehensive sports medicine service and athletic trainer coverage it provides to 30 local high schools and colleges, club sports and arts organizations.
Soft landing
Stephanie Smith is the Sportsmetrics program manager. She and other certified trainers guide athletes through three sessions weekly of the six-week preseason program.
"We start with a dynamic warm-up and then the focus is around plyometrics, teaching them how to land safely. We move through agility, speed and strength training drills and finish with flexibility," Smith says.
"We start to see significant difference as to how athletes land from a jump — the impact of landing. We're trying to decrease ground reaction forces."
The softer landings cut down on the pressure put on the joints. That, along with coordination, agility and muscle strength, are the winning components of Sportsmetrics, Noyes says.
"You can never (totally) prevent ACL injuries," he says. "We don't oversell the program.
"But it's showed efficacy across the spectrum, from middle school to professional athletes. We are pleased that Mercy Health has supported (our) efforts. It's a great example of a community hospital system getting involved."
High school students learn trainers do much more than tape ankles Mercy Health athletic trainers Barbara Battaglia and Kyle Hickey recently had students in the Sports Medicine Club at Turpin High School paint the soles of their feet and then tread across a long sheet of butcher paper.  Highschool students in a Sports Medicine Club sponsored by Mercy Health of Cincinnati analyze their gaits to predict the risk of injury. It was a colorful way to analyze gaits and predict risk of injury. "Everyone made a different imprint, showing who was more prone to injury because of their foot patterns," says Battaglia. Battaglia and Hickey started the Sports Medicine Club at the Cincinnati-area high school this school year to introduce students to related careers and familiarize them with first aid and health topics. Sports medicine is a big tent that takes in physicians, athletic trainers, physician assistants, physical therapists, occupational therapists, nurses, and others. A couple of times a month, about 15 to 25 students — freshmen to seniors — meet after school. "It was a way that we as athletic trainers were looking to get more involved with the students," says Battaglia, who notes that many students and adults do not really know what athletic trainers do, and often don't see an athletic trainer unless they have been injured. Athletic trainers condition athletes to advance their performance, prevent injury and promote injury recovery, among other things. "It isn't just taping ankles and filling water bottles," says Hickey. "It's a health profession and a well-rounded health profession. There are so many topics to touch on." Jobs in athletic training are expected to grow by 21 percent between 2014 and 2024, much faster than most professions, according to the U.S. Bureau of Labor Statistics. That increase is attributed to a better understanding of the effects of sports-related injuries and an aging population that is remaining active in their senior years. During the same time, the Bureau of Labor Statistics forecasts a Mercy Health partners with 25 high schools in Cincinnati and its suburbs. It provides a certified athletic trainer to be the school's primary athletic trainer. A Mercy health sports medicine specialist is the team physician at these schools. So far, Turpin is the only school with an athletic training club, though others offer sports medicine classes. "Not everyone will become an athletic trainer," says Hickey, but the tools and skills are helpful to any athlete: stretching, nutrition, how to build a first aid kit, injury prevention and rehabilitation, and strength training. This year the club took a field trip to Mercy Health — Wellington Orthopaedic and Sports Medicine to try out some of the equipment there, including an AlterG antigravity treadmill, which lets injured runners resume training by reducing the pressure on their joints. Next year Hickey and Battaglia are planning on bringing in more guest speakers for the club. Eventually, they would like to start a program that would allow students to shadow them as athletic training aides. "This has been a really cool opportunity to get to know students and promote our field," says Hickey. "We have a lot of fun with it." — COLLEEN SCHRAPPEN |
