Goal is to reduce use of opiates in the ER
By BETSY TAYLOR
PATERSON, N.J. — It's a Monday morning at St. Joseph's Regional Medical Center, and the emergency department is hopping. Patients arrive sick, injured and in pain, whether from a heart ailment or a wrenched back, from sickle cell disease or kidney stones.
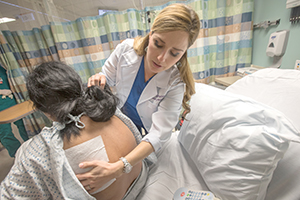
Photo by Jennifer Brown
All of these patients — those lined up at the admissions desk and others transported in by ambulance — are seeking care and pain relief at an emergency department that in January of 2016 set out to manage acute pain without prescribing opioids whenever possible.
New Jersey, like much of the nation, is struggling with an epidemic of opioid abuse and addiction. More Americans than ever before died in 2015 from drug overdoses, and 33,091 of those deaths involved opioids, according to a December data analysis from the Office of National Drug Control Policy. These deaths are from drugs sold on the street like heroin and heroin cut with fentanyl, a synthetic opioid; and also from prescribed opioid pain medications. In New Jersey, the drug-related death count started to mount six years ago, with about 1,300 people dying from opioid-involved overdoses in 2015, the most recent year for which figures are available from the New Jersey medical examiner's office.
Dr. Alexis LaPietra is the medical director of emergency medicine pain management for St. Joseph's Healthcare System, the system that includes St. Joseph's Regional Medical Center. She opposes the widespread practice of prescribing opioids as a first-line response to pain: "It's almost like using a sledgehammer to sink a cork." And the ripple effects can capsize the lives of individuals who become addicted to the pain medication or take it differently than prescribed.
For increasing numbers of Americans, prescription drugs serve as their first exposure to addictive substances and provide a "first stepping stone to future addictive use," writes Dr. Anna Lembke, a psychiatrist and the chief of addiction medicine at Stanford University School of Medicine in her 2016 book Drug Dealer, MD: How Doctors Were Duped, Patients Got Hooked, and Why It's So Hard to Stop. She writes that the majority of new heroin users "cite prescription opioids as their first exposure to opioids, a clear generational shift."
No more sledgehammer
St. Joseph's Regional Medical Center care providers researched best practices to find alternatives to opioids while still aggressively managing pain in the emergency room. Physicians say the change in approach to pain management at St. Joseph's Regional Medical Center has benefited patient care and created a culture change where they're more mindful about the risks and benefits of prescribing opioids in every instance.

Photo by Jennifer Brown
Opioids continue to have appropriate uses, including for severe cancer pain or for patients in intense pain related to a recent physical trauma, said Dr. Mark Rosenberg. He chairs emergency medicine for St. Joseph's Healthcare System and is its medical director of population health. But the pain associated with certain fractures can be successfully controlled with ultrasound-guided nerve blocks. And some back pain responds well to trigger point injections, he said.
Dr. Kristy Ziontz oversees the care of patients under observation in the ER. She said under the new protocols, she'll get a physical therapist involved early in treatment of a patient with back pain, to assess if strengthening exercises and movement might address the root cause of the pain and be beneficial to healing. In the past, the same patient might have been prescribed bed rest and be sent home with a prescription for an opioid painkiller.
An emergency department physician, Dr. Marco Propersi treated a patient in November who was suffering the excruciating pain of acute sickle cell crisis. Propersi first tried the patient on "a ketamine drip" — an intravenous dose of the anesthetic drug — before prescribing an opioid, Dilaudid, because the patient remained in pain after the first medication.
People's choice
St. Joseph's may have as many as 150 patients in its emergency department at any one time. Patient feedback about trying treatments other than opioids has been positive. "I don't think I've had any complaints at all," Propersi said. "People here for medical issues want to feel better," he said, and doctors are using effective approaches to manage pain.
LaPietra checks in on one of her patients, Dilia Lascarro Nieto of Garfield, N.J., who came to the ER complaining of chest pain and back pain. LaPietra started her on acetaminophen, an anti-inflammatory and a lidocaine patch, which numbed her back pain. LaPietra said these medications "get to the root of" the patient's pain, without the sedating effects of an opioid that can compromise a patient's breathing.

Photo by Jennifer Brown
A Spanish speaker, Nieto said she was worried about what doctors would tell her about her heart, but felt better than when she first arrived. "Bueno, bueno," she said by way of description.
Turning the tide
St. Joseph's emergency department began its Alternatives to Opioids Program with the three-pronged goal of keeping people from becoming dependent on opioids, offering drug-seeking addicts a path to rehabilitate from their addiction (see below), and reducing the supply of prescription opioid drugs being resold on the streets.
Rosenberg said in the first year of the new program, the emergency department prescribed opioids about 50 percent less than doctors here used to. Rosenberg said physicians at the hospital supported the changes: "This did not require a sales pitch to the doctors in our department," he noted. "This has been a major culture change."
Doctors here said St. Joseph's is part of a nationwide reset in thinking about the use of opioids for pain management. Government and health care organizations around the U.S. stepped up efforts in 2016 to combat opioid addiction, while also highlighting that pain still must be appropriately treated.
The Centers for Disease Control and Prevention, as one example, issued new guidelines for prescribing opioids last year — saying that health care providers in 2012 wrote enough opioid prescriptions for every adult in the nation to have a bottle of the pills. However, the CDC said few studies have been done to rigorously assess the long-term benefits of opioids for chronic pain, or pain lasting greater than three months or past the time of normal tissue healing. Furthermore, from 1999 to 2014, more than 165,000 people in the U.S. died from opioid pain medication-related overdoses. It's a health crisis many years in the making.
Rosenberg said "his hope and dream" is that the Alternatives to Opioids Program helps launch a new standardized approach to how pain is managed in trauma care and acute care settings.


