By JULIE MINDA
While hospice care is a covered service for patients with Medicare and most private insurance, not all people who are eligible enroll. Terminally ill patients who are not accessing this care are disproportionately from minority and other vulnerable population groups. Ministry members have identified hospice underuse as a health equity concern that they are working to understand and remedy.

Despite the availability of insurer reimbursement, "we still have about 50% of those who can benefit from hospice care who aren't receiving it," said Ben Marcantonio, chief operating officer of the nonprofit National Hospice and Palliative Care Organization. He said some of the most underserved population groups when it comes to hospice care are African Americans, Latino Americans, Asian Americans, people who are LGBTQ and people who live in rural areas.
The Medicare hospice benefit pays for a multidisciplinary team to provide patient-centered medical care, pain management and emotional and spiritual support. Medicaid, the Veterans Administration and many private insurers also reimburse for hospice services, which can reduce suffering and hospitalizations at the end of life.

Calvary Hospital's Nancy D'Agostino said, "Patients and families are more in control of their situation when they are on hospice, since it is their goals that are being addressed." D'Agostino is vice president of community patient services for the Bronx, New York, palliative care hospital and hospice provider.

Cultural perceptions
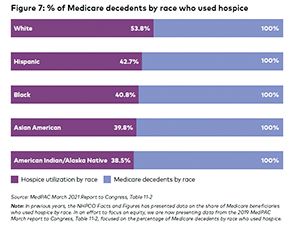
According to the 2021 edition of the National Hospice and Palliative Care Organization's "Facts and Figures Report," 40.8% of Black decedents insured under Medicare at the time of their death used hospice, as compared with 53.8% of white, 42.7% of Hispanic, 39.8% of Asian American and 38.5% of American Indian/Alaskan Native decedents. The data is based on MedPAC's March 2019 report to Congress. Roughly 10% of Medicare beneficiaries are Black.
The hospice organization's March 2021 edition of its "Black and African-American Outreach Guide" says that hospice and palliative care organizations that want to be intentional about reaching out to that underserved patient group must address "the unique health needs of Black/African-Americans," and take into account how access to care, cultural risk factors and socioeconomic barriers contribute to the prevalence of certain diseases. The guide says cultural competency is crucial to raising awareness of palliative care among Black consumers as it is in providing quality care to Black patients.
It recommends outreach that recognizes the influence of church leaders and family, Black media and cultural icons. It says the death in August 2020 of Chadwick Boseman drew attention in the Black community to the fact that colorectal cancer disproportionately impacts Blacks and that screenings for early detection save lives.

Boseman, 43, rose to iconic status in 2018 as the superhero lead in the blockbuster "Black Panther." He had kept private his 2016 cancer diagnosis. The shock of his death was a reminder that African Americans treat a decline in health as a "private, personal journey," according to the guide, a preference that palliative care and hospice providers should consider in shaping their strategies to advance health equity.
The New York City communities Calvary Hospital serves are as diverse as the United Nations, said D'Agostino, and hospital staff have set out to learn why members of certain racial, ethnic and religious groups seek hospice care to a lesser degree than whites. Not surprisingly, they determined that the general distrust many Black patients express toward health care providers based on historic wrongs combined with any individual's experience of racism or inequity in health care factored into decisions to avoid hospice care. Also, Black consumers may not be getting information on hospice in a culturally sensitive way.
Dr. Tammie Quest directs the Emory Palliative Care Center at Emory University. Speaking on a Nov. 1 webinar given by the Institute for Human Caring, part of Providence St. Joseph Health, she asked the audience to ponder how hospice concepts including "quality of life," "limitations on medical interventions" and the concept of "a good death" might be perceived by and applied to minority populations.
The distrust issue also is relevant for people who are LGBTQ, said the National Hospice and Palliative Care Organizations' Marcantonio. "Most hospices recognize that there are a wide range of families in the U.S. that are not defined by blood relations. But there is still education needed to ensure all families are treated with respect and compassion.
"Hospices tend to be more flexible and welcoming than many other conventional health care settings, but for a nontraditional family who has been poorly treated (by health care providers) in the past, those fears may be carried over to hospice," he said.
Calvary's service area includes large populations of Asian Americans. D'Agostino said many older Chinese Americans may have a cultural aversion to speaking about death.

Kyle Terry directs the hospice program of Saint Francis Health System of Tulsa, Oklahoma. He said that among some Asians in Saint Francis' hospice service area there is a perception that if people seek help outside the immediate family by accessing hospice, family members have failed in their duties to their sick loved one. And among some people of Latino heritage, there is a perception that suffering is God's will and that pain should be accepted rather than medically palliated, Terry said.

Rabbi Yerachmiel Rothberger, Calvary's Jewish community liaison, said some superstitious people may fear that talking about hospice will invite death. Some people may harbor misperceptions that high doses of morphine will be administered even if that goes against a patient's express wishes not to take treatment that could hasten death.
Community outreach
Ministry systems and facilities are taking on the perception issues that are hampering hospice use by intensifying their outreach and education work, particularly among vulnerable populations.
D'Agostino said to learn more about the sensitivities of minority populations and how best to reach them with hospice education, she often will talk with hospital staff members from those communities and with community leaders including religious leaders. They help Calvary understand how to gain people's trust and attention. They also provide advice on developing resources and materials that appeal to people in those communities.
Rabbi Rothberger said he has made progress dispelling myths among people in some of the Jewish communities Calvary serves and increasing their understanding of hospice's benefits. He offers an education program for community leaders and rabbis that includes hospice. He has built relationships with local rabbis and rabbinical organizations, and he's linked rabbis with Calvary clinicians so they feel comfortable engaging with hospital staff on behalf of families in their synagogues.
Calvary has a Shabbos lounge where families observing the strict prohibitions against exertion on the Sabbath can sleep. Two refrigerators in the kosher hospitality room across the hall are stocked with microwavable kosher meals.

Better together
Jennifer Finley, agency manager at Avera@Home Home Health and Hospice in South Dakota, said her organization partners with other health care organizations, churches, nonprofit organizations, state agencies and federal agencies including the Department of Veterans Affairs to raise awareness of hospice services among rural residents.
Avera@Home taps into this network to bridge any gaps in care that arise because the patient is too far from the health system's hospice service area. For instance, Avera may provide the nurse practitioner directing a rural clinic outside the Avera network with a hospice standing order set for a patient and offer the Avera hospice pharmacist's expertise to provide symptom management.

Finley said, "Our main goal is to be of help to people in providing end-of-life care. We will do what is needed to find ways to support people and be their safety net."
Her colleague Jill Cragoe, regional director of patient care services for Avera@Home, said, "We don't want anyone to die alone or in pain or without the right level of care for them."
Conversations on end of life not always happening at right time, say providers
Kyle Terry, director of the hospice program of Saint Francis Health System of Tulsa, Oklahoma, said it would benefit people to start thinking about and documenting how much health care they would want if they were to become critically ill and no longer able to speak for themselves. He suggests people do this in their 50s, before health crises become more likely.
But, people don't want to think about death and dying, he said, and they often turn and walk away when they see the hospice sign on the information booth he staffs at health fairs.
Nancy D'Agostino is vice president of community patient services for Calvary Hospital, a Bronx, New York, palliative care hospital and hospice provider. She said oftentimes when a patient is very seriously ill, clinicians, patients and family members understandably become so focused on saving the patient's life, that it is hard to acknowledge when curative care becomes futile. As a result, hospice may not be considered as a treatment option by the patient or family until death is imminent. (Medicare rules generally prohibit beneficiaries from accessing hospice while also seeking curative treatment, rules that hospice providers are challenging.)
Terry noted that during the pandemic many terminally ill patients have delayed seeking care and may have endured preventable suffering and distress as a result.
D'Agostino said it should be routine for health care providers from primary care family doctors to palliative care specialists to talk with patients about their end-of-life goals. For patients with progressive, chronic illness, it's important to have a conversation about advance planning for disease progression. She said clinicians should talk more deeply about patients' values and wishes if those patients have a serious illness that is worsening. If the condition is terminal and supportive care is needed at home, hospice can provide useful resources.
Jennifer Finley, agency manager at Avera@Home Home Health and Hospice in South Dakota, said when patients enroll in hospice, a social worker visits the patient usually with family present to discuss what's important to the patient and begin to establish a plan to support those goals.
Most hospice patients receive services at home or in a nursing home and hospice team members supplement care delivered by the patients' loved ones or facility staff. Visiting team members normally include a nurse, physician, social worker, chaplain and nurse aide.
D'Agostino said hospice care has been shown to lengthen the life of some patients, prevent hospitalizations and relieve pain and anxiety. Importantly, she said, it may enable patients to focus on achieving their goals, which might include resolving emotional pain or family conflict, attending a wedding or graduation, or simply spending more time with the people they love.
Guide helps hospice and palliative care providers become more inclusive
The National Hospice and Palliative Care Organization published a guide about a year ago to help hospice and palliative care providers to be a more inclusive presence in their communities.

The "Inclusion and Access Toolkit" makes a business case for including people of all backgrounds in outreach efforts, on boards and leadership teams, in the workforce and as clients. The 40-page tool kit provides strategies and practical tips for hospice and palliative care providers to assess how inclusive their organizations are and then to make needed improvements.
It contains advice for tailoring hospice and palliative care services and marketing to distinctive audiences.
An appendix lists common traditions and health beliefs, communication preferences and other relevant characteristics of African Americans, Chinese Americans, Latino and Hispanic Americans, and people in the LGBTQ+ community.
The tool kit can be downloaded for free at nhpco.org/diversity.
