A couple years ago, members of a caregiver support group at Peace Lutheran Church in Grand Island, Nebraska, got to talking about what it was like taking their loved ones with dementia to the hospital. Many of them had experienced difficulties because clinicians hadn't known the patients had cognitive impairments and unknowingly responded unhelpfully to behaviors associated with dementia.

The support group brought their concerns to Beth Deida, a fellow church member who is a maternal-child nurse educator and patient safety specialist at Grand Island's CHI Health St. Francis. Deida met with the group repeatedly to understand their concerns, engaged leadership at the CommonSpirit Health hospital to respond and formed a committee at the hospital to create solutions.
The result is St. Francis' REMEMBER initiative, which provides visual cues to hospital staff to alert them when a patient has dementia or other cognitive impairments. Staff have been trained on how to take evidence-based approaches to protect these patients' safety and well-being and to provide them and their families with wraparound support. The program launched in October.
When Deida reconnected with the caregiver support group that inspired the program, a woman whose husband has dementia told her, "Everything that we told you about the issues that we had, you've addressed." She said that prior to the REMEMBER program's inception, she was hesitant to bring her husband to St. Francis. But with the program in place, the woman relayed she would now say, "Only take him to St. Francis.'"
Deida says the woman's response "gives me goosebumps."
A disorientating experience
According to the Alzheimer's Association, more than 7 million Americans have Alzheimer's disease, and that count is increasing continually. Deida says the hospital has seen such increases locally.
A St. Francis press release on REMEMBER says a hospital stay can be disorientating for patients who have dementia. Unfamiliar surroundings, changes in routine and new medications can intensify their confusion and cause anxiety and agitation. This can distress patients, their loved ones and their medical team.
Fritz Anderson is a member of the Peace Lutheran support group for caregivers of people with dementia. The group meets monthly to discuss challenges their loved ones face, how the challenges impact them and potential solutions.

Five years ago, clinicians diagnosed Anderson's wife of 54 years, Kathy Anderson, with frontal temporal lobe dementia. The most dangerous aspect of her condition, Anderson says, is that her motor skills have degraded significantly, severely compromising her balance. Since her diagnosis, she has been to St. Francis' emergency department multiple times for head trauma after falls. She's also been admitted for surgeries unrelated to the falls.
Anderson says his main concern when his wife is hospitalized is that she will try to get out of bed, fall and sustain new head trauma.
He spoke about those concerns during the support group's initial meetings with Deida. He says support group members have described how their spouses were highly agitated in the hospital. In some cases, they didn't understand that their medical team members were clinicians trying to help them, and so they would resist care. The clinicians did not understand the dynamic and would mischaracterize the patients and treat them as combative. Group members also said during the sessions with Deida that there was poor communication about whether patients needed help eating. They also said there was a rotating roster of therapists, so family members had to re-explain the patient's conditions and needs with each fresh face.
Deida says that while the 153-bed St. Francis always has delivered high-quality care in line with industry standards, these patients and their families were nonetheless having negative experiences because clinicians didn't always know which patients had dementia and thus needed a different approach to care. , If clinicians did know the patients had dementia, they didn't always know how to alter their approach accordingly.
Deida recalls, "I promised the group I would personally ensure positive changes would happen and report back."
Forget-me-nots
Deida says while dementia is well outside her wheelhouse, she took to heart a St. Francis motto that "every patient is my patient."
She formed an interdisciplinary team of administrators and other leaders, nurses, therapists, social workers, imaging specialists and others. "All members of the committee are passionate about this project as they've each been impacted with a loved one who has had dementia or memory care issues," Deida says. Her twin sister, Emily Jensen, who has worked for the hospital for more than 20 years, co-chairs the group.
The group began meeting in January 2025. They conducted a literature review, consulted with the local Alzheimer's Foundation and talked with local specialists. They came up with the REMEMBER program. REMEMBER stands for Recognizing, Educating, Managing, Empowering, Multidisciplinary approach, Better experience, Enhancing safety, and Respect.
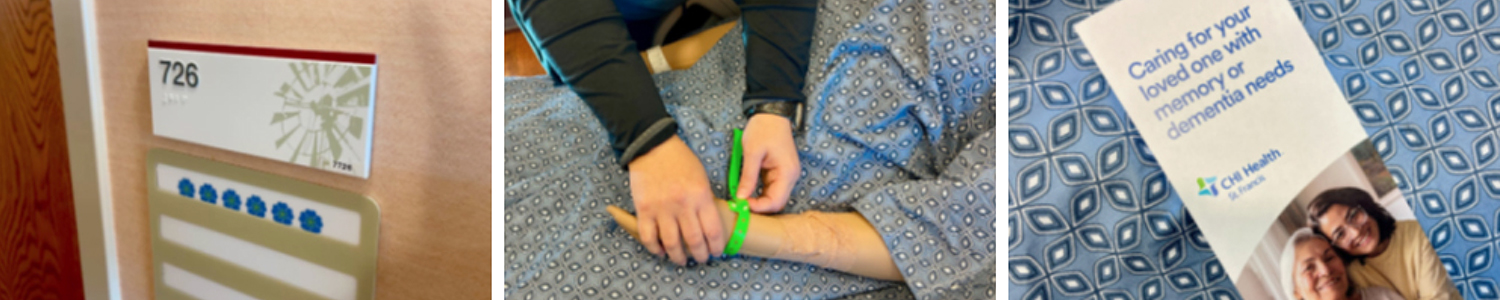
When patients opt into the program, they wear a blue hospital gown and green wristband (the reverse of all other inpatients), and staff affix blue and green forget-me-not flower decals outside the patient room door. These visual cues let staff know they should apply their specialized training as they interact with the patients.
Hospital-wide rollout
Leading up to the October hospital-wide rollout, Deida and her committee ensured every St. Francis department received information about REMEMBER. At department meetings, staff members heard the backstory of the program and learned what they can do to aid the patients and their families. They all received an email with more information.
The committee gave each department a tote bag containing the gowns, wristbands and door signage as well as brochures for patients and their families.
Additionally, the committee ensured that a tool St. Francis uses for smooth patient handoffs includes a prompt on patient dementia and memory issues. The committee also has recommended that clinicians suggest that patients' loved ones accompany them when they go to new areas of the hospital.
The committee also arranged for an expert to offer a certified dementia practitioner course at St. Francis. Anyone can take it. St. Francis' foundation takes care of the cost of the course for staff. The training covers how best to tailor care for people with dementia, how to protect their safety and how to communicate with them and their families.
Plans call for St. Francis to update the electronic health record system to flag patients who have memory issues. Plans also call for St. Francis to have a way for families to pre-enroll patients in REMEMBER so that the hospital has their information on hand in the event of a hospitalization.
The committee plans to share the program with other hospitals, including by presenting the program at a scholar and nurse leader conference this month and by publishing a manuscript in the Advancing Medical-Surgical Nursing Journal.
Daily rounding
The committee has been soliciting feedback on the new approach from hospital staff, families and the church caregiver support group. The feedback has been overwhelmingly positive, Deida says.
Clinicians say the new approach helps ensure that whenever a staff member — no matter what department they are with — walks into a patient's room, they know because of the visual cues that they may need to approach the patient in a different way than usual. Deida says it helps them to deliver more appropriate care, even when patients can't tell the care team about their needs or when loved ones aren't there to explain what is needed.
St. Francis is keeping data to better understand how care delivered under the REMEMBER approach impacts various metrics, including on patient falls. They've already seen a decrease in falls involving injury.
St. Francis nursing leaders now make daily rounds to check on how patients with dementia are faring under REMEMBER.
"Our patients are getting more personalized care that is helping not only to keep them safe, but to provide dignity," Deida says. "Their loved ones can feel secure in the care being provided and that their loved ones' unique needs are communicated shift to shift and department to department."
Anderson, the church caregiver group member, says, "What this team has developed at his facility should be more widely adopted; it should become the standard. The medical staff at St. Francis has been super, and it starts from the top down."
Further reading: In a CHA webinar, a hospice nurse challenges assumptions about people experiencing dementia losing their dignity.
