Strategies for SupportHERBERT SCHUMM, MD Early in the pandemic, Tait Shanafelt, MD, of the Stanford University School of Medicine, and colleagues conducted an analysis and identified six core requests from health professionals.1 Hear me: Listen to and act upon my expert perspective and experience. Protect me: Reduce the risk that I will acquire infection or be a transmission portal to my family. Prepare me: Provide training and expert oversight so I can provide high-quality care. Support me: Provide support that acknowledges human limitations during extreme work demands. Care for me: Provide holistic support for individuals and their families, especially if needing quarantine. Honor me: Acknowledge and express gratitude for dedication and sacrifice. These core requests remain powerfully relevant today, but the Delta variant presented some new challenges. First, our teams are tired. We are tired. While military troops may be deployed on a mission for three to four months, health care teams have been battling the pandemic for over 18 months. Secondly, our trust is tattered. The community that has always trusted caregivers now protests and resists their advice. Society's anger and frustration are evident across the care continuum, sometimes in an aggressive and hostile manner. Finally, it is fair to say that the empathy tanks of many are now empty. Empathy, which could be defined as compassion in action, requires a sense of time affluence and spiritual refueling.2, 3 Both are difficult to obtain with the current clinical and societal demands. Telling a housekeeper, medical assistant, nurse or physician to "just take more time" when striving to meet a patient's needs creates moral distress during a period of time poverty and lack of adequate staffing. In the midst of so many physical, emotional and spiritual hardships for caregivers, myself and others are asking, "What can we do as leaders and colleagues to make a difference and fuel my soul?" The following is a simple, yet sometimes difficult, strategy. It does not require money, an outside consultant or a new policy. 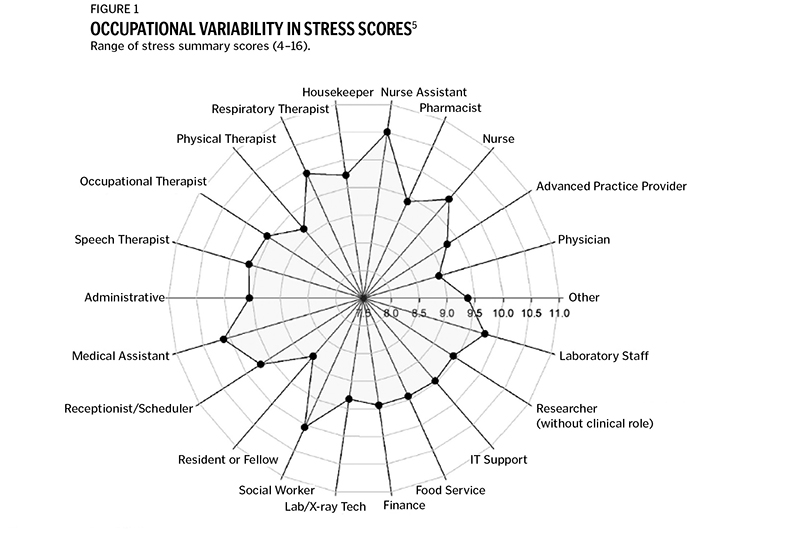
UNLOAD
Unload yourself and your team of anything non-critical to your current mission. Troops stop training and drilling when they are on a mission. Bon Secours Mercy Health recently evaluated mandatory learning and reduced the list to the critical few. The health care system modified the in-depth annual provider engagement survey to a much shorter survey focused on listening to the needs and perspectives of professionals.
ROUND
Round with empathy. Shanafelt and Quint Studer, known for his work in improving patient and associate satisfaction, have demonstrated the value of regular rounding for both the rounder and staff member.4 Empathy rounding focuses more on soothing and less on solving, more on listening and less on directing. Rounding can address all six caregiver requests identified by Shanafelt and coauthors. Recently, while rounding, a senior leader at Bon Secours Mercy responded to a patient's call light. The patient could not find his phone, something any administrator could "fix." When the patient attempted to get up, he set off the fall alarms. As three nurses rushed to prevent a fall, the leader felt she had created more work than relief, especially when one nurse noted the phone was in the patient's hand. Sheepishly, the leader apologized for creating more work. The nurses responded that they really needed a good laugh, especially at that time and perhaps at their leader's expense. A helpful guideline is: soothing, not solving; listening not directing. While our nurses and physicians tend to lead the care team, it is important to remember that all team members are hurting. A recent study showed medical assistants, housekeeping staff, social workers and therapists are experiencing even more stress than other health care workers.5 (See Figure 1.) Empathy rounding demonstrates that we care for each other, which is why the Bon Secours Mercy peer support program for physicians and advanced practice clinicians (APCs) was started with volunteers. Thus far, more than 200 individuals in need of support have called to talk with a colleague. As a result of these conversations, a greater awareness and reduction of barriers occurred regarding the employee assistance program. Physicians and APCs had a 70% higher rate of usage of the EAP than other associates. Think about your circle of influence. Who have you been missing? Who have you noticed is not their usual self? Round by reaching out for a chat, break or beverage — whether in-person or virtually. Soothe, don't solve; listen, don't lead. CREATE QUIET
Adopt a quiet time away from text or email, recognizing that we are all addicted to our devices. Even if you tell your team not to answer you at night, their devices still alert them. Your noncritical message adds to the nonstop data noise. Learn how to delay sending your emails after work and on weekends. Assure your team you will call or text if you need something after hours. CREATE BREAKS
Adopt a 25/50 rule by ending your meetings at 25 and 50 minutes respectively. We all have experienced back-to-back virtual meetings. Zoom fatigue is real and its draining effects are among us. Communicating electronically all day can deplete people's energy. Give your colleagues a break and end early. |