SUSAN DONLEY
America's population is aging fast. As more of us grow older, most families will need some type of extra support. Whether it's long-term or for just a few days, the quality care and services provided by the aging services sector can help us live better and thrive. Aging services — like home and community-based care, assisted living, adult day programs and life plan communities — help us maintain and lead independent, healthy and full lives.
COVID-19 has drawn significant focus on the aging services field over the past two years. While older adults and their care providers bore the brunt of this unprecedented crisis, the pandemic also created opportunities for positive transformation, including necessary policy changes, long-overdue public investments and heightened awareness of the sector.
LeadingAge, a national association representing more than 5,000 aging services nonprofits and other mission-minded organizations, is seizing this moment to benefit our members, the broader sector of aging services providers and the millions of older adults and families who we serve.
In January 2021, we launched Opening Doors to Aging Services, a research and communications initiative to help older adults and their families better understand how aging services deliver the care and support that many of us will need to lead a fulfilling life as we grow older. The endeavor was developed, in part, in response to members' concerns about the negativity directed at aging services providers (especially nursing homes) during the first year of the COVID-19 pandemic.
Many factors shape how people view the sector, so we began by exploring everything from the media and political environment to the opinions of leaders and influencers to the views of the general public. Our work included a range of research tactics:
- A landscape analysis of the aging services sector.
- Two national public opinion surveys of U.S. adults ages 18 years and older (conducted in May 2021 among 1,200 respondents and June 2021 among 800 respondents).
- A series of in-depth interviews with stakeholders from the field and adjacent sectors.
- A survey of LeadingAge members, with 262 respondents.
- A set of focus groups composed of potential consumers and family members of aging services, current consumers and family members, current staff and certified nursing assistants not working in aging services.
The results of our research paint a complex picture of a sector that is not well-understood, but has the potential for meaningful public support.
 THE LANDSCAPE: EXTERNAL FACTORS SHAPING PERCEPTIONS
THE LANDSCAPE: EXTERNAL FACTORS SHAPING PERCEPTIONS
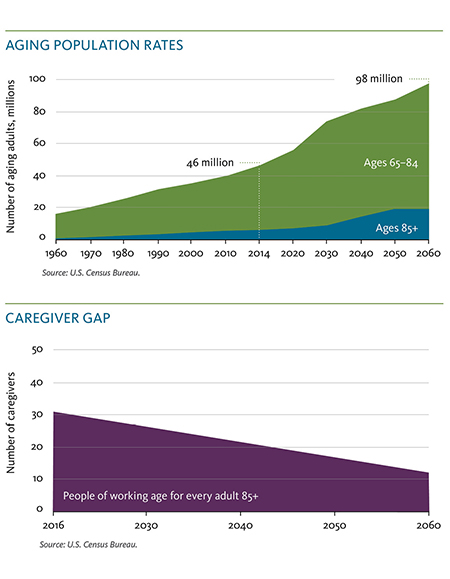
The landscape is grounded in a simple reality: we are all growing older. In fact, the aging population in the United States is growing exponentially.1 Americans from all across this country are poised to live well into our eighth or ninth decade of life, and according to the Administration for Community Living, seven in 10 will need long-term care and services — on top of the support to be provided from our families and friends.2 At the same time, there is an emerging gap between the number of available family caregivers and the number required to meet the needs of older adults. The caregiver support ratio in the United States is expected to decline between 2016 and 2060 from 31 to just 12 people of working age for every adult 85 and older, according to the U.S. Census Bureau. Aging services experts for years have raised awareness of the protracted challenges of workforce recruitment and retention. The demands of the pandemic, some health care workers' resistance to the COVID vaccine and staff outages due to COVID infection exacerbated this trend during the winter of 2021-2022.
The country is wholly unprepared for the aging boom and resulting care gap, according to experts. Policymakers have ignored the problem for decades, leaving us with a systemic lack of resources for aging services, and a complex web of disconnected services, regulations and reimbursement formulas. Many Americans expect to need support beyond family caregivers: the LeadingAge survey found that 62% of Americans may seek professional services as they age.3 Meanwhile, family caregivers are providing an average of 34 unpaid care hours a week, decreasing their employability and earnings, according to the Family Caregiver Alliance.4 On top of this, nearly half of all Americans have no retirement savings.5
In the wake of these overlapping crises, too many older adults are unable to access or afford desperately needed care and services; providers are unable to pay wages necessary to recruit and retain care professionals; and families are increasingly stressed, stretched and stranded in unsustainable situations.
Then the COVID-19 pandemic hit. Nursing homes were ground zero for the spread of the virus, and throughout the pandemic's first year especially, older adults and the aging services they depend on bore the brunt of the unprecedented crisis. This was notably so as COVID-19 put older adults at a disproportionate risk and exacerbated long-standing neglect of the aging services sector. As thousands of aging services and direct care professionals heroically battled the virus without the needed level of government support, supplies or resources, public confidence in congregate care settings, such as nursing homes, assisted living communities and senior housing, faltered.
While many policymakers and influencers were critical of long-term care during the height of the pandemic, some academics and aging services experts defended the field by pointing out that stories of "bad apple" providers receive disproportionate attention and fueled some misperceptions. They also reasoned that no part of our country's health care sector was prepared for this kind of public health emergency.
Just as growing social justice movements in the United States gave prominence to equity issues, the COVID-19 pandemic put a national spotlight on older adults and their care. Per LeadingAge's findings, more than half (54%) of U.S. adults do "not" agree that older adults are treated well in the United States.6 And the public has become more attuned to their needs and the professionals who care for them, who are predominantly women of color, including many immigrants. At the same time, the voices of advocates have become stronger, and care economy issues were front and center in the national policy debate during much of 2021.
As the media has followed these changes in the public discourse, it has focused on aging services more than ever. Researchers tracked news narratives that evolved over time, from a focus on COVID-related deaths in long-term care settings, outlier stories of abuse and neglect and federal aid misdirected to profiteers, to the emotional impact of isolation, heartwarming stories about reunions and coverage of proposed investments in the care economy. While many influential voices remain critical of parts of the sector, nearly all support increased public investment in care and services for older adults.
Many working in the sector felt stressed and under attack during the pandemic, but remain largely optimistic as greater attention is being focused on aging services, which they report is often ignored. Mission-driven aging services professionals, including LeadingAge members, are enthusiastic to adopt new learnings and technologies from the pandemic and to leverage the chance to enhance public understanding about the sector. They also indicate excitement about a new focus by policymakers on the needs of older adults and about finally building a system that supports access to affordable care and services for all.
 PUBLIC PERCEPTIONS OF AGING SERVICES
PUBLIC PERCEPTIONS OF AGING SERVICES
The views of policymakers, advocates and other stakeholders are important to how the field of aging services thrives, but no group is more critical to how the sector achieves its mission than the general public. These are the neighbors, clients, residents and families that aging services professionals serve every day.
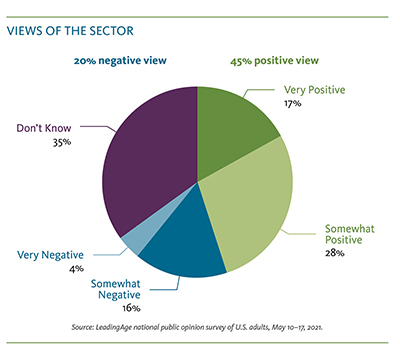
Today, public perceptions are mixed: according to LeadingAge's national public opinion survey, more than twice as many Americans view the aging services sector favorably (45%) as those who view it unfavorably (20%), but a large number of Americans (35%) say they don't know how they view the sector. These numbers suggest the sector does not face a public perception
crisis — but there is a real need and opportunity to improve the public's understanding of the field. When asked what comes to mind about the sector, the public most cites nursing homes, assisted living and health care, demonstrating a clear lack of familiarity with the breadth and variety of available aging services.
The COVID-19 pandemic took a heavy toll on older adults and eroded views of some providers. Per LeadingAge's findings, the public has a negative bias against nursing homes. The data shows that U.S. adults have the least favorable views (43%) of nursing homes, among 14 provider types. But consumers do not widely blame nursing homes for the tragedies of COVID.
Many parts of the sector are viewed positively by the public. In fact, LeadingAge's public opinion survey revealed that the majority (68%) of people who have had direct experience with aging services say it was a positive experience, most often citing quality as the reason. Quality is also a factor in why those surveyed have a more favorable view of nonprofits (63%) than for-profits (47%): they believe quality at nonprofit providers is better than at for-profit providers. The findings also revealed that U.S. adults view faith-based aging services providers favorably (63%).
Care professionals are also held in high esteem by the public, who describe them as compassionate, dedicated, essential and professional. The words they say least describe care professionals are lazy, incompetent, unskilled and disengaged. Adults in the LeadingAge survey consider them heroes of the pandemic, and as indicated in follow-up findings, found it credible to refer to them as experts.
However, results revealed that public opinion is less positive as it relates to the overall view of how older adults are treated in this country. Fewer than half of U.S. adults (46%) agree that "older adults are treated well in the United States." That number drops among women (36%) and in rural areas, where just one in three (32%) rural Americans agree that we treat seniors well.
Views are even more negative when it comes to policymakers: 83% of those who responded believe that "elected officials have failed older adults and the people who care for them by ignoring and underfunding America's aging services for decades." This dissatisfaction could stem from the finding that 89% expect the government to play an important role in ensuring that older adults are taken care of, and overwhelmingly support a greater public investment in aging services.
Public views on the sector have a uniquely "American" character to them. An independent spirit and a belief in the right to pursue happiness color perceptions of what it means to grow older and the kind of care Americans want. According to the LeadingAge findings, a full 85% agree that every American has a right to receive a basic level of housing, health care and essential support regardless of age. Even more Americans deeply value our right to the essentials that allow us to live with meaning and purpose: 91% of those surveyed say that older adults should have the support and resources they need to lead a fulfilling life. They also place high value on supporting independence and health as we age.
 But results showed that fear and denial of aging also play an indisputable role in perceptions. Many Americans do not consider themselves old, including 27% of people 65+ years old. Research shows that many people are concerned about being alone, needing care in a nursing home or experiencing health issues as they age. The rugged individualism that is deeply embedded in our nation's lore, combined with long-persisting ageism, has a stubborn impact on how the public views aging services.
But results showed that fear and denial of aging also play an indisputable role in perceptions. Many Americans do not consider themselves old, including 27% of people 65+ years old. Research shows that many people are concerned about being alone, needing care in a nursing home or experiencing health issues as they age. The rugged individualism that is deeply embedded in our nation's lore, combined with long-persisting ageism, has a stubborn impact on how the public views aging services.
CONCLUSION
The aging services sector is nuanced and complex. While it is not well understood by the general public, the sector has the potential for meaningful support, according to research. Factors indicating significant opportunity to increase public understanding and improve perceptions of aging services include:
1) Those who have experience with the sector feel positive about those experiences.
2) There is widespread admiration and support for those who work in the sector.
3) A large segment of the population is unfamiliar or unsure of what they think about the sector, creating an opportunity for learning.
4) The public has strong expectations that policymakers must support older adults and their families and invest greater resources in aging services.
5) The spotlight on the sector is brighter than ever, presenting opportunities to open our doors and showcase all that we have to offer.
SUSAN DONLEY is senior vice president, Communications and Marketing, at LeadingAge in Washington, D.C.
NOTES
- Mark Mather, Linda A. Jacobsen, and Kelvin M. Pollard, "Aging in the United States," Population Bulletin 70, No. 2 (December 2015): 3, https://www.prb.org/wp-content/uploads/2019/07/population-bulletin-2015-70-2-aging-us.pdf.
- "How Much Care Will You Need?", Administration for Community Living, https://acl.gov/ltc/basic-needs/how-much-care-will-you-need.
- "Public Survey Research on Perceptions of Aging Services," LeadingAge, May 10-17, 2021, https://leadingage.org/sites/default/files/Opening%20Doors%20Research_Public%20Perspective%2C%20Part%20Two.pdf.
- "Caregiver Statistics: Work and Caregiving," Family Caregiver Alliance, https://www.caregiver.org/resource/caregiver-statistics-work-and-caregiving/.
- Monique Morrissey, "The State of American Retirement Savings," Economic Policy Institute, December 10, 2019, https://www.epi.org/publication/the-state-of-american-retirement-savings/.
- "U.S. Attitudes About Investing in Aging Services for Older Adults," LeadingAge, June 29, 2021, https://leadingage.org/sites/default/files/3W%20Insights%20Survey_Attitudes%20About%20Investing%20in%20Aging%20Services_6.2021.pdf.
OPENING DOORS TO AGING SERVICESThrough LeadingAge's launch of its Opening Doors to Aging Services initiative in 2021, a full communications framework — including strategies, messages, audience insights and more — has been developed as a result of this research. Freely available to the aging services community, the Opening Doors to Aging Services strategic framework is designed to maintain and improve public perceptions of aging services, and all providers are invited to use the strategic findings and materials. For more information on the research and methodology, visit OpeningDoors.org. |