BY: FR. JOHN F. TUOHEY, PhD
The Oregon Tool for Emergency Preparedness
Fr. Tuohey is director, Providence Center for Health Care Ethics, Providence St. Vincent Medical Center, Portland, Ore.
In recent years, there has been a great deal of interest in emergency preparedness. This is especially true in light of concerns about a pandemic of the H5N1 virus, the "bird flu."* Ethical concerns include ensuring access to basic resources such as health care, and the duties of professionals to perform their task in the face of such events.1† Like other states, Oregon set out to establish an emergency preparedness plan to address these issues. A part of this planning included the establishment of a Medical Advisory Group (MAG), whose charge it was in part to describe the role ethics would play in decision making during a pandemic.§ In this article, I intend to describe why and how we in Oregon took an approach that differed in some ways from other plans.
* This concern is also fueled by memories of the SARS event in 2002, which had a 9.6 percent mortality rate worldwide; a continued increase in the number of West Nile cases each year; and the infrastructure failures resulting from events such as Hurricane Katrina in 2005.
† These expectations have been called into question by the behavior of some professionals after Katrina. For example, Anna Pou, MD, and two nurses were alleged to have euthanized four patients at Memorial Medical Center in New Orleans after three days without electricity or water. On July 25, 2007, a Louisiana grand jury refused to return an indictment against the three.
§ The Medical Advisory Group was established by the director of Oregon's Department of Health Services (DHS), Susan Allan, MD, JD, MPH, as an interdisciplinary group. The group's membership includes county health departments, health professional organizations, health insurors, local governments and tribal organizations, a researcher with expertise in mass communications, and an ethicist (the author of this article). In a DHS news release of February 2007, Allan said, "This group is helping establish guidelines and frameworks that will be instrumental for making complex decisions quickly in a time of crisis. Members of this group also may be asked to review proposed recommendations by the state during a crisis. Many of them represent professionals who will be at the forefront in carrying out those decisions. It is far better to build an understanding of what is at stake now, while we have time to discuss potential issues and identify the critical factors that would have to be balanced."
A Critique of the Ethical Basis of Preparedness Plans
It is beyond the scope of this article to provide a thorough analysis of the relevant literature, or of state and local emergency preparedness plans themselves. It can be said that such plans generally contain a reference to the ethical principles that should inform decision making during a pandemic. At the same time, there is a wide variety as to what principles are listed and how they are defined.
For example, Stand on Guard for Thee, the plan of the University of Toronto's Joint Centre for Bioethics, offers 15 different ethical values; 10 of which are described as "substantive" values (intended to inform decision making) and five are described as "procedural values" (to guide implementation).2 In contrast, the plan offered by the Minnesota Center for Health Care Ethics has only six ethical principles in its recommendations, of which four are really outcomes measures.3 These principles are intended to achieve the primary goal of "maximizing Minnesotans' chances of surviving," with a secondary goal of protecting "against the loss of any single generation when reasonable measures to do so are available" [emphasis added].¥
For all these plans' strengths, these two examples illustrate the common absence of a decision-making matrix in emergency preparedness plans. Stand on Guard for Thee does state that decisions should be reasonable, transparent, and inclusive—but these procedural values do not, by themselves, provide insight into what is "reasonable" in a particular situation or who should be included in the process. Because the Minnesota model appears more oriented toward outcomes, one cannot but wonder how it might be possible to demonstrate that protecting against the loss of any single generation might be "unreasonable."
To ensure consistency and accountability in responding to a catastrophic event like a pandemic, preparedness plans need more than a commitment to acting reasonably and with transparency in the pursuit of principles or outcomes. A commitment to acting ethically requires a definition of what it means in a crisis to act "reasonably." Moreover, if we are to avoid utilitarianism, we cannot make achieving objective outcomes a primary goal. The measure of acting ethically is the measure of the quality of the relationships in a particular situation.* The way to ensure quality relationships is through a defined and tested decision-making matrix that can demonstrate consistency and accountability in the honesty, reliability, and fairness with which decisions are made.† For that reason, the Oregon MAG decided that in its own preparedness plan ethical grounding would be assured through a decision-making matrix to be used in all aspects of the implementation of a preparedness response.
Beginning with Context
Decision making is always contextual. Decisions are made not in the abstract but, rather, in the context of concrete circumstances and situations. A decision-making matrix, therefore, must be adequate to the context in which it will be used. Changes in context can make a once robust and appropriate decision-making matrix feeble or dangerous.
For example, one challenge in a pandemic found in another context is the allocation of limited resources. One typical scenario is the allocation of vital organs to people needing organ transplants. Looking at this issue from her vast experience in the transplant field, Margaret Riggs Allee has articulated the ethical concerns that should inform allocation decisions in this context.4 Although Allee does not offer a decision-making matrix per se, her discussion of benefit, quality of life, duration of benefit, and the urgency of patient need are specific enough to allow a community to know that organs are being allocated in a way that is consistently honest, reliable, and fair.
Three years ago, the allocation question emerged in an entirely new context. On October 5, 2004, the Centers for Disease Control and Prevention (CDC) was notified by the Chiron Corporation that, because of contamination during production at the firm's plant in Great Britain, none of its influenza vaccine Fluvirin would be available for distribution in the United States. In this case, the context was not about allocating scarce resources among the people who needed them but, rather, about allocating resources to prevent the outbreak of an infectious disease. With a prophylaxis, the concern is not who gets the vaccine, but who should get the vaccine in order to reduce the risk of an outbreak among the general populace. Public health, not personal health, is the value at risk.
In this new context, Allee's considerations concerning who should receive an organ will not lead to honest, reliable, and fair decisions when applied to questions about who should receive the flu vaccine. The clinical difference between the vaccine's benefit for the elderly, on one hand, and the young, on the other, is insufficient to favor one age group over the other. The flu vaccine's prophylactic benefit is the same for all, regardless of age. If there is not enough for all those who will equally benefit clinically, but there is not enough of it to go around, by what criteria should the vaccine be allocated? Because the context here is public health, allocation decision-making criteria should be applied toward public health and public order concerns, such as vaccinating health care workers—in some cases before vaccinating at-risk patients.
The point here is that context is ethically significant. Emergency preparedness plans must have context-specific ethical approaches if they are to be applied consistently and held accountable as being honest, reliable, and fair.
Context for a Pandemic
The context within which decision making will likely be made for current emergency preparedness plans is that of an infectious agent, namely H5N1.* An infectious-agent context is one that refers to the presence of one or more pathogens, with various degrees of infectivity, in a community for an indefinite period of time. If infectivity is low, as it is with Norovirus, which causes gastrointestinal disorders, it is common to speak of an "outbreak" that directly and indirectly impacts a limited number of people.
Where there is an increase in infectivity or in the number of pathogens, a dramatic change in context results. As the infection rate from a pathogen moves beyond a localized area to involve the general population within a large geographic area, the term epidemic is applied. An example cited often of an epidemic is the "Spanish flu" that occurred in the United States between 1918 and 1920. The direct impact of that epidemic was the approximately 550,000 deaths attributed to it.† There was also a dramatic increase in the indirect impact. One study of the epidemic notes that it was "a large shock that had substantial macroeconomic effects," causing the post-World War I recession to extend into 1921.5 The study shows that states that sustained the highest direct impact of the epidemic, large numbers of deaths, also sustained the greatest indirect impact, such as business failures.
The fear with H5N1 is that it will be so highly infectious and spread so easily in today's global economy that there will be no natural geographic boundaries or geopolitical populations capable of isolating the virus. This is a pandemic. Other pathogens theoretically capable of causing a pandemic include Ebola virus, antibiotic resistant strains such as vancomycin-resistant staphylococcus aureus (VRSA), and sudden acute respiratory syndrome (SARS). The virulent nature of such a pathogen, and the ease with which it can spread due to global travel will cause its direct and indirect impacts to grow exponentially.
In the context of a pandemic, the values at risk are clearly astounding. Certainly among them is the value of the life and health of each affected person. But if H5N1 should develop a subtype that allows human-to-human transmission, the likely result in mortality, which will be far higher than that of the 1918-1920 flu pandemic, these will not be the only values at risk. With an event of that size, the values related to the social, psychological, political, economic spheres of life will also be put at extreme risk.§ Just as it is not possible to make decisions regarding the allocation of a prophylaxis according to the ethical considerations used in allocating kidneys, so this new pandemic context also requires a specific approach to decision making. The principles involved may be the same, but the context shapes the way those principles are brought to bear. This particular ethical discussion, with its epidemiological, social, political, psychological, and economic dimensions, cannot be adequately managed in a way that ensures consistency and accountability for honesty, reliability, and fairness unless it is done with a robust decision-making matrix within which ethical principles are applied specifically to the context.
Constructing an Ethical Decision-Making Matrix
For Oregon's MAG, constructing the matrix involved several full days and numerous meetings in which we sought a thorough understanding of the context of the course of a pandemic, defined by the World Health Organization as having inter-pandemic, pandemic alert, and pandemic stages6, in order to identify the key values most at risk in this context. These we came to describe as "social solidarity," "adherence to the standards of one's profession," and "justice." We then went on to describe the characteristics of those three values, a process that helped us clarify both what was at risk and the goods we hoped to pursue. Lastly, we sought to articulate the principles we believed were most relevant to those values. The same ethical principles can fit in different value spheres. Still, we felt that if our decision making was to be dynamic, flexible, and robust enough to respond in real time to predicted and unseen challenges, we needed to work with ethical principles within a specific value, not with principles "in general."
Most challenging perhaps was developing a diagram to illustrate the interchange between the different values, characteristics, and principles. What is key here is that the measure of the matrix's usefulness is the quality of the relationships in the community before, during, and after the pandemic event. If the community is inclined to agree that decisions are made consistently and with accountability, and that they reflect honesty, reliability, and fairness in accounting for the values of social solidarity, adherence to standards, and justice are brought to bear on the question at hand, then we will be acting ethically.
The three circles represent the three key values. The words in bold type indicate the value's characteristics, whereas those in italic type indicate the principles involved. Real-time decision making takes place within the overlapping areas of the matrix. A decision is never, for example, simply about clinical infectivity; such a decision might suggest that closing schools is a good idea. A decision on school closing must also account for the impact of that decision on social solidarity, as well as the justice obligation to the children who will not get a meal because they are not in school. A decision to keep open or close schools must be accountable to all facets of the matrix, even though the decision makers can ultimately choose only one. This is what distinguishes this model for preparedness from some others. The matrix makes decision making explicit, and therefore more readily consistent and accountable.
Describing the Decision-Making Matrix
As stated above, this matrix has three values: social solidarity, professionalism, and justice. Each value has its own characteristics and ethical principles most relevant to it.
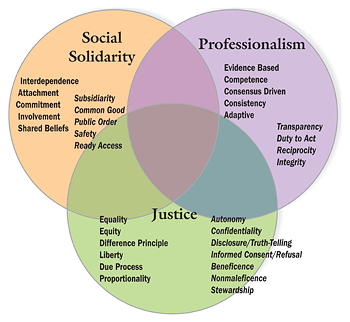
Social Solidarity
This value refers to the bonds that unify a community, as well as to the structures, such as schools and organizations, that support and maintain those bonds. Characteristics of social solidarity include a person's interdependence with and among others, attachment to or interest in others and their concerns, commitment to or support for the social structures that make social life possible, and personal involvement or engagement in the community's social life. Social solidarity is also characterized by shared beliefs and convictions, which contribute to the community's ability to achieve consensus on important issues. These characteristics will be at risk in a pandemic, and must be explicitly accounted for in all decisions.
- With this understanding of solidarity, the MAG identified those ethical principles most relevant to it. Among these were:
- Subsidiarity, the moral requirement that decisions be made at the most local level possible to promote the common good.
- The common good, those conditions such as health care, housing, and food, that each person and groups of persons need to live a full and productive life.
- Public order, the minimal structures needed to maintain a well-functioning society.
- Safety, the ability to move about and engage with others and in social life without fear of harm.
- Ready access to public services, so as to be able to receive health care and basic necessities such as food, shelter, clean water, with relative ease, or at least without bureaucratic obstacles.
These principles must explicitly inform ethical decision making, and do so in a dynamic interplay with other principles that reflect the other values.
Adherence to the Standards of One's Profession
This value, also referred to as " professionalism," although it truly denotes much more than "being a professional," refers to the importance of maintaining the competence, performance measures, and social contribution of groups, organizations, and professions upon which society depends. First responders and health care providers are obviously included in this category. But it also includes people whose work may be related more to a pandemic's indirect impact, such as sanitation engineers, who must maintain a level of professionalism if the overall effects of the pandemic are to be mitigated.
Professionalism is characterized by adherence to evidence-/experience-based standards that are, like the prognostic scales used in critical care,7 sufficiently verifiable or accepted by the professional community to be used in life and death situations or for limiting access to critical services. Competence, entailing both knowledge and skill sets, also characterizes this sphere, as does consensus-driven rather than individual-based protocols and practices. Consistency is that characteristic that speaks to the ability to perform according to professional standards on a regular and ongoing basis, especially in times of stress. Finally, this value is characterized by the ability to adapt competencies, standards, and practices to challenges. This value is also referred to as "alternative standards," meaning adaptive responses that nevertheless reflect the other characteristics needed to better achieve the ends of social solidarity and the demands of justice. It is important not to confuse "alternative standards" with a utilitarian "whatever-it-takes" approach to achieving some desired outcome.*
We suggest that the ethical principles most relevant in this sphere include:
- Duty to act, which refers to a person's obligation to fulfill his or her professional role without inducements.8
- Transparency, openness and accountability for how one performs his or her work.
- Reciprocity, the need to make available to the individuals and groups whose work supports the life of the community the things they need in order to perform those tasks, such as vaccinations for health care professionals as they seek to manage the risks inherent upon them in providing health care.†
- Integrity is important here, reflecting the need to act with honesty, reliability, and fairness, and a willingness to be held accountable to explain one's actions, especially when they depart from the consensus in one's field.
Justice
This value involves the fundamental commitment that individuals have toward one another, a commitment that makes social solidarity possible and drives professional decisions regarding the provision of services. Justice, as its biblical grounding in righteousness suggests, requires that we strive to ensure that "right relationships" exist between and among individuals and groups in society.
Justice is characterized by equality, with its avoidance of bias. To say people are equal, however, does not suggest that all have equal access or receive equal treatment. Equity is that characteristic of justice which understands access not as equal access by all groups but, rather, access by specific groups in light of a particular risk, disease or need in a particular situation.9 With Rawls, we see the difference principle as a characteristic of justice.10 This idea is similar to the Catholic social teaching related to a preferential option for the poor in that both concepts characterize justice as allowing society to show some preference to its most vulnerable members. In a strict sense, preference may be seen as related to the role a person plays, not to the person himself or herself, or even to the position that person holds.
Justice is also characterized by liberty, the individual and civil freedoms that are inherent in human dignity and necessary to the pursuit of the goods of social solidarity and professionalism. These are balanced by due process, in the event it becomes necessary, in light of social solidarity or professionalism, to impose limits on liberty.
Finally, justice is characterized by proportionality. Proportionality is what makes the "right" possible in "right relationships," in that it speaks of the due relationship between tensions that can arise between the liberty of the individual, the needs of society, and the standards of a profession. Proportionality is the measure, for example, that ensures the justice of either closing a school during a pandemic or keeping it open, as we balance the need of children in general to associate, the need of poor children in particular to have access to school for the lunch it provides them, and the community's epidemiological need to contain an infectious pathogen.
In the context of a pandemic, the ethical principles most relevant to justice are:
- Autonomy, with its respect for the individual and his or her claims and aspirations.
- Confidentiality and the protection of individual privacy.
- Disclosure and truth-telling, which ensure access to complete, accurate, and timely information, along with the related principle of informed consent/refusal.
- Beneficence and its obligation to provide for the good of others (not just in health care).
- Nonmaleficence and its prima facie but not absolute duty to protect oneself from harm, whether inflicted by another or by oneself.
- Stewardship, the right use of resources, which itself is a measure of proportionality in a given situation, is an ethical principle related to justice as well.
Decision Making and the Matrix
The Oregon MAG's goal was to articulate a firm ethical underpinning for its emergency preparedness plan. We wanted, first, to explicitly acknowledge the ethical significance of the pandemic context and, second, to provide a dynamic and robust matrix that could be applied in real time and in a way that offered consistency and accountability in the honesty, reliability, and fairness with which decisions are made.
In ways and in degrees that make it different from other crises, a pandemic places the values of social solidarity, adherence to professional standards, and justice at great risk. Each of these values has characteristics that help one understand what is at risk, as well as ethical principles that help one account for these values in difficult decisions.
The matrix described in this article is meant to capture those dynamics. The members of Oregon's MAG believe that if the decisions made during a pandemic are made according to our matrix, the decision makers will be able to say in the midst of tragic loss of life and the catastrophic loss of social, political, and economic opportunity that they acted justly, with professional competence, and preserved social solidarity.
NOTES
- See K. Morin, D. Higginson, and M. Goldrich, "Physician Obligation in Disaster Preparedness and Response," Cambridge Quarterly of Healthcare Ethics, vol. 15, no. 4, Fall 2006, pp. 417-421; in the same issue, see R. Rhodes, "Commentary: The Professional Obligation of Physicians in Times of Hazard and Need," pp. 424-428; and A. B. Zwi, P. M. McNeill, and N. J. Grove, "Commentary: Responding More Broadly and Ethically," pp 428-431. See also C. Ruderman, et al., "On Pandemics and the Duty to Care: Whose duty? Who cares?" British Medical Ethics, vol. 7, no. E5, April 20, 2006 (www.biomedcentral.com/1472-6939/7/5).
- University of Toronto Joint Centre for Bioethics Pandemic Influenza Working Group, Stand on Guard for Thee: Ethical Considerations in Preparedness Planning for Pandemic Influenza, Toronto, Ontario, Canada, 2005.
- The six principles include: "Contain and limit serious harm to Minnesota's public health," and "Reduce significant difference in influenza-related mortality." See "Allocating Pandemic Influenza Vaccines in Minnesota: Recommendations of the Pandemic Influenza Ethics Work Group," Minnesota Center for Health Care Ethics, Minneapolis, Minn., September 2006.
- Margaret Riggs Allee, "Ethical Considerations in the Allocation of Scarce Resources," Transplant Trends, vol. 6, no. 5, 2004, pp. 82-83.
- E. Brainerd and M.V. Siegler, "The Economic Effects of the 1918 Influenza Epidemic," Centre for Economic Policy Research Discussion Papers, Centre for Economic Policy Research, London, England, February 2002 (www.cepr.org/pubs/dps/DP3791.asp).
- See www.who.int.
- See F. L. Ferreira, et al., "Serial Evaluation of the SOFA Score to Predict Outcome in Critically Ill Patients," JAMA, vol. 286, no. 14, October 10, 2001, pp. 1,754-1,758.
- M. I. Meltzer, N. J. Cox, and K. Fukuda, "The Economic Impact of Pandemic Influenza in the United States: Priorities for Intervention," Emerging Infectious Diseases, vol. 5, no. 5, September-October 1999, pp. 659-671.
- See President's Commission for the Study of Ethical Problems in Medicine and Biomedical and Behavioral Research, Screening and Counseling for Genetic Conditions, Washington, DC, 1983, especially p. 84.
- John Rawls, A Theory of Justice, Harvard University Press, Cambridge, Mass., 1971.
Copyright © 2007 by the Catholic Health Association of the United States
For reprint permission, contact Betty Crosby or call (314) 253-3477.