BY: PAUL B. HOFMANN, Dr.P.H., FACHE
Valuable Feedback Guides California Hospital in Improvement Efforts
Dr. Hofmann is president, Hofmann Healthcare Group, Moraga, Calif.
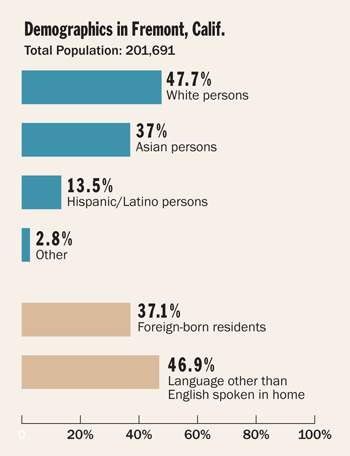
As hospitals devote continuing efforts to improving end-of-life care, more attention should focus on evaluating whether these efforts are actually effective. One community hospital, Washington Hospital in Fremont, Calif., offers an example of an evaluation process that may assist other hospitals across the county in assessing their end-of-life programs. The not-for-profit hospital, which is a 359-bed acute care facility in the San Francisco-Oakland metro area, serves an ethnically diverse community of about 202,000 people.
The hospital's end-of-life task force had been conducting monthly meetings to improve end-of-life care for patients and their families. Among other initiatives, the task force proposed changes in forms for standing orders, recommended policy and procedural refinements, sponsored medical staff educational programs, evaluated and promoted the completion of advance directives, created family conference guidelines and encouraged provision of more palliative care services. It also explored opportunities to increase the timeliness of patient referrals for hospice care and recommended several steps aimed at more effective end-of-life care. These steps principally influenced services in the intensive care unit, where monthly ethics rounds were conducted to identify and address ethical concerns and challenges related to recent and current cases.
Although it was generally felt that end-of-life care had improved at the hospital, no formal or informal effort had been made to obtain feedback from families of relatives who received end-of-life care. Recognizing the importance of conducting such a study with exceptional sensitivity, the task force decided a carefully designed project could make an important contribution to its mission.
Anticipating that a written survey would be likely to result in a relatively low response rate, the task force recommended brief phone interviews with patients' next of kin. The final proposal included a description of the project's purpose, findings from a literature review, the study's methodology and timeline, a list of the interview questions, and a draft letter from the hospital CEO to study participants. In addition, approvals were required by senior management, the bioethics committee, the institutional review board, the medical staff executive committee and the hospital's governing board.
Selection of Study Participants and Data Collection
Potential participants were identified as the people noted as next of kin on the patient's admission form. Criteria for selection included the following:
- The patient had a length of stay of at least three days in the intensive care unit.
- The patient's primary attending physician had no objection to a relative's participation in the study.
- The patient's death occurred between four and six weeks prior to a relative's receipt of the CEO's letter.
A form was designed to simplify the process of collecting information. For each case, the patient's medical record number, name, gender and dates of hospitalization were obtained. The name and relationship of the next of kin, as well as this person's address and phone number, were also documented. In addition to listing the patient's primary attending physician, another column was provided to confirm his or her approval.
Methodology
During a four- to six-week interval after a patient's death, the CEO sent a letter to the next of kin conveying her condolences and describing the hospital's ongoing commitment to take every possible step to improve end-of-life care for patients and their families. The CEO described the evaluation project and expressed her hope that the letter's recipient would be willing to take 15 to 20 minutes to speak with the hospital's representative. She emphasized participation was completely voluntary and that comments used would not be attributed to specific individuals. If the patient's next of kin declined participation, the person was asked to call her office or to inform the representative who placed the call.
Unless the letter's recipient informed the CEO's office that he or she preferred not to be contacted, the representative initiated a phone call within a week to 10 days of the letter's date, identified himself, and said he was calling regarding the CEO's recent letter. He verified that the letter had been received, conveyed his condolences and reiterated the hospital's strong commitment to improving patient care and support of family members. After confirming the time was convenient for a brief conversation, he re-emphasized that all comments would be kept confidential unless the family member specifically requested identifiable information be brought to the attention of others.
Interview Process
In recognition that the next of kin had experienced a recent painful loss, the hospital's representative asked only five questions. The person was requested to assess the hospital's care in three areas: 1) the hospital's overall care of the patient; 2) how well the patient's pain and symptoms were managed; and 3) the adequacy of the staff's communication with the patient and the patient's family.
Next the representative asked, "Do you have some specific comments regarding any particularly positive or negative aspects of your relative's experience or yours in the hospital?" Lastly, he said, "Do you have any suggestions to help improve the care and support of future patients and their family members?"
Because more than 100 different languages are spoken in the community, the representative was prepared to schedule a mutually convenient date and time to have a subsequent conversation should it be determined that translation assistance was needed. He also anticipated the possibility that the next of kin might prefer that a different family member respond to the questions.
Study Results
The original proposal suggested that at least 20 phone interviews be completed. None of the patients' physicians objected to the study, nor did the CEO receive any "do not contact" requests from next of kin. Eventually, 21 people were contacted and all agreed to answer the five study questions.
The median length of intensive care unit stay of patients whose next of kin were reached was six days, and the patient stays ranged from four to 98 days. Twelve patients were women; nine were men. Seventeen different physicians accounted for the 21 patients. The respondents were principally wives, husbands, sons and daughters, but the individuals also included a mother-in-law, a son-in-law, a daughter-in-law and an aunt.
Here's a summary of responses to the five questions:
1. Perceptions of the hospital's overall care of the patient
- Most relatives were very pleased with the care provided, and a number of verbatim comments were cited in the final report. For example, a patient's son said, "In general, the nursing care was so good, it is hard to describe."
- Two respondents were critical of the care. One relative said the physician came by only once a day and the patient seemed to have a different nurse each day. Another person reported, "The staff worked so fast and sometimes seemed to lack feeling."
2. Management of the patient's pain and symptoms
- Although none of the relatives had complaints about pain and symptom management, some indicated the patient was frequently unconscious, so it was difficult to know whether he or she was in pain or discomfort.
- Several respondents made very positive observations. One of the most appreciative individuals commented, "Although she had a stroke and didn't seem to know what was happening, the staff treated her as if she were conscious and always told her what they were doing."
3. Communication with the patient and the patient's family
- With a few exceptions, the relatives were complimentary about communication with the staff. A typical response was, "The family was always kept informed. All our questions were answered."
- Among the critical feedback was the following remark: "I was frustrated at times regarding the lack of information about physician coverage; my father's physician would be away for a day or two, and the family was not informed and had to ask who was covering in his absence." Another family member reported a problem related to abrupt notification of her mother-in-law's death. "The previous night, around 10:30 p.m., we spoke with a nurse and learned that her breathing was becoming very labored and more suctioning was required," she said. "We made sure to keep the phone close to our bed because we expected to receive a call indicating she had died, but missed several calls because one of our children turned off the ringer. Eventually, we did receive a call and were asked the question, 'What arrangements do you want us to make for the body?'"
4. Additional specific comments regarding positive or negative aspects of their relative's intensive care unit stay
- The vast majority of relatives either had favorable comments or no negative observations. A representative comment was, "She was in the best hands possible. I particularly appreciated the specialist, maybe a neurologist, who took time to explain why there was no hope of her recovery. Everyone was so professional and sympathetic."
- A few relatives shared some negative comments, such as, "The funeral home was in another county, and there was a long delay in obtaining the death certificate. It was very frustrating. We were told by the funeral home that the delay was due to being in a separate county and disagreement among physicians about who should sign the certificate." A patient's daughter said, "She had decided in advance that she did not want to have extraordinary measures like a breathing tube, but she had one anyway. Although it was not what she wanted, we were grateful to have a little more time with her."
5. Suggestions to help improve the care and support of future patients and their family members
- Family members appreciated the invitation to offer suggestions, but most did not have specific ideas. Many used the opportunity to reiterate their gratitude to the staff. For example, a patient's mother-in-law said, "I can't imagine how they could improve. The staff was like family. It was unbelievable." Several relatives praised physicians and nurses by name.
- Some relatives did have opinions for improving care and support. A patient's son mentioned, "It would have been helpful to have known the name of the physician and nurse with responsibility for her care each day." Another person commented, "Perhaps there should be more space for visitors. One patient had such a large extended family that there was a lot of congestion."
Observations
This informal study collected useful anecdotal information from relatives of patients who died after a minimum three-day length of stay in the intensive care unit. Although it was known that some relatives had not been totally satisfied with the care provided to their family member, no families were excluded from the study. Data on all consecutive intensive care unit patient deaths meeting the minimum length of stay criterion were collected.
Either at the beginning or end of each phone conversation, almost every relative expressed appreciation to the hospital for asking their opinions of the care provided to their loved one, including those who had criticisms. In only one case was the relative unable to communicate in English. In this instance, a son offered to translate questions and his mother's responses. During several interviews, it was evident the respondent's first language was not English, but the questions and answers still appeared to be clear.
Both the CEO's letter and the interviewer's introductory comments emphasized that the interviews were confidential, but there were three specific situations in which the respondent either requested or gave permission to be identified. In the first case, the wife of a patient expressed concern about the timeliness and accuracy of her husband's diagnosis. At the end of another conversation, the person wanted her name disclosed so that the staff would be aware of her gratitude for the care provided to her husband. In the third situation, a daughter was upset about the behavior of a staff member whom she described as angry and unprofessional. In each case, the family members said they would like to have their comments conveyed to appropriate individuals at the hospital, and this was done.
Lessons Learned
Following completion of the study, presentations of its findings and recommendations were made to the task force, the bioethics committee, the senior management, the governing board and the other groups identified in the original proposal. The recommendations were endorsed, including one to assign a staff member to conduct similar phone interviews of relatives periodically, perhaps annually, to demonstrate a continuing interest in obtaining constructive feedback and improving end-of-life care in the intensive care unit as well as elsewhere in the hospital. There was also agreement to initiate a comprehensive program to increase the proportion of employees, physicians, volunteers and board members who have prepared their advance directives.
This project was not designed as a conventional scientific study. Instead, it was an informal effort to collect anecdotal information from family members regarding their perceptions of end-of-life care in the intensive care unit. Although conducting the study did not require significant resources, the benefits were substantial. Among them, task force members felt the findings confirmed their past efforts had been worthwhile; family members were grateful to the hospital for its interest in obtaining their impressions; specific problems were identified and addressed; practical recommendations were developed for improving end-of-life care; and the results provided an opportunity to reinforce and celebrate the staff's dedication to providing compassionate and effective care.
At a time when every hospital remains committed to improving the quality and cost effectiveness of patient care, any relatively simple process that contributes to this objective should be strongly encouraged.
Criteria for Selecting Study Participants
Potential study participants were identified as the people noted next of kin on the patient's admission form. Criteria for selection included the following:
- The patient had a length of stay of at least three days in the intensive care unit.
- The patient's primary attending physician had no objection to a relative's participation in the study.
- The patient's death occurred between four and six weeks prior to a relative's receipt of the CEO's letter.
The participants were asked to assess the following areas:
- The hospital's overall care of the patient
- How well the patient's pain and symptoms were managed
- The adequacy of the staff's communication with the patient and the patient's family
Copyright © 2009 by the Catholic Health Association of the United States
For reprint permission, contact Betty Crosby or call (314) 253-3477.