BY: BRIAN YANOFCHICK, M.A., M.B.A.
Survey Analysis Suggests Approaches to Strengthen the Ministry
Mr. Yanofchick is senior director, mission and leadership development, Catholic Health Association, St. Louis.
About two years ago, the Catholic Health Association and the National Association of Catholic Chaplains partnered to begin work on a survey of pastoral care. This effort gave both organizations an opportunity to renew a vital partnership, to begin a preliminary effort to gain a better understanding of the state of pastoral care in Catholic health care, and to use this data to help our members chart a course for a renewed and strengthened pastoral care function. We understood that the survey results would serve to describe current status but not to set norms. The analysis offered in this article will show that there are very few areas in which the current state of pastoral care may be considered normative or acceptable and will indicate numerous opportunities for improvement.
This joint effort was unique and somewhat complicated in that the survey invited responses from members of CHA, which are institutions, and members of the National Association of Catholic Chaplains, who are individuals. Additionally, members of the National Association of Catholic Chaplains serve in diverse settings, including other-than-Catholic health care settings, academic institutions and forensic sites, such as prisons. This diversity needed to be accounted for in the questionnaire. After a concerted effort to design a questionnaire that would serve the needs of both groups, the survey was eventually posted online in January 2008. It was available for about three weeks for participants to complete.
In total, 738 CHA members and 2,200 members of the National Association of Catholic Chaplains were invited to complete the survey. We received 528 responses, representing 1,130 facilities. (The survey allowed places with a regional staffing model to answer for more than one facility or more than one type of facility.) These responses represented about 33 percent of CHA's membership and about 22 percent of the membership of the National Association of Catholic Chaplains. In the case of CHA members we encouraged mission leaders to ensure that the facility level director of pastoral care be designated to complete the survey.
Two-thirds of the overall responses represented people working in acute care settings, 9.9 percent in continuing care institutions and 7.4 percent on "additional campuses" related to acute care hospitals (such as outpatient surgery centers). The remaining 16.6 percent of the responses came from settings labeled as "other," most of which represented the diverse settings in which members of the National Association of Catholic Chaplains serve.
In addition to reporting on data from the survey, this report offers an analysis for a preferred future for pastoral care in the areas listed below, each one the subject of intense discussion in the health care field:
- Salary
- Characteristics of chaplains currently serving, including age, gender, religious affiliation and status (ordained, religious or lay)
- Use of volunteers on pastoral care staffs
- Certification of chaplains
- Academic preparation
- Staffing models
- Deployment of pastoral care staff
- Sacramental life in Catholic facilities
The survey confirms that serious effort must be undertaken to assure that pastoral care remains an effective service with well prepared and justly compensated staff in place. The broad range of services performed by chaplains is an indication of the potential that pastoral care offers to enhance the quality of the patient and staff experience in Catholic health care facilities. However, the need is evident for serious discussion to see that the potential becomes reality. This survey is shared in the hope that it will challenge the acceptance of mediocre models of pastoral care and spark energetic discussion about what is yet to be achieved.
Academic Preparation: High
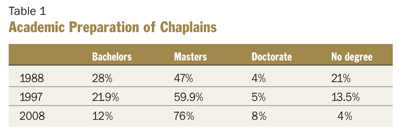
One of the most heartening developments during the past 20 years is the clear trend toward the professionalization of chaplaincy, demonstrated by a dramatic rise in the number of chaplains who have earned master and doctoral degrees. Table 1, prepared by David Lichter, D.Min., executive director of the National Association of Catholic Chaplains, shows the trend in academic preparation, based on the CHA's pastoral care surveys of 1988, 1997 and 2008.
As Table 1 indicates, the number of chaplains with a master's degree has increased by almost 30 percent in 20 years, and the number with a doctorate has doubled to 8 percent in the same period. Another bit of good news is that the number of chaplains with no degree at all has dwindled to just 4 percent, compared to 21 percent in 1988.
This achievement is due in no small part to more stringent certification requirements put in place by such organizations as the Association of Professional Chaplains and the National Association of Catholic Chaplains, which now list among their requirements for certification a master's degree, four units of Clinical Pastoral Education, and at least 1,600 hours of supervised training.1 It is heartening to note that our survey respondents report a certification rate of nearly 82 percent.
This good news, however, is countered by another reality: Many mission leaders and chaplains continue to report a lack of awareness and interest on the part of operational leaders regarding the professional requirements for certification as a chaplain. Too often chaplains hear from leaders that the only requirements for chaplains are that they be "nice" and offer pleasant and prayerful visits with sick patients. Such a false impression should be countered by the delineation of a preferred future that would include:
- More aggressive efforts on the part of mission leaders and directors of pastoral care to "tell the story" of chaplaincy's professional requirements so that operational leaders are as aware and respectful of these requirements as they are of requirements for other trained professionals in their institutions.
- A commitment on the part of pastoral care departments to require their staff to be certified, if not at the point of hire, then within some reasonable time frame afterward, as a condition of continued employment.
Support for the professional nature of chaplaincy needs to extend to access to the educational resources future chaplains will need for certification. Many chaplains in the past were priests and religious whose communities funded their educations. Today more lay people are functioning as chaplains. Lacking the financial support of religious communities, they must balance educational requirements and costs with family obligations and financial constraints.
In addition, access to Clinical Pastoral Education programs presents challenges. The cost of these programs and the challenge of accessing them, especially in rural settings, adds another hurdle to maintaining high professional standards. A low number of institutions — 27 percent — report having a Clinical Pastoral Education program on site.
These education-related issues should be addressed by defining a preferred future in which:
- Health systems design and implement detailed plans, including financing, to support access to programs required for chaplain certification, much as they do for other clinical positions that present hiring challenges.
- A concerted national effort is directed at increasing the number of qualified Clinical Pastoral Education supervisors so that quality programs can become more accessible, especially in rural areas.
Salaries: Low
Graph 1 shows the average salary levels reported for various categories of pastoral staff. Certified chaplains clearly enjoy a salary advantage. However, the average salary of $42,507 for a master's prepared, certified chaplain with 1,600 hours of supervised training compares unfavorably with salaries of other similarly prepared professionals, such as social workers. It would be inadequate for a health system or institution to judge its pay rates based on this average. Instead, an in-depth comparative study of the kind reported by Catholic Healthcare Partners in 2006 should be completed to determine a level of pay that honors the professional preparation of chaplains.2 A study of this kind would show the inadequacy of basing chaplain pay on "market studies" based only on what chaplains at other institutions are paid.
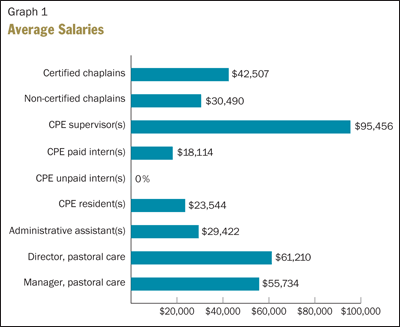
The reported average salary shown in Graph 1 calls into question whether well-prepared chaplains will be available in the future as the number of priests and religious continues to diminish. Lay individuals with family obligations will find it difficult to choose chaplaincy as a career, given its unfavorable ratio of pay to preparation required.
These salary data call for health systems to prepare for a preferred future in which:
- Compensation policies for pastoral care professionals offer salaries comparable to those in similar professions.
- Plans are in place to assure the continued presence of professionally prepared chaplains by developing support programs that promote chaplaincy as a career and aid in education for promising candidates.
An Aging Resource
The average age of chaplains responding to the survey is about 58. By comparison, the average age of members of the National Association of Catholic Chaplains is about 63, and other health systems report averages in the low 60s. Despite the slightly younger average age of survey respondents, concerns about the availability of chaplains in the near future are warranted. The survey indicates that almost one-third of chaplains are already near or past retirement age and more than one-third will follow during the next 10 years. In this context too, it is important to emphasize the need for aggressive efforts to promote chaplaincy as a career and to make it an attractive and viable career choice for lay persons with families. Consideration should be given, too, to targeting individuals who are searching for second career options. The experience and commitment of many active chaplains for whom this work is a second career contribute in a positive way to the quality of chaplaincy services.
Trends in Religious Affiliation
Table 2 by David Lichter of the National Association of Catholic Chaplains shows the trends in religious affiliation of pastoral staff. Two of the most noteworthy results from the survey are the decrease of Catholic clergy (to 58.6 percent from 87.2 percent in 1988) and the increase of other-than-Catholic Christian affiliations (to 38 percent from 12.3 percent in 1988).

This data represents a positive development. Pastoral care staffs have become more ecumenical and more closely mirror the religious affiliations of patients in our facilities. However, the availability of sacraments for Catholic patients and the development of a quality liturgical life within the institutions are becoming more and more of a challenge as fewer priests serve in hospital settings. Whereas in the past, pastoral care work was done principally by priests and vowed religious women, today, when the categories of Catholic lay persons and ordained other-than-Catholic Christian ministers are combined, they represent 52.6 percent of all pastoral care staff as shown in Graph 2.
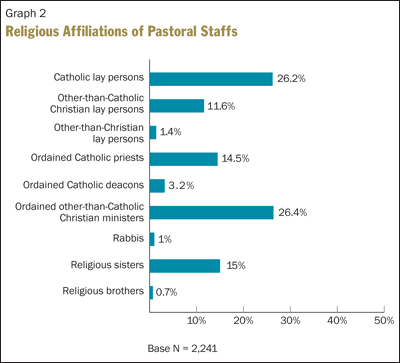
Although pastoral care departments at Catholic facilities are better prepared to meet the pastoral needs of a broader range of patients of other-than-Catholic traditions, it has become more difficult for them to address the sacramental requirements outlined in the Ethical and Religious Directives for Catholic Health Care Services.3 For example, survey respondents reported that at 68.4 percent of facilities, daily Mass is no longer offered. The shortage of available priests serving as chaplains has prompted some health care institutions to look for support from community Catholic clergy, who are already over-extended by the pastoral demands of large parishes and clusters of parishes. Moreover, there is growing evidence that the clergy shortage in the United States is being addressed through recruitment of foreign Catholic priests. Although these efforts may address the shortage in terms of simple numbers, great care must be given to assess the ability of foreign-born priests to establish fruitful pastoral relationships. Cultural and language differences sometimes make this difficult.
These changes in Catholic health care facilities challenge us to prepare for a preferred future in which:
- Catholic health care institutions work collaboratively with local dioceses, using the best and most creative resources of both institutions, to meet the pastoral and sacramental needs of Catholic patients. This includes efforts to strengthen lay ministry formation programs.
- Catholic and other-than-Catholic faith communities are engaged in a partnership with Catholic health care institutions to address the health needs of the members of their respective faith communities, not only when they enter a facility for treatment, but also in an ongoing way through programs focused on preventive care, spirituality and other areas that touch on holistic health.
Regarding pastoral care staffing, the survey gathered information about the percentages of staff in other categories such as paid full-time-equivalents and others. Graph 3 shows the reported distribution.
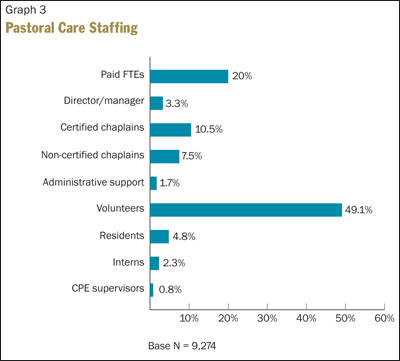
Post-survey discussions with various pastoral care leaders within the ministry revealed surprise with the high percentage of volunteers (49.1 percent). Some caveats should be noted, however. Many volunteers may provide services that do not require professional training. For example, there may be a large group of parish-based lay Eucharistic ministers who regularly bring communion to Catholic patients in a hospital. If they serve under the auspices of a pastoral care department, they would be counted as "volunteers" in this survey.
An important question that requires further study is the extent to which volunteers are used in pastoral care departments as a low-cost substitute for trained and certified chaplains. Unfortunately, the survey questions were not designed to give an answer.
Deployment of Pastoral Care Staff
The survey revealed a significant presence (39 percent) of regional staffing models, meaning those in which a director of pastoral care has responsibility for more than one facility. These may also include staffing methods in which chaplains are deployed to different facilities within a geographic area depending on patient census, rather than remaining dedicated to just one facility. The remaining 60.7 percent showed single-facility staffing models. Because previous surveys did not probe these arrangements, earlier comparisons are not available.
Forty-five percent of respondents deploy chaplains to more than one facility based on census and need. The remaining 55 percent of those dedicate their chaplains to one facility but have a regional director who oversees the program for multiple facilities. This indicates a significant effort to develop efficient and responsive staffing models.
The survey asked about staff deployment in direct patient service as well as in other institutional services, such as quality improvement, ethics and community education.
The results of the survey in this category were somewhat confusing. Graphs 4 and 5 illustrate the percentage of respondents whose chaplains are involved in the services indicated. It would be expected that participation in some service areas, such as end-of-life consultation, bereavement, etc., would be reported by close to 100 percent of respondents rather than by just 30 to 40 percent. It is possible that the format of the question encouraged under-reporting.
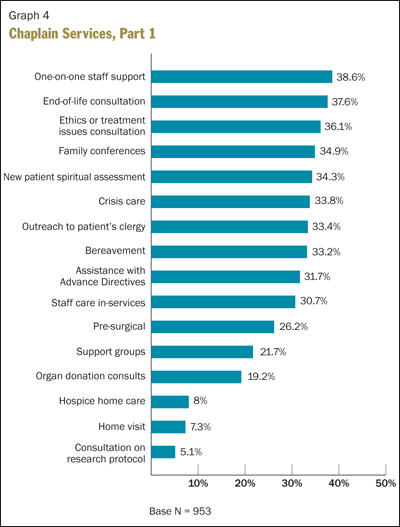
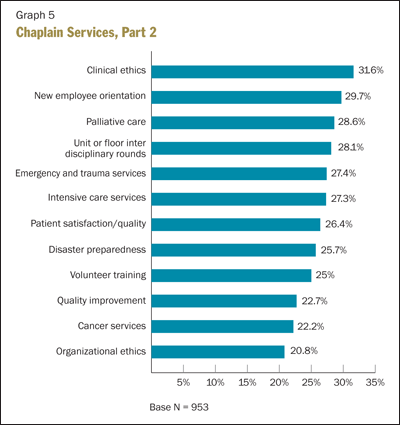
The good news revealed in this area of the survey is that chaplains contribute to a significant range of services within their institutions. The broad scope illustrates the versatility of skills and services chaplaincy offers. This information might prompt an institution to review the expectations of its pastoral care program. Are chaplains being used to their full potential? Does the current pastoral care staff possess the right mix of competencies to maximize its impact on the institution? Do current staffing levels allow for the fullest possible range of pastoral care services?
The fact that chaplains are clearly contributing in areas beyond the bedside raises questions about ongoing staff development. Do the current certification standards of institutions such as the National Association of Catholic Chaplains and the Association of Professional Chaplains call for this broader range of skills? While affirming the importance of direct patient care, should there be a developmental track for chaplains who are gifted as contributors to other organizational activities?
Another element of good news from the survey is that almost 94 percent of chaplains report making entries in patient charts. Given past resistance to allowing chaplains to enter appropriate information in patient records, this represents clear progress and a recognition that a chaplain's insights may contribute to the quality of patient care. It is fair to say that this is, and should remain, a standard of practice for pastoral care.
Regarding accessibility of chaplains, the survey showed good coverage. Eighty-eight percent of those who responded reported that chaplains are available on a 24/7 basis. Most facilities use a combination of on-site and on-call arrangements to assure accessibility to chaplains.
Reporting Structure
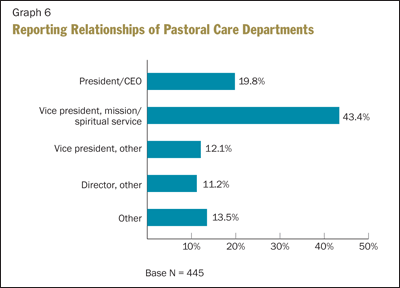
The survey asked participants to describe reporting relationships of their pastoral care departments. Graph 6 illustrates that most departments fall within the responsibility of the mission leader. However, a significant number of other reporting relationships are also indicated. The size and type of facility very likely influences this, particularly in rural acute care settings and smaller long-term care facilities where a mission leader may not be present.
Although pastoral care departments are characterized by a variety of internal reporting arrangements, Graph 7 indicates that a majority of departments are led by a director-level person.
It is interesting to note that, while almost 40 percent of respondents reported a regional staffing model, only 4.5 percent reported a direct relationship to a regional director of pastoral care. Again, the survey questions may not have allowed for a more detailed reporting of all the many variations in reporting arrangements. It may be, for example, that a facility level chaplain reports to a manager within a given facility rather than to a regional director.
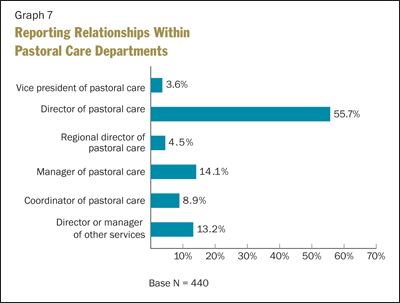
The fact that 13 percent of respondents report to a director of services other than pastoral care is likely explained again by respondents from rural settings and smaller long-term care facilities where this would be the norm.
Conclusion
The survey results have focused on issues that are generating the most concern and discussion among pastoral care professionals. CHA is pleased that these results, which have been shared and discussed with some member systems at their request, have already helped to influence their direction and strategies. It is our hope that this survey will be a catalyst for other systems to create a new vision for their pastoral care service. It is interesting that in the closing paragraph of the introduction to Part Two of the Ethical and Religious Directives for Catholic Health Care Services, the bishops acknowledge that the directives cannot address every need and situation pastoral care professionals will encounter. As a result, they see the need for the "creative response" of pastoral caregivers to the many needs of those they serve. A similarly creative response is required in the ongoing dialogue about the role of pastoral care and the resources required to assure its excellence in Catholic health care settings.
NOTES
- The complete lists of chaplaincy certification requirements for the National Association of Catholic Chaplains and the Association of Professional Chaplains are available online at www.nacc.org and www.professionalchaplains.org, respectively. The requirements vary by organization. The Association of Clinical Pastoral Education provides educational credits designed specifically for spiritual caregivers of all faiths.
- Jean Lambert and Michael Connelly, "Revitalizing Spiritual Care," Health Progress 88, no. 4 (July-August 2007): 36-40.
- For example, Directive no. 12 reads as follows: "For Catholic patients or residents, provision for the sacraments is an especially important part of Catholic health care ministry. Every effort should be made to have priests assigned to hospitals and health care institutions to celebrate the Eucharist and provide the sacraments to patients and staff."
For More Information
Learn more about the latest in pastoral care by visiting www.chausa.org/pastoralcare. Member access is required to visit this webpage. Send your comments about this article to Brian Yanofchick at [email protected].
Copyright © 2009 by the Catholic Health Association of the United States
For reprint permission, contact Betty Crosby or call (314) 253-3477.