BY: WILLIAM VICTOR TROGDON, M.Div., BCC
Helping Operational Leaders Make Good Funding Decisions Requires Candid and Ongoing Communication
Mr. Trogdon is director, pastoral care, St. Mary's Health System, Evansville, Ind.
Outside a winter storm has developed into a state of emergency for the tri-state area, leaving hundreds of thousands of people without electricity in their homes. Around the world an economic crisis has become one of the focal points for the new presidential administration. Meanwhile, inside St. Mary's Medical Center, Timothy Flesch, president and CEO of St. Mary's Health System, agreed to speak to me about a problem seemingly less dramatic but of critical importance to Catholic health care. The topic: pastoral care.
Our conversation began with my providing information related to the unsuccessful efforts to establish benchmarks (defined as standards of practice across similar professional groups) for this area of the Catholic health ministry. Then I posed a question to Flesch: "What do you as an operational leader look for when making decisions about allocating resources for pastoral care?"
Flesch answered with a smile, "Normally, I would ask you to show me your benchmarks. But from what you are telling me, there aren't any."
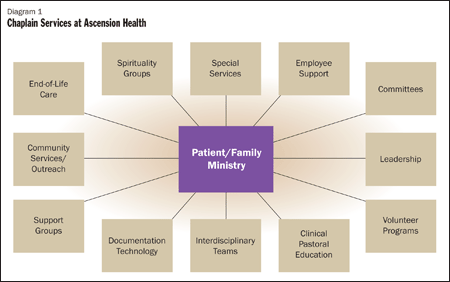
Although benchmarks for chaplains have proven elusive, I suggested that we review a diagram developed by an Ascension Health spiritual care task force. (St. Mary's is a member of Ascension Health.) The diagram, which provides an example of the types of pastoral care services being provided in the health system, could help us focus on areas in which we might measure for value of services. (See representation of diagram.)
Just how difficult is it to establish benchmarks for pastoral care services? Carol Schmidt, vice president of operational excellence for Ascension Health, discovered the lack of national benchmarks and data on pastoral care departments in health care as she led the system's financial performance improvement initiative. One of the problems is the assortment of ways in which pastoral care services are provided across the nation, as well as within the 76 acute care hospitals operated by Ascension Health.
Schmidt noted, "Providing pastoral care is integral to who we are at Ascension Health and it is not a matter of whether we continue to support these services. Rather [it is a matter of] the ability to provide information to help local leaders determine the correct number and appropriate skill set for persons performing this ministry." She added, "I have come to appreciate the many ways chaplains contribute to the overall ministry and the many things they do in a given day. A chaplain's duties can go unnoticed because organizational leaders may be unaware of all that they do within the organization. We must be able to fully articulate the many ways chaplains support holistic healing."
At Ascension Health, as for other health systems, it is worth asking why we provide pastoral care to patients. The Ethical and Religious Directives for Catholic Health Care Services clearly identify reasons why holistic care of patients, (physical, psychological, social and spiritual) is essential for the care of the sick and vulnerable. For example, "Catholic health care has the responsibility to treat those in need in a way that respects the human dignity and eternal destiny of all. The words of Christ have provided inspiration for Catholic health care: 'I was ill and you cared for me (Mt 25:36).'"1 Other directives identify specific ministries pastoral care services are responsible for along with the direction for the "appropriate professional preparations" for those who serve the pastoral care ministry.2 Another reason we provide pastoral care is to meet the standards outlined by The Joint Commission, which accredits and certifies more than 16,000 health care organizations and programs across the United States.3
Surveys conducted in 1994, 2006 and 2008 by Rev. Dean V. Marek, director of chaplaincy at Mayo Clinic Rochester (Minn.), demonstrated what patients expect from chaplains.4 General responses included the following: To remind me of God's care, to pray or read Scripture, to be with me at times of anxiety and uncertainty, to listen to me, to meet my needs for ritual, and to counsel me.
Responses from patients who identified themselves as Catholic were similar, but added the following: offer counsel related to moral and ethical decisions; provide a visit even though I haven't requested one.
Regarding the 2008 survey, Katherine M. Piderman, Ph.D., who works with Rev. Marek, noted that the survey is ongoing. "We will soon conclude a second phase of our patients' expectation survey with inpatients recently discharged from Mayo Clinic Hospitals in Phoenix, Ariz., and Jacksonville, Fla.," she said. "We plan to compare the data collected with that previously collected in Rochester to determine if there are any differences based on location and/or ethnicity. This will provide us with data from two additional geographical areas with different demographics to use in comparison with existing data from the parent study and add to our understanding of what patients expect from hospital chaplains."
Although such input it obviously useful, leaders want more. Even where it is clear that system leaders and patients value the role of pastoral care, the question remains: How do we assist operational leaders to make the best decisions related to allocation of funds to support pastoral care?
The CEO's Perspective
My conversation with our president and CEO proved to be fruitful in helping identify how to support operational leaders as they continually address ways to improve financial performance throughout Ascension Health. Flesch affirmed it is essential to engage in an ongoing dialogue and to recognize that the conversation will always be in flux. As in any other department or service within our health care ministry, pastoral care focus and needs continually change and the resources must be closely managed in order to maintain the welfare of the whole ministry.
As a CEO, Flesch encourages pastoral care leaders to continue to find ways to measure the values of these services. Measuring productivity and cost per unit of service can be useful for identifying productivity of individuals and perhaps for determining when and where to allocate full-time equivalent positions. Flesch said identifying the cost per unit of service is only one part of the economic equation operational leaders would want to evaluate. Additional questions operational leaders may need to consider include:
- What is the return on investment?
- Why is it so hard to establish benchmarks when other fields have done so?
- How does one understand "demand vs. constraint?"
- Is the marginal cost equal to the marginal value?
Pastoral care leaders, many of whom are still learning how to use financial tools and to articulate the value of chaplaincy in organizational terms, have much to learn from others in Catholic health care. As one example, Flesch explained the difference between "demand vs. constraint" by noting that people who have health insurance are sheltered from the cost (i.e. constraint) of medical procedures they believe they need, which results in increased demand. If required to pay more of the cost, they might be more discerning about the procedures they regard as the most needed and when to seek them. On the flip side, given excessive constraints, patients might delay the care they need, neglect preventive medicine and, in the long run, use more resources than would have been needed had they sought care sooner.
How then does "demand vs. constraint" relate to pastoral care services? Although we would not want to turn away patients, visitors, associates or physicians requesting our services, are there ways in which we create demand without clearly identifying the cost? One example might be a now virtually obsolete practice of asking a chaplain to feed a patient at meal time when family is not present and the nursing staff is busy. Here, compliance resulted in demand, and though it has been argued that this was an appropriate utilization of a chaplain's time, it is fair to ask whether, in today's health care setting, this is good stewardship of resources. Would/should nursing services be willing to provide additional full-time equivalents for pastoral care to provide such a service? Much work needs to be done so all can understand the purpose of the services pastoral care provides and associated cost of the ministry, given that no direct charge for pastoral care services is billed to the patient or to a service line.
Over time, expectations of a chaplain's ministry have broadened to include staff support, organizational development and community outreach. Though chaplains have been trained to understand this expanded role, leaders are still learning the variety of ways in which chaplains support holistic care through the ministry. The chaplaincy services diagram developed by the Ascension Health spiritual care task force depicts the many ways pastoral care supports healing. Chaplains contribute throughout the ministry, whether it is providing patient and family care, staff support, end-of-life care, or working with spirituality groups, interdisciplinary teams and volunteer programs.
Educating Colleagues
At St. Mary's Health System, one component of ensuring that pastoral care services are valued is educating associates about what chaplains do. For example, managers need to understand that chaplains provide pastoral care for all health care professionals, including physicians and those who work in ancillary and clinical services. One of a chaplain's functions is to minister to direct caregivers, supporting them as they provide spiritual and emotional care to patients and families. This type of support includes one-on-one interaction where a chaplain can help an associate process feelings, frustrations and grief. Both chaplains and managers need to understand the purpose of staff support so that important spiritual assistance will not be misconstrued as unproductive socializing. (Usually, such misunderstandings reflect an issue with timing or unclear boundaries and can be resolved through open and honest dialogue.)
Professional chaplains are also needed to supervise persons who desire to serve the ministry as volunteers. For example, St. Mary's Health System utilizes at least 50 volunteers to provide Communion to Catholic patients. These volunteers are a valuable asset and help free board certified chaplains to provide the advanced pastoral care services for which they have been trained. These services, integrated with work of the entire patient care team during a patient's hospital stay, might include doing pastoral care assessments and developing care plans; counseling patients and families about advance directives; offering grief counseling related to a patient's illness or death; and guidance and support related to ethical issues, including end-of-life care and organ donation.
In addition to the volunteers, our pastoral care team includes a priest who celebrates Mass six days a week, and a harpist, both under contractual arrangement; an administrative assistant; and seven waiting room receptionists. Although the skill sets are different, we work together as a team to minister to those we serve. We do so in a cost-responsible way, which includes making sure people have skill sets appropriate to the services they provide, thus maintaining a good return on the hospital's investment in resources allotted to pastoral care.
Clearly, in order for pastoral care services to effectively integrate with the work of other health care professionals, it is important that the chaplain be formally trained and abide by accountabilities and expectations established as common foundations for professional pastoral care providers and educators.5 Health care leaders may be unaware of the extent of training needed to become a certified chaplain. Today, certified chaplains must have a master's degree and four units of Clinical Pastoral Education, which translates into at least 1,600 hours of supervised, hands-on training. In the certification process, chaplains are required to demonstrate mastery of certain skills.
Attempting to Establish Benchmarks
During the past few years, St. Mary's has worked to create best practices and measure outcomes, but, as Flesch noted, more information is needed to complete the equation. Operational leaders are accustomed to making decisions related to benchmarks, which are used to determine staffing levels in areas such as pharmacy, nursing and social work. When Flesch thinks about potential benchmarks for chaplaincy, one area he mentions is staffing needs as they relate to discharge procedures, inpatient days, palliative care protocols and hospital deaths. These benchmarks would be compared with data from similar medical facilities.
Since national benchmarks don't exist in pastoral care, and establishing such benchmarks continues to be elusive, the focus at St. Mary's has shifted to a "best practice" model throughout the local system. One reason for this change is that the need for pastoral care services is determined less by overall patient census and more by individual patient needs.
Final Thoughts
Catholic health care ministries will benefit when those who serve within them clearly understand the challenges their operational leaders face and the needs of their communities. The mutual trust and support that derives from such understanding will provide a strong foundation for developing best practices for pastoral care services. Relationships between operational leaders and pastoral care leaders will foster creativity in finding ways to measure value and cost of services, manage productivity and correlate resources with patient satisfaction. At St. Mary's we will continue to devise new ways to gather data. We remain dedicated to supporting the many other departments and persons who are members of St. Mary's Health System and Ascension Health and will continue to find better ways to do so and to track the impact of our services.
The healing ministry of Jesus allows God to minister to others through each of us, and investing resources wisely allows us to continue to touch others with God's love. Although other professionals in the hospital setting help with responding to spiritual needs, it is the chaplain who is trained to respond to advanced pastoral care needs. Professional chaplains are formally trained in theology, behavioral sciences, spirituality, sociology, ethics and counseling and hired for this ministry and service. They are qualified to meet these needs, but also to empower other members of the health care team to care for the spiritual and emotional needs of patients.
My conversation with our president and CEO provided an opportunity to discuss the challenge operational leaders face, given limited resources, in allocating funds for pastoral care. As a professional chaplain who has served in health care, hospice and the military for the past 28 years, I know the tremendous good chaplaincy can do in providing services for God's people. I serve on various committees and task forces to advance and support pastoral care services and chaplaincy. Something I bring to all these roles is my understanding of and appreciation for systems, their well-being and the part I and others play in making a positive or negative contribution to the systems of which we are a part. It reminds me that each party at the table has to be open to discussion and learning.
Pastoral care is one concrete expression of the mission at St. Mary's Health System. We recognize it as a vital part of healing and a complement to other services that are provided, but there will always be competing demands within the ministry. The need for ongoing and open conversations will continue well into the future.
NOTES
- United States Conference of Catholic Bishops, Ethical and Religious Directives for Catholic Health Care Services, 4th Edition (Washington, D.C.: USCCB, July 2001), Part Two, www.usccb.org.
- USCCB, Directives Nos. 10-22.
- Read the standards at the Joint Commission website at www.jointcommission.org.
- Katherine Piderman et al., "Patients' Expectations of Hospital Chaplains," Mayo Clinic Proceedings 83, no. 1 (January 2008): 58-65.
- These common foundations were agreed upon by the following collaborating groups: Association of Professional Chaplains; American Association of Pastoral Counselors; Association of Clinical Pastoral Education; National Association of Catholic Chaplains; Association of Jewish Chaplains; and the Canadian Association of Pastoral Practice and Education. For more information, contact Mary Kendrick Moore, Association of Professional Chaplains, [email protected] or David Lewellen, National Association of Catholic Chaplains, [email protected].
Copyright © 2009 by the Catholic Health Association of the United States
For reprint permission, contact Betty Crosby or call (314) 253-3477.