BY: MELINDA LEE, MD, and SARAH BOOTH
Dr. Lee is medical director and Ms. Booth is social work program manager, Providence ElderPlace, Portland, Ore.
The Program of All-Inclusive Care for the Elderly (PACE) is a unique model of care delivery that provides excellent geriatric and palliative care for our most vulnerable older citizens. 1-4 The PACE model is one of the options available to Catholic health systems seeking to improve care for people in the final stages of their lives. Providence ElderPlace is a PACE organization in Portland, Ore., that has developed a unique approach to end-of-life care for enrolled participants, called the Supportive Care Program. By collaborating with caregivers in a variety of long-term care settings, ElderPlace has been able to provide palliative care for the majority of ElderPlace participants in their residences until they die.
In 1997, a retrospective review of end-of-life care in ElderPlace over a three-year period revealed that interdisciplinary care teams recognized that a participant was in a state of decline or in the process of dying in more than 90 percent of cases. Only 9 percent of deaths were unexpected. Based on these findings and a review of the literature in 2002, ElderPlace implemented the Supportive Care Program, a palliative care model that recognizes distinct phases of decline and emphasizes individualized end-of-life care planning.
The Supportive Care Program
The Supportive Care Program recognizes three phases of decline that precede death for most older people. Phase I is characterized by functional decline that persists despite careful evaluation and interventions aimed at reversing it. Phase II is defined as organ system failure, dementia or failure to thrive according to hospice guidelines for predicting the final six months of life. Phase III is active dying. The goals of a supportive care plan are to ease physical and emotional symptoms, support function and autonomy, support spiritual needs, eliminate inappropriate medical interventions and support family and caregivers in caring and bereavement. Each supportive care plan varies with the participant's preferences, cognition, function and underlying conditions. The basis for the decision, the criteria, and the care plan are all documented in the electronic medical record and "Supportive Care Phase I, II, or III" is placed at the top ofthe medical problem list.
The same care team, including primary care provider (PCP), primary nurse, community care nurse, social worker and chaplain continue to care for the participant after the shift to supportive care, and the participant continues to live in his or her residential setting as long as needs can be met there. ElderPlace staff have worked closely with contracted residential care and assisted living providers, as well as adult foster caregivers to enhance their skill and comfort with continuing to care for people through the dying process. Training on end-of-life care for ElderPlace staff is also ongoing. A Supportive Care Steering Committee oversees the program and is charged with initiating improvements when needed.
Monitoring Success
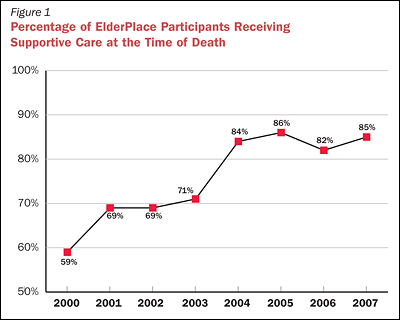
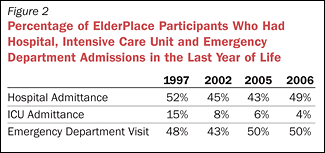
ElderPlace has monitored several outcomes to evaluate whether implementing the Supportive Care Program has improved end-of-life care for participants. For example, the percentage of participants who have a supportive care plan in place at the time of death has increased from 59 percent prior to 2002 to 85 percent in 2007 (Figure 1). During the same period, hospital and intensive care unit admissions among participants in the last year of life have also declined (Figure 2) . The percentage of participants who have been able to die in their place of residence has increased since the Supportive Care Program was implemented, and has remained above 70 percent for four years. In 2007, 45 percent of ElderPlace participants died in their adult foster homes, 22 percent died in their residential care or assisted living facilities, and 4 percent died in their family homes, while 7 percent died in the hospital and 22 percent died in nursing facilities. A 2005 ElderPlace survey revealed a high degree of satisfaction with end-of-life care for loved ones among surviving family members. Ninety-seven percent of respondents agreed that the quality of care during the dying process was very good, 96 percent agreed that ElderPlace staff treated them with respect, and 93 percent agreed that the participant's goals and preferenceswere supported (Figure 3).

Collaboration with Long-Term Care Providers
Much of the success of the ElderPlace Supportive Care Program is based on collaborative relationships with community-based caregivers in licensed residential settings. The federal government has authorized payment for resident care to several types of residential settings under the Medicaid Home and Community Based Waiver Program in Oregon. These housing options include adult foster homes, relative foster homes, residential care facilities, assisted livingfacilities and assistance in a resident's own home.
Adult foster homes are a unique alternative to nursing facility care and are an important and valued resource to Providence ElderPlace . There are approximately 650 adult foster homes in Multnomah County, the ElderPlace service area. The adult foster home setting is licensed to care for up to five residents in a private home-like residence. There is generally a live-in caregiver/manager. The advantages to the foster home setting are the close bond that can develop between the participant and caregiver and the individualized care that can be provided by a consistent caregiver. The small scale makes it possible to tailor the day-to-day care experience to enhance the participant's ability to make choices. Thirty percent of caregivers in adult foster homes are racially or ethnically diverse. ElderPlace is often able to facilitate placing a participant in a home with a provider of the same ethnic group. This can enhance the placement immeasurably by providing common language, food types and cultural values in the foster home.
The ElderPlace participant's family often develops a close and trusting relationship with the foster home provider. This may be especially true as the participant approaches the end of life and the family is looking to the caregiver for support and assurance that its family member is receiving the highest quality care.
In an attempt to encourage foster caregivers to continue to care for ElderPlace participants through the dying process and to support them in their caregiving , ElderPlace began a series of educational workshops. These training sessions allow caregivers to examine their own attitudes and beliefs about death and dying and to appreciate how their own values about end-of-life preferences may differ from those of the participants they are caring for. Some training sessions have focused on recognizing issues around dignity for the participant and how increased dependency and loss of control may be affecting him or her. Caregivers are encouraged to allow time and space to listen and provide time for the participant to reflect on the experiences of each day.
Members of the ElderPlace interdisciplinary team remain actively involved with the participant, family and caregiver through the end of the participant's life. The community care nurse has a particularly critical partnership with the adult foster caregiver. The nurse meets with the caregiver initially when a participant is placed in a home and when there are significant changes to the care plan. When a participant chooses to shift his or her care goals to supportive care, the community care nurse makes a visit to review the Physician Orders for Life-Sustaining Treatment and changes to the care plan with the caregiver. The nurse makes regular visits to assess any symptoms of distress or pain and to teach the caregivers how to monitor symptoms and when it's appropriate to call ElderPlace with questions or concerns. The community care nurses get to know caregivers and recognize their strengths or areas where they may need more preparation or education.
The primary care team members serve as guides to the participant and family through this last stage of the participant's life. The PCP, chaplain and social worker are in daily communication with the community care nurse regarding the participant's condition and how the participant, family and caregiver are coping. Both the chaplain and the social worker are available to the participant and family for emotional and spiritual needs. They suggest things that family members and caregivers can do to help the participant feel calm and peaceful. The chaplain and PCP make bedside visits. After the participant's death, the PCP, nurse, social worker and chaplain each contact the family to offer condolences and bereavement support.
Care Extends Beyond Death
The community care nurse makes a home visit after the participant's death to allow the caregivers the opportunity to talk and process through the death. The caregiver, the participant's family, other ElderPlace participants and staff are invited to attend a memorial service that is coordinated by the chaplain and held at the ElderPlacecenter that the participant had attended.
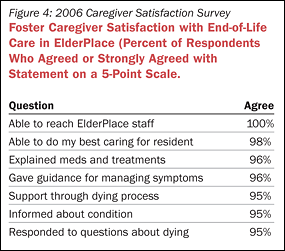
In 2006, ElderPlace completed an adult foster caregiver satisfaction survey in order to learn how caregivers felt about their experiences caring for participants who died in their homes. Survey results indicate that caregivers feel they are able to do their best caring for participants through the dying process, are able to reach ElderPlace staff when they need support, and that ElderPlace staff explain treatments and respond to their questions about the dying process (Figure 4).
ElderPlace also has partnerships with many residential care and assisted living facilities. These established professional relationships with staff at these facilities have made it possible for many participants to remain in their residential settings through the dying process. Similar to their roles providing palliative care in adult foster homes, ElderPlace team members provide guidance, mentoring and preparation for what to expect through the participant's end of life process. In these settings, family members often find that they are able to provide a reassuring presence to their loved one while having the comfort and knowledge that the participant is receiving the best care in the setting of his or her choice.
Conclusions
PACE provides comprehensive, coordinated care by the same primary care team in all settings. Integration of financing and care delivery allows flexibility in care planning and removes obstacles to assembling needed services. The PACE model, as exemplified by Providence ElderPlace's Supportive Care Program, can facilitate desirable outcomes for participants in the final stages of life. There is a strong emphasis on advance care planning and use of the POLST to implement participants' preferences. By defining criteria for Supportive Care Phase I, as mentioned above, ElderPlace teams have been able to identify irreversible decline early and develop person-centered supportive care plans. More than 85 percent of participants who die in ElderPlace are receiving supportive care at the time of death. Families and caregivers are involved in the supportive care process and are highly satisfied with the quality of care. ICU utilization in the final year of life has decreased and home deaths have increasedsince the Supportive Care Program was implemented.
Most importantly, over 70 percent of ElderPlace participants are able to remain in their residences until they die. Strong partnerships with caregivers in adult foster homes, residential care facilities and assisted living facilities are instrumental in providing high quality palliative care in this model.
NOTES
- T. Bodenheimer , "Long-Term Care for Frail Elderly People: The On   Model," New England Journal of Medicine 341 (1999):1324-1328.
- C. Eng, "Future Considerations for Improving End-of-Life Care for Older Persons: Program of All-Inclusive Care for the Elderly (PACE)," Journal of Palliative Medicine 5, no. 2 (2002): 305-309.
- U.S. Government Accountability Office, "End-of-Life Care: Key Components Provided by Programs in Four States," (December 2007), www.gao.gov/new.items/0866.pdf
- M.A. Lee et al., "Physician Orders for Life-Sustaining Treatment (POLST): Outcomes in a PACE Program," Journal of the American Geriatric Society 48 (2000): 1-6.
PACE AT PROVIDENCE ELDERPLACE
PACE grew out of a visionary experiment in care delivery for frail elders at On Lok in San Francisco in 1971. Along with Providence ElderPlace , there are 41 PACE organizations across the United States exist. PACE integrates care delivery and financing to enhance quality of life, autonomy and dignity for frail elders and to enable them to live in the community as long as medically and socially feasible. PACE serves individuals age 55 and older, certified by their state to need nursing home care, able to live safely in the community at the time of enrollment, and living in a PACE service area. The PACE program receives monthly capitated payments from Medicare and Medicaid to provide comprehensive, interdisciplinary care. This includes medical, nursing, rehabilitation, nutrition services, medications, medical equipment, transportation, day center visits, activities and personal care. The same PACE care team provides care in all settings across the continuum of care, which includes PACE centers (combined adult day centers and clinics), the participant's residence, the hospital and nursing home.
Providence Health System founded ElderPlace in 1991 with support from the Robert Wood Johnson Foundation. Providence ElderPlace currently serves 720 participants and operates five health and social service centers in Portland. Interdisciplinary teams include physicians, nurse practitioners, clinic and home care nurses, social workers, physical, occupational and speech therapists, life enrichment coordinators, chaplains, clinical pharmacists, drivers, certified nursing assistants and homecare aides.
ElderPlace participants range in age from 55 to 100, with a mean age of 80 years. Seventy-five percent are women, 16 percent are married and 89 percent are white. African-Americans comprise 8 percent of the participants, reflecting Portland demographics. The average ElderPlace participant has 14 diagnoses (including geriatric syndromes like falls and incontinence) and takes 13 medications, including over-the-counter products. Most participants need assistance with one or more activities of daily living (ADLs), such as bathing (85 percent), dressing (67 percent), and feeding (39 percent). More than half of enrolled participants (52 percent) live in residential care or assisted living facilities. Another 43 percent live in adult foster homes, and 4 percent live in their homes alone or with others. Nursing home stays are usually short for PACE participants. Currently, 1 percent of ElderPlace participants reside in nursing homes long term.
ElderPlace provides comprehensive health services and personal care for most participants until they die, providing a seamless transition to end-of-life care for about 125 participants per year. The disenrollment rate for reasons other than death is less than 1 percent. In 1997, ElderPlace began to monitor advance care planning as a quality indicator and made it a priority to facilitate completion of durable power of attorney for health care by participants who are capable of appointing a proxy. Currently, 80 percent of ElderPlace participants with this capacity have appointed a health care proxy.
In 1995, Oregon developed the Physician Orders for Life-Sustaining Treatment (POLST), a portable doctor's order sheet on bright pink card stock that specifies whether CPR, endotracheal intubation, hospital transport, IV fluid, feeding tube or antibiotics are indicated in an emergency.* A valid POLST form signed by a doctor is honored by Oregon emergency medical personnel, ensuring that a person's treatment preferences will be carried out in an emergency. Since 1997, ElderPlace has made it a priority to discuss preferences and complete a POLST for willing participants within months of enrollment. Since then, the rate of completed POLST forms in ElderPlace has remained at 98 percent. A large majority of ElderPlace participants (85 percent) prefer not to have CPR. While 15 percent want a comfort care approach and no hospitalization, 17 percent would want full hospital interventions, including ICU, if appropriate. Fifty-five percent of participants indicate they would want a trial period of tube feeding if indicated. The original POLST form is kept with the participant at all times, and a copy is kept in the electronic medical record, making it accessible to the participant's physician or the physician on call to guide decisions.
* M.A. Lee et al., "Physician Orders for Life-Sustaining Treatment (POLST): Outcomes in a PACE Program," Journal of the American Geriatric Society 48 (2000): 1-6.
For more information, contact Providence ElderPlace at (503) 215-6556 or visit www.providence.org/elderplace.
For more information about PACE, visit the National PACE Association website at
www.npaonline.org .
Copyright © 2008 by the Catholic Health Association of the United States.
For reprint permission, contact Betty Crosby or call (314) 253-3477.