BY: JEANNE S. TWOHIG and IRA BYOCK, MD
Ms. Twohig is deputy director, Promoting Excellence in End-of-Life Care,
University of Montana, Missoula, MT; Dr. Byock, director, palliative medicine,
Dartmouth Hitchcock Medical Center, Lebanon, NH, is also director of Promoting
Excellence in End-of-Life Care.
Mr. Jessop, a 70-year-old veteran, spent his last 13 days of life in the ICU.
Throughout his life he was fiercely independent. Although he had neither a living
will nor power of attorney for health care, he had often told his wife and family
that he wasn't afraid of dying. Years earlier, his brother had suffered
a stroke during heart surgery. After visiting him, Mr. Jessop had remarked to
his family that he would rather die than end up strapped to a bed in an ICU.
Now that was exactly what was happening.
His wife of 38 years and his adult children felt bewildered; it had all happened
so fast. But in the last days of his life they became angry — at themselves,
because they felt they had betrayed Mr. Jessop's trust, and at his doctors
for never really giving their family a say in critical treatment decisions.
But how could this have occurred? Ironically, it was nobody's fault — or
at least no one person's fault. The causes of this situation are rooted
in our systems, assumptions, and routine ways of acting.
Mr. Jessop had been a vigorous man all his life, but chronic bronchitis and
advanced congestive heart failure conspired to erode his health when he was
in his 60s. He received good medical care from his cardiologist and pulmonologist;
the correct treatments and medications, in correct doses, were given for his
condition at each point in time. One winter he was hospitalized three times
in as many months for episodes of bronchitis and pulmonary edema. He was intent
on getting better. Helped by around-the-clock, low-flow oxygen via a nasal cannula,
and inhalers, diuretics, and occasional antibiotics, Mr. Jessop was able to
care for himself and enjoy most days.
Two weeks before his death, his breathing gradually worsened. While moving
his bowels one morning, he suddenly became severely short of breath. His wife,
not knowing what else to do, called an ambulance. Paramedics, having found Mr.
Jessop cyanotic and struggling for breath, intubated him en route to the hospital.
He was placed on a ventilator and admitted to the ICU. He initially improved
and regained consciousness, but within a few hours his blood pressure dropped
and a heart attack was diagnosed. Over the next two days, he was intermittently
agitated and required anti-anxiety medication and morphine for comfort. Delirium
worsened, forcing caregivers to apply restraints to prevent him from dislodging
his breathing tube. Bilateral pneumonia was treated with high dose antibiotics
and his blood pressure was maintained with cardiac pressor medications.
Mrs. Jessop was emotionally distraught. She spent many hours at her husband's
bedside, but said little to the nurses or staff. Every day various specialists
explained her husband's condition from their respective perspectives, encouraging
her to be hopeful. They emphasized that he was critically ill, but they never
explicitly said he might die. Mrs. Jessop found it difficult to determine who
was in charge of her husband's care and to know how to interpret seemingly
conflicting messages.
Mr. Jessop, in his second week in the ICU, remained somnolent and intermittently
agitated. Standing beside her mother, Mr. Jessop's daughter said to the
cardiologist as he made morning rounds, "This is wrong. My father would
not want to be here like this." The cardiologist was surprised by the comment
and felt criticized. He replied that removing the breathing tube or untying
Mr. Jessop "would kill him." To this Mr. Jessop's daughter replied,
"It feels like you are torturing him. Won't you please just allow
my father to die?"
Mr. Jessop's pulmonologist felt uncomfortable about withdrawing mechanical
ventilation, fearing that it would cause suffering and might be perceived as
euthanasia. He asked for an ethics committee evaluation. Before his case could
be considered, however, Mr. Jessop developed ventricular fibrillation. Resuscitation
efforts failed and he was pronounced dead.
Crisis at the End of Life
Mr. Jessop's case epitomizes an all-too-common predicament. Evidence suggests
that many Americans die in physical distress, while receiving aggressive medical
treatment that may not be consistent with their preferences for care and is
not justified by its likely benefit. This state of affairs is amply documented
in published research and apparent in poignant accounts of many who have endured
the loss of a loved one.
In 1995 results were released of a study, commissioned by the Robert Wood Johnson
Foundation, which had involved 9,000 critically ill patients at five major U.S.
medical centers. The findings of the $28 million Study to Understand Prognosis
and Preference for Outcomes and Risks of Treatment (SUPPORT) confirmed that
a crisis exists in the way Americans are cared for at the end of life.1
Many patients die in ICUs, often in pain and often without their preferences
for care having been elicited or honored. Despite the expansion in home care
and the growth of hospice in the past two decades, little progress has been
made in the way a majority of Americans die.
Recent studies indicate an incongruity between what seriously ill people feel
is most important about health care and what the current health care system
provides. In a study involving qualitative analysis of interviews with patients,
recently bereaved family members, and experienced clinicians, researchers found
that seriously ill patients and their families value pain and symptom management,
clear decision making, preparation for death and life completion, a sense of
having contributed to others, and affirmation as a whole person.2
Another qualitative study concluded that patients and families value clinicians
who talk in honest, straightforward ways about their patients' conditions, and
who can sensitively break bad news without shirking discussions about death.3
Patients and family members want clinicians who encourage questions and are
sensitive to when patients are ready to talk about death.
Although reasonable, these values and expectations are not consistently achieved.
Indeed, two authorities in the field describe a heath care system in which end-of-life
discussions are not routine and care is frequently fragmented and often provided
by multiple clinicians at multiple sites.4
Contemporary physicians have fewer long-term relationships with patients, less
time for communication, and do not feel charged with or compensated for discussions
with patients' and families' about psychosocial and spiritual needs related
to life completion.
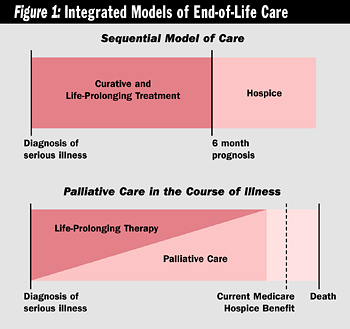 Further complicating the misalignment between the needs of seriously ill patients and their families, on one hand, and current modes of health care delivery, on the
other, are the reimbursement policies of Medicare and many insurance plans,
which typically require patients to forgo life-prolonging care as a condition
for receiving comprehensive palliative care. By statute and regulation, Medicare's
hospice benefit is available only to recipients who are judged to have a life
expectancy of six or less months and are willing to forgo disease-modifying
care. Although such eligibility criteria were reasonable when Congress enacted
the Medicare hospice benefit in 1982, they are out of step with today's
health care environment, in which patients with chronic illnesses may live for
many months at high risk of dying, yet with acceptable quality of life. The
line between treatments intended to prolong life and those intended to improve
comfort and quality of life has blurred. The current dichotomy between life-prolonging
and palliative care results in a sequential approach to care, whereas
a concurrent approach would much better respond to the needs of seriously
ill patients and families.
Further complicating the misalignment between the needs of seriously ill patients and their families, on one hand, and current modes of health care delivery, on the
other, are the reimbursement policies of Medicare and many insurance plans,
which typically require patients to forgo life-prolonging care as a condition
for receiving comprehensive palliative care. By statute and regulation, Medicare's
hospice benefit is available only to recipients who are judged to have a life
expectancy of six or less months and are willing to forgo disease-modifying
care. Although such eligibility criteria were reasonable when Congress enacted
the Medicare hospice benefit in 1982, they are out of step with today's
health care environment, in which patients with chronic illnesses may live for
many months at high risk of dying, yet with acceptable quality of life. The
line between treatments intended to prolong life and those intended to improve
comfort and quality of life has blurred. The current dichotomy between life-prolonging
and palliative care results in a sequential approach to care, whereas
a concurrent approach would much better respond to the needs of seriously
ill patients and families.
Society's cultural fixation on cure and its relative inattention to comfort
and quality of life — combined with third-party payer rules that impose an
arbitrary either-or choice between "curative care" and palliative
care — inadvertently add to the burden that patients with advanced illness
may experience. A compelling need exists to realign health service delivery
with the clinical realities and real needs of chronically ill patients and their
families.
A Strategic Response
Since the results of the SUPPORT study were released, clinicians, health
care administrators, health care consumers, funders, and payers have expressed
keen interest in redesigning the health care system so that it can respond to
the suffering experienced by patients with advanced, incurable illness. Recognizing
this, the Robert Wood Johnson Foundation embarked on a strategic plan to improve
care through the end of life. Employing a multifaceted approach that acknowledged
the complexity of achieving cultural change and simultaneously targeted multiple
leverage points, the foundation developed a broad quality-improvement strategy
that includes efforts to elucidate clinical-practice standards and domains of
quality for palliative care, measurement tools and methodologies applicable
to these standards and domains, evaluation of performance and outcomes, training
curricula, continuing education for clinicians that encompass the breadth of
palliative care practice, and support for relevant certification and accreditation
processes.5 The foundation's strategy also
includes support for research and development of demonstration projects to build
and assess innovative models of care delivery. Public education to raise awareness
of palliative care and end-of-life issues; to empower consumer and citizen advocacy;
and to prompt needed changes in policy, reimbursement, and regulatory matters
round out this strategy.
Palliative Care
At the heart of these strategic efforts is an unwavering belief that seriously
ill patients and their family members deserve coordinated and continuous attention
provided by a skilled team to their psychosocial and spiritual needs, as well
as to their physical needs. This approach, which puts the patient and family
(rather than providers or the reimbursement system), front and center is called
palliative care. Palliative care is defined as interdisciplinary care
for persons with life-threatening illness or injury that addresses physical,
emotional, social, and spiritual needs and seeks to improve quality of life
for the ill person and his or her family. Treatment and secondary prevention
of symptoms and suffering and preservation of personal opportunity are hallmarks
of palliative care.6
Palliative care includes a defined array of services that are provided to patients
and families in an organized, cohesive manner. Hospice has traditionally been
the primary means for delivering palliative care. However, because Medicare
and many third-party payers limit hospice care to patients who have a terminal
prognosis and who agree to treatment that is exclusively focused on comfort
and quality of life, many seriously ill Americans decline to avail themselves
of this benefit, or do so only after exhausting all potentially life-prolonging
interventions. Prognostic uncertainty, distrust of the health care system — especially
among disadvantaged ethnic groups — and an understandable desire to pursue
potentially life-extending treatment further confound appropriate referral to
and acceptance of hospice care.
Over the past decade, efforts have been under way to build on the comprehensive,
holistic, patient- and family-centered care traditionally delivered by hospice
by making such care available to everyone needing palliation, regardless of
diagnosis, prognosis, age, socioeconomic status, or venue of care. Promoting
Excellence in End-of-Life Care, a national initiative of the Robert Wood Johnson
Foundation, is one such effort.
Promoting Excellence
The Promoting Excellence program was launched in 1997 to support innovative
health service delivery to identified patient populations and clinical settings
in which hospice care was underutilized or unavailable. Setting the best hospice
programs and care as "gold standards," the program sought to extend palliative
care "upstream" in the course of illness, concurrent with the provision of ongoing
life-extending care. Local hospice programs were collaborating partners in many
of the program's demonstration projects, and most projects developed a continuum
of services that included referral to hospice.
The 28 demonstration projects that were awarded Promoting Excellence grants
represented a broad range of patient populations and contexts of care. They
included four projects based in university cancer centers; two in tertiary care
pediatric hospitals; a set of regional dialysis clinics; several hospice and
home health agencies in highly penetrated managed care environments; and projects
in rural and frontier communities, inner cities, nursing homes, dementia programs,
and even (in four states) in penitentiaries.
Creating prototypical models of care was chosen as the most direct means of
determining whether palliative care could be delivered to patient populations
within challenging contexts of care. Demonstration projects provide tangible
examples of what is — and is not — feasible and how highly it is valued.
The models developed by Promoting Excellence grantees represent applied research,
the translation of theory into practice. Whenever possible, clinical tools,
curricula, and programmatic resources were crafted to be adoptable, or adaptable,
in similar settings. If successful, such prototypes have the potential to stimulate
improvement well beyond local systems and communities, raising collective expectations
and challenging administrators, health planners, and public policymakers to
aim higher than they otherwise might.
Common Programmatic Threads
Corresponding to the diversity of settings, illnesses, and patient populations
served, Promoting Excellence projects are each unique, with operational strategies
and patterns of service that respond to the needs of local stakeholders — patients,
families, clinicians, health system managers, administrators, and policymakers — fitting
their particular health systems and communities. Within this diversity, however,
the programs share common elements of care, component services, and qualities
(see below).
Each program strives to deliver state-of-the-art clinical care to both patients
and their families and is committed to respecting the cultural, ethnic, religious,
and personal values of those they serve. Each program emphasizes clear communication
with patients and families through clinical protocols, education, and quality
improvement. Each has an interdisciplinary team that creates multifaceted, highly
individualized plans of care reflecting the patient's and family's
values and preferences for care. Crisis prevention and early crisis management
is a common component of practice and care planning. Care plans are frequently
updated to reflect the changing condition of the patient and family.
Recognizing the importance of continuity of care, the Promoting Excellence
grantees have provided case management in every program, but in a diversity
of ways. Most often, a specified nurse or social worker serves as a "care
coordinator." The responsibilities of this key position include maintaining
updated knowledge about the patient's and family's status; overseeing
implementation of the plan of care; acting as an advocate for the patient and
his or her family and assisting them in obtaining and coordinating services
and appointments; and maintaining communication among patients, families, and
the health care team.
In building innovative models, the grantees confronted challenges that, once
overcome, led to strong, successful and sustainable programs for delivering
care (see below). Lessons learned by the grantees suggest
that palliative care programs can align with and advance the institution's
mission.
To succeed, programs must begin with a manageable scope, allowing nascent initiatives
to achieve early successes and earn support and commitment from recognized leaders
in both clinical and administrative realms. Palliative care teams are more readily
integrated into the institution's clinical practice when they are able
to reduce the burden experienced by time-pressured clinicians who are often
untrained to delve into patients' and families' psychosocial needs
and discuss ramifications of the patients' life-compromising illnesses.
Successful interdisciplinary teams embed palliative care practices into routine
operations and have authority to carry out their recommendations and interventions
for patient care. Teams earn the confidence of colleagues by skillfully and
reliably caring for difficult, complex cases.
In addition to focusing on clinical aspects of integrating palliative care
and cure-oriented treatment, sustainable programs also develop long- range business
and communications plans to ensure that all stakeholders receive targeted, cohesive
messages about the availability of palliative care services and their benefits,
and that these messages are augmented by supporting data that demonstrates efficacy.
Promising Results in Los Angeles
The Promoting Excellence initiative supported the creation of new models
of care delivery, requiring that grantees develop sound evaluation plans to
measure the impact of their innovative work. Evaluation focused on demonstrating
the feasibility of the delivery model, its acceptability to a diverse mix of
stakeholders, and its sustainability. As far as was possible, grantees
also evaluated:
- Whether access to palliative care improved
- The impact of the initiative's intervention on quality of care, as
perceived by patients, families, and clinicians
- The financial ramifications of providing palliative care concurrently with
life-prolonging care
Most Promoting Excellence projects have completed their grant-funded work and
continue to analyze data to gauge the impact of providing comprehensive palliative
care simultaneously with potentially life-prolonging treatments. Their preliminary
data on access, quality, and cost is promising. A brief look at one project
may serve as an illustration. The Pathways of Caring program, sponsored by the
U.S. Department of Veterans Affairs' Greater Los Angeles Healthcare System
(GLA), is unique. However, the experience and findings of this project exemplify
the programmatic experience of others.
Pathways of Caring was committed to providing, for patients with advanced life-limiting
illnesses, what the project's clinician-researchers termed the "seemingly
contradictory approaches" of side-by-side disease-modifying treatment and
palliative care focused on increasing comfort and quality of life. The patients
involved were specific groups of veterans, including those with lung cancer,
advanced congestive heart failure, and chronic obstruction pulmonary disease.
The Pathways researchers began by identifying patients in GLA's hospital,
clinic rolls, and medical records who had poor prognoses and were likely to
benefit from comprehensive symptom management. The project's goals included
ensuring relative comfort for patients, coordinating care through the course
of illness, and expanding access to home care and hospice. A nurse case manager
educated patients and their families regarding decision making and self-management
of symptoms. The nurse also provided continuity of care, serving as the hub
of an interdisciplinary team that included a social worker, chaplain, dietician,
and physician, all of whom worked together to meet each patient's and family's
needs.
Preliminary data on 54 participants who died while enrolled in the Pathways
program, compared with a retrospectively matched control group of patients who
did not receive the palliative intervention, show dramatic differences. Available
evidence indicates improvements in the proportion of cases with documented goals
of care and completed advance directives. Forty-three percent of Pathways patients
were able to die at home, compared to just 7 percent of matched control patients.
Forty-five percent of Pathways patients died in a hospital or long-term care
facility, compared to 68 percent of control patients.
The Pathways program averaged 3.5 hospital days per patient during the final
month of life, compared with 8.2 days for the control group. More striking still,
the patients who died while served by Pathways spent an average of just 0.4
days in an intensive care unit during the last month of life, compared with
4.5 days for those in the group not served. Pathways patients on average also
spent far less time on mechanical ventilators in their final month, just 0.1
days per patient in the group served versus 3.5 days in the comparison group.
The program's ability to better manage its patients with life-threatening
illnesses in more appropriate and cost-effective settings has important financial
ramifications, with overall savings of 45 percent on the cost of care in the
final month of life (see Table 1).
Table 1: Cost Per Patient
in the Final Month of Life
|
| |
Pathways of Caring
|
Control Group
|
| Number |
54
|
28
|
| Inpatient costs, mean* |
$ 4,416
|
$ 15,506
|
| Nursing home care unit costs, mean |
$ 2,428
|
$ 1,424
|
| ICU costs, mean |
$ 2,250
|
$ 4,871
|
| Outpatient costs, mean |
$ 3,069
|
$ 1,923
|
| Total costs, mean |
$ 10,248
|
$ 18,853
|
|
* Does not include long-term care facility costs listed
separately.
Source: Department of Veterans Affairs, Greater Los
Angeles Healthcare System
|
The feasibility of this service delivery model and its acceptance by veterans,
their families, and clinicians was clearly evidenced by the appreciation expressed
and the steady rise in referrals and caseload. The ability of the Pathways team
to document the program's success, including its salutary impact on the system's
efficiency and use of health resources, provided a convincing argument for sustaining
the program beyond the grant's duration. In fact, the Pathways program is currently
being expanded, with increases in the number of case management nurses and palliative
care staff physicians, expansion and further integration of the palliative care
consultation team, and formalization of an outpatient palliative care clinic.
Further description of Pathways of Caring, as well as of other Promoting Excellence
grant programs and resources, including two monographs, "Financial Implications
of Promoting Excellence in End-of-Life Care" and "Living and Dying Well with
Cancer," can be found at www.promotingexcellence.org. A special series of articles
in the Journal of Palliative Medicine describes Promoting Excellence
programs and preliminary findings.7
Mr. Jessop Again
Although it is impossible to say with certainty what the final days of life
would have been like for Mr. Jessop, had he been a patient in a program like
Pathways of Caring, some things would undoubtedly have been different. Because
of the severity of his chronic illness, Mr. Jessop would have been identified
during a clinic visit or during one of his previous emergency hospitalizations
as someone who would benefit from palliative care. A palliative care coordinator
would have assessed the immediate needs of both Mr. Jessop and his family and
provided education about advanced congestive heart failure and its unpredictable
trajectory. Mr. Jessop's family situation, values, religious or spiritual concerns,
and wishes would have been explored, and he would have been guided to put his
preferences for care in writing within an advance directive. A team of clinicians,
including his primary physician and palliative care coordinator, would have
contributed to a multifaceted plan of care and been available to manage the
crises.
If Mr. Jessop had been in a palliative care program when the latest exacerbation
of his illness occurred, events might have unfolded quite differently than they
did. With a plan of care already in place and the availability of a familiar
nurse coordinator to assess and guide, Mr. Jessop and his family would have
reported his symptoms to the nurse with whom they were familiar. After assessing
his symptoms by phone the nurse would have instructed him to take an extra dose
of diuretic or made a home visit to further evaluate, adjust his medications,
and plan careful follow-up. It's possible the crisis would have been adverted — and
his life prolonged.
If his condition had worsened, Mr. Jessop and his family could have made an
informed decision whether to go to the hospital or be cared for at home. At
the least, his desire to die peacefully, without an extended traumatic stint
in an ICU, could have been known and honored.
While the number of patients studied in the Pathways project is small, the
findings show trends that were substantiated by other Promoting Excellence projects.
Early results from these prototypes suggest that concurrent palliative and cure-oriented
care is clinically effective and associated with systems efficiencies and no
increase in total health care resources; in fact, they indicate that fewer resources
were needed for patients in palliative care than for those who were not.
Building on Positive Results
The Institute of Medicine's landmark 1997 report, Approaching Death:
Improving Care at the End of Life, recognized an urgent need to improve
care through the end of life and called for significant improvements in clinical
education, health systems design, and service delivery, as well as for changes
in health care financing, outcomes measurement, quality improvement, and oversight.8
In the era of patient-centered care it is no longer acceptable for our health
care system to do what is expedient for institutions and providers. Patients
with advanced, incurable conditions and their loved ones must be able to expect
clear communication, shared decision making, effective management of symptoms,
continuity of care, prevention of or early response to crises, and support for
families in their caregiving and in their grief. Although preliminary, the early
programmatic and clinical findings of Promoting Excellence projects have clearly
shown that these reasonable expectations are achievable.
Most of these projects are continuing beyond their period of grant support.
They have proven their feasibility and efficiency within their local health
systems and have been highly valued by patients, families, and providers alike.
Collectively, these prototypes have demonstrated that it is possible to align
health services to meet the needs of seriously ill patients and their families,
notably improve outcomes of care, while remaining fiscally responsible for the
financial well-being of the institutions involved. The challenge now is to build
upon this promising work through population-based demonstration projects and
studies.
NOTES
- The SUPPORT study is discussed in W. A. Knaus, J. Lynn, J. Teno, et al.,
"A Controlled Trial to Improve Care for Seriously Ill Hospitalized Patients,"
JAMA, vol. 274, no. 20, 1995, pp. 1,591-1,598.
- K. E. Steinhauser, E. C. Clipp, M. McNeilly, et al., "In Search of
a Good Death: Observations of Patients, Families, and Providers," Annals
of Internal Medicine, vol. 132, no. 10, 2000, pp. 825-832.
- M. D. Wenrich, J. R. Curtis, S. E. Shannon, et al., "Communicating
with Dying Patients within the Spectrum of Medical Care from Terminal Diagnosis
to Death," Archives of Internal Medicine, vol. 161, no. 6, 2001,
pp. 356-362.
- D. Larson and D. Tobin, "End-of-Life Conversations: Evolving Practice
and Theory," JAMA, vol. 284, no. 12, 2000, pp. 1,573-1,578.
- I. Byock, "Dying Well in America: What Would Success Look Like?" This was
an address to the Second Last Acts National Conference, October 1997, in Washington,
DC; it can be found at www.lastacts.org/la_ala/levdying.htm.
- Standards and Accreditation Committee, A Pathway for Patients and Families
Facing Terminal Disease, National Hospice Organization, Washington, DC, 1997.
- See, for example, M. Bakitas, M. Stevens, T. Ahles, et al., "Project
ENABLE: A Palliative Care Demonstration Project for Advanced Cancer Patients
in Three Settings," and M. Ratcliff and E. Craig, "The GRACE Project: Giving
End-of-Life Care in Corrections 1998-2001," both in the Journal of Palliative
Medicine, Vol. 7, no. 2, April 2004. For the Pathways of Caring program,
see K. Rosenfeld and J. Rasmussen, "Palliative Care Management: A Veterans
Administration Demonstration Project," Journal of Palliative Medicine,
vol. 6, no. 5, October 2003, pp. 832-839.
-
M. J. Field and C. K. Cassel, eds., Approaching Death: Improving Care at
the End of Life, National Academies Press, Washington, DC, 1997.
CALL Care and "Promoting Excellence"
Between August 2001 and February 2003, 11 Catholic health care organizations
involved in CALL Care, a nationwide project sponsored by Supportive Care of
the Dying: A Coalition for Compassionate Care, Portland, OR, were Promoting
Excellence demonstration sites and received funds from the Robert Wood Johnson
Foundation.
For more on CALL Care, see Sylvia McSkimming, RN, PhD; Marla London; Carol
Lieberman; and Ellen Geerling in "Improving
Response to Life-Threatening Illness," Health Progress, January-February
2004, pp. 26-33, 56.
The participating CALL Care organizations were:
- Good Samaritan Health Center of Merrill, Merrill, WI
- Holy Cross Hospital, Silver Spring, MD
- Mercy Rehabilitation and Care Center, Roseburg, OR
- Our Lady of Lourdes Regional Medical Center, Lafayette, LA
- Sacred Heart Medical Center, PeaceHealth-Oregon Region, Eugene, OR
- Providence Hospitals and Medical Centers, Southfield, MI
- St. John Neumann Nursing Home, Philadelphia
- St. John's Regional Medical Center, Joplin, MO
- St. Joseph Mercy-Oakland, Pontiac, MI
- St. Mary's Hospital and Medical Center, Grand Junction, CO
- Via Christi Regional Medical Center, Wichita, KS
SSM Cardinal Glennon Children's Hospital, St. Louis, is currently
a Promoting Excellence demonstration site.
Typical Palliative Care
Services
Palliative care services usually include:
- Ongoing communication and review of goals of care
- Advance care planning
- Formal symptom assessment and treatment
- Care coordination
- Spiritual care and attention to psychosocial needs
- Anticipatory guidance related to adaptation to illness and issues of life
completion and life closure
- Crisis prevention and early crisis management
- Bereavement support
- Around-the-clock availability of a clinician knowledgeable about the patient
and family
10 Essential Ingredients
for Building Successful Palliative Care Programs
To succeed, a palliative care program should have:
- A well defined vision that
- Advances the institution's mission
- Encompasses a comprehensive definition of palliative care
A well-planned implementation strategy that is
- Manageable in scope
- Consistent with available human and financial resources
Unwavering support from clinical and administrative leaders willing to
- Champion the program
- Help secure operational resources
Ongoing efforts to bridge the differences between palliative and acute care
clinical cultures that
- Entails learning on both sides
- Integrates experienced staff with diverse expertise, including psychosocial
and spiritual care
A focus on making "the right way the easy way" by
- Responding to workday needs of time-pressured clinicians and management
- Redesigning operations to embed and trigger palliative practices in daily
routines
Ongoing education, support, and attention to team building for clinicians
and system personnel to
- Ease adoption of innovation
- Strengthen clinical interventions
An assurance that palliative care teams have authority to carry out their
clinical recommendations and interventions for patient care and have "safe
havens" for the discussion of problems and ideas
Attention to diverse ethnic and religious cultures of individual patients
and families through
- Sensitivity to the uniqueness of individuals and their preferences
- Careful selection of language to convey program elements
Targeted data collection focusing on
- Increased access to palliative care
- Improved quality of care
- Resource utilization and cost
- Patient/family/clinician satisfaction
A communications strategy for succinctly presenting relevant data to stakeholders
Copyright © 2004 by the Catholic Health Association of the United States
For reprint permission, contact Betty Crosby or call (314) 253-3477.