BY: BISHOP JOSEPH M. SULLIVAN, DD
Bishop Sullivan is former auxiliary bishop, Diocese of Brooklyn, N.Y.
In 1986, the Catholic Health Association (CHA) Board of Trustees appointed a task force to promote a better under-standing of aging issues and the implications for the Catholic Church in the United States. Two years later, CHA published A Time to Be Old, A Time to Flourish: The Special Needs of the Elderly-At-Risk. The report was person-centered, focused on the needs of the frail elderly, especially the poor. In an earlier report by CHA, No Room in the Marketplace: The Health Care of the Poor, addressed the needs of all poor persons. A Time to Be Old specifically focused on the elderly-at-risk and the need for a coherent set of long-term care services.
Health care in the 1980s was undergoing financial pressures as costs escalated at a double-digit rate. Medicare and Medicaid expenditures were not sustainable. The industry was alarmed at the increase in premiums, which threatened its competitiveness in a global market. Government was turning to the marketplace to reign in costs. For-profit companies were established to provide health care services that would compete with not-for-profit providers for market share. Not-for-profit voluntary corporations were creating systems of health service delivery in order to be able to compete. In the turmoil of health care, it was possible to lose sight of a rapidly aging population.
CHA saw an urgent need to call attention of its members to the rapidly aging population, a phenomenon that was entirely new. The retiring elderly population was increasing more rapidly than the number of persons entering the workforce, according to the Administration on Aging (AOA), which is part of the U.S. Department of Health & Human Services. In 1900, the ratio was 7 elderly to 100 people of working age. By 2020, it is projected that the ratio will increase to 29 per 100, and by 2050, 83 per 100.
Second, it was judged the U.S. long-term policy was outmoded and a lack of a coherent set of long-term care services existed. The fragmentation in funding drove a fissure in service delivery.
Third, serious concern existed about a new form of ageism, where the elderly were believed to be getting more than its fair share of resources. They were perceived by some as a powerful political block able to obtain benefits unavailable to any other age group, especially children. The potential danger of intergenerational conflict was real. The 1988 CHA report was intended to educate, to provide a better understanding of aging issues and their implications for the church and its institutions at the local, state and national levels.
The report on the elderly-at-risk made specific recommendations to the church, to parishes, to dioceses, to state conferences, Catholic health care providers, CHA and government. It called for the creation of a continuum of care, i.e., a coordinated, integrated array of effective long-term services with an explicit focus on the person. The system should be comprehensive, calling for a change in the present delivery system. It should emphasize collaboration, not competition. It should stress prevention and rehabilitation.
In 2003, Father Michael Place, STD, then president and CEO of CHA, directed a review of the implementation of the report by CHA. In 1995, CHA was the prime convener of The New Covenant meeting. This meeting spawned the Coalition of Catholic Health Care Ministries, a forum for the National Conference of Catholic Bishops; Catholic health care sponsors; the Leadership Conference of Women Religious; the Council of Major Religious Superiors; the Conference of Major Superiors of Men; Catholic Charities USA (CCUSA); and CHA to discuss issues of collaboration on health care at the national level. Eventually Ministering Together, a 501(c)(3) corporation, comprised of a wide-range of church-related organizations launched by the coalition to promote collaboration of diverse ministries at the local level, was formed. CHA and CCUSA subsequently developed a directory of Catholic health and social services at the diocesan and community level. CHA advocated safeguarding and enhancing benefits to low income individuals who were dually eligible under Medicare and Medicaid and for fair reimbursement to long-term care providers. CHA recognized the need for more to be done for a rapidly growing population of the elderly, the chronically disabled and caregivers.
Twenty years ago, CHA and other organizations anticipated a rapidly growing population aged 65 years and older. The vast majority of older Americans want to age in their own homes and communities as along as possible. The aging population poses new challenges for the delivery of local services, such as health care, housing, transportation, recreation, public safety, employment and education. At the same time, the aging population presents opportunities to communities as a large group of educated and skilled older adults.

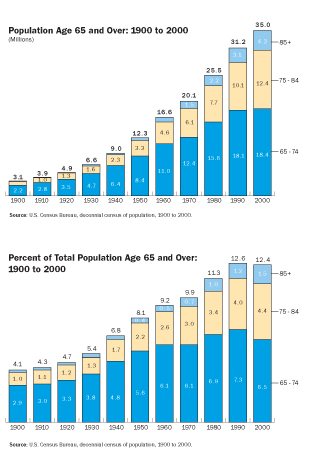
The growth rate of the elderly population far exceeded the growth rate of the total population during the 20th century, according to the U.S. Census Bureau. While the total population more than tripled, the 65 years and older population grew more than tenfold. Strangely, from 1990 to 2000, for the first time in the history of the census, the 65 years old and above population grew slower than the total population. This was directly related to the low fertility rate of the late 1920s and 1930s. The growth of the aged 85 years and older for the century is particularly notable from 122,000 in 1900 to 4.2 million in 2000. The aged 85 and older group increased as a proportion of the elderly population, from 4 percent in 1900 to 12 percent in 2000. In the 1990s, the 85 and older group increased by 38 percent, significantly higher than the 65-to-74-year old group (less than 2 percent), and the 75-to-84-year old group, 23 percent.
America is aging rapidly. As the baby boomers (those born between 1946 and 1964) reach retirement, the number of Americans above 65 years old is expected to reach 71.5 million by 2030, twice the number in 2000, according to the AOA. The vast majority of older Americans want to age in their homes and communities as long as possible. The aging population poses new challenges for the delivery of local services, such as health care, housing, transportation, recreation, public safety, employment and education.
Health Care Providers
In the past generation, we have witnessed health care providers reorganize into systems that have tried to develop integrated service delivery systems comprising acute care, long-term care, community and home-based services. Driven largely by funding sources, lengths of stay were shortened and people were discharged to alternative levels of care. A major result impacting the elderly was the shift of responsibility towards unpaid providers, increasing burdens on family caregivers. More than three-quarters of adults living in the community and in need of long-term care depend on family and friends. Among the most severely disabled older persons living in the community, about two-thirds rely solely on family members and other informal/unpaid help. Astonishingly, 30 percent of persons caring for elderly long-term care users were themselves 65 or above, according to the AOA.
A gross measure of the availability of informal caregivers is the ratio of the population in the average giving range — ages 50 to 64 — to the population aged 85 and above. In 1990, the rate was 11 to 1; by 2050, it will be 4 to 1.1
The trend toward community-based services as opposed to institutional placement was formalized by The Olmstead Decision in 1999. The U.S. Supreme Court upheld the right of individuals to receive care in the community, as opposed to an institution, wherever possible.
Church Response
As Jack E. Curley, Jr., former president of CHA, noted in 1988 that the church brings substantial resources to help it respond to the challenges of an aging population. These include 63 systems of health care; more than 600 acute care hospitals; more than 500 nursing homes; 122 home health agencies; innumerable community-based clinics; 16 managed care agencies; and 36 hospices. In addition to this vast array of health resources, 173 Catholic Charities agencies provide community-based social services, senior citizen centers offering counseling, nutritional, recreational information and referral services. One of the least known resources of the church for the elderly is the number of housing units for the elderly sponsored by dioceses, religious communities and Catholic Charities.
More than 19,400 parishes in 196 dioceses provide pastoral services to the elderly, senior citizens clubs and volunteers doing home visits. They offer transportation to clinics and deliver meals-on-wheels. Some parishes have visiting nurses programs for the elderly and respite services for caregivers of the elderly. Others have educational programs which inform the elderly about public policy issues and engage them in advocacy for the needs of the elderly. Potential at the parish level exists to tap the talent, knowledge and experience of the well-elderly, to improve the quality of life for all in the local community. The movement toward collaborative ministries at the local level, promoted by Ministering Together, is one of the positive directions for the church's efforts to overcome fragmentation in service delivery and to create community-based services to respond to the needs of the elderly and their caregivers.
Government
The project, "Maturing of America — Getting Communities on Track for an Aging Population," led by the National Association of Area Agencies on Aging in collaboration with the International City/County Management Association; the National Association of Counties; National League of Cities; and Partners for Livable Communities, funded by the MetLife Foundation, identified ways to prepare for the aging of the population.
The report surveyed 10,000 local governments to:
- Determine their "aging readiness" to provide programs, policies and services to older adults and caregivers
- Ensure their communities are livable for all age groups
- Harness the talent, wisdom and experience of older adults to contribute to their community
The survey indicated 46 percent of American communities have begun to address the needs of older adults. Few, however, have undertaken a comprehensive assessment to make their communities "elder friendly." Local governments generally offer basic health and nutrition programs but do not have policies, programs and services to promote the quality of life and the ability of older adults to live independently and contribute to their communities. The needs of older adults are interdependent and require a new comprehensive, holistic approach to service delivery organization and management. Those communities who have already begun to assess their "aging readiness" are now beginning to engage older citizens to discuss what changes to local government services may be needed to enhance their quality of life. Although some changes may require significant investment, many quality of life improvements are not costly, such as road signs that are more visible and easily read, changing timing of directional signals at pedestrian crossings and changing zoning ordinances to allow smaller residences.
The Maturing of America report makes recommendations in 11 different areas of concern ranging from nutrition and health concerns to housing and transportation. This article focuses on six topics:
- Health — communities should play a major role in ensuring access to a range of needed preventive health care services
- Nutrition — communities should support a range of healthy home-delivered and congregate meals
- Exercise — communities should provide a range of fitness programs to assist older adults to safely and effectively exercise
- Transportation — communities should offer driving assessment and training and assess their existing public transportation system
- Housing — communities should play a role in promoting the development of home modification and development of housing options
- Aging /Human Services — communities should promote the development of a single point of entry for information and access to all aging services
Commercial Sector
For-profit investor owned corporations have been able to raise significant capital to address the residential needs of the more affluent senior population. Retirement communities and assisted living residences have provided opportunities for seniors to age in place. Capital investment in medical technology also has made it possible for many to remain in their own homes or apartments. Capital investment in pharmaceutical research has, and will develop, breakthroughs in medical treatment.
This issue of Health Progress is dedicated to reviewing where we stand as a nation in dealing with a graying population. The demographics of aging were predictable. We are on the brink of a massive infusion of baby boomers into the ranks of the elderly. There were 35 million people 65 and older in 2006. This is projected to double by 2030, making for an increase from 12 percent of the total population to 20 percent. A major challenge to health and human service providers is the growth of the 85 and above population. The level of disability and cognitive impairments among those who receive assistance with daily tasks has risen sharply. The population receiving help with three to six activities of daily living increased from 35.4 percent to 42.9 percent between 1984 and 1994. In 2005, an estimated 5 million people were aged 85 and older. This means that there could be an increase from 1.6 million to 6.2 million age 85 or above with severe or moderate memory impairment in 2050, according to the Family Caregiver Alliance.
Conclusion
Probably the most significant indicator of the flawed financing of health and human services is the number of people uninsured for health care cited by the U.S. Census Bureau: 47 million. Although the federal government has invested significant funds for prescription drugs, the elderly are paying substantial out-of-pocket costs. Medicare and Medicaid face serious financial challenges and a way must be found to ensure their financial sustainability. Social Security, one of the most important supports for elderly income, needs to be shored up to meet the massive expansion posed by retiring baby boomers. The nation has to address the affordable housing needs of all low income people, and in particular the elderly.
The AOA reports that the number of disabled persons will grow rapidly, more than triple between 1986 and 2040. It is projected that the number of moderately or severely disabled will grow from about 5.1 million in 1986 to 22.6 million in 2040. There is a dramatically greater risk of impairment for persons with lower income: 71 percent of the impaired elderly have incomes under 200 percent of the federal poverty level. Analysts predict that those clinically diagnosed with Alzheimer's disease may be as many as 10.2 million by 2050. Most of those cases, some 70 percent, occur among ages 85 and over.
Plus, the AOA reveals that the number of persons residing in nursing homes will double or triple by 2030. The number could rise by more than 200 percent for those aged 85 and above. Even if residency ratios decrease by 6.5 percent per decade to 2030, the number of residents in nursing homes will increase by 57 percent.
Even more, often overlooked is the adequacy and availability of a trained work force. Few physicians choose geriatrics. Only 8,800 of the 684,000 U.S. physicians (1.2 percent) are certified in geriatric medicine. Also, the shortage of paraprofessional workers (certified nursing aides in nursing homes and home-care aides) is probably the most serious issue to be addressed.2
As we look to the future and the challenges of our aging population, we will be accompanied by the unresolved problems of the past — the financing of health care, the fragmented service delivery systems, insufficient home and community-based programs and services, the underdeveloped information technology to assist families with knowledge of access to available resources, the support services for caregivers and the daunting reality of chronic disability of the frail elderly, especially those 85 years and above.
The problem of the uninsured has caught the attention of the American people so that health care reform is the major domestic policy issue for the 2008 U.S. presidential election. The national debt and the diversion of major financial resources to the war and the fight against terror present a major obstacle to attending to domestic health, education and social service needs.
We have made progress addressing the long-term care needs of the aging population. Yet, we have a long way to go in addressing the needs of aging people of color, of the aged 85 and older and the chronically disabled. The financing of long-term care will present a major challenge conceptually and politically. However, the lack of a well-trained, well-qualified work force for long-term care is a graver problem. The progress of the past 20 years and a better informed population gives us some reasonable hope that we can more effectively respond to our elderly at risk, especially the frail.
NOTE
- Robyn I. Stone, "Long Term Care for the Elderly with Disabilities: Current Policy, Emerging Trends, and Implications for the 21st Century," August 2000, Milbank Memmorial Fund, NYC.
- Stone.
Copyright © 2008 by the Catholic Health Association of the United States.
For reprint permission, contact Betty Crosby or call (314) 253-3477.