By JULIE MINDA
Joanna Mills says she is not sure how she would have gotten through the last five months, were it not for Melanie Rae Pappalardi and the virtual bereavement support group Pappalardi runs every Thursday evening on Zoom. Pappalardi is a social worker providing bereavement support under an expansion of services by New York's ArchCare long-term care system and its Calvary Hospital, an acute palliative care hospital in the Bronx. The Archdiocese of New York sponsors ArchCare.
Joanna Mills, right, is shown here with her mother, Nora Mills, during one of the many hospitalizations before her death. Mills attends ArchCare at Calvary Hospital's virtual bereavement group.
Mills, of Yonkers, New York, had been one of the main caregivers of her mother, Nora Mills, who had a degenerative heart condition and chronic obstructive pulmonary disease. A massive stroke in March caused a profound deterioration in Nora Mills' condition, and she spent much of the spring on hospice care at home — with some of her care delivered by ArchCare staff. By early June, she was so debilitated that she no longer could be cared for at home, and she was admitted to Calvary, where she died June 18.
Joanna Mills says the trauma of witnessing her mother's deterioration, the deep grief that her death has brought, along with ongoing family battles surrounding her mother's illness and death have left her in a very dark place emotionally. Although Mills was allowed compassionate visits before her mother died, an exception to visitation restrictions that was made at all ArchCare sites in line with state health department guidelines, she still felt robbed of precious hours with her mother.

Joanna Mills and her mother Nora Mills in a photo taken early this year.
The bereavement support group props Mills up in her still-fresh grief. She looks forward to Thursdays, when she can join a dozen or so grieving adult children who empathize with and support each other in their sorrow.
While Calvary always has offered bereavement services, it wasn't until the pandemic hit and New York shut down in-person gatherings that Calvary moved all of them from in-person format to virtual format, expanded the breadth of its services, and tailored some of those services specifically for the close survivors of ArchCare nursing home patients who died during the pandemic.
Hotspot
ArchCare has five nursing homes and a network of other programs in New York City and Upstate New York. Four of their nursing homes are in New York City.
Roughly half of the state's confirmed and probable COVID deaths that happened in nursing homes were in New York City, according to data from the New York State Department of Health.
ArchCare nursing homes had recorded 295 patient deaths from COVID-19 by late October.
Fr. John Anderson is ArchCare's vice president of mission integration. He says that while ArchCare's nursing homes have access to a team of staff chaplains and social workers who provide bereavement support, the system did not have enough staff to keep up with the extraordinary level of need amid the pandemic.
Prior to the pandemic, Fr. Anderson had been in conversation with Maria Georgopoulos, Calvary director of bereavement services, about how Calvary might partner with ArchCare's long-term care sites on bereavement services.

Nora Mills visits with her nephew in her apartment.
Georgopoulos says the onset of the pandemic put those conversations on the fast track, and in a matter of a month, Calvary and its corporate parent ArchCare had come up with programming that they have since expanded. Calvary shifted Pappalardi's time, which had been devoted solely to Calvary, to ArchCare's long-term care sites, and hired additional staff.
Pappalardi and the other master's prepared therapists now call loved ones of every newly deceased resident of an ArchCare nursing home to offer them bereavement support and resources. They've made more than 700 such calls since April (in some cases, they call multiple family members of the deceased).
Not alone
The therapists making the calls offer one-on-one bereavement counseling and access to the bereavement support groups and resources helpful in the grieving process. Pappalardi says a goal is to ensure families know they are not alone in their grief. All the services are available to loved ones of any client of ArchCare, whether or not the client died of a COVID-related cause.
Pappalardi says she and the other therapists who offer the one-on-one phone counseling provide "client-centered therapy, where we meet them where they are emotionally and support them with empathetic listening, and there is no judgment." Over the course of a few calls, a therapist will encourage the client to share stories of their loved one, to talk about how they are processing their grief and to set goals for their progress in healing. After providing this initial support, counselors can refer the clients to a bereavement support group at Calvary or other providers who can offer longer-term grief counseling.
Group support
Prior to the pandemic, Calvary had conducted about 30 in-person bereavement groups — sessions were categorized by the type of relationship the client had to the deceased, and were offered at no cost. Anyone could attend, whether or not their loved one had died at Calvary.
Calvary switched all of those groups to either telephone conference or videoconference mode after New York shut down in-person gatherings amid the pandemic. Calvary also added support groups specifically for those who had lost a loved one to COVID. According to Pappalardi, Calvary added those groups in recognition of the "additional impact COVID has made in the grieving process."
The people whose loved ones died at an ArchCare nursing home can choose the support group from among Calvary's offerings that best fits their circumstances, just as anyone else in the community would.
Mills takes part in the virtual sessions for people whose parent or parents have died. Each week there is a mix of familiar and new faces. After introducing themselves, each participant has the opportunity to describe their loss and how they are experiencing the grief process.
Mills says Pappalardi often will give "homework assignments" in advance of the sessions, sharing topics she plans to bring up for discussion. For instance, Mills says, the group soon will be talking about how they plan to navigate the holidays, with the sadness of not being able to celebrate the season with their loved one.
Mills says that, like her, many in the group struggle with guilt, sadness and regret around what they lost out on, because of COVID restrictions. Her mother never tested positive for coronavirus, but because of the restrictions intended to limit viral spread, Mills only could visit when her mother was on the brink of death, and then only briefly.
"It was killing me not to be able to be there with her" the whole time she was at Calvary, Mills says, adding that the group therapy is helping her. "I'm now talking about my mother's death, and I'm starting to do a little better now."
Amid coronavirus, recreational therapists become Skype coordinators, family counselors
In early March, recreational therapists at the ArchCare at Terence Cardinal Cooke Health Care Center in New York City were busily organizing the annual St. Patrick's Day celebration for residents — booking a band, planning decorations and party food — while juggling the numerous ongoing social activities at the 600-bed continuum-of-care facility.
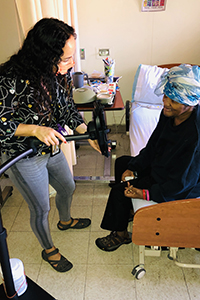
Kimmy Diaz, left, a recreational therapist at ArchCare at Terence Cardinal Cooke Health Care Center in New York City, sets up a Skype call between resident Dorothy Forbes and her family.
But a COVID-19 surge in New York City threw a wrench in all such plans. Residents could not safely congregate even in small groups. And the ArchCare long-term care system discontinued nonessential visitation at all five of its nursing homes on March 12, including Terence Cardinal Cooke because of COVID infection concerns. (Recently, the Terence Cardinal Cooke home resumed in-person visitation on a very limited basis; and it is restarting social activities involving 10 or fewer residents.)
When the pandemic hit full force in New York City in the late winter, recreational therapists were pressed into new duties that called for heightened sensitivity to residents' and family members' social and emotional well-being. The new duties also challenged the staff members' resilience. They consoled lonely and isolated residents and they facilitated sometimes fraught phone calls between residents and their loved ones. They got questions about treatments or prognosis that the therapists were unprepared or legally not allowed to answer.
Similar scenes played out at every one of ArchCare's facilities, according to Thomas McDonald, director of therapeutic recreational and volunteer services at Terence Cardinal Cooke.
Because of a severe shortage of personal protective equipment in the late winter and spring, recreational therapists did not have full PPE when they held computer tablets near the faces of patients who required such assistance during video calls — a situation that put both patient and staff member at potential risk of infection. ArchCare has ample personal protective gear now, and, at the recommendation of a Wellness Advisory Committee, the nursing homes have wheeled devices with an extendable arm that can hold the tablets in position for residents engaged in video calls, allowing for more privacy and, because the therapist no longer need stand close to hold a screen for a resident, an added protection against viral transmission.
Occasionally, the calls become emotionally charged; unpacking complex family dynamics that go well beyond the scope of a recreational therapist's training.
"They could be in the room for one horrific video call then immediately have to take the tablet into the next resident room for the next call" with no time to decompress emotionally, says Fr. John Anderson, ArchCare vice president of mission integration.
Heads together
Fr. Anderson, established ArchCare's wellness committee in the spring to find ways to mitigate against the emotional distress of staff and patients alike. He chairs the committee, which meets weekly. Made up of directors and other managers of recreational therapy, pastoral care and other departments across all of ArchCare, the committee tackles concerns raised by staff, patients and family members. The committee functions as a liaison between frontline staff and system-level executives.
The committee provides guidance and training for recreational therapists and other staff striving to compassionately care for residents and families under extreme pressure. It wrote protocols and informal scripts for recreational therapists to use when difficult situations arise during resident calls with family members.
Recreational therapists now know to refer family members to the residents' nursing team for clinical questions. And, they've learned how to deescalate emotionally fraught conversations and immediately connect willing family members and residents to ArchCare pastoral care team members, social workers or bereavement counselors from Calvary Hospital in the Bronx. (See story.)
Recreational therapists soon will get training from a bereavement counselor on how to respond to the needs of grieving residents and their loved ones.
"The reality is that recreational therapists have been doing a very different job than they were trained to do," Fr. Anderson says. "A lot of their work in the past was done to build community, and that is still the goal," but now they are on the frontlines of helping residents and families in crisis.
Onslaught
McDonald says the onset of the pandemic had recreation therapists scurrying to find new ways to keep residents engaged, when they could have no outside visitors and could not be physically proximate to their peers inside the facility.
The small staff of therapists — the ratio of residents to recreational therapy staff is about 50 to 1 — at first focused on one-on-one activities with residents and connecting residents to loved ones by phone or Skype. There continues to be a full schedule of video calls at the facility. During the first week of October, for instance, therapists coordinated 722 video calls for residents of the Terrance Cardinal Cooke facility.
McDonald confided his team's struggles to Fr. Anderson soon after ArchCare facilities began caring for COVID patients. Hearing similar concerns from ArchCare's other sites, Fr. Anderson organized the Wellness Advisory Committee. Since April, the group has convened weekly for at least an hour to brainstorm how to solve issues, sharing the strengths and weaknesses of approaches they've already tried.
As a result of the committee's input, ArchCare began biweekly systemwide update calls — one for staff and one for residents' families. Fr. Anderson started a weekly virtual prayer group that McDonald says has greatly comforted staff members. The system added resources to support staff and reduce the risk of burnout.
In late October the committee's focus was on the safe resumption of limited visitation and the reintroduction of group recreational therapy activities.
McDonald calls the recreational therapists at ArchCare heroic and says that once they were given the support they needed, the therapists "hit a groove. They've all really stepped up in a difficult situation, and they have been doing a great job."
— JULIE MINDA
Calvary offers emotional support to caregivers worn down by COVID
Staff members at ArchCare's long-term care sites have been struggling amid the pandemic with burnout, fatigue and grief, says Fr. John Anderson, ArchCare vice president of mission integration. He says frontline staff especially have been strained by the responsibilities of keeping residents safe, active, engaged and connected to their loved ones. These are difficult goals to achieve in usual times, much less now, given the dangers of the virus and the restrictive protocols that reduce the risk of viral spread.
Added to those stressors is the sadness many staff experience with the deaths of beloved residents and their empathy for the grieving families, he says. While such strains were present before the pandemic hit, they are more prevalent now, because the death rate in the nursing homes spiked with the onset of the pandemic.
Calvary, a hospice and palliative care hospital in the Bronx, is providing supportive services to staff of its sister facilities in the ArchCare system. In addition to five nursing homes, those facilities include a residential specialty hospital for medically fragile children and units for people with Huntington's disease.
Most of the psychological support services for staff are delivered by Maria Georgopoulos, Calvary director of bereavement services, and her team of master's prepared therapists. They offer one-on-one counseling to ArchCare colleagues over Zoom videoconference, by phone, or on rare occasion, in-person and a weekly support group over videoconference.
Compassion fatigue
Georgopoulos says, "The services are geared to those struggling with death and other losses. Many staff members are experiencing heightened anxiety, less social support, more compassion fatigue and high demands that lead to burnout."
She says in the spring, most New York long-term care facilities were seeing an influx of COVID-positive patients, and were struggling to contain viral spread in-house and doing so without sufficient protective gear. Staff members "were surrounded by death, and we were definitely seeing needs" for mental and emotional support, Georgopoulos says.
While there have been no COVID deaths in ArchCare facilities since July — staff are dealing with latent trauma, say Georgopoulos and Fr. Anderson.
Georgopoulos says, "When frontline staff come to work, they tend to compartmentalize the difficult experiences they have to get through the day. But they need a place to go with their feelings and reactions and to understand their own inner processing. We are helping staff find ways to acknowledge what they are going through" and work through it.
Calvary soon will offer skill-building workshops to staff of ArchCare long-term care sites. While the curriculum is still under development, Georgopoulos says the plan is to have interactive training that provides basic interventions staff can use to care for residents and their loved ones at times of heightened emotion.
The interventions will be helpful for use with people experiencing anxiety or loss because of the pandemic, or because of approaching death. With the training, staff will be better equipped to provide an initial response to residents and loved ones' needs before referring them to the Calvary therapists, says Georgopoulos.