Neurological institute provides no cost medical care, physical therapy to homeless women
By JULIE MINDA
Earlier this year, a domestic abuse survivor traveled nearly six hours by car to seek care from Dignity Health's Barrow Neurological Institute in Phoenix.
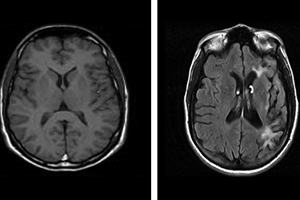
Brain scans provided by Dignity Health's Barrow Neurological Institute in Phoenix show the contrast between a normal brain, at left, and the brain of a patient diagnosed with traumatic brain injury. The white shadowing is damaged tissue in the injured brain, where atrophy is present, according to Barrow experts
Institute social worker Ashley Bridwell recalls of the woman: "After 14 years of terrible abuse by her spouse, she couldn't find a provider in San Diego" who fully understood her neurological symptoms and could address them effectively. The woman's physician had read of Barrow's work with women and men who sustained traumatic brain injury from intimate partner violence and recommended she contact the institute.
Bridwell says the woman "wept when she found us, she was so relieved. She saw that the people here understood." The clinicians who evaluated her confirmed the symptoms she was experiencing were caused by traumatic brain injury.
The woman is one of approximately 300 patients who have been evaluated and treated through the novel Domestic Violence Traumatic Brain Injury Program at Barrow's Concussion and Brain Injury Center. The neurological institute is part of Dignity Health St. Joseph's Hospital and Medical Center in Phoenix.
An estimated 1.7 million people in the U.S. suffer from traumatic brain injury. Normally caused by a blow or series of blows, a jolt or a penetrating injury to the head, traumatic brain injury has been connected to a wide range of physical, behavioral and cognitive symptoms. These can include headaches; changes in vision and hearing; dizziness and balance problems; seizures; problems with concentration, learning and remembering; sleep disorders; difficulties performing daily activities; emotional disturbances and problems relating to others and issues with substance abuse.

Bridwell
At Barrow a multi-disciplined care team designs patient-specific treatments that may include some combination of neuropsychology, physical therapy, occupational therapy, speech therapy, medication, social work and injury prevention education.
In some cases, full recovery is possible. In all cases, the treatment team aims to help restore people to their highest attainable mental and physical function.
Intuitive leap
The clinical program for abuse survivors was the brainchild of Bridwell and Dr. Javier Cárdenas, the neurologist who directs the Concussion and Brain Injury Center. It stemmed from experience evaluating and treating brain injured, homeless individuals, through a relationship between the center and a medical respite facility in Phoenix. The program for abuse survivors treats uninsured and insured patients.
Bridwell, who is the Concussion and Brain Injury Center's social worker, noticed there was a high incidence of brain injury among homeless women.

Cárdenas
Through discussions with the women and through a review of the sparse literature available on medical conditions suffered by abuse survivors, Cárdenas and Bridwell hypothesized that the homeless women's brain injuries resulted from past physical assaults.
Bridwell says both she and Cárdenas thought social justice required that the women have access to medical care and rehabilitation services commensurate with the access afforded to other patients with brain injuries, including athletes with traumatic brain injuries. (The institute's patients include NFL players with traumatic brain injury. Its physicians provide neurological medical services during Arizona Cardinal home football games, assessing players for concussions.)
Brain Clubs
The institute began its program for domestic abuse survivors in 2012 by partnering with a Phoenix domestic violence shelter called UMOM. It now partners with multiple Phoenix-area domestic abuse and homeless shelters, with plans to add more. Barrow secured grants to cover all the costs of treatment for these patients.
The institute educates shelter staff about the potential connection between abuse and brain injury, teaches them to recognize symptoms and impacts and gives them a simple four-question screening tool to administer to all willing clients. Clients who screen positive for brain injury can opt to go to the institute for a full neurological screening by institute neurologists and for treatment for any identified injury.
In addition to treating the medical aspects of the women's conditions, the program addresses the underlying emotional and behavioral aspects as well. Bridwell helps patients referred through the shelter partnerships to navigate the treatment process. She also helps them attain mental health counseling, job placement services, housing support and other social services.
Once a month, an institute therapist hosts an upbeat "Brain Club" at each participating shelter, providing information on brain injuries and practical tips for improving functioning. Shelter clients who attend these events get day planners, accordion filing systems and other tools to help them organize tasks of daily living, which can be a challenge for patients with traumatic brain injury.

Zieman
New insights
Dr. Glynnis Zieman, a neurologist and researcher with the Concussion and Brain Injury Center, says that there has been very little research on the incidence of traumatic brain injury among victims of domestic abuse. "All of us in health care know domestic violence happens and that it is common, but we're not necessarily always so good at making the connection between domestic violence and neurological symptoms." She hopes the work underway at Barrow will change that.
Together with Bridwell and Cárdenas, Zieman published a paper in 2016 that offers some insight into the experiences of patients cared for in the Domestic Violence Traumatic Brain Injury Program. (See sidebar below.)
The institute also is building awareness of the link between domestic abuse and brain injury through clinician education in the Phoenix area.
|
Barrow research establishes link between abuse, brain injury
Research from Dignity Health's Barrow Neurological Institute demonstrates a connection between domestic violence and traumatic brain injury.
Published in the Journal of Neurotrauma online in July 2016 and in print in February 2017, the study is called "Traumatic Brain Injury in Domestic Violence Victims: A Retrospective Study at the Barrow Neurological Institute." It is co-authored by Dr. Glynnis Zieman, a neurologist and researcher; Ashley Bridwell, a social worker; and Dr. Javier Cárdenas, a neurologist. Zieman and Bridwell are staff members of the institute's Concussion and Brain Injury Center, which Cárdenas directs.
To produce the study, Zieman, Bridwell and Cárdenas reviewed the charts of 115 institute patients with a self-reported history of head trauma resulting from domestic violence. All patients included in the study had been referred to the institute through its Domestic Violence Traumatic Brain Injury Program, which is a partnership with domestic violence shelters in the greater Phoenix area. All patients included in the study had received care at the institute between the program's inception in April 2012 and November 2015.
The chart analysis revealed that 88 percent of the patients had suffered more than one head injury in connection with abuse and 81 percent had sustained "too many injuries to count."
About 80 percent of the patients had reported a loss of consciousness related to at least one of their injuries.
Just 20 percent had sought medical care at the time of at least one of their injuries. Nearly 90 percent of the patients in the study had an abnormal neuro-psychology evaluation at Barrow. And 14 percent had brain abnormalities visible in an MRI scan.
The chief complaint of the patients was headache, followed by memory loss.
Psychiatric disease was diagnosed in 84 percent of the study's patients.
Zieman, Bridwell and Cárdenas concluded in the study that "traumatic brain injury is a frequent sequela of domestic violence, from which many victims sustain multiple injuries without seeking medical care. Brain injuries are often sustained over many years and lead to lasting physical, behavioral, and cognitive consequences."
They wrote that better understanding of such injuries will lead to improved care for abuse survivors.
— JULIE MINDA
|
Copyright © 2018 by the Catholic Health Association
of the United States
For reprint permission, contact Betty Crosby or call (314) 253-3490.