By JULIE MINDA
While most residents of Benedictine Living Community | Garrison, North Dakota, had been troubled by the visitation lockdowns that were necessary to prevent viral spread during the pandemic, a particular resident had an especially difficult time with the isolation.
Scott Foss, the eldercare facility's executive director, says, "When open visitation returned, she was able to actually see her family, including her Tennessee family, in-person on her birthday! You could sense her smile from a mile away and her laugher that we haven't heard for so long returned. It was like sweet music!"
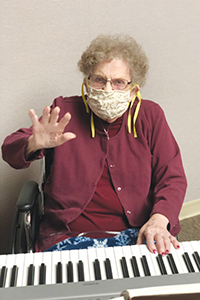
Ethel Hauf, 93, is eager to resume playing for chapel services at Benedictine Living Community | Garrison in North Dakota. She's played piano all her life.
With vaccination rates very high among residents of eldercare facilities nationwide and with COVID infection rates low in numerous communities, public health agency guidelines are allowing facility doors to open wider to visitors and, for the vaccinated, the protective plexiglass barriers no longer need separate them from visitors.
"The joy and life that have been injected back into our residents is such a blessing!" says Foss. "Families are so grateful they get to see their loved ones again; there are many tears of joy!"
A long year
The Centers for Medicare and Medicaid Services issued a memorandum in March 2020 recommending that, to prevent viral spread, long-term care facilities restrict all visitors and nonessential staff from entrance, with few exceptions.
Long-term care facilities across the U.S. adapted to the initial lockdown on visitation by connecting residents with their loved ones via videoconferencing, phone calls and window visits. They erected plexiglass and other nonporous barriers when protocols allowed for indoor visitation without contact.
Melodies
Now, in many facilities, protocols are allowing for vaccinated residents to hug their visitors and to visit with them without a barrier separating them, provided they use masks, otherwise maintain social distancing and wash their hands before and after the visit. Groups of residents are again gathering. Here too, social distancing and masking are still required. Protocols vary by state and locality, and even by facility, with some sites choosing a more conservative approach to visitation and group gatherings.
The first thing 93-year-old Ethel Hauf did when she was able to leave her room at the Benedictine Garrison facility was to head straight for the keyboard in the chapel. She's been playing piano all her life and loves religious music, but had to stop while sequestered in her room during the pandemic. It felt really good to be making music again, says Hauf, who is known as the life of the party in the skilled nursing facility.
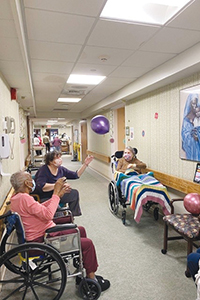
Residents of Saint Mary Home in West Hartford, Connecticut, bop balloons around a corridor. Loosened restrictions allow for residents to gather for such activities.
Foss says that Hauf telegraphed her happiness with every note. "Staff and residents listened to her beautiful music, and she brought many to tears of joy. Everyone connected to her in that moment and could see what it meant for her to play in the chapel again."
Barriers down
"I think everybody is very optimistic about what is going on," says David Becker, vice president for post-acute care for Covenant Health of Tewksbury, Massachusetts, which has 12 long-term care facilities, mainly in the northeastern U.S. "Everybody has been just ready to be with their families. They have been looking forward to this for a year."
Marissa Varney is director of nursing and assistant administrator at Covenant's St. Mary's d'Youville Pavilion in Lewiston, Maine. She says that facility had been locked down to visitors for the past year and had not seen a single COVID case during that time. She says staff and residents had worked so hard to achieve that zero-infection rate that they were very nervous before visitation resumed, but that hesitancy gave way to elation. In line with regulatory guidelines, the facility brought back indoor visitation in March, complete with hugs and hand-holding.

Dorothy Ahmann plays window tic tac toe with Benedictine Living Community | Garrison employee Desiree Klinker and Klinker's son Archer. Ahmann is a resident of the North Dakota facility.
"Residents are very excited. When you tell them they have a visitor coming, you can see the spark in their eyes now, when they know it will be an in-person visit," Varney says. Staff get emotional too as they witness the long-awaited reunions.
Laurette Chamberlain and her daughters Doris Chamberlain and Doreen Caron were among the many who had struggled over the past year with the lockdown. Laurette Chamberlain has dementia, and she had some trouble understanding the dynamics of the visits separated by windows or plexiglass dividers. And Caron found it difficult to endure the year with no physical contact with her mother.
When visitation without barriers opened in late March for the vaccinated, Caron embraced her mom for the first time in over a year. Her mother wept.
Doris Chamberlain lives in Florida — last summer she had to miss the long stretch of in-person visits she normally has with her mother during her annual trip to her hometown. When she sees her mother this summer, she plans to sit outdoors and reminisce with her as the two love to do.

Trosen
Normalcy
Kara Trosen, a therapeutic recreation director at Saint Mary Home in West Hartford, Connecticut, says that during one of the first in-person visits at her facility, a usually composed man practically sprinted to his waiting mom for their first hug in a year.
Another family was overjoyed to celebrate their loved one's 103rd birthday with her in-person. "It sends a shiver down my spine to witness these moments," says Trosen.

Mueller
Sigh of relief
Like Saint Mary Home, the Sanctuary at Holy Cross in South Bend, Indiana, is part of Trinity Health Senior Communities, which operates Trinity Health's 33 eldercare facilities in six states. Holy Cross Executive Director Jack Mueller says this period of gradual reopening has felt like a spring reawakening. He mentions the daughter who had come to see her mother three times a day before the pandemic and is beyond grateful to get back to that schedule. He says one gentleman now waits eagerly at the door each day for his wife's visit. "The staff has been ecstatic, because we'd seen what isolation has done to our residents, and that has been terrible."
Now, in addition to hosting in-person visits, residents can leave the facility, dine with their loved ones and return without having to quarantine. Mueller says residents talk excitedly about the meals they enjoyed during their excursions.
The resumption of in-person, barrier-free visits "has been a huge change for long-term care, and we are thrilled," Mueller says. "We've been really privileged to watch residents come back out of their shells and come back into themselves."
Some eldercare residents hesitant to resume activities, socialize with others
While most long-term care residents had been eager for a resumption of group activities and have embraced the chance to socialize again, some elders have been so significantly impacted by the amount of time they've spent isolated in their rooms as part of contagion prevention protocols, they have been slow to reengage.
"They feel comfortable in their rooms watching TV. There is a sense of disconnect and also a little bit of depression," said Fr. Matthew Perumpil, mission integration director of the St. Camillus eldercare campus in Wauwatosa, Wisconsin.
He said visitors who have returned to the facility after a year away comment on the emotional and physical toll the isolation has taken on residents.

Fr. Sheehan
Lonely, anxious, depressed
Fr. Myles Sheehan, SJ, is a physician who directs the Pellegrino Center for Clinical Bioethics at Georgetown University Medical Center. In his presentation at a recent CHA webinar on the plight of long-term care patients during the pandemic, he said that lockdowns were necessary to help prevent infection among those most likely to die from COVID-19. However, the lockdowns were "a very bad thing in the way that they impacted those individuals with loneliness, anxiety, depression and just boredom and the pain from deprivation of normal contact and activities."
Fr. Sheehan said for nursing home residents with mild cognitive disorders, the lack of stimulation and routine that happened during the pandemic lockdowns may have caused decline. He said, "Lacking the markers that would help to reorient a person, (they could) become more confused and … have their cognitive problems worsen quite a bit." The added burden of depression also may have worsened conditions.
"I just can't imagine what it's like for somebody in their 80s or 90s to be shut in a room, not able to see their kids or their grandkids," Fr. Sheehan said. "They have to have their meals in the room. Not to have any of the activities that they might've looked forward to — it's almost like being in prison."
He said he believes many long-term care residents were traumatized. "It was day after day of real fear for one's life. Worrying about how you would get through the day without having some of the supports you were used to as well as that trauma of being ripped away from your loved ones — multiple events that cause great stress and cumulative trauma on our older residents."
Webinar co-presenter Dr. Leonardo Palombi, director of the department of biomedicine and prevention, and professor of hygiene, epidemiology and public health at University Tor Vergata in Rome, said there is a link between loneliness and isolation and worsening of diseases, including cardiovascular conditions.
Out of hibernation
Scott Foss, executive director of Benedictine Living Community | Garrison, North Dakota, said such impacts were evident throughout the lockdown, including when it came to residents experiencing depression connected with the isolation. He says while staff had spent extra time in residents' rooms to engage them and had connected them with loved ones via technology during the lockdowns, "That only goes so far. Human interaction and getting out and about really is meaningful for our residents and truly gives them a sense of purpose."
Foss said as that facility began reopening earlier this year, "Initially it was very different for our residents and staff. The residents literally were very wary of coming out of their rooms especially on the first couple of days. It really almost seemed like they had been in hibernation and had to get reacclimated to all of their surroundings.
"We had several residents that had lost some weight and were a little depressed. But that quickly began to change after they were able to get out of their room more, socialize and even eat in the dining room on a rotation with social distancing."

Amado
Kaysee Amado, a therapeutic recreation director at Saint Mary Home in West Hartford, Connecticut, said she's seen some residents so used to worrying about socializing that they are nervous to join newly restarted group activities. She said she and fellow recreation therapists like to experiment with different activities and approaches to see what will draw out the few holdouts who used to do group activities but have not rejoined them.
Kathleen Kelleher is director of mission and spiritual care for Youville House in Cambridge and Youville Place in Lexington, both Covenant Health eldercare sites in Massachusetts. She said that when both facilities' chapels reopened with limited capacity, not all available chairs were filled initially. She attributed that to cognitive and physical decline, and residents having become accustomed to viewing chapel services from their apartments. They are slowly coming back to the chapel.
Kelleher said staff have been coaxing people out to receive spiritual and sacramental nourishment. "We're trying to help them feel safe and comfortable" so they can embrace the new level of freedom.
— JULIE MINDA